Abstract
Aim
Artificial Intelligence (AI) interventions in healthcare must be well-accepted and understood by physicians and medical practitioners before they are fully adopted for the patient’s well-being. AI-based diabetes diagnostic interventions can contribute to early diagnosis, accuracy and decision-making, providing a basis for disease prediction, determining the course of action for diabetes therapy and management. Keeping this in view, the current research builds on the technology acceptance model (TAM) to examine the physicians’ perceptions about AI-based diabetes diagnostic interventions and test their experience with the AI intervention as a moderator.
Subject and methods
Respondents were traced and engaged through online and offline surveys based on a questionnaire adapted from earlier research. Data (N = 202) were collected via purposive sampling from two states in India, which were then analysed using structured equation modelling.
Results
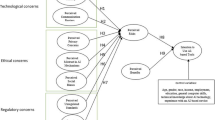
In comparison with other sectors, AI adoption in healthcare is increasing, but at the same time, AI-based diabetes diagnostic interventions among doctors are low. Our results show that perceived usefulness, perceived ease of use and subjective norms directly impact a doctor’s behavioural intention to use AI technologies. Moreover, perceived risk associated with AI technologies exerts a negative influence. Further, the study found that experience with AI tools positively moderates the relationship between perceived usefulness, perceived ease of use, perceived risk and behavioural intentions.
Conclusion
Most physicians, diabetologists and endocrinologists appear to be aware of the increasing application of AI-based diabetes diagnostic interventions but lack practical experience and related knowledge, leading to little or no adoption. Further education and hands-on training should be conducted to improve user experience.

Similar content being viewed by others
Data availability
The raw data supporting the conclusions of this article will be made available by the authors, without undue reservation.
References
Ajzen I, Fishbein M (1975) A Bayesian analysis of attribution processes. Psychol Bull 82(2):261. https://doi.org/10.1037/h0076477
Alamri MM, Almaiah MA, Al-Rahmi WM (2020) Social media applications affecting students’ academic performance: a model developed for sustainability in higher education. Sustainability 12(16):6471. https://doi.org/10.3390/su12166471
Alhashmi SF, Salloum SA, Mhamdi C (2019) Implementing artificial intelligence in the United Arab Emirates healthcare sector: an extended technology acceptance model. Int J Inform Technol Language Stud 3(3):27–42
Alkawsi G, Ali NA, Baashar Y (2021) The moderating role of personal innovativeness and users experience in accepting the smart meter technology. Appl Sci 11(8):3297. https://doi.org/10.3390/app11083297
Al-Qaysi N, Mohamad-Nordin N, Al-Emran M (2021) Developing a comprehensive theoretical model for adopting social media in higher education. Interact Learn Environ 31(7):1–22. https://doi.org/10.1080/10494820.2021.1961809
Bentler PM, Chou CP (1987) Practical issues in structural modeling. Sociol Methods Res 16(1):78–117. https://doi.org/10.1177/0049124187016001004
Bhattacherjee A, Premkumar G (2004) Understanding changes in belief and attitude toward information technology usage: a theoretical model and longitudinal test. MIS quarterly: 229–254. https://www.jstor.org/stable/25148634
Boon-itt S (2019) Quality of health websites and their influence on perceived usefulness, trust and intention to use: an analysis from Thailand. J Innov Entrepreneurship 8(4):1–18. https://doi.org/10.1186/s13731-018-0100-9
Castaneda JA, Munoz-Leiva F, Luque T (2007) Web acceptance model (WAM): moderating effects of user experience. Inform Manag 44(4):384–396. https://doi.org/10.1016/j.im.2007.02.003
