Abstract
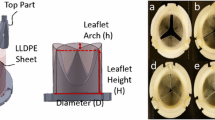
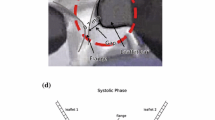
Polymeric heart valves have the potential to reduce thrombogenic complications associated with current mechanical valves and overcome fatigue-related problems experienced by bioprosthetic valves. In this in vitro study, the velocity fields inside and downstream of two different prototype tri-lealfet polymeric heart valves were studied. Experiments were conducted on two 23 mm prototype polymeric valves, provided by AorTech Europe, having open or closed commissure designs and leaflet thickness of 120 and 80 μm, respectively. A two-dimensional LDV system was used to measure the velocity fields in the vicinity of the two valves under simulated physiological conditions. Both commissural design and leaflet thickness were found to affect the flow characteristics. In particular, very high levels of Reynolds shear stress of 13,000 dynes/cm2 were found in the leakage flow of the open commisure design. Maximum leakage velocities in the open and closed designs were 3.6 m/s and 0.5 m/s respectively; the peak forward flow velocities were 2.0 m/s and 2.6 m/s, respectively. In both valve designs, shear stress levels exceeding 4,000 dyne/cm2 were observed at the trailing edge of the leaflets and in the leakage and central orifice jets during peak systole. Additionally, regions of low velocity flow conducive to thrombus formation were observed in diastole. The flow structures measured in these experiments are consistent with the location of thrombus formation observed in preliminary animal experiments.
Similar content being viewed by others
References
Bernacca, G. M., T. G. Mackay, and D. J. Wheatley. In vitro function and durability of a polyurethane heart valve: Material considerations. J. Heart Valve Dis. 5(5):538–542, 1996.
Bernacca, G. M., T. G. Mackay, M. J. Gulbransen, A. W. Donn, and D. J. Wheatley. Polyurethane heart valve durability: Effects of leaflet thickness and material. Int. J. Artif. Organs 20(6):327–331, 1997.
Bernacca, G. M., B. O’Connor, D. F. Williams, and D. J. Wheatley. Hydrodynamic function of polyurethane prosthetic heart valves: Influences of Young’s modulus and leaflet thickness. Biomaterials 23(1):45–50, 2002.
Chandran, K. B., R. Fatemi, R. Schoephoerster, D. Wurzel, G. Hansen, G. Pantalos, L. S. Yu, and W. J. Kolff. In vitro comparison of velocity profiles and turbulent shear distal to polyurethane trileaflet and pericardial prosthetic valves. Artif. Organs 13(2):148–154, 1989.
Daebritz, S. H., J. S. Sachweh, B. Hermanns, B. Fausten, A. Franke, J. Groetzner, B. Klosterhalfen, and B. J. Messmer. Introduction of a flexible polymeric heart valve prosthesis with special design for mitral position. Circulation 108 (Suppl 1):II134–II139, 2003.
Ellis, J. T., T. M. Healy, A. A. Fontaine, R. Saxena, and A. P. Yoganathan. Velocity measurements and flow patterns within the hinge region of a medtronic parallel bileaflet mechanical valve with clear housing. J. Heart Valve Dis. 5(6):591–599, 1996.
Ellis, J. T. and A. P. Yoganathan. A comparison of the hinge and near-hinge flow fields of the St Jude medical hemodynamic plus and regent bileaflet mechanical heart valves. J. Thorac Cardiovasc. Surg. 119(1):83–93, 2000.
Ellis, J. T., B. R. Travis, and A. P. Yoganathan. An in vitro study of the hinge and near-field forward flow dynamics of the St. Jude Medical Regent bileaflet mechanical heart valve. Ann. Biomed. Eng. 28(5):524–532, 2000.
Healy, T. M., J. T. Ellis, A. A. Fontaine, C. A. Jarrett, and A. P. Yoganathan. An automated method for analysis and visualization of laser Doppler velocimetry data. Ann. Biomed. Eng. 25(2):335–343, 1997.
Herold, M., H. B. Lo, H. Reul, H. Muckter, K. Taguchi, M. Giesiepen, G. Birkle, G. Hollweg, G. Rau, and B. J. Messmer. The Helmoltz-institute-tri-leaflet-polyurethane-heart valve prosthesis: Design, manufacturing and first in-vitro and in vivo results, In: Polyurethanes in Biomedical Engineering II, edited by H. E. A. Planck. Elsevier Science Publishers, 1987. pp. 231–268.
Hung, T. C., R. M. Hochmuth, J. H. Joist, and S. P. Sutera. Shear-induced aggregation and lysis of platelets. Trans. Am. Soc. Artif. Intern. Organs. 22:285–291, 1976.
