Abstract
Purpose
To retrospectively compare the clinical and pathological characteristics of breast masses and non-mass lesions that underwent ultrasound (US)-guided 16-gauge spring-loaded core needle biopsy (CNB) or 12-gauge spring-loaded vacuum-assisted biopsy (VAB).
Methods
We retrospectively compared the results from US-guided diagnostic breast biopsy performed with a 16-gauge CNB (Magnum™) or a 12-gauge VAB (Celero®). The patients’ backgrounds and pathological features for each device were examined.
Results
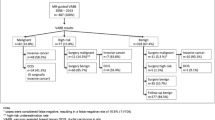
In 453 patients with 500 lesions, 373 lesions underwent CNB and 127 underwent VAB. The positive biopsy rate (positive predictive value 3) was significantly higher for VAB (92/127; 72.4%) than for CNB (231/373; 61.9%) (P = 0.032). Non-mass lesions were biopsied more frequently with VAB (57/127; 47.4%) than with CNB (27/378; 7.14%) (P = 0.000). The upgrade rate from high-risk to malignant lesions was significantly higher for CNB (5/19; 26.3%) than for VAB (1/8; 12.5%) (P = 0.043). There were five (1.34%) specimen failures with CNB and one (0.78%) with VAB, 18 (4.82%) re-biopsies with CNB and three (2.36%) with VAB, and 11/21 (52.4%) upgrades from ductal carcinoma in situ (DCIS) to invasive ductal carcinoma (IDC) with CNB and 11/30 (36.7%) with VAB. Although these rates tended to be higher with CNB than with VAB, the difference was not significant.
Conclusion
Although VAB had a significantly higher rate of non-mass lesion biopsies, the upgrade rate from high-risk to malignant lesions was significantly lower for VAB than for CNB. US-guided 12-gauge spring-loaded VAB may be more appropriate for biopsy of non-mass lesions.



Similar content being viewed by others
Data Availability
Not Applicable.
References
Hooley RJ, Scoutt LM, Philpotts LE. Breast ultrasonography: state of the art. Radiology. 2013;268:642–59.
Fujioka T, Mori M, Kubota K, et al. Simultaneous comparison between strain and shear wave elastography of breast masses for the differentiation of benign and malignant lesions by qualitative and quantitative assessments. Breast Cancer. 2019;26:792–8.
Tan PH, Ellis I, Allison K. The 2019 World Health Organization classification of tumours of the breast. Histopathology. 2020;77:181–5.
Mendelson E, Baum J, Berg W, et al. Breast imaging reporting and data system, BI-RADS: Ultrasound. Reston: American College of Radiology; 2003.
Ko KH, Hsu HH, Yu JC, et al. Non-mass-like breast lesions at ultrasonography: feature analysis and BI-RADS assessment. Eur J Radiol. 2015;84:77–85.
Uematsu T. How to choose needles and probes for ultrasonographically guided percutaneous breast biopsy: a systematic approach. Breast Cancer. 2012;19:238–41.
Goldhirsch A, Winer EP, Coates AS, et al. Personalizing the treatment of women with early breast cancer: highlights of the St Gallen International Expert Consensus on the Primary Therapy of Early Breast Cancer 2013. Ann Oncol. 2013;24:2206–23.
Simon JR, Kalbhen CL, Cooper RA, et al. Accuracy and complication rates of US-guided vacuum-assisted core breast biopsy: initial results. Radiology. 2000;215:694–7.
Nakano S, Imawari Y, Mibu A, et al. Differentiating vacuum-assisted breast biopsy from core needle biopsy: is it necessary? Br J Radiol. 2018;91:20180250.
Philpotts LE, Hooley RJ, Lee CH. Comparison of automated versus vacuum-assisted biopsy methods for sonographically guided core biopsy of the breast. AJR Am J Roentgenol. 2003;180:347–51.
Cho N, Moon WK, Cha JH, et al. Sonographically guided core biopsy of the breast: comparison of 14-gauge automated gun and 11-gauge directional vacuum-assisted biopsy methods. Korean J Radiol. 2005;6:102–9.
Choe J, Chikarmane SA, Giess CS. Nonmass findings at breast US: definition, classifications, and differential diagnosis. Radiographics. 2020;40:326–35.
Krishnamurthy S, Bevers T, Kuerer H, et al. Multidisciplinary considerations in the management of high-risk breast lesions. AJR Am J Roentgenol. 2012;198:W132–40.
Suh YJ, Kim MJ, Kim EK, et al. Comparison of the underestimation rate in cases with ductal carcinoma in situ at ultrasound-guided core biopsy: 14-gauge automated core-needle biopsy vs 8- or 11-gauge vacuum-assisted biopsy. Br J Radiol. 2012;85:e349–56.
Feig SA. Auditing and benchmarks in screening and diagnostic mammography. Radiol Clin North Am. 2007;45:791–800.
Acknowledgements
This study received no specific grant from any funding agency.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
We declare that the authors have no conflicts of interest.
Ethical approval
This retrospective study was approved by the medical ethics committee of our institution, which waived the requirement for written informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Yashima, Y., Fujioka, T., Kubota, K. et al. Comparison of the clinical and pathological characteristics of ultrasound-guided biopsy for breast masses and non-mass lesions between 16-gauge spring-loaded core needle biopsy and 12-gauge spring-loaded vacuum-assisted biopsy. J Med Ultrasonics 50, 205–212 (2023). https://doi.org/10.1007/s10396-022-01279-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10396-022-01279-3