Abstract
Aim
This study assesses the impact of a community-based intervention package delivered through community lady health workers (LHWs) to improve early postpartum and newborn care practices.
Methods
A cluster randomized controlled trial was carried out in Sukkur, Sindh Province, Pakistan. We conducted a baseline survey and delivered an enhanced postpartum care package through the existing LHW cadre to the intervention clusters.
Results
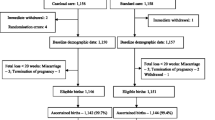
Thirty clusters were randomly assigned to the intervention and control groups. A total of 3999 women in the intervention group and 3234 women in the control group were enrolled. During the study period, there were 1296 births in the intervention arm and 1326 in the control arm. Compared with the control group, the intervention group showed a significant improvement in the number of women receiving antenatal care (p = 0.001), fewer home deliveries (p = 0.022), increased number of deliveries by skilled birth attendants (p = 0.005), and more participation in care-seeking practices during the postpartum period (p = 0.023). Similarly, hygienic cord-cutting (p = 0.014) and a cord clamp (p = 0.049) were prevalent in the intervention group. Moreover, the intervention group had more visits by LHWs during pregnancy and in the postpartum period.
Conclusion
The use of maternal and neonatal intervention packages through trained community LHWs within the existing health system has the potential to improve maternal, perinatal and neonatal care practices, particularly in low-resource settings where home deliveries still occur.

Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Code availability
SPSS v.14 was used for data anlysis.
References
Agarwal S, Curtis SL, Angeles G, Speizer IS, Singh K, Thomas JC (2019) The impact of India’s accredited social health activist (ASHA) program on the utilization of maternity services: a nationally representative longitudinal modelling study. Human Resour Health 17(1):68. https://doi.org/10.1186/s12960-019-0402-4
Ariff S, Soofi SB, Sadiq K, Feroze AB, Khan S, Jafarey SN, Ali N, Bhutta ZA (2010) Evaluation of health workforce competence in maternal and neonatal issues in public health sector of Pakistan: an assessment of their training needs. BMC Health Serv Res 10(1):319. https://doi.org/10.1186/1472-6963-10-319
Ariff S, Mir F, Tabassum F, Raza F, Habib A, Turab A, LeFevre A, Bartlett LA, Soofi SB, Bhutta ZA (2020) Determinants of health care seeking behaviors in puerperal sepsis in rural Sindh, Pakistan: a qualitative study. Open J Prev Med 10(9):9. https://doi.org/10.4236/ojpm.2020.109018
Ayaz A, Saleem S (2010) Neonatal mortality and prevalence of practices for newborn care in a squatter settlement of Karachi, Pakistan: a cross-sectional study. PLOS ONE 5(11):e13783. https://doi.org/10.1371/journal.pone.0013783
Bhutta ZA, Lassi ZS (2010) Empowering communities for maternal and newborn health. Lancet (London, England) 375(9721):1142–1144. https://doi.org/10.1016/S0140-6736(10)60324-8
Bhutta ZA, Memon ZA, Soofi S, Salat MS, Cousens S, Martines J (2008) Implementing community-based perinatal care: results from a pilot study in rural Pakistan. Bull World Health Organization 86(6):452–459. https://doi.org/10.2471/BLT.07.045849
Bhutta ZA, Das JK, Bahl R, Lawn JE, Salam RA, Paul VK, Sankar MJ, Blencowe H, Rizvi A, Chou VB, Walker N, Lancet Newborn Interventions Review Group, Lancet Every Newborn Study Group (2014) Can available interventions end preventable deaths in mothers, newborn babies, and stillbirths, and at what cost? Lancet (London, England) 384(9940):347–370. https://doi.org/10.1016/S0140-6736(14)60792-3
Blencowe H, Cousens S, Mullany LC, Lee AC, Kerber K, Wall S, Darmstadt GL, Lawn JE (2011) Clean birth and postnatal care practices to reduce neonatal deaths from sepsis and tetanus: a systematic review and Delphi estimation of mortality effect. BMC Public Health 11(3):S11. https://doi.org/10.1186/1471-2458-11-S3-S11
