Abstract
Background
Occupation is a major determinant of health outcomes. Healthcare workers are assumed to know how to prevent diseases and live a healthy life. The aim of this study is to determine the association between working in healthcare as a pre-retirement occupation and health outcomes after retirement.
Method
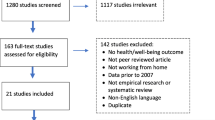
This cross-sectional study was conducted among 4813 members of the National Pensioners Association in Ghana. Thirteen study centres were used in the study.
Results
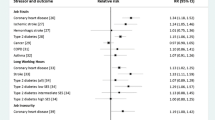
A total of 403 study participants (8.4%) were healthcare workers. After retirement, healthcare workers died earlier compared to non-healthcare workers. Life-table analysis of data demonstrated that 51.9% (95% CI = 47.1–56.9) of health workers died within 5 years after retirement, compared to 35.9% (95% CI = 34.5–37.4) of non-healthcare workers within same time period. Healthcare workers had a significantly higher prevalence of obesity (34.0, 95% CI = 29.5–38.8), self-reported hypertension (54.8%, 95% CI = 49.9–59.7) and high serum total cholesterol (46.4%, 95% CI = 48.7–58.5) compared to non-health workers. Logistic regression of factors on health outcomes after retirement among healthcare workers revealed that healthcare workers were nearly twice as likely to have arthritis (AOR = 1.6, 95% CI = 1.2–2.1), hearing loss (AOR = 2.0, 95% CI = 1.2–3.1), ischaemic heart disease (AOR = 2.0, 95% CI = 1.2–3.3), and cerebrovascular accident (AOR = 2.1, 95% CI = 1.1–4.0) compared to non-healthcare workers.
Conclusion
Retired healthcare workers die earlier after retirement and have a higher prevalence of non-communicable disease and its risk factors compared to non-healthcare workers. It is imperative to put in place measures to ensure individual health workers and occupational health teams develop innovative ways to care for themselves.

Similar content being viewed by others
Availability of data and materials
The datasets generated during and analysed during the current study are available from the corresponding author on reasonable request.
References
Allorto NL, Zoepke S, Clarke DL, Rode H (2016) Burn surgeons in South Africa: a rare species. S Afr Med J 106:186–188. https://doi.org/10.7196/SAMJ.2016.v106i2.9954
Aluko OO, Adebayo AE, Adebisi TF et al (2016) Knowledge, attitudes and perceptions of occupational hazards and safety practices in Nigerian healthcare workers. BMC Res Notes 9:71. https://doi.org/10.1186/s13104-016-1880-2
Andreassi MG, Piccaluga E, Guagliumi G et al (2016) Occupational health risks in cardiac catheterization laboratory workers. Circ Cardiovasc Interv 9:e003273. https://doi.org/10.1161/CIRCINTERVENTIONS.115.003273
Auta A, Adewuyi EO, Tor-Anyiin A et al (2018) Global prevalence of percutaneous injuries among healthcare workers: a systematic review and meta-analysis. Int J Epidemiol 47:1972–1980. https://doi.org/10.1093/ije/dyy208
Beard JR, Officer A, de Carvalho IA et al (2016) The World report on ageing and health: a policy framework for healthy ageing. Lancet 387:2145–2154. https://doi.org/10.1016/S0140-6736(15)00516-4
Bianchi R, Schonfeld IS, Laurent E (2015) Burnout–depression overlap: a review. Clin Psychol Rev 36:28–41. https://doi.org/10.1016/J.CPR.2015.01.004
Boutayeb A, Boutayeb S, Boutayeb W (2013) Multi-morbidity of non communicable diseases and equity in WHO eastern Mediterranean countries. Int J Equity Health 12:60. https://doi.org/10.1186/1475-9276-12-60
Chatterji S, Byles J, Cutler D et al (2015) Health, functioning, and disability in older adults—present status and future implications. Lancet (Lond Engl) 385:563–575. https://doi.org/10.1016/S0140-6736(14)61462-8
Clegg A, Young J, Iliffe S et al (2013) Frailty in elderly people. Lancet 381:752–762. https://doi.org/10.1016/S0140-6736(12)62167-9
Coppola N, De Pascalis S, Onorato L et al (2016) Hepatitis B virus and hepatitis C virus infection in healthcare workers. World J Hepatol 8:273–281. https://doi.org/10.4254/wjh.v8.i5.273
Crimmins EM, Beltran-Sanchez H (2011) Mortality and morbidity trends: is there compression of morbidity? J Gerontol Ser B Psychol Sci Soc Sci 66B:75–86. https://doi.org/10.1093/geronb/gbq088
das Merces MC, E Silva D de S, Lua I et al (2016) Burnout syndrome and abdominal adiposity among primary health care nursing professionals. Psicol Refl Crít 29:44. https://doi.org/10.1186/s41155-016-0051-7
