Abstract
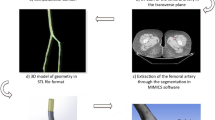
The influence of wall motion on the hemodynamic characteristics of the human femoral bifurcation and its effects on the development of peripheral artery disease has not been previously investigated. This study aimed in investigating the hemodynamics of a compliant patient-specific femoral artery bifurcation model by a fluid structure interaction (FSI) scheme. The complex physiological geometry of the femoral artery bifurcation was reproduced from sequentially obtained transverse CT scan images. Velocity waveforms derived from phase contrast MR images were extracted and mapped to define boundary conditions. Equations governing blood flow and wall motion were solved using an FSI framework that utilizes commercial codes: FLUENT for computational fluid dynamics and ANSYS for computational structural dynamics. The results showed that wall compliance decreased flow velocities at the relatively high curvature geometries including common and superficial femoral artery (SFA), and it created strong recirculation in the profunda femoris artery close to the bifurcation. In the SFA region near the apex, time averaged wall shear stress (TAWSS) differences up to 25% between compliant and rigid models were observed. The compliant model also exhibited lower TAWSS and oscillatory shear at the superior section of the common femoral artery close to the bifurcation. The presence of wall motion, however, created minor differences in the general flow-field characteristics. We conclude that wall motion does not have significant influence on the global fluid dynamic characteristics of the femoral artery bifurcation. Longer arterial segments need to be simulated to see the effect of wall motion on tortuousity which was previously cited as an important factor in the development of atherosclerosis at the femoral artery.












Similar content being viewed by others
References
Anayiotos A., S. Jones, D. P. Giddens, S. Glagov, C. K. Zarins. Shear stress at a compliant model of the human carotid bifurcation. J. Biomech. Eng. 116(1): 98–106, 1994. doi:10.1115/1.2895710
Anayiotos A., P. D. Pedroso, E. C. Elefhteriou, R. Venugopalan, W. Holman. Effect of a flow-streamlining implant at the distal anastomosis of a coronary artery bypass graft. Ann. Biomed. 30(7): 917–926, 2002. doi:10.1114/1.1500407
Back L. H., M. R. Back, E. Y. Kwack, D. W. Crawford. Flow measurements in a human femoral artery model with reverse lumen curvature. J. Biomech. Eng. 110(4): 300–309, 1988
Bao X., C. Lu, J. A. Frangos. Temporal gradient in shear but not steady shear stress induces PDGF-A and MCP-1 expression in endothelial cells: role of NO, NF kappa B, and egr-1. Arterioscler. Thromb. Vasc. Biol. 19(4): 996–1003, 1999
Flow in large blood vessels, Fluid Dynamics in Biology, Contemporary Math. Series, edited by A. Y. Cheer and C. P. Van Dam, Amer. Math. Soc. Providence, 1992, pp. 479–518
Botnar R., G. Rappitsch, M. B. Scheidegger, D. Liepsch, K. Perktold, P. Boesiger. Hemodynamics in the carotid artery bifurcation: a comparison between numerical simulations and in vitro MRI measurements. J. Biomech. 33(2): 137–144, 2000. doi:10.1016/S0021-9290(99)00164-5
Cho Y. I., L. H. Back, D. W. Crawford. Pressure difference-flow rate variation in a femoral artery branch casting of man for steady flow. J. Biomech. Eng. 105(3): 258–262, 1983
Cho Y. I., L. H. Back, D. W. Crawford. Experimental investigation of branch flow ratio, angle, and Reynolds number effects on the pressure and flow fields in arterial branch models. J. Biomech. Eng. 107(3): 257–267, 1985
Duchon J. Splines minimizing rotation-invariant semi-norms in Sobolev spaces. Constructive Theory of Functions of Several Variables. Lect. Notes Math. 571: 85–100, 1977