Chau PY, Hu PJH (2002) Investigating healthcare professionals’ decisions to accept telemedicine technology: an empirical test of competing theories. Inform Manag 39(4):297–311. https://doi.org/10.1016/s0378-7206(01)00098-2
Chin WW (2000) Frequently Asked Questions – Partial Least Squares & PLS-Graph. Retrieved from http://disc-nt.cba.uh.edu/chin/plsfac/plsfac.htm
Chow YS, Teicher H (2012) Probability theory: independence, interchangeability, martingales. Springer Sci Business Media. https://doi.org/10.1007/978-1-4684-0062-5
Davis FD (1989) Perceived usefulness, perceived ease of use, and user acceptance of information technology. MIS Q 13(3):319. https://doi.org/10.2307/249008
Dishaw MT, Strong DM (1999) Extending the technology acceptance model with task–technology fit constructs. Inform Manag 36(1):9–21. https://doi.org/10.1016/S0378-7206(98)00101-3
Eberl M (2010) An application of PLS in multi-group analysis: the need for differentiated corporate level marketing in the mobile communications industry. In: Esposito Vinzi V, Chin W, Henseler J, Wang H (eds) Handbook of Partial Least Squares. Springer, Berlin, pp 487–514
Featherman MS, Pavlou PA (2003) Predicting e-services adoption: a perceived risk facets perspective. Int J Hum Comput Stud 59(4):451–474. https://doi.org/10.1016/S1071-5819(03)00111-3
Fenner BJ, Wong RL, Lam WC, Tan GS, Cheung GC (2018) Advances in retinal imaging and applications in diabetic retinopathy screening: a review. Ophthalmol Therapy 7:333–346. https://doi.org/10.1007/s40123-018-0153-7
Gibson SD (2003) The case for ‘risk awareness’. Secur J 16:55–64. https://doi.org/10.1057/PALGRAVE.SJ.8340140
Goodman JS, Blum TC (1996) Assessing the non-random sampling effects of subject attrition in longitudinal research. J Manag 22(4):627–652. https://doi.org/10.1016/S0149-2063(96)90027-6
Gupta S, Mittal R, Mittal A (2019) Modelling the intentions to adopt UPIs: a PLS-SEM approach. In 2019 6th International Conference on Computing for Sustainable Global Development (INDIACom) (pp 246–250). IEEE
Hair JF, Sarstedt M, Ringle CM, Mena JA (2012) An assessment of the use of partial least squares structural equation modeling in marketing research. J Acad Mark Sci 40(3):414–433. https://doi.org/10.1007/s11747-011-0261-6
Holden RJ, Karsh BT (2010) The technology acceptance model: its past and its future in health care. J Biomed Inform 43(1):159–172. https://doi.org/10.1016/j.jbi.2009.07.002
Hsieh PJ (2015) Physicians’ acceptance of electronic medical records exchange: an extension of the decomposed TPB model with institutional trust and perceived risk. In J Med Inform 84(1):1–14. https://doi.org/10.1016/j.ijmedinf.2014.08.008
Hua D, Petrina N, Young N, Cho JG, Poon SK (2024) Understanding the factors influencing acceptability of AI in medical imaging domains among healthcare professionals: a scoping review. Artificial Intell Med 147. https://doi.org/10.1016/j.artmed.2023.102698
Hyde MK, White KM (2009) To be a donor or not to be? Applying an extended theory of planned behavior to predict posthumous organ donation intentions. J Appl Soc Psychol 39(4):880–900. https://doi.org/10.1111/j.1559-1816.2009.00464.x
Jamwal M, Kanojia H, Dhiman N (2023) What motivates users to continually use wearable medical devices? Evidence from a developing nation. Int J Pharmaceut Healthcare Market 18(1):47–66. https://doi.org/10.1108/IJPHM-11-2022-0097
Kasaye MD, Mengestie ND, Beyene S, Kebede N, Ngusie HS, Kalayou MH (2023) Acceptance of electronic medical records and associated factor among physicians working in University of Gondar comprehensive specialized hospital: a cross-sectional study. Digital Health 9. https://doi.org/10.1177/20552076231213445
Ketikidis P, Dimitrovski T, Lazuras L, Bath PA (2012) Acceptance of health information technology in health professionals: an application of the revised technology acceptance model. Health Informatics J 18(2):124–134. https://doi.org/10.1177/1460458211435425
