Abstract
Aim
Asian Americans have high levels of undiagnosed diabetes, but little is known about what influences diabetes screening in this group. We determined which sociodemographic, socioeconomic, and clinical factors were associated with diabetes screening in the American Diabetes Association’s (ADA) recommended screening groups for Asian Americans.
Subjects and methods
We included Asian Americans from the 2015 and 2017 Behavioral Risk Factor Surveillance System who fit the ADA’s diabetes screening guidelines and responded to a diabetes screening question. Logistic regression models were created to examine associations between sociodemographic, socioeconomic, and clinical factors and diabetes screening in Asian Americans.
Results
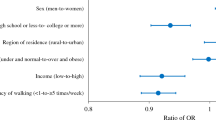
Being a college graduate and having high blood pressure were associated with higher levels of diabetes screening for the two screening groups. A trend of decreased diabetes screening with less educational attainment was observed in both screening groups.
Conclusion
Diabetes screening in Asian Americans is influenced by socioeconomic and clinical factors. Additional work is needed to identify other Asian American-specific cultural factors that may have an impact on the decision to seek diabetes screening.
Similar content being viewed by others
References
Agardh EE, Sidorchuk A, Hallqvist J et al (2011) Burden of type 2 diabetes attributed to lower educational levels in Sweden. Popul Health Metr 9:60. https://doi.org/10.1186/1478-7954-9-60
American Diabetes Association (ADA) (2014) American Diabetes Association Releases Position Statement on New BMI Screening Cut Points for Diabetes in Asian Americans
American Diabetes Association (ADA) (2019) Complications. https://www.diabetes.org/diabetes/complications.
Andresen EM, Catlin TK, Wyrwich KW, Jackson-Thompson J (2003) Retest reliability of surveillance questions on health related quality of life. J Epidemiol Community Health 57:339–343. https://doi.org/10.1136/jech.57.5.339
Araneta MR, Kanaya AM, Hsu WC et al (2015) Optimum BMI cut points to screen Asian Americans for type 2 diabetes. Diabetes Care 38:814–820. https://doi.org/10.2337/dc14-2071
Arnetz L, Ekberg NR, Alvarsson M (2014) Sex differences in type 2 diabetes: focus on disease course and outcomes. Diabetes Metab Syndr Obes 7:409–420. https://doi.org/10.2147/DMSO.S51301
Becerra MB, Becerra BJ (2015) Disparities in age at diabetes diagnosis among Asian Americans: implications for early preventive measures. Prev Chronic Dis 12:E146. https://doi.org/10.5888/pcd12.150006
Casagrande SS, Cowie CC (2012) Health insurance coverage among people with and without diabetes in the U.S. adult population. Diabetes Care 35:2243–2249. https://doi.org/10.2337/dc12-0257
Centers for Disease Control and Prevention (CDC) (2012) Behavioral Risk Factor Surveillance System Survey data. CDC, Atlanta
Centers for Disease Control and Prevention (CDC) (2014a) Behavioral Risk Factor Surveillance System. 2013 codebook report. Land-line and cell-phone data
Centers for Disease Control and Prevention (CDC) (2014b) Behavioral Risk Factor Surveillance System. Survey data. CDC, Atlanta
Centers for Disease Control and Prevention (CDC) (2016a) Behavioral Risk Factor Surveillance System. 2015 codebook report. Land-line and cell-phone data. https://www.cdc.gov/brfss/annual_data/2015/pdf/codebook15_llcp.pdf
Centers for Disease Control and Prevention (CDC) (2016b) Behavioral Risk Factor Surveillance System. Survey data. CDC, Atlanta, GA
Centers for Disease Control and Prevention (CDC) (2016c) Diabetes and Asian Americans. https://www.cdc.gov/diabetes/library/spotlights/diabetes-asian-americans.html
Centers for Disease Control and Prevention (CDC) (2017a) LLCP 2016 codebook report. Overall version data weighted with _LLCPWT. Behavioral Risk Factor Surveillance System. https://www.cdc.gov/brfss/annual_data/2016/pdf/codebook16_llcp.pdf
Centers for Disease Control and Prevention (CDC) (2017b) National Diabetes Statistics Report, 2017. http://www.diabetes.org/assets/pdfs/basics/cdc-statistics-report-2017.pdf
Centers for Disease Control and Prevention (CDC) (2018a) Behavioral Risk Factor Surveillance System. Comparability of data BRFSS 2017. https://www.cdc.gov/brfss/annual_data/2017/pdf/compare-2017-508.pdf
Centers for Disease Control and Prevention (CDC) (2018b) LLCP 2017 codebook report. Overall version data weighted with _LLCPWT. Behavioral Risk Factor Surveillance System. https://www.cdc.gov/brfss/annual_data/2017/pdf/codebook17_llcp-v2-508.pdf
