Abstract
Purpose
To examine the effect of switching from a prostanoid FP receptor agonists to EP2 receptor agonist (omidenepag isopropyl) on the deepening of the upper eyelid sulcus (DUES) and intraocular pressure (IOP) in Japanese glaucoma patients over 3 months post treatment.
Study design
Prospective observational study.
Methods
Patients with glaucoma who received FP receptor agonists treatment and had complained of DUES-related reduction in quality of life were included. Their FP receptor agonists was switched to omidenepag isopropyl without a drug holiday. At baseline and 1 and 3 months post-switch, photographs were taken and the changes in DUES were assessed by three independent observers. IOP and adverse events were also assessed.
Results
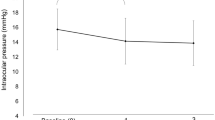
The study included 23 eyes of 23 patients (6 men, 17 women; average age, 60.6 years). After switching, DUES improved in 12 eyes at 1 month and in 16 eyes at 3 months; eyes in the remaining patients showed no worsening of the condition. The mean IOP before switching was 15.3 ± 3.3 mmHg (95% confidence interval 13.9–16.7 mmHg). Following the switch, the mean IOP values were 15.6 ± 3.3 mmHg (14.1–17.0 mmHg) at 1 month and 15.5 ± 3.3 mmHg (14.1–16.9 mmHg) at 3 months (P = 1.0 at 1 month, P = 1.0 at 3 months; both adjusted by Bonferroni correction). No adverse effects were observed.
Conclusion
Omidenepag isopropyl improved DUES while maintaining IOP in over 70% of Japanese patients with glaucoma who exhibited DUES caused by FP receptor agonists; the improvement was observed within 3 months after switching from FP receptor agonists.


Similar content being viewed by others
References
The Japan Glaucoma Society. Glaucoma Practice Guidelines (4th edition). Nippon Ganka Gakkai Zasshi. 2018;122:5–53 (in Japanese).
Kashiwagi K, Furuya T. Persistence with topical glaucoma therapy among newly diagnosed Japanese patients. Jpn J Ophthalmol. 2014;58:68–74.
Li T, Lindsley K, Rouse B, Hong H, Shi Q, Friedman DS, et al. Comparative effectiveness of first-line medications for primary open-angle glaucoma: a systematic review and network meta-analysis. Ophthalmology. 2016;123:129–40.
Cheng JW, Cai JP, Wei RL. Meta-analysis of medical intervention for normal tension glaucoma. Ophthalmology. 2009;116:1243–9.
Alm A, Grierson I, Shields MB. Side effects associated with prostaglandin analog therapy. Surv Ophthalmol. 2008;53(Suppl 1):S93-105.
Tan P, Malhotra R. Oculoplastic considerations in patients with glaucoma. Surv Ophthalmol. 2016;61:718–25.
Aihara M, Shirato S, Sakata R. Incidence of deepening of the upper eyelid sulcus after switching from latanoprost to bimatoprost. Jpn J Ophthalmol. 2011;55:600–4.
Kucukevcilioglu M, Bayer A, Uysal Y, Altinsoy HI. Prostaglandin associated periorbitopathy in patients using bimatoprost, latanoprost and travoprost. Clin Exp Ophthalmol. 2014;42:126–31.
Park J, Cho HK, Moon JI. Changes to upper eyelid orbital fat from use of topical bimatoprost, travoprost, and latanoprost. Jpn J Ophthalmol. 2011;55:22–7.
Taketani Y, Yamagishi R, Fujishiro T, Igarashi M, Sakata R, Aihara M. Activation of the prostanoid FP receptor inhibits adipogenesis leading to deepening of the upper eyelid sulcus in prostaglandin-associated periorbitopathy. Invest Ophthalmol Vis Sci. 2014;55:1269–76.
Lee YK, Lee JY, Moon JI, Park MH. Effectiveness of the ICare rebound tonometer in patients with overestimated intraocular pressure due to tight orbit syndrome. Jpn J Ophthalmol. 2014;58:496–502.
Miki T, Naito T, Fujiwara M, Araki R, Kiyoi R, Shiode Y, et al. Effects of pre-surgical administration of prostaglandin analogs on the outcome of trabeculectomy. PLoS ONE. 2017;12:e0181550.
Sakata R, Shirato S, Miyata K, Aihara M. Incidence of deepening of the upper eyelid sulcus in prostaglandin-associated periorbitopathy with a latanoprost ophthalmic solution. Eye (Lond). 2014;28:1446–51.
Jayaram A, Wladis E, Akkara JD, Yen MT, Seibold LK, Burkat CN. Prostaglandin associated periorbitopathy. In: EyeWiki. American Academy of Ophthalmology. https://eyewiki.aao.org/Prostaglandin_Associated_Periorbitopathy.
Kirihara T, Taniguchi T, Yamamura K, Iwamura R, Yoneda K, Odani-Kawabata N, et al. Pharmacologic characterization of omidenepag isopropyl, a novel selective EP2 receptor agonist, as an ocular hypotensive agent. Invest Ophthalmol Vis Sci. 2018;59:145–53.
Aihara M, Lu F, Kawata H, Iwata A, Odani-Kawabata N, Shams NK. Omidenepag isopropyl versus latanoprost in primary open-angle glaucoma and ocular hypertension: the phase 3 AYAME study. Am J Ophthalmol. 2020;220:53–63.
Yamamoto Y, Taniguchi T, Inazumi T, Iwamura R, Yoneda K, Odani-Kawabata N, et al. Effects of the selective EP2 receptor agonist omidenepag on adipocyte differentiation in 3T3-L1 cells. J Ocul Pharmacol Ther. 2020. https://doi.org/10.1089/jop.2019.0079.
Sakata R, Shirato S, Miyata K, Aihara M. Recovery from deepening of the upper eyelid sulcus after switching from bimatoprost to latanoprost. Jpn J Ophthalmol. 2013;57:179–84.
Sakata R, Shirato S, Miyata K, Aihara M. Incidence of deepening of the upper eyelid sulcus on treatment with a tafluprost ophthalmic solution. Jpn J Ophthalmol. 2014;58:212–7.
Breslow NE, Clayton DG. Approximate inference in generalized linear mixed models. J Am Stat Assoc. 1993;88:9–25.
Jayaprakasam A, Ghazi-Nouri S. Periorbital fat atrophy—an unfamiliar side effect of prostaglandin analogues. Orbit. 2010;29:357–9.
Nakakura S. Icare((R)) rebound tonometers: review of their characteristics and ease of use. Clin Ophthalmol. 2018;12:1245–53.
Whitson JT, Trattler WB, Matossian C, Williams J, Hollander DA. Ocular surface tolerability of prostaglandin analogs in patients with glaucoma or ocular hypertension. J Ocul Pharmacol Ther. 2010;26:287–92.
Acknowledgements
This study was funded by Santen Pharmaceutical Co., Ltd, Osaka.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
R. Sakata, None; T. Fujishiro, None; H. Saito, None; N. Nakamura, None; M. Honjo, None; S. Shirato, None; E. Miyamoto, Employee (Santen); Y. Yamada, Employee (Santen); M. Aihara, None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Corresponding Author: Rei Sakata
About this article
Cite this article
Sakata, R., Fujishiro, T., Saito, H. et al. Recovery of deepening of the upper eyelid sulcus after switching from prostaglandin FP receptor agonists to EP2 receptor agonist: a 3-month prospective analysis. Jpn J Ophthalmol 65, 591–597 (2021). https://doi.org/10.1007/s10384-021-00855-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10384-021-00855-3