Kleine AK, Kokje E, Lermer E, Gaube S (2023) Attitudes toward the adoption of 2 artificial intelligence–enabled mental health tools among prospective psychotherapists: cross-sectional study. JMIR Human Factors 10. https://doi.org/10.2196/46859
Kooli C, Al Muftah H (2022) Artificial intelligence in healthcare: a comprehensive review of its ethical concerns. Technol Sustainab 1(2):121–131. https://doi.org/10.1108/TECHS-12-2021-0029
Leigh S, Ashall-Payne L, Andrews T (2020) Barriers and facilitators to the adoption of mobile health among health care professionals from the United Kingdom: discrete choice experiment. JMIR mHealth and uHealth 8(7). https://doi.org/10.2196/17704
Lemay DJ, Doleck T, Bazelais P (2017) “Passion and concern for privacy” as factors affecting snapchat use: a situated perspective on technology acceptance. Comput Hum Behav 75:264–271. https://doi.org/10.1016/j.chb.2017.05.022
Makroum MA, Adda M, Bouzouane A, Ibrahim H (2022) Machine learning and smart devices for diabetes management: systematic review. Sensors 22(5):1843. https://doi.org/10.3390/s22051843
Martins C, Oliveira T, Popovič A (2014) Understanding the internet banking adoption: a unified theory of acceptance and use of technology and perceived risk application. Int J Inf Manage 34(1):1–13. https://doi.org/10.1016/j.ijinfomgt.2013.06.002
McLean G, Osei-Frimpong K (2019) Chat now… Examining the variables influencing the use of online live chat. Technol Forecast Soc Chang 146:55–67. https://doi.org/10.1016/j.techfore.2019.05.017
Miao R, Wu Q, Wang Z, Zhang X, Song Y, Zhang H, Sun Q, Jiang Z (2017) Factors that influence users’ adoption intention of mobile health: a structural equation modeling approach. Int J Prod Res 55(19):5801–5815. https://doi.org/10.1080/00207543.2017.1336681
Mishra AN, Anderson C, Angst CM, Agarwal R (2012) Electronic health records assimilation and physician identity evolution: an identity theory perspective. Inf Syst Res 23(3):738–760. https://doi.org/10.1287/isre.1110.0407
Mittal A, Mantri A, Tandon U, Dwivedi YK (2022) A unified perspective on the adoption of online teaching in higher education during the COVID-19 pandemic. Inform Discov Delivery 50(2):117–132. https://doi.org/10.1108/IDD-09-2020-0114
Moores TT (2012) Towards an integrated model of IT acceptance in healthcare. Decis Support Syst 53(3):507–516. https://doi.org/10.1016/j.dss.2012.04.014
Neuman WL (2009) Social research methods: qualitative and quantitative approaches, 7th edn. Pearson/Allyn & Bacon, Boston
Pan J, Ding S, Wu D, Yang S, Yang J (2019) Exploring behavioural intentions toward smart healthcare services among medical practitioners: a technology transfer perspective. Int J Prod Res 57(18):5801–5820. https://doi.org/10.1080/00207543.2018.1550272
Podsakoff PM, MacKenzie SB, Podsakoff NP (2012) Sources of method bias in social science research and recommendations on how to control it. Annu Rev Psychol 63:539–569. https://doi.org/10.1146/annurev-psych-120710-100452
Rago CAP, Zucchi P (2020) Can Ease of Use and Usefulness perception be influenced by physicians characteristics in the adoption of technology innovations?. Int J Innov Educ Res 8(10): 87–93. https://doi.org/10.31686/ijier.vol8.iss10.2660
Rahimi B, Nadri H, Lotfnezhad H, Timpka T (2018) A systematic review of the technology acceptance model in health informatics. Appl Clin Inform 9(3):604–634. https://doi.org/10.1055/s-0038-1668091
Rho MJ, Young Choi I, Lee J (2014) Predictive factors of telemedicine service acceptance and behavioral intention of physicians. Int J Med Informatics 83(8):559–571. https://doi.org/10.1016/j.ijmedinf.2014.05.005
Rouidi M, Elouadi A, Hamdoune A (2022) Acceptance and use of telemedicine technology by health professionals: development of a conceptual model. Digital Health 8. https://doi.org/10.1177/20552076221081693
Schaupp LC, Carter L, McBride ME (2010) E-file adoption: a study of US taxpayers’ intentions. Comput Hum Behav 26(4):636–644. https://doi.org/10.1016/j.chb.2009.12.017