Jamieson, W. R., L. H. Burr, W. N. Jr., Anderson, J. B. Chambers, J. P. Gams, and C. M. Dowd, Prosthesis-related complications: First-year annual rates. J. Heart Valve Dis. 11(6):758–763, 2002.
Jansen, J., S. Willeke, B. Reiners, P. Harbott, H. Reul, H. B. Lo, S. Dabritz, C. Rosenbaum, A. Bitter, and K. Ziehe. Advances in design principle and fluid dynamics of a flexible polymeric heart valve. ASAIO Trans. 37(3):M451–M453, 1991.
Lelah, M. D., and S. L. Cooper. Polyurethanes in Medicine. Boca Raton, Fla.: CRC Press, 1986, 225 p.
Lu, P. C., H. C. Lai, and J. S. Liu. A reevaluation and discussion on the threshold limit for hemolysis in a turbulent shear flow. J. Biomech. 34(10):1361–1364, 2001.
Mackay, T. G., D. J. Wheatley, G. M. Bernacca, A. C. Fisher, and C. S. Hindle. New polyurethane heart valve prosthesis: Design, manufacture and evaluation. Biomaterials. 17(19):1857–1863, 1996.
Nemerson, Y., and V. T. Turitto. The effect of flow on hemostasis and thrombosis. Thromb. Haemost. 66(3):272–276, 1991.
Ramstack, J. M., L. Zuckerman, and L. F. Mockros. Shear-induced activation of platelets. J. Biomech. 12(2):113–125, 1979.
Sallam, A. M., and N. H. Hwang. Human red blood cell hemolysis in a turbulent shear flow: Contribution of Reynolds shear stresses. Biorheology 21(6):783–797, 1984.
Sandwell, D. T. Biharmonic spline interpolation of GEOS-3 and SEASAT Altimeter data. Geophys. Res. Lett. 2:139–142, 1987.
Simionescu, D. T., J. J. Lovekamp, and N. R. Vyavahare. Extracellular matrix degrading enzymes are active in porcine stentless aortic bioprosthetic heart valves. J. Biomed. Mater. Res. 66A(4):755–763, 2003.
Slack, S. M., Y. Cui, and V. T. Turitto. The effects of flow on blood coagulation and thrombosis. Thromb. Haemost. 70(1):129–134, 1993.
Slack, S. M., L. K. Jennings, and V. T. Turitto. Platelet size distribution measurements as indicators of shear stress-induced platelet aggregation. Ann. Biomed. Eng. 22(6):653–659, 1994.
Slack, S. M., and V. T. Turitto. Flow chambers and their standardization for use in studies of thrombosis. On behalf of the subcommittee on rheology of the scientific and standardization committee of the ISTH. Thromb. Haemost. 72(5):777–781, 1994.
Spina, M., F. Ortolani, A. E. Messlemani, A. Gandaglia, J. Bujan, N. Garcia-Honduvilla, I. Vesely, G. Gerosa, D. Casarotto, L. Petrelli, and M. Marchini. Isolation of intact aortic valve scaffolds for heart-valve bioprostheses: Extracellular matrix structure, prevention from calcification, and cell repopulation features. J. Biomed. Mater. Res. 67A(4):1338–1350, 2003.
Tiederman, W. G., R. M. Privette, and W. M. Phillips. Cycle-to-cycle variation effects on turbulent shear stress measurment in pulsatile flows. Exp. Fluids. 6:265–272, 1988.
Turitto, V. T., and C. L. Hall. Mechanical factors affecting hemostasis and thrombosis. Thromb Res. 92(6 Suppl 2):S25–S31, 1998.
Wheatley, D. J., L. Raco, G. M. Bernacca, I. Sim, P. R. Belcher, and J. S. Boyd. Polyurethane: Material for the next generation of heart valve prostheses? Eur. J. Cardiothorac. Surg. 17(4):440–448, 2000.
Wheatley, D. J., G. M. Bernacca, M. M. Tolland, B. O’Connor, J. Fisher, and D. F. Williams. Hydrodynamic function of a biostable polyurethane flexible heart valve after six months in sheep. Int. J. Artif. Organs. 24(2):95–101, 2001.
Woo, Y. R., F. P. Williams, and A. P. Yoganathan. In vitro fluid dynamic characteristics of the abiomed trileaflet heart valve prosthesis. J. Biomech. Eng. 105(4):338–345, 1983.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Leo, HL., Simon, H., Carberry, J. et al. A Comparison of Flow Field Structures of Two Tri-Leaflet Polymeric Heart Valves. Ann Biomed Eng 33, 429–443 (2005). https://doi.org/10.1007/s10439-005-2498-z
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s10439-005-2498-z