Cheung BMY, Li C (2012) Diabetes and hypertension: is there a common metabolic pathway? Curr Atheroscler Rep 14:160–166. https://doi.org/10.1007/s11883-012-0227-2
Conway BN, Han X, Munro HM et al (2018) The obesity epidemic and rising diabetes incidence in a low-income racially diverse southern US cohort. PLoS One 13:e0190993
Faught EL, Gleddie D, Storey KE, Davison CM, Veugelers PJ (2017) Healthy lifestyle behaviours are positively and independently associated with academic achievement: An analysis of self-reported data from a nationally representative sample of Canadian early adolescents. PLoS One 12:e0181938. https://doi.org/10.1371/journal.pone.0181938
Fewell Z, Davey Smith G, Sterne JAC (2007) The impact of residual and unmeasured confounding in epidemiologic studies: a simulation study. Am J Epidemiol 166:646–655. https://doi.org/10.1093/aje/kwm165
Fletcher B, Gulanick M, Lamendola C (2002) Risk factors for type 2 diabetes mellitus. J Cardiovasc Nurs 16:17–23
Ganz ML, Wintfeld N, Li Q, Alas V, Langer J, Hammer M (2014) The association of body mass index with the risk of type 2 diabetes: a case–control study nested in an electronic health records system in the United States. Diabetol Metab Syndr 6:50. https://doi.org/10.1186/1758-5996-6-50
Harris MI, Eastman RC (2000) Early detection of undiagnosed diabetes mellitus: a US perspective. Diabetes Metab Res Rev 16:230–236. https://doi.org/10.1002/1520-7560(2000)9999:9999<::AID-DMRR122>3.0.CO;2-W
Hsu WC, Araneta MRG, Kanaya AM, Chiang JL, Fujimoto W (2015) BMI cut points to identify at-risk Asian Americans for type 2 diabetes screening. Diabetes Care 38:150–158. https://doi.org/10.2337/dc14-2391
Jager KJ, Zoccali C, MacLeod A, Dekker FW (2008) Confounding: what it is and how to deal with it. Kidney Int 73:256–260. https://doi.org/10.1038/sj.ki.5002650
Jansen T, Rademakers J, Waverijn G, Verheij R, Osborne R, Heijmans M (2018) The role of health literacy in explaining the association between educational attainment and the use of out-of-hours primary care services in chronically ill people: a survey study. BMC Health Serv Res 18:394. https://doi.org/10.1186/s12913-018-3197-4
Jin XW, Slomka J, Blixen C (2002) Cultural and clinical issues in the care of Asian patients. Cleve Clin J Med 69:50. https://doi.org/10.3949/ccjm.69.1.50
Juckett G (2005) Cross-cultural medicine. Am Fam Physician 72:2267–2274
Judd SE, Gutiérrez OM, Newby PK et al (2013) Dietary patterns are associated with incident stroke and contribute to excess risk of stroke in black Americans. Stroke 44:3305–3311. https://doi.org/10.1161/strokeaha.113.002636
Kautzky-Willer A, Harreiter J, Pacini G (2016) Sex and gender differences in risk, pathophysiology and complications of type 2 diabetes mellitus. Endocr Rev 37:278–316. https://doi.org/10.1210/er.2015-1137
Kim W, Keefe RH (2010) Barriers to healthcare among Asian Americans. Soc Work Public Health 25:286–295. https://doi.org/10.1080/19371910903240704
Kim JE, Zane N (2016) Help-seeking intentions among Asian American and White American students in psychological distress: Application of the health belief model. Cultur Divers Ethnic Minor Psychol 22:311–321
Klompas M, Cocoros NM, Menchaca JT et al (2017) State and local chronic disease surveillance using electronic health record systems. Am J Public Health 107:1406–1412. https://doi.org/10.2105/ajph.2017.303874
Lachman ME, Weaver SL (1998) The sense of control as a moderator of social class differences in health and well-being. J Pers Soc Psychol 74:763–773
McNamee R (2005) Regression modelling and other methods to control confounding. Occup Environ Med 62:500–506
Narayan KMV, Boyle JP, Thompson TJ, Gregg EW, Williamson DF (2007) Effect of BMI on lifetime risk for diabetes in the U.S. Diabetes Care 30:1562–1566. https://doi.org/10.2337/dc06-2544
National Heart, Lung, and Blood Institute (2019) Overweight and obesity. https://www.nhlbi.nih.gov/health-topics/overweight-and-obesity
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) (2016) Risk factors for type 2 diabetes. https://www.niddk.nih.gov/health-information/diabetes/overview/risk-factors-type-2-diabetes
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) (2018) Prediabetes screening: how and why. https://www.niddk.nih.gov/health-information/communication-programs/ndep/health-professionals/game-plan-preventing-type-2-diabetes/prediabetes-screening-how-why
