Abstract
Purpose
To assess the feasibility of an automated fractional shortening (Auto FS) measurement method using two-dimensional tracking and to construct a reference range for normal fetuses.
Methods
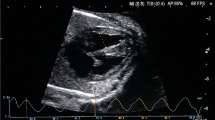
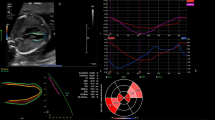
This study was conducted from May 2017 to March 2018. First, cardiac motion in the four-chamber view was recorded in the B-mode. Subsequently, the region of interest was set on the edge of the ventricular septum or ventricular muscle at a point one-third away from the atrioventricular valve toward the cardiac apex. Tracking was automatically performed. Values measured between the ventricular septum and right ventricle were defined as R-Auto FS, whereas those measured between the ventricular septum and left ventricle were defined as L-Auto FS. Those on each ventricular muscle were defined as Combined-Auto FS.
Results
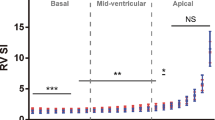
Data were obtained from 131 singleton fetuses. R-Auto FS significantly decreased with an increase in the number of gestational weeks, and L-Auto FS and Combined-Auto FS showed the same tendency (Spearman’s correlation analysis: p = − .528, p = − .351, and p = − .636, respectively).
Conclusion
We succeeded in defining a reference Auto FS value for normal singleton pregnancies. Auto FS was negatively correlated with gestational age. This novel technique can assess fetal heart contractility.




Similar content being viewed by others
Change history
19 June 2019
In the original publication of the article, the Conflict of interest statement.
References
Wladimiroff JW, McGhie JS. M-mode ultrasonic assessment of fetal cardiovascular dynamics. Br J Obstet Gynaecol. 1981;88:1241–5.
DeVore GR, Siassi B, Platt LD. Fetal echocardiography. IV. M-mode assessment of ventricular size and contractility during the second and third trimesters of pregnancy in the normal fetus. Am J Obstet Gynecol. 1984;150:981–8.
Hsieh YY, Chang FC, Tsai HD, et al. Longitudinal survey of fetal ventricular ejection and shortening fraction throughout pregnancy. Ultrasound Obstet Gynecol. 2000;16:46–8.
Gardiner HM, Pasquini L, Wolfenden J, et al. Myocardial tissue Doppler and long axis function in the fetal heart. Int J Cardiol. 2006;113:39–47.
Huhta JC. Guidelines for the evaluation of heart failure in the fetus with or without hydrops. Pediatr Cardiol. 2004;25:274–86.
DeVore GR. Assessing fetal cardiac ventricular function. Semin Fetal Neonatal Med. 2005;10:515–41.
Michelfelder E, Allen C, Urbinelli L. Evaluation and management of fetal cardiac function and heart failure. Curr Treat Options Cardiovasc Med. 2016;18:55.
Simpson JM, Cook A. Repeatability of echocardiographic measurements in the human fetus. Ultrasound Obstet Gynecol. 2002;20:332–9.
Royston P, Wright EM. How to construct ‘normal ranges’ for fetal variables. Ultrasound Obst Gyn. 1998;11:30–8.
DeVore GR. Computing the Z score and centiles for cross-sectional analysis: a practical approach. J Ultrasound Med. 2017;36:459–73.
Takano M, Nakata M, Nagasaki S, et al. Assessment of diastolic function of normal fetal heart using dual-gate Doppler. Ultrasound Obstet Gynecol. 2018;52:238–42.
Jones CJ, Raposo L, Gibson DG. Functional importance of the long axis dynamics of the human left ventricle. Br Heart J. 1990;63:215–20.
Maciver DH. The relative impact of circumferential and longitudinal shortening on left ventricular ejection fraction and stroke volume. Exp Clin Cardiol. 2012;17:5–11.
Wandt B. Long-axis contraction of the ventricles: a modern approach, but described already by Leonardo da Vinci. J Am Soc Echocardiogr. 2000;13:699–706.
Luewan S, Yanase Y, Tongprasert F, et al. Fetal cardiac dimensions at 14-40 weeks’ gestation obtained using cardio-STIC-M. Ultrasound Obstet Gynecol. 2011;37:416–22.
Johnson P, Maxwell DJ, Tynan MJ, et al. Intracardiac pressures in the human fetus. Heart. 2000;84:59–63.
Reed KL, Meijboom EJ, Sahn DJ, et al. Cardiac Doppler flow velocities in human fetuses. Circulation. 1986;73:41–6.
Molina FS, Faro C, Sotiriadis A, et al. Heart stroke volume and cardiac output by four-dimensional ultrasound in normal fetuses. Ultrasound Obstet Gynecol. 2008;32:181–7.
Kenny JF, Plappert T, Doubilet P, et al. Changes in intracardiac blood flow velocities and right and left ventricular stroke volumes with gestational age in the normal human fetus: a prospective Doppler echocardiographic study. Circulation. 1986;74:1208–16.
De Smedt MC, Visser GH, Meijboom EJ. Fetal cardiac output estimated by Doppler echocardiography during mid- and late gestation. Am J Cardiol. 1987;60:338–42.
Acknowledgements
This work was partially supported by JSPS KAKENHI (Grant No.: JP16K11114).
Author information
Authors and Affiliations
Contributions
Sumito Nagasaki designed the study and wrote the initial manuscript draft. Masahiko Nakata contributed to the analysis and interpretation of data and assisted in the preparation of the manuscript. All other authors contributed to data collection and interpretation, and critically reviewed the manuscript. All authors approved the final version of the manuscript and agreed to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
All declare that they there is conflict of interest.
Ethical approval
This manuscript has not been published or presented elsewhere in part or in entirety and is not under consideration by another journal. All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional) and with the Helsinki Declaration of 1964 and later versions. All study participants provided informed consent, and the study design was approved by the appropriate ethics review board.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Nagasaki, S., Nakata, M., Takano, M. et al. Feasibility of automated fetal fractional shortening measurement with two-dimensional tracking and construction of a reference range for normal fetuses. J Med Ultrasonics 46, 467–472 (2019). https://doi.org/10.1007/s10396-019-00942-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10396-019-00942-6