Abstract
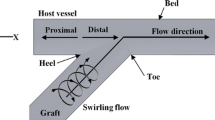
Platelet concentration near the blood vessel wall is one of the major factors in the adhesion of platelets to the wall. In our previous studies, it was found that swirling flows could suppress platelet adhesion in small-caliber artificial grafts and end-to-end anastomoses. In order to better understand the beneficial effect of the swirling flow, we numerically analyzed the near-wall concentration distribution of platelets in a straight tube and a sudden tubular expansion tube under both swirling flow and normal flow conditions. The numerical models were created based on our previous experimental studies. The simulation results revealed that when compared with the normal flow, the swirling flow could significantly reduce the near-wall concentration of platelets in both the straight tube and the expansion tube. The present numerical study therefore indicates that the reduction in platelet adhesion under swirling flow conditions in small-caliber arterial grafts, or in end-to-end anastomoses as observed in our previous experimental study, was possibly through a mechanism of platelet transport, in which the swirling flow reduced the near-wall concentration of platelets.
Similar content being viewed by others
References
Longest, P.W., Kleinstreuer, C.: Comparison of blood particle deposition models for non-parallel flow domains. J. Biomech. 36, 421–430 (2003)
Schoephoerster, R.T, Oynes, F., Nunez, G., et al.: Effects of local geometry and fluid dynamics on regional platelet deposition on artificial surfaces. Arterioscler Thromb. 13, 1806–1813 (1993)
Karino, T., Goldsmith, H.L.: Adhesion of human platelets to collagen on the walls distal to a tubular expansion. Microvasc Res. 17, 238–262 (1979)
Affeld, K., Reininger, A.J., Gadischke, J., et al.: Fluid mechanics of the stagnation point flow chamber and its platelet deposition. Artif. Organs. 19, 597–602 (1995)
David, T., Thomas, S., Walker, P.G.: Platelet deposition in stagnation point flow: an analytical and computational simulation. Med. Eng. Phys. 23, 299–312 (2001)
Stonebridge, P.A., Brophy, C.M.: Spiral laminar flow in arteries? Lancet. 338, 1360–1361 (1991)
Stonebridge, P.A., Hoskins, P.R., Allan, P.L., et al.: Spiral laminar flow in vivo. Clin. Sci. 91, 17–21 (1996)
Frazin, L.J., Lanza, G., Mehlman, D., et al.: Rotational blood flow in the thoracic aorta. Clin. Res. 38, 331A (1990)
Houston, J.G., Gandy, S.J., Milne, W.: Spiral laminar flow in the abdominal aorta: a predictor of renal impairment deterioration in patients with renal artery stenosis? Nephrol Dial Transplant. 19, 1786–1791 (2004)
Frazin, L.J., Vonesh, M.J., Chandran, K.B., et al.: Confirmation and initial documentation of thoracic and abdominal aortic helical flow: An ultrasound study. ASAIO. J. 42, 951–956 (1996)
Caro, C.G., Cheshire, N.J., Watkins, N.: Preliminary comparative study of small amplitude helical and conventional ePTFE arteriovenous shunts in pigs. J. R. Soc. Interface. 2, 261–266 (2005)
Zhan, F., Fan, Y.B., Deng, X.Y.: Swirling flow created in a glass tube suppressed platelet adhesion to the surface of the tube: Its implication in the design of small-caliber arterial grafts. Thromb. Res. 125, 413–418 (2010) DOI 10.1016/j.thromres.2009.02.011
Zhan, F., Fan, Y.B., Deng, X.Y., et al.: The beneficial effect of swirling flow on platelet adhesion to the surface of a sudden tubular expansion tube: its potential application in end-toe-nd arterial anastomosis. ASAIO. J. 56, 172–179 (2010) DOI 10.1097/MAT.0b013e3181d0ea15
Chiu, J.J., Chen, C.N., Lee, P.L., et al.: Analysis of the effect of disturbed flow on monocytic adhesion to endothelial cells. J. Biomech. 36, 1883–1895 (2003)
Longest, P.W., Kleinstreuer, C.: Particle-hemodynamics modeling of the distal end-to-side femoral bypass: effects of graft caliber and graft-end cut. Med. Eng. Phys. 25, 843–858 (2003)
Fluent, Inc.: Fluent 6.1.22 Users’ Guide (2004)
Morsi, S.A., Alexander, A.J.: An investigation of particle trajectories in two phase flow systems. J. Fluid Mech. 55, 193–208 (1972)
Sauvage, L.R., Walker, M.W., Berger, K., et al.: Current arterial prostheses: Experimental evaluation by implantation in the carotid and circumflex coronary arteries of the dog. Arch. Surg. 114, 687–691 (1979)
Rickard, R.F., Meyer, C., Hudson, D.A.: Computational modeling of microarterial anastomoses with size discrepancy (small-to-large). J. Surg. Res. 153, 1–11 (2009)
Turitto, V.T., Hall, C.L.: Mechanical factors affecting hemostasis and thrombosis. Thromb. Res. 92(6 Suppl 2), S25–S31 (1998)
Nemerson, Y., Turitto, V.T.: The effect of flow on hemostasis and thrombosis. Thromb. Haemost. 66, 272–276 (1991)
Kroll, M.H., Hellums, J.D., McIntire, L.V., et al.: Platelets and shear stress. Blood. 88, 1525–1541 (1996)
Author information
Authors and Affiliations
Corresponding author
Additional information
The project was supported by Grant-in-Aid from the National Natural Science Foundation of China (10632010, 11072023).
Rights and permissions
About this article
Cite this article
Zhan, F., Fan, YB. & Deng, XY. Effect of swirling flow on platelet concentration distribution in small-caliber artificial grafts and end-to-end anastomoses. Acta Mech Sin 27, 833–839 (2011). https://doi.org/10.1007/s10409-011-0486-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10409-011-0486-0