Embriaco N, Papazian L, Kentish-Barnes N et al (2007) Burnout syndrome among critical care healthcare workers. Curr Opin Crit Care 13:482–488. https://doi.org/10.1097/MCC.0b013e3282efd28a
Fabbri E, Zoli M, Gonzalez-Freire M et al (2015) Aging and multimorbidity: new tasks, priorities, and frontiers for integrated gerontological and clinical research. J Am Med Dir Assoc 16:640–647. https://doi.org/10.1016/J.JAMDA.2015.03.013
Fitzpatrick MD, Moore TJ (2018) The mortality effects of retirement: evidence from social security eligibility at age 62. J Public Econ 157:121–137. https://doi.org/10.1016/J.JPUBECO.2017.12.001
Fujishiro K, Xu J, Gong F (2010) What does “occupation” represent as an indicator of socioeconomic status?: exploring occupational prestige and health. Soc Sci Med 71:2100–2107. https://doi.org/10.1016/J.SOCSCIMED.2010.09.026
He W, Goodkind D, Kowal P (2016) An aging world: 2015. US Census Bureau, Washington, DC
Kunna R, San Sebastian M, Stewart Williams J (2017) Measurement and decomposition of socioeconomic inequality in single and multimorbidity in older adults in China and Ghana: results from the WHO study on global AGEing and adult health (SAGE). Int J Equity Health 16:79. https://doi.org/10.1186/s12939-017-0578-y
Marengoni A, Angleman S, Melis R et al (2011) Aging with multimorbidity: a systematic review of the literature. Ageing Res Rev 10:430–439. https://doi.org/10.1016/J.ARR.2011.03.003
Minicuci N, Biritwum RB, Mensah G et al (2014) Sociodemographic and socioeconomic patterns of chronic non-communicable disease among the older adult population in Ghana. Glob Health Action 7:21292. https://doi.org/10.3402/gha.v7.21292
Mohanty A, Kabi A, Mohanty AP (2019) Health problems in healthcare workers: a review. J Fam Med Prim Care 8:2568–2572. https://doi.org/10.4103/jfmpc.jfmpc_431_19
Morrissey SP, Johnson JE (2017) The retirement readiness crisis in healthcare: crisis calls for customized benefits. J Econ Bank 3. https://doi.org/10.18103/jeb.v3i3.1481
Ndejjo R, Musinguzi G, Yu X et al (2015) Occupational health hazards among healthcare workers in Kampala, Uganda. J Environ Public Health 2015:1–9. https://doi.org/10.1155/2015/913741
Nuertey BD, Alhassan AI, Nuertey AD et al (2017) Prevalence of obesity and overweight and its associated factors among registered pensioners in Ghana; a cross sectional studies. BMC Obes 4:26
O’Neill J, Tabish H, Welch V et al (2014) Applying an equity lens to interventions: using PROGRESS ensures consideration of socially stratifying factors to illuminate inequities in health. J Clin Epidemiol 67:56–64. https://doi.org/10.1016/J.JCLINEPI.2013.08.005
Sorour AS, El-Maksoud MMA (2012) Relationship between musculoskeletal disorders, job demands, and burnout among emergency nurses. Adv Emerg Nurs J 34:272–282. https://doi.org/10.1097/TME.0b013e31826211e1
Taulbut AM, McCartney G (2011) Health outcomes and determinants by occupation and industry in Scotland, 2008–2011. Public Health Scotland, Edinburgh
World Health Organization (2017) Global action plan on the public health response to dementia 2017–2025. World Health Organisation, Geneva
Wyse CA, Celis Morales CA, Graham N et al (2017) Adverse metabolic and mental health outcomes associated with shiftwork in a population-based study of 277,168 workers in UK biobank. Ann Med 49:411–420. https://doi.org/10.1080/07853890.2017.1292045
Funding
No funding was received to assist with the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Benjamin D. Nuertey and Joyce Addai. The first draft of the manuscript was written by Benjamin D. Nuertey and Joyce Addai, and all authors made significant intellectual input to previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The study protocol was reviewed and approved by the National Pensioners’ Association Board. The board further monitored each step of the data collection process.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent to publish
Not applicable.
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest or non-financial interest in the subject matter or materials discussed in this manuscript.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nuertey, B.D., Udofia, E.A., Yawson, A.E. et al. Health outcomes following retirement: a comparative study of health and non-health pensioners in Ghana. J Public Health (Berl.) 30, 1641–1650 (2022). https://doi.org/10.1007/s10389-021-01557-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10389-021-01557-3