Darmstadt GL, Choi Y, Arifeen SE, Bari S, Rahman SM, Mannan I, Seraji HR, Winch PJ, Saha SK, ASMNU A, Ahmed S, Begum N, ACC L, Black RE, Santosham M, Crook D, Baqui AH, Study Group for the BP2 (Mirzapur) (2010) Evaluation of a cluster-randomized controlled trial of a package of community-based maternal and newborn interventions in Mirzapur, Bangladesh. PLOS ONE 5(3):e9696. https://doi.org/10.1371/journal.pone.0009696
Geldsetzer P, Mboggo E, Larson E, Lema IA, Magesa L, Machumi L, Ulenga N, Sando D, Mwanyika-Sando M, Spiegelman D, Mungure E, Li N, Siril H, Mujinja P, Naburi H, Chalamilla G, Kilewo C, Ekström AM, Foster D et al (2019) Community health workers to improve uptake of maternal healthcare services: a cluster-randomized pragmatic trial in Dar es Salaam, Tanzania. PLoS Med 16(3):e1002768. https://doi.org/10.1371/journal.pmed.1002768
Gogia S, Sachdev HS (2010) Home visits by community health workers to prevent neonatal deaths in developing countries: a systematic review. Bull World Health Organ 88(9):658–666B. https://doi.org/10.2471/BLT.09.069369
Gogia S, Sachdev HPS (2016) Home-based neonatal care by community health workers for preventing mortality in neonates in low- and middle-income countries: a systematic review. J Perinatol 36(Suppl 1(Suppl 1)):S55–S73. https://doi.org/10.1038/jp.2016.33
Government of Pakistan Ministry of Health (2010) National Program for Family Planning and Primary Health Care; The-Lady-Health-Workers-Programme, January 2010 June 2015. https://scorecard.prb.org/wp-content/uploads/2018/05/National-Program-for-Family-Planning-and-Primary-Health-Care-%E2%80%9CThe-Lady-Health-Workers-Programme%E2%80%9C-January-2010-June-2015.Sindh-Pakistan.pdf. Accessed 22 November 2022
Haider R, Ashworth A, Kabir I, Huttly SR (2000) Effect of community-based peer counsellors on exclusive breastfeeding practices in Dhaka, Bangladesh: a randomised controlled trial. Lancet (London, England) 356(9242):1643–1647. https://doi.org/10.1016/s0140-6736(00)03159-7
Hayes RJ, Bennett S (1999) Simple sample size calculation for cluster-randomized trials. Int J Epidemiol 28(2):319–326. https://doi.org/10.1093/ije/28.2.319
Jacobs C, Michelo C, Chola M, Oliphant N, Halwiindi H, Maswenyeho S, Baboo KS, Moshabela M (2018) Evaluation of a community-based intervention to improve maternal and neonatal health service coverage in the most rural and remote districts of Zambia. PloS One 13(1):e0190145. https://doi.org/10.1371/journal.pone.0190145
Kassebaum NJ, Bertozzi-Villa A, Coggeshall MS, Shackelford KA, Steiner C, Heuton KR, Gonzalez-Medina D, Barber R, Huynh C, Dicker D, Templin T, Wolock TM, Ozgoren AA, Abd-Allah F, Abera SF, Abubakar I, Achoki T, Adelekan A, Ademi Z et al (2014) Global, regional, and national levels and causes of maternal mortality during 1990–2013: a systematic analysis for the Global Burden of Disease Study 2013. The Lancet 384(9947):980–1004. https://doi.org/10.1016/S0140-6736(14)60696-6
Kirkwood BR, Manu A, AHAt A, Soremekun S, Weobong B, Gyan T, Danso S, Amenga-Etego S, Tawiah-Agyemang C, Owusu-Agyei S, Hill Z (2013) Effect of the Newhints home-visits intervention on neonatal mortality rate and care practices in Ghana: a cluster randomised controlled trial. Lancet (London, England) 381(9884):2184–2192. https://doi.org/10.1016/S0140-6736(13)60095-1
Lawn JE, Cousens S, Zupan J, Lancet Neonatal Survival Steering Team (2005) 4 million neonatal deaths: When? Where? Why? Lancet (London, England) 365(9462):891–900. https://doi.org/10.1016/S0140-6736(05)71048-5
Li XF, Fortney JA, Kotelchuck M, Glover LH (1996) The postpartum period: the key to maternal mortality. Int J Gynecol Obstet 54(1):1–10. https://doi.org/10.1016/0020-7292(96)02667-7