Soodan V, Jamwal M, Rana NP, Sharma D, Chakraborty S (2023) Modelling the adoption of agro-advisory mobile applications: a theoretical extension and analysis using result demonstrability, trust, self-efficacy and mobile usage proficiency. J Agribusiness Dev Emerg Econ.https://doi.org/10.1108/JADEE-05-2022-0087
Sykes TA, Venkatesh V, Gosain S (2009) Model of acceptance with peer support: a social network perspective to understand employees' system use. MIS quarterly 371–393. https://www.jstor.org/stable/20650296
Taherdoost H (2019) Importance of Technology Acceptance Assessment for Successful Implementation and Development of New Technologies. Glob J Eng Sci 1(3). https://doi.org/10.33552/gjes.2019.01.000511
Tran AQ, Nguyen LH, Nguyen HAS, Nguyen, CT, Vu LG, Zhang M, Vu TMT, Nguyen SH, Xuan Tran BX, Latkin CA, Ho RCM, Ho CS (2021) Determinants of intention to use artificial intelligence-based diagnosis support system among prospective physicians. Front Public Health 9. https://doi.org/10.3389/fpubh.2021.755644
Tubaishat A (2018) Perceived usefulness and perceived ease of use of electronic health records among nurses: application of technology acceptance model. Inform Health Soc Care 43(4):379–389. https://doi.org/10.1080/17538157.2017.1363761
Venkatesh V, Morris MG, Davis GB, Davis FD (2003) User acceptance of information technology: Toward a unified view. MIS Quart 425–478. https://doi.org/10.2307/30036540
Venkatesh V, Thong JY, Xu X (2012) Consumer acceptance and use of information technology: extending the unified theory of acceptance and use of technology. MIS Quart 157–178. https://doi.org/10.2307/41410412
Verma B, Tandon U (2022) Modelling barriers to wearable technologies in Indian context: validating the moderating role of technology literacy. Glob Knowledge, Memory Communhttps://doi.org/10.1108/GKMC-08-2022-0209
Weiss L, Johar GV (2013) Egocentric categorization and product judgment: seeing your traits in what you own (and their opposite in what you don’t). J Consumer Res 40(1):185–201. https://doi.org/10.1086/669330
Acknowledgements
This paper and the research behind it would not have been possible without the exceptional support of my earlier supervisor, Dr Savdeep Vasudeva and my current supervisor, Dr Maninder Singh and Co-Supervisor Dr Mohit Jamwal. All their enthusiasm, knowledge and exacting attention to detail have been an inspiration and kept my work on track for my research paper as a PhD scholar. Finally, I would like to thank everyone at Mittal School of Business, Lovely Faculty of Business and Arts, and Lovely Professional University for successfully pursuing my PhD in Operations Management.
Funding
The authors declare that this research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
Mrinmoy Roy: Conceptualized the study, developed the theoretical framework, conducted the primary literature review, designed the methodology, analysed the data, and drafted the manuscript.
Mohit Jamwal: Was responsible for data curation, assisted with statistical analysis of the results, and contributed to manuscript revisions.
Savdeep Vasudeva: Supervised the project, provided resources, and critically reviewed and edited the manuscript.
Maninder Singh: Assisted in drafting the final manuscript, and revised it based on feedback.
Corresponding author
Ethics declarations
Ethics statement
The authors confirm that this study did not involve human or animal subjects or tissue.
Consent to participate
The authors declare that the research or manuscript does not report on or involve any animals, humans, human data, human tissue or plants.
Consent for publication
The authors declare that the research or manuscript does not contain any individual person’s data.
Conflict of interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Roy, M., Jamwal, M., Vasudeva, S. et al. Physicians behavioural intentions towards AI-based diabetes diagnostic interventions in India. J Public Health (Berl.) (2024). https://doi.org/10.1007/s10389-024-02235-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10389-024-02235-w