Abstract
Purpose
To investigate the characteristics of retinal detachment (RD) and compare the outcomes of surgical interventions, such as scleral buckling (SB), pars plana vitrectomy (PPV), or PPV combined with SB, conducted on holidays and on workdays to determine the optimal surgical timing for primary RD treatment in clinical practice.
Study design
Retrospective cohort study.
Methods
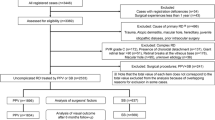
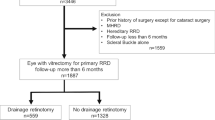
The cohort included 3178 patients with primary RD registered in the Japan Retinal Detachment Registry between February 2016 and March 2017. Surgery data were divided into holiday and workday groups. A descriptive analysis of primary RD characteristics was performed, and the outcomes for each surgical intervention were assessed. The primary outcome was anatomical failure at 6 months post-surgery classified as follows: level 1, inoperable state; level 2, anatomical recovery with silicone-oil use; and level 3, additional surgery required for RD repair.
Results
The holiday group comprised 108 and the workday, 3070 cases of primary RD. Compared with those in the workday group, surgery in the holiday group took longer (PPV, P < 0.0001; SB, P = 0.047) and was performed by less experienced surgeons (P = 0.014). However, there were no statistically significant differences in surgical failure 6 months post-surgery between the workday and holiday groups.
Conclusion
Although surgery conducted on holidays and workdays was not significantly different in terms of outcome, some surgery should be postponed with proper preoperative interim measures to limit RD progress until it can be conducted on workdays by a well-prepared team.

Similar content being viewed by others
References
Hillier RJ, Felfeli T, Berger AR, Wong DT, Altomare F, Dai D, et al. The pneumatic retinopexy versus vitrectomy for the management of primary rhegmatogenous retinal detachment outcomes randomized trial (PIVOT). Ophthalmology. 2019;126:531–9.
Yannuzzi NA, Li C, Fujino D, Kelly SP, Lum F, Flynn HW Jr, et al. Clinical outcomes of rhegmatogenous retinal detachment treated with pneumatic retinopexy. JAMA Ophthalmol. 2021. https://doi.org/10.1001/jamaophthalmol.2021.1860.
van Bussel EM, van der Valk R, Bijlsma WR, La Heij EC. Impact of duration of macula-off retinal detachment on visual outcome: A systematic review and meta-analysis of literature. Retina. 2014;34:1917–25.
Vail D, Pan C, Pershing S, Mruthyunjaya P. Association of rhegmatogenous retinal detachment and outcomes with the day of the week that patients undergo a repair or receive a diagnosis. JAMA Ophthalmol. 2020;138:156–63.
Lee IT, Lampen SIR, Wong TP, Major JC Jr, Wykoff CC. Fovea-sparing rhegmatogenous retinal detachments: impact of clinical factors including time to surgery on visual and anatomic outcomes. Graefes Arch Clin Exp Ophthalmol. 2019;257:883–9.
Perner A, Bellomo R, Moller MH. Is research from databases reliable? No Intensive Care Med. 2019;45:115–7.
Bray BD, Steventon A. What have we learnt after 15 years of research into the “weekend effect”? BMJ Qual Saf. 2017;26:607–10.
Dajani O, MacCumber MW. Do rhegmatogenous retinal detachment repair and outcomes vary by day of the week? JAMA Ophthalmol. 2020;138:163–4.
Sakamoto T, Kawano S, Kawasaki R, Hirakata A, Yamashita H, Yamamoto S, et al. Japan-Retinal Detachment Registry Report I: preoperative findings in eyes with primary retinal detachment. Jpn J Ophthalmol. 2019;64:1–12.
Adelman RA, Parnes AJ, Sipperley JO, Ducournau D. Strategy for the management of complex retinal detachments: the European vitreo-retinal society retinal detachment study report 2. Ophthalmology. 2013;120:1809–13.