Duncan D. D., C. B. Bargercon, S. E. Borchart, O. J. Deters, S. A. Gearhart, F. F. Mark, M. H. Friedman. The effect of compliance on wall shear in casts of a human aortic bifurcation. J. Biomech. Eng. 112(2): 183–188, 1990. doi:10.1115/1.2891170
Farhat C., M. Lesoinne. Two efficient staggered algorithms for the serial and parallel solution of three-dimensional nonlinear transient aeroelastic problems. Comput. Meth. 182: 499–515, 2000
Farhat C., M. Lesoinne, P. LeTallec. Load and motion transfer algorithms for fluid/structure interaction problems with non-matching discrete interfaces: momentum and energy conservation, optimal discretization and application to aeroelasticity. Comput. Meth. 157: 95–114, 1998
Friedman M. H., G. M. Hutchins, C. B. Bargeron, O. J. Deters, F. F. Mark. Correlation between intimal thickness and fluid shear in human arteries. Atherosclerosis 39(3): 425–436, 1981. doi:10.1016/0021-9150(81)90027-7
Futterman L. G., L. Lemberg. Peripheral arterial disease is only the tip of the atherosclerotic “Iceberg”. Am. J. Crit. Care. 11(4): 390–394, 2002
Garasic J. M., M. A. Creager. Percutaneous interventions for lower-extremity peripheral atherosclerotic disease. Rev. Cardiovasc. Med. 2(3): 120–125, 2001
Gijsen F. J. H., D. E. M. Palmen, M. H. E. van der Beek, F. N. van de Vosse, M. E. H. van Dongen, J. D. Janssen. Analysis of the axial flow field in stenosed carotid artery bifurcation models-LDA experiments. J. Biomech. 29(11): 1483–1489, 1996. doi:10.1016/0021-9290(96)84544-1
Giordana S., S. J. Sherwin, J. Peiro, D. J. Doorly, J. S. Crane, K. E. Lee, N. J. W. Cheshire, C. G. Caro. Local and global geometric influence on steady flow in distal anastomoses of peripheral bypass grafts. J. Biomech. Eng. 127(7): 1087–098, 2005. doi:10.1115/1.2073507
Higgins, C. B., and A. Roos. MRI and CT of the Cardiovascular System, 2nd edn. Lippincott Williams & Wilkins, 2005
Hirsch A. T., M. H. Criqui, D. T. Jacobson, J. G. Regensteiner, M. A. Creager, J. W. Olin, S. H. Krook, D. B. Hunninghake, A. J. Comerota, M. E. Walsh, M. M. McDermott, W. R. Hiatt. Peripheral arterial disease detection, awareness, and treatment in primary care. JAMA 286(11): 1317–1324, 2001. doi:10.1001/jama.286.11.1317
Ito Y., A. M. Shih, B. K. Soni, K. Nakahashi. Multiple marching direction approach to generate high quality hybrid meshes. AIAA J. 45(1): 162–167, 2007. doi:10.2514/1.23260
Ito Y., P. C. Shum, A. M. Shih, B. K. Soni, K. Nakahashi. Robust generation of high-quality unstructured meshes on realistic biomedical geometry. Int. J. Numer. Meth. Eng. 65(6): 943–973, 2006. doi:10.1002/nme.1482
Jones C. J. H., M. J. Lever, Y. Ogasawara, K. H. Parker, K. Tsujioka, O. Hiramatsu, K. Mito, C. G. Caro, F. Kajiya. Blood velocity distributions within intact canine arterial bifurcations. Am. J. P. 262: H1592–H1599, 1992
Kim, Y. H. Development of efficient algorithms for fluid-structure interaction framework and its applications. Ph.D. Dissertation, University of Alabama at Birmingham, 2006
Kim Y. H., J. E. Kim. New hybrid interpolation method for motion transfer in fluid structure interactions. J. Aircraft 43(2): 567–569, 2006. doi:10.2514/1.15097
Kornet L., A. P. Hoeks, J. Lambregts, R. S. Reneman. Mean wall shear stress in the femoral arterial bifurcation is low and independent of age at rest. J. Vasc. Res. 37(2): 112–122, 2000 doi:10.1159/000025722
Ku D. N., D. P. Giddens, C. K. Zarins, S. Glagov. Pulsatile flow and atherosclerosis in the human carotid bifurcation. Arteriosclerosis 5(3): 293–302, 1985
Lei M., C. Kleinstreuer, J. P. Archie. Geometric design improvements for femoral graft-artery junctions mitigating restenosis. J. Biomech. 29(12): 1605–1614, 1996