Liu L, Oza S, Hogan D, Chu Y, Perin J, Zhu J, Lawn JE, Cousens S, Mathers C, Black RE (2016) Global, regional, and national causes of under-5 mortality in 2000–15: an updated systematic analysis with implications for the Sustainable Development Goals. The Lancet 388(10063):3027–3035. https://doi.org/10.1016/S0140-6736(16)31593-8
Lunze K, Higgins-Steele A, Simen-Kapeu A, Vesel L, Kim J, Dickson K (2015) Innovative approaches for improving maternal and newborn health-a landscape analysis. BMC Preg Childbirth 15(1):337. https://doi.org/10.1186/s12884-015-0784-9
McConnell M, Ettenger A, Rothschild CW, Muigai F, Cohen J (2016) Can a community health worker administered postnatal checklist increase health-seeking behaviors and knowledge? Evidence from a randomized trial with a private maternity facility in Kiambu County, Kenya. BMC Preg Childbirth 16(1):136. https://doi.org/10.1186/s12884-016-0914-z
National Institute of Population Studies (NIPS) Pakistan, ICF (2019) Pakistan Demographic and Health Survey 2017-18. The DHS Program; Demographic and Health Surveys. https://dhsprogram.com/publications/publication-fr354-dhs-final-reports.cfm. Accessed 2 December 2022
National Institute of Population Studies (NIPS) Pakistan, ICF (2020) Pakistan Maternal Mortality Survey Summary Report 2019. The DHS Program; Demographic and Health Surveys. https://dhsprogram.com/pubs/pdf/PR128/PR128.pdf. Accessed 2 December 2022
Oxford Policy Management (2009) Lady Health Worker Programme: External evaluation of a national programme for family planning and primary health care. https://www.opml.co.uk/files/Publications/6241-evaluating-lady-health-worker-programme/lhw-4th-evaluation-summary-of-results.pdf?noredirect=1. Accessed 25 November 2022
Pakistan Bureau of Statistics (2021) Final district wise results of 6th population and housing census 2017. https://www.pbs.gov.pk/sites/default/files/population/2017/results/08201.pdf. Accessed 25 November 2022
Say L, Chou D, Gemmill A, Tunçalp Ö, Moller AB, Daniels J, Gülmezoglu AM, Temmerman M, Alkema L (2014) Global causes of maternal death: a WHO systematic analysis. Lancet Global Health 2(6):e323–e333. https://doi.org/10.1016/S2214-109X(14)70227-X
Shah R, Munos MK, Winch PJ, Mullany LC, Mannan I, Rahman SM, Rahman R, Hossain D, Arifeen SE, Baqui AH (2010) Community-based health workers achieve high coverage in neonatal intervention trials: a case study from Sylhet, Bangladesh. J Health, Population, Nutr 28(6):610–618. https://doi.org/10.3329/jhpn.v28i6.6610
Sharma S, Teijlingen EV, Belizán JM, Hundley V, Simkhada P, Sicuri E (2016) Measuring what works: an impact evaluation of Women’s groups on maternal health uptake in rural Nepal. PLOS ONE 11(5):e0155144. https://doi.org/10.1371/journal.pone.0155144
Tripathy P, Nair N, Barnett S, Mahapatra R, Borghi J, Rath S, Rath S, Gope R, Mahto D, Sinha R, Lakshminarayana R, Patel V, Pagel C, Prost A, Costello A (2010) Effect of a participatory intervention with women’s groups on birth outcomes and maternal depression in Jharkhand and Orissa, India: a cluster-randomised controlled trial. Lancet (London, England) 375(9721):1182–1192. https://doi.org/10.1016/S0140-6736(09)62042-0
UN IGME (2014) Levels and trends in child mortality 2014; Estimates developed by the UN inter-agency Group for Child Mortality Estimation. UNICEF Data: Monitoring the situation of children and women. https://data.unicef.org/resources/levels-trends-child-mortality-report-2014/. Accessed 2 December 2022
UN IGME (2020) Mortality rate, neonatal (Pakistan). The World Bank. https://data.worldbank.org/indicator/SH.DYN.NMRT?locations=PK. Accessed 2 December 2022
UNICEF (2021) Levels & trends in child mortality; Report 2021 Estimates developed by the UN Inter-agency Group for Child Mortality Estimation. https://childmortality.org/wp-content/uploads/2021/12/UNICEF-2021-Child-Mortality-Report.pdf. Accessed 22 November 2022