Kumawat D, Sachan A. The pneumatic retinopexy versus vitrectomy for the management of primary rhegmatogenous retinal detachment outcomes randomized trial (PIVOT) (Ophthalmology. 2019;126:531–539). Ophthalmology. 2019;126:e84.
Muni RH, Juncal VR, Hillier RJ. Questions on rhegmatogenous retinal detachment and the day of the week of repair or diagnosis. JAMA Ophthalmol. 2020;138:802–3.
Wykoff CC, Flynn HW Jr, Scott IU. What is the optimal timing for rhegmatogenous retinal detachment repair? JAMA Ophthalmol. 2013;131:1399–400.
Ng H, La Heij EC, van Meurs JC. The duration of macular detachment in retinal detachment is difficult to determine. Acta Ophthalmol. 2020;98:e396–7.
Lee CS, Shaver K, Yun SH, Kim D, Wen S, Ghorayeb G. Comparison of the visual outcome between macula-on and macula-off rhegmatogenous retinal detachment based on the duration of macular detachment. BMJ Open Ophthalmol. 2021;6:e000615.
Kawano H, Ito T, Yamada S, Hashiguchi T, Maruyama I, Hisatomi T, et al. Toxic effects of extracellular histones and their neutralization by vitreous in retinal detachment. Lab Investig. 2014;94:569–85.
Geller SF, Lewis GP, Fisher SK. FGFR1, signaling, and AP-1 expression after retinal detachment: reactive Müller and RPE cells. Invest Ophthalmol Vis Sci. 2001;42:1363–9.
de Jong JH, Vigueras-Guillén JP, Simon TC, Timman R, Peto T, Vermeer KA, et al. Preoperative posturing of patients with macula-on retinal detachment reduces progression toward the fovea. Ophthalmology. 2017;124:1510–22.
Casswell EJ, Yorston D, Lee E, Heeren TFC, Harris N, Zvobgo TM, et al. Effect of face-down positioning vs support-the-break positioning after macula-involving retinal detachment repair: the PostRD randomized clinical trial. JAMA Ophthalmol. 2020;138:634–42.
Kontos A, Williamson TH. Rate and risk factors for the conversion of fovea-on to fovea-off rhegmatogenous retinal detachment while awaiting surgery. Br J Ophthalmol. 2017;101:1011–5.
Wykoff CC, Smiddy WE, Mathen T, Schwartz SG, Flynn HW Jr, Shi W. Fovea-sparing retinal detachments: time to surgery and visual outcomes. Am J Ophthalmol. 2010;150:205-10.e2.
Callizo J, Pfeiffer S, Lahme E, van Oterendorp C, Khattab M, Bemme S, et al. Risk of progression in macula-on rhegmatogenous retinal detachment. Graefes Arch Clin Exp Ophthalmol. 2017;255:1559–64.
Acknowledgements
This study was supported by the Japan Retina Vitreous Society and by JSPS KAKENHI Grant Number JP21H03095. The sponsor or funding organization had no role in the design or conduct of this research. We would like to thank Editage (http://www.editage.com) for English language editing.