Li Z., C. Kleinstreuer. Fluid-structure interaction effects on sac-blood pressure and wall stress in a stented aneurysm. J. Biomech. Eng. 127(4): 662–671, 2005. doi:10.1115/1.1934040
Liepsch D., S. Moravec. Pulsatile flow of non-newtonian fluid in distensible models of human arteries. Biorheology 21(4): 571–586, 1984
LoGerfo F. W., M. D. Nowak, W. C. Quist, H. M. Crawshaw, B. K. Bharadvaj. Flow studies in a model carotid bifurcation. Arteriosclerosis 1(4): 235–241, 1981
Loth F., N. Arslan, P. F. Fischer, C. D. Bertram, S. E. Lee, T. J. Royston, R. H. Song, W. E. Shaalan, H. S. Bassiouny. Transitional flow at the venous anastomosis of an arteriovenous graft: Potential relationship with activation of the ERK1/2 mechanotransduction pathway. J. Biomech. Eng. 125(1): 49–61, 2003. doi:10.1115/1.1537737
Mark F. F., C. B. Bergeron, O. J. Deters, M. H. Friedman. Variations in geometry and shear rate distributions in casts of human aortic bifurcations. J. Biomech. 22(6–7): 577–582, 1989. doi:10.1016/0021-9290(89)90009-2
Maurits N. M., G. E. Loots, A. E. P. Veldman. The influence of vessel wall elasticity and peripheral resistance on the carotid artery flow wave form: a CFD model compared to in vivo ultrasound measurements. J. Biomech. 40(2): 427–436, 2007. doi:10.1016/j.jbiomech.2005.12.008
McDermott M. M., K. Liu, P. Greenland, J. M. Guralnik, M. H. Criqui, C. Chan, W. H. Pearce, J. R. Schneider, L. Ferrucci, L. Celic, L. M. Taylor, E. Vonesh, G. J. Martin, E. Clark. Functional decline in peripheral arterial disease: associations with the ankle brachial index and leg symptoms. JAMA 292(4): 453–461, 2004. doi:10.1001/jama.292.4.453
Mooney M. A theory of large elastic deformation. J. Appl. Physiol. 11: 582–592, 1940. doi:10.1063/1.1712836
Motomiya M., T. Karino. Flow patterns in the human carotid artery bifurcation. Stroke 15(1): 50–56, 1984
Mozersky D. J., D. S. Sumner, D. E. Hokanson, D. E. Strandness Jr. Transeutaneous measurement of the elastic properties of the human femoral artery. Circulation 46(5): 948–955, 1972
Ostchega Y., R. Paulose-Ram, C. F. Dillon, Q. Gu, J. P. Hughes. Prevalence of peripheral arterial disease and risk factors in persons aged 60 and older: data from the national health and nutrition examination survey 1999–2004. J. Am. Geriatr. Soc. 55(4): 583–589, 2007. doi:10.1111/j.1532-5415.2007.01123.x
Papaharilaou Y., J. A. Ekaterinaris, E. Manousaki, A. N. Katsamouris. A decoupled fluid structure approach for estimating wall stress in abdominal aortic aneurysms. J. Biomech. 40(2): 367–377, 2007. doi:10.1016/j.jbiomech.2005.12.013
Perktold K., G. Rappitsch. Computer-simulation of local blood-flow and vessel mechanics in a compliant carotid-artery bifurcation model. J. Biomech. 28(7): 845–856, 1995. doi:10.1016/0021-9290(95)95273-8
Prendergast P. J., C. Lally, S. Daly, A. J. Reid, T. C. Lee, D. Quinn, F. Dolan. Analysis of prolapse in cardiovascular stents: a constitutive equation for vascular tissue and finite element modeling. J. Biomech. Eng. 125(5): 692–699, 2003. doi:10.1115/1.1613674
Rhee K., S. M. Lee. Effects of radial wall motion and flow waveform on the wall shear rate distribution in the divergent Vascular Graft. Ann. Biomed. 26(6): 955–964, 1998. doi:10.1114/1.31
Sanctis J. T. D. Percutaneous interventions for lower extremity peripheral vascular disease. Am. Fam. Physician 64(12): 1965–1972, 2001
Smedby O. Do plaques grow upstream or downstream: an angiographic study in the femoral artery. Arterioscler. Thromb. Vasc. Biol. 17(5): 912–918, 1997
Smedby O., L. Bergstrand. Tortuosity and atherosclerosis in the femoral artery: what is cause and what is effect? Ann. Biomed. 24(4): 474–480, 1996. doi:10.1007/BF02648109