USAID (2014) Pakistan Emergency Situational Analysis—District Sukkur.OCHA Services reliefweb. https://reliefweb.int/report/pakistan/pakistan-emergency-situational-analysis-district-sukkur-september-2014. Accessed 2 December 2022
WHO (2012) WHO recommendations; Optimizing health worker roles to improve access to key maternal and newborn health interventions through task shifting. World Health Organization, institutional repository for information sharing. https://apps.who.int/iris/handle/10665/77764. Accessed 2 December 2022
WHO (2016) WHO recommendations on antenatal care for a positive pregnancy experience. World Health Organization, Geneva http://www.ncbi.nlm.nih.gov/books/NBK409108/. Accessed 2 December 2022
WHO (2019) Maternal mortality. World Health Organization. https://www.who.int/news-room/fact-sheets/detail/maternal-mortality. Accessed 8 December 2022
WHO (2020) WHO recommendations for the prevention and treatment of postpartum haemorrhage. World Health Organization, Publications. https://www.who.int/publications-detail-redirect/9789241548502. Accessed 12 December 2022
WHO, UNICEF, United Nations Fund for Population Activities (2015) Pregnancy, childbirth, postpartum and newborn care: A guide for essential practice (3rd edition). World Health Organization publications. https://www.who.int/publications/i/item/9789241549356. Accessed 10 Dec 2022
WHO, World Bank, United Nations Population Fund, UNICEF (2015) Trends in maternal mortality: 1990-2015: estimates from WHO, UNICEF, UNFPA, World Bank Group and the United Nations Population Division. World Health Organization, institutional repository for information sharing. https://apps.who.int/iris/handle/10665/194254. Accessed 22 Nov 2022
Wilunda C, Tanaka S, Putoto G, Tsegaye A, Kawakami K (2016) Evaluation of a maternal health care project in Southwest Shoa Zone, Ethiopia: before-and-after comparison. Reprod Health 13:95. https://doi.org/10.1186/s12978-016-0213-1
Acknowledgements
We would like to thank the Aga Khan University, Pakistan, for supporting this study. We are also immensely grateful to all participants for their cooperation during the study.
Funding
This study was funded by PAIMAN (Pakistan Initiative for Mothers and Newborns) and John Snow Inc, via a grant from the US Agency for International Development (USAID; Award Number: 36098-01, cooperative agreement number 391-A-00-05-01037-00).
Author information
Authors and Affiliations
Contributions
ZAB conceptualized the study, provided technical supervision. SA and SBS designed the study, developed the sampling strategy, assisted with interpreting the results, and reviewed the manuscript. MB, AK and SA drafted the manuscript. MS and AR were involved in data management and analysis. SK, MU and IA critically reviewed the manuscript. All authors reviewed and approved the final manuscript for submission.
Corresponding author
Ethics declarations
Ethics approval
The study was approved by the Ethical Review Committee of the Aga Khan University, Pakistan (770-Ped/ERC-06). This trial was registered at ClinicalTrial.gov. ID: NCT01389219, dated 01 October 2007.
Informed consent
Informed written consent was obtained from all individual participants included in the study.
Consent for publication
Not Applicable
Confidentiality
The confidentiality of the data collected during this study was guaranteed.
Conflicts of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ariff, S., Soofi, S.B., Bhura, M. et al. Impact of a community-based intervention package delivered through community health workers on post-partum care practices: a cluster randomized controlled trial. J Public Health (Berl.) (2023). https://doi.org/10.1007/s10389-023-01955-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10389-023-01955-9