Group Information: The members of THE J-RD Registry project are as follows: Chiba University: Shuichi Yamamoto, Takayuki Baba, Eiju Sato, Masayasu Kitahashi, Tomoaki Tatsumi, Gen Miura, and Tomohiro Niizawa. Kagoshima University: Taiji Sakamoto, Keita Yamakiri, Toshifumi Yamashita, Hiroki Otsuka, Seiji Sameshima, Narimasa Yoshinaga, and Shozo Sonoda. Kyorin University: Akito Hirakata, Takashi Koto, Makoto Inoue, Kazunari Hirota, Yuji Itoh, Tadashi Orihara, Yoshinobu Emoto, Masahiko Sano, Hiroyuki Takahashi, and Ryo Tokizawa. Yamagata University: Hidetoshi Yamashita, Koichi Nishitsuka, Yutaka Kaneko, and Katsuhiro Nishi. Asahikawa Medical University Hospital: Akitoshi Yoshida, Shinji Ono, Hiroyuki Hirokawa, Kenji Sogawa, Tsuneaki Omae, and Akihiro Ishibazawa. Gunma University: Shoji Kishi, Hideo Akiyama, Hidetaka Matsumoto, Ryo Mukai, and Masahiro Morimoto. Hirosaki University: Mitsuru Nakazawa, Yukihiko Suzuki, Takashi Kudo, and Kobu Adachi. Hokkaido University: Susumu Ishida, Kousuke Noda, Satoru Kase, Syouhei Mori, Ryo Ando, Michiyuki Saito, and Tomohiro Suzuki. Kansai Medical University Hospital: Kanji Takahashi, Yoshimi Nagai, Tadashi Nakauchi, and Haruiko Yamada. Kindai University Sakai Hospital: Shuji Kusaka, and Daishi Tsujioka. Kyoto University: Akitaka Tsujikawa and Kiyoshi Suzuma. Kyushu University: Tatsuro Ishibashi, Koh-Hei Sonoda, Yasuhiro Ikeda, Riichiro Kohno, and Keijiro Ishikawa. Mie University: Mineo Kondo and Maki Kozawa. Nagasaki University: Takashi Kitaoka and Eiko Tsuiki. Nagoya City University: Yuichiro Ogura, Munenori Yoshida, Hiroshi Morita, Aki Kato, Yoshio Hirano, and Kazuhiko Sugitani. Nagoya University: Hiroko Terasaki, Takeshi Iwase, Yasuki Ito, Shinji Ueno, Hiroki Kaneko, Norie Nonobe, and Taro Kominami. National Center for Child Health and Development: Noriyuki Azuma and Tadashi Yokoi. Nihon University Hospital: Hiroyuki Shimada, Hiroyuki Nakashizuka, Takayuki Hattori, Ari Shinojima, and Yorihisa Kutagawa. Okayama University: Fumio Shiraga, Yuki Morizane, and Shuhei Kimura. Osaka Medical School: Tsunehiko Ikeda, Teruyo Kida, Takaki Sato, and Masanori Fukumoto. Osaka Rosai Hospital: Kazuyuki Emi and Hiroshi Nakashima. Shiga Medical University: Masahito Ohji, Masashi Kakinoki, and Osamu Sawada. Takeuchi Eye Clinic: Shinobu Takeuchi and Sumiyoshi Tanaka. Tokyo Women’s Medical College: Tomohiro Iida, Hideki Koizumi, Ichiro Maruko, Taiji Hasegawa, and Akiko Kogure. Yamanashi University: Hiroyuki Iijima, Tomohiro Oshiro, Yasushi Tateno, Wataru Kikushima, Atsushi Sugiyama, and Seigo Yoneyama. Yokohama City University Medical Center: Kazuaki Kadonosono, Shimpei Sato, and Shin Yamane.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflicts of interest
S. Kawano, Lecture fee (Novartis); T. Imai, None; T. Sakamoto, Grant, Consultant fee (Novartis, Bayer), Grant, Honoraria (Santen), Grant (Senju), Lecture fee (Alcon), Consultant fee (Bausch + Lomb).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Corresponding Author: Taiji Sakamoto
The members of Japan-Retinal Detachment Registry Group are mentioned in “Acknowledgements”.
Supplementary Information
Below is the link to the electronic supplementary material.
About this article
Cite this article
Kawano, S., Imai, T., Sakamoto, T. et al. Differences in primary retinal detachment surgery conducted on holidays and workdays analyzed using the Japan Retinal Detachment Registry. Jpn J Ophthalmol 66, 271–277 (2022). https://doi.org/10.1007/s10384-022-00911-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10384-022-00911-6