Smedby O., J. Johansson, J. Molgaard, A. G. Olsson, G. Walldius, U. Erikson. Predilection of atherosclerosis for the inner curvature in the femoral artery. A digitized angiography study. Arterioscler. Thromb. Vasc. Biol. 15(7): 912–917, 1995
Smedby O., S. Nilsson, L. Bergstrand. Development of femoral atherosclerosis in relation to flow disturbance. J. Biomech. 29(4): 543–547, 1996. doi:10.1016/0021-9290(95)00070-4
Smilde T. J., F.W. van den Berkmortel, G. H. Boers, H. Wollersheim, T. de Boo, H. van Langen, A. F. Stalenhoef. Carotid and femoral artery wall thickness and stiffness in patients at risk for cardiovascular disease, with special emphasis on hyperhomocysteinemia. Arterioscler. Thromb. Vasc. Biol. 18(12): 1958–1963, 1998
Steinman D. A. Image-based computational fluid dynamics modeling in realistic arterial geometries. Ann. Biomed. 30(4): 483–497, 2002. doi:10.1114/1.1467679
Tai N. R., A. Giudiceandrea, H. J. Salacinski, A. M. Seifalian, G. Hamilton. In vivo femoropopliteal arterial wall compliance in subjects with and without lower limb vascular disease. J. Vasc. Surg. 30(5): 936–945, 1999. doi:10.1016/S0741-5214(99)70020-0
Wensing P. J., L. Meiss, W. P. Mali, B. Hillen. Early atherosclerotic lesions spiraling through the femoral artery. Arterioscler. Thromb. Vasc. Biol. 18(10): 1554–1558, 1998
Wood N. B., S. Z. Zhao, A. Zambanini, M. Jackson, W. Gedroyc, S. A. Thom, A. D. Hughes, X. Y. Xu. Curvature and tortuosity of the superficial femoral artery: a possible risk factor for peripheral arterial disease. J. Appl. Physiol. 101(5): 1412–1418, 2006. doi:10.1152/japplphysiol.00051.2006
Wu S. P., S. Ringgaard, S. Oyre, M. S. Hansen, S. Rasmus, E. M. Pedersen. Wall shear rates differ between the normal carotid, femoral, and brachial arteries: an in vivo MRI study. J. Magn. Reson. Imaging, 19(2): 188–193, 2004. doi:10.1002/jmri.10441
Younis H. F., M. R. Kaazempur-Mofrad, R. C. Chan, A. G. Isasi, D. P. Hinton, A. H. Chau, L. A. Kim, R. D. Kamm. Hemodynamics and wall mechanics in human carotid bifurcation and its consequences for atherogenesis: investigation of inter-individual variation. Biomech. Model. Mechanobiol. 3: 17–32, 2004. doi:10.1007/s10237-004-0046-7
Zeng D., R. Ethier. A semi-torsional spring analogy model for updating unstructured meshes in 3D moving domains. Finite. Elem. Anal. Des. 41(11–12): 1118–1139, 2005
Zhang W., C. Herrera, S. N. Atluri, G. S. Kassab. Effect of surrounding tissue on vessel fluid and solid mechanics. J. Biomech. Eng. 126(6): 760–769, 2004. doi:10.1115/1.1824128
Zhao S. Z., P. Papathanasopoulou, Q. Long, I. Marshall, X. Y. Xu. Comparative study of magnetic resonance imaging and image-based computational fluid dynamics for quantification of pulsatile flow in a carotid bifurcation phantom. Ann. Biomed. 31(2): 962–971, 2003. doi:10.1114/1.1590664
Zhao S. Z., X. Y. Xu, A. D. Hughes, S. A. Thom, A. V. Stanton, B. Ariff, Q. Long. Blood flow and vessel mechanics in a physiologically realistic model of a human carotid arterial bifurcation. J. Biomech. 33(8): 975–984, 2000. doi:10.1016/S0021-9290(00)00043-9
Acknowledgment
The authors would like to thank Mr. Corey Shum in the Enabling Technology Laboratory, University of Alabama at Birmingham for extracting geometry data from the CT scan.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kim, YH., Kim, JE., Ito, Y. et al. Hemodynamic Analysis of a Compliant Femoral Artery Bifurcation Model using a Fluid Structure Interaction Framework. Ann Biomed Eng 36, 1753–1763 (2008). https://doi.org/10.1007/s10439-008-9558-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-008-9558-0