Abstract
Purpose
We present a novel technique for measuring volume of space replaced by air during fluid-air exchange in vitrectomy (vitrectomized space) for intravitreal gas injection. To confirm the feasibility of this technique, we assessed postoperative intraocular pressure (IOP) and the duration of injected gas. Using this technique, we found remarkable differences in volume between high myopic eyes with retinal detachment caused by peripheral break (PB-RD group) and those with macular hole retinal detachment (MH-RD group). We studied the relationships between the volume and biometric values, axial length (AL) and corneal curvature radius (CCR) in both PB-RD and MH-RD group.
Study design
Retrospective study.
Methods
During fluid-air exchange, the aspirated fluid accumulates in the measuring cup between the infusion needle and vitrectomy instrument. Vitrectomized space volume is obtained by subtracting the volume of the tube between the infusion needle and the 3-way stopcock from the aspirated fluid volume. We performed phaco-vitrectomies by measuring the vitrectomized space volume and then injected pure SF6 at 15% of the volume into the vitreous cavity in 156 myopic eyes (AL > 26 mm) with RD consisting of 144 eyes in PB-RD group and 12 in MH-group.
Results
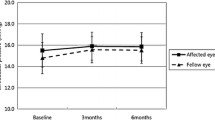
The IOP (mean ± SD) was 13.5 ± 3.4 mmHg preoperatively, 23.4 ± 10.4 mmHg on day 1, 18.2 ± 7.4 mmHg on day 2, and 16.1 ± 4.5 on day 7. The gas disappeared in 16.1 ± 1.9 days. Axial length was longer in the MH-RD group but the volume of vitrectomized space was larger in the PB-RD group. AL and volume were significantly correlated in both groups (P < 0.01), but the fitting lines differed. The CCR and volume significantly correlated in the PB-RD group (P < 0.01) but not in the MH-RD group.
Conclusion
Our novel technique for measuring the volume of vitrectomized space can achieve target gas concentration in the vitreous cavity. The difference in the shape of eyeballs may explain discrepancies in relationship between volume and the biometric factors.





Similar content being viewed by others
References
Escoffery RF, Olk RJ, Grand MG, Boniuk I. Vitrectomy without scleral bukling for primary rhegamatonenous retinal detachment. Am J Ophthalmol. 1985;99:275–81.
McCuen BW, Landers MB, Machemer R. The use of silicone oil following failed vitrectomy for retinal detachment with advanced proliferative vitreoretinopathy. Ophthalmology. 1985;92:1029–34.
Kelly NE, Wendel RT. Vitreous surgery for idiopathic macular holes. Results of a pilot study. Arch Ophthalmol. 1991;109:654–9.
Sugimoto M, Horiguchi M, Tanikawa A, Shimada Y. Novel retrobulbar anesthesia technique through the sub-Tenon’s space using a sharp needle in a blunt cannula. Ophthalmic Surg Lasers Imaging Retina. 2013. https://doi.org/10.3928/23258160-20130909-11.
Horio N, Horiguchi M, Yamamoto N. Triamcinolone-assisted internal limiting membrane peeling during idiopathic macular hole surgery. Arch Ophthalmol. 2005;123:96–9.
Williams DF, Peters MA, Abrams GW, Han DP, Mieler WF. A two-stage technique for intraoperative fluid-gas exchange following pars plana vitrectomy. Arch Ophthalmol. 1990;108:1484–6.
Shunmugam M, Shunmugam A, Williamson TH, Laidlaw DA. Air-gas exchange reevaluated: clinically important results of a computer simulation. Invest Ophthalmol Vis Sci. 2011;21(52):8262–5.
Han DP, Abrams GW, Bennett SR, Williams DF. Perfluoropropane 12% versus 20%. Effect on intraocular pressure and gas tamponade after pars plana vitrectomy. Retina. 1993;13:302–6.
Han DP, Lewis H, Lambrou FH Jr, Mieler WF, Hartz A. Mechanisms of intraocular pressure elevation after pars plana vitrectomy. Ophthalmology. 1989;96:1357–62.
Sigler EJ, Randolph JC, Charles S, Calzada JI. Intravitreal fluorinated gas preference and occurrence of rare ischemic postoperative complications after pars plana vitrectomy: a survey of the american society of retina specialists. J Ophthalmol. 2012;2012:230596.
Kannan NB, Adenuga OO, Kumar K, Ramasamy K. Outcome of 2 cc pure sulfur hexafluoride gas tamponade for macular hole surgery. BMC Ophthalmol. 2016;16:73.
Atchinson DA, Jones CA, Schmid KL, Prichard N, Rope JM, Strugnell WE, et al. Eye shape in emmetropia and myopia. Invest Ophthalmol Vis Sci. 2004;45:3380–6.
Curtin BJ. The myopias. Philadelphia: Harper; 1985.
Kato D, Mizuguchi T, Shimada Y, