Abstract
Purpose
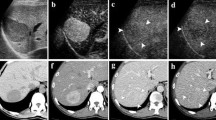
The study aimed to clarify whether contrast-enhanced (CE) three-dimensional (3D) ultrasonography (US) can depict characteristic hyperstain and washout patterns in minute nodules ≤10 mm of hepatocellular carcinoma (minute HCC), and whether it serves as a potent diagnostic modality.
Methods
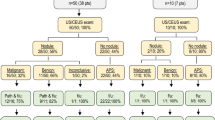
CE 3D US was carried out to depict hyperstain and washout of a solitary nodule ≤10 mm in patients with liver cirrhosis. When both patterns were depicted with success, CE computed tomography (CT) and CE magnetic resonance imaging (MRI) were also carried out as part of a comparative study, and then a histological specimen was obtained by needle biopsy. The final diagnosis was based on the histopathological findings and a follow-up on the growth of nodules.
Results
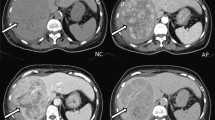
All 12 minute nodules exhibiting hyperstain and washout showed evidence of HCC when examined by CE 3D US. The CE CT and CE MRI examinations could depict both of these patterns, characteristic of HCC, in most of the nodules but rather less successfully than CE 3D US.
Conclusion
CE 3D US can depict hyperstain and washout patterns in minute HCC and serves as a potent modality for diagnosis.




Similar content being viewed by others
References
Hayashi PH, Trotter JF, Forman L, et al. Impact of pretransplant diagnosis of hepatocellular carcinoma on cadaveric liver allocation in the era of MELD. Liver Transplant. 2004;10:42–8.
Libbrecht L, Cassiman D, Berslype C, et al. Clinicopathological features of focal nodular hyperplasia-like nodules in 130 cirrhotic explant livers. Am J Gastroenterol. 2006;101:2341–6.
Bolondi L, Sofia S, Siringo S, et al. Surveillance programme of cirrhotic patients for early diagnosis and treatment of hepatocellular carcinoma: a cost effectiveness analysis. Gut. 2001;48:251–9.
Bolondi L, Gaiani S, Celli N, et al. Characterization of small nodules in cirrhosis by assessment of vascularity: the problem of hypovascular hepatocellular carcinoma. Hepatology. 2005;42:27–34.
Bruix J, Sherman M. AASLD practice guideline. Management of hepatocellular carcinoma. Hepatology. 2005;42:1208–36.
Forner A, Vilana R, Ayuso C, et al. Diagnosis of hepatic nodules 20 mm or smaller in cirrhosis: prospective validation of the noninvasive diagnostic criteria for hepatocellular carcinoma. Hepatology. 2008;47:97–104.
Burns PN, Wilson SR. Focal liver masses: enhancement patterns on contrast-enhanced images—concordance of US scans with CT scans and MR images. Radiology. 2007;242:162–74.
Jang HJ, Kim TK, Burns PN, et al. Enhancement patterns of hepatocellular carcinoma at contrast-enhanced US: comparison with histologic differentiation. Radiology. 2007;244:898–906.
Nicolau C, Vilana R, Catala V, et al. Importance of evaluating all vascular phases on contrast-enhanced sonography in the differentiation of benign from malignant focal liver lesions. AJR Am J Roentgenol. 2006;186:158–67.
Gaiani S, Celli N, Piscaglia F, et al. Usefulness of contrast-enhanced perfusional sonography in the assessment of hepatocellular carcinoma hypervascular at spiral computed tomography. J Hepatol. 2004;41:421–6.
Leen E, Ceccotti P, Kalogeropoulou C, et al. Prospective multicenter trial evaluating a novel method of characterizing focal liver lesions using contrast-enhanced sonography. AJR Am J Roentgenol. 2006;186:1551–9.
Wen YL, Kudo M, Zheng RQ, et al. Characterization of hepatic tumors: value of contrast-enhanced coded phase-inversion harmonic angio. AJR Am J Roentgenol. 2004;182:1019–26.
Nino-Murcia M, Olcott EW, Jeffrey RB, et al. Focal liver lesions: pattern-based classification scheme for enhancement at arterial phase CT. Radiology. 2000;215:746–51.
Lim JH, Kim CK, Lee WJ, et al. Detection of hepatocellular carcinomas and dysplastic nodules in cirrhotic livers: accuracy of helical CT in transplant patients. AJR Am J Roentgenol. 2000;175:693–8.
Valls C, Cos M, Figueras J, et al. Pretransplantation diagnosis and staging of hepatocellular carcinoma in patients with cirrhosis: value of dual-phase helical CT. AJR Am J Roentgenol. 2004;182:1011–7.
Yoon SH, Lee JM, So YH, et al. Multiphasic MDCT enhancement pattern of hepatocellular carcinoma smaller than 3 cm in diameter: tumor size and cellular differentiation. AJR Am J Roentgenol. 2009;193:482–9.
Jeong YY, Mitchell DG, Kamishima T. Small (<20 mm) enhancing hepatic nodules seen on arterial phase MR imaging of the cirrhotic liver: clinical implications. AJR Am J Roentgenol. 2002;178:1327–34.
Shimizu A, Ito K, Koike S, et al. Cirrhosis or chronic hepatitis: evaluation of small (≤2-cm) early-enhancing hepatic lesions with serial contrast-enhanced dynamic MR imaging. Radiology. 2003;226:550–5.
Burrel M, Llovet JM, Ayuso C, et al. MRI angiography is superior to helical CT for detection of HCC prior to liver transplantation: an explant correlation. Hepatology. 2003;38:1034–42.
Ito K, Fujita T, Shimizu A, et al. Multiarterial phase dynamic MRI of small early enhancing hepatic lesions in cirrhosis or chronic hepatitis: differentiating between hypervascular hepatocellular carcinomas and pseudolesions. AJR Am J Roentgenol. 2004;183:699–705.
Choi D, Mitchell DG, Verma SK, et al. Hepatocellular carcinoma with indeterminate or false-negative findings at initial MR imaging: effect on eligibility for curative treatment—initial observations. Radiology. 2007;244:776–83.
Kim SH, Kim SH, Lee J, et al. Gadoxetic acid-enhanced MRI versus triple-phase MDCT for the preoperative detection of hepatocellular carcinoma. AJR Am J Roentgenol. 2009;192:1675–81.
Sun YH, Lee JM, Shin CII, et al. Gadoxetic acid-enhanced magnetic resonance imaging for differentiating small hepatocellular carcinomas (≤2 cm in diameter) from arterial enhancing pseudolesions: special emphasis on hepatobiliary phase imaging. Invest Radiol. 2010;45:96–103.
Iwasaki M, Furuse J, Yoshino M, et al. Sonographic appearances of small hepatic nodules without tumor stain on contrast-enhanced computed tomography and angiography. J Clin Ultrasound. 1998;26:303–7.
Durand F, Regimbeau JM, Belghiti J, et al. Assessment of the benefits and risks of percutaneous biopsy before surgical resection of hepatocellular carcinoma. J Hepatol. 2001;35:254–8.
Ohto M, Kato H, Tsujii H, et al. Vascular flow patterns of hepatic tumors in contrast-enhanced 3-dimensional fusion ultrasonography using plane shift and opacity control modes. J Ultrasound Med. 2005;24:49–57.
Yukisawa S, Ohto M, Masuya Y, et al. Contrast-enhanced three-dimensional fusion sonography of small liver metastases with pathologic correlation. J Clin Ultrasound. 2007;35:1–8.
Luo W, Numata K, Morimoto M, et al. Three-dimensional contrast-enhanced sonography of vascular patterns of focal liver tumors: pilot study of visualization methods. AJR Am J Roentgenol. 2009;192:165–73.
Edey AJ, Ryan SM, Beese RC, et al. Ultrasound imaging of liver metastases in the delayed parenchymal phase following administration of Sonazoid using a destructive mode technique (agent detection imaging). Clin Radiol. 2008;63:1112–20.
Hatanaka K, Kudo M, Minami Y, et al. Differential diagnosis of hepatic tumors: value of contrast-enhanced harmonic sonography using the newly developed contrast agent, Sonazoid. Intervirology. 2008;51:61–9.
Numata K, Morimoto M, Ogura T, et al. Ablation therapy guided by contrast-enhanced sonography with Sonazoid for hepatocellular carcinoma lesions not detected by conventional sonography. J Ultrasound Med. 2008;27:395–406.
Luo W, Numata K, Morimoto M, et al. Focal liver tumors: characterization with 3D perflubutane microbubble contrast agent-enhanced US versus 3D contrast-enhanced multidetector CT. Radiology. 2009;251:287–95.
Luo W, Numata K, Morimoto M, et al. Clinical utility of contrast-enhanced three-dimensional ultrasound imaging with Sonazoid: findings on hepatocellular carcinoma lesions. Eur J Radiol. 2009;72:425–31.
International Consensus Group for Hepatocellular Neoplasia. Special article. Pathologic diagnosis of early hepatocellular carcinoma: a report of the International Consensus Group for Hepatocellular Neoplasia. Hepatology. 2009;49:658–64.
Kondo F. Histological features of early hepatocellular carcinomas and their developmental process: for daily practical clinical application: hepatocellular carcinoma. Hepatol Int. 2009;3:283–93.
Tsai TJ, Chau GY, Lui WY, et al. Clinical significance of microscopic tumor venous invasion in patients with resectable hepatocellular carcinoma. Surgery. 2000;127:603–8.
Utsunomiya T, Matsumata T, Adachi E, et al. Limitations of current preoperative liver imaging techniques for intrahepatic metastatic nodules of hepatocellular carcinoma. Hepatology. 1992;16:694–701.
Izumi R, Shimizu K, Ii T, et al. Prognostic factors of hepatocellular carcinoma in patients undergoing hepatic resection. Gastroenterology. 1994;106:720–7.
Lauwers GY, Terris B, Balis UJ, et al. Prognostic histologic indicators of curatively resected hepatocellular carcinomas. A multi-institutional analysis of 425 patients with definition of a histologic prognostic index. Am J Surg Pathol. 2002;26:25–34.
Sobin LH, Wittekind CH. International Union Against Cancer, TNM classification of malignant tumours, 6th ed. New York: Wiley-Liss; 2002. p. 82–5.
Kutami R, Nakashima Y, Nakashima O, et al. Pathomorphologic study on the mechanism of fatty change in small hepatocellular carcinoma of humans. J Hepatol. 2000;33:282–9.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Ohto, M., Ito, R., Soma, N. et al. Contrast-enhanced 3D ultrasonography in minute hepatocellular carcinoma. J Med Ultrasonics 38, 3–12 (2011). https://doi.org/10.1007/s10396-010-0283-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10396-010-0283-6