Oberoi S, Chaudhary N, Patnaik S, Singh A (2016) Understanding health seeking behavior. J Family Med Prim Care 5:463–464. https://doi.org/10.4103/2249-4863.192376
Pourhoseingholi MA, Baghestani AR, Vahedi M (2012) How to control confounding effects by statistical analysis. Gastroenterol Hepatol Bed Bench 5:79–83
Raparelli V, Morano S, Franconi F, Lenzi A, Basili S (2017) Sex differences in type-2 diabetes: implications for cardiovascular risk management. Curr Pharm Des 23:1471–1476. https://doi.org/10.2174/1381612823666170130153704
Schneider KL, Clark MA, Rakowski W, Lapane KL (2012) Evaluating the impact of non-response bias in the Behavioral Risk Factor Surveillance System (BRFSS). J Epidemiol Community Health 66:290–295. https://doi.org/10.1136/jech.2009.103861
StataCorp (2017) Stata statistical software: release 15. StataCorp LLC, College Station, TX
Steele CJ, Schöttker B, Marshall AH et al (2017) Education achievement and type 2 diabetes—what mediates the relationship in older adults? Data from the ESTHER study: a population-based cohort study. BMJ Open 7:e013569. https://doi.org/10.1136/bmjopen-2016-013569
Stegenga H, Haines A, Jones K, Wilding J; Guideline Development Group (2014) Identification, assessment, and management of overweight and obesity: summary of updated NICE guidance. BMJ 349:g6608
Tung EL, Baig AA, Huang ES, Laiteerapong N, Chua K-P (2017) Racial and ethnic disparities in diabetes screening between Asian Americans and other adults: BRFSS 2012–2014. J Gen Intern Med 32:423–429. https://doi.org/10.1007/s11606-016-3913-x
US Preventive Services Task Force (2015) Final recommendation statement. Abnormal blood glucose and type 2 diabetes mellitus: screening
van der Heide I, Wang J, Droomers M, Spreeuwenberg P, Rademakers J, Uiters E (2013) The relationship between health, education, and health literacy: results from the Dutch Adult Literacy and Life Skills Survey. J Health Commun 18(Suppl 1):172–184. https://doi.org/10.1080/10810730.2013.825668
Wang JH, Sheppard VB, Schwartz MD, Liang W, Mandelblatt JS (2008) Disparities in cervical cancer screening between Asian American and Non-Hispanic white women Cancer Epidemiol Biomarkers Prev 17:1968–1973. https://doi.org/10.1158/1055-9965.Epi-08-0078
Zhang X, Bullard KM, Gregg EW et al (2012) Access to health care and control of ABCs of diabetes. Diabetes Care 35:1566–1571. https://doi.org/10.2337/dc12-0081
Zimmerman EB, Woolf SH, Haley A (2015) Understanding the relationship between education and health: a review of the evidence and an examination of community perspectives. In: Kaplan RM, Spittel ML, David DH (eds) Population health: behavioral and social science insights. AHRQ publication no. 15-0002, pp 347–384
Acknowledgements
There are no acknowledgements. This work was not funded by any financial grants or other sources of funding.
Author information
Authors and Affiliations
Contributions
PT originated the idea and the study design. LaT ran the data analyses and interpreted the results. LiT assisted with the study design. All authors contributed to writing the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Research involving human participants and/or animals
This article does not contain any studies with human participants or animals performed by any of the authors. The BRFSS data used in this study is a secondary publicly available data source that has been completely anonymized and released for public use by the United States Centers for Disease Control and Prevention (CDC).
Informed consent
This article is exempt from needing informed consent as no human participants were involved in the study and the data used have been completely anonymized and approved for public use by the United States Centers for Disease Control and Prevention (CDC).
Disclosure
PT does not have any financial support or relationship that may pose a conflict of interest. LaT does not have any financial support or relationship that may pose a conflict of interest. LiT does not have any financial support or relationship that may pose a conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tran, P., Tran, L. & Tran, L. Sociodemographic, socioeconomic, and clinical factors associated with diabetes screening in Asian Americans. J Public Health (Berl.) 29, 1455–1462 (2021). https://doi.org/10.1007/s10389-020-01267-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10389-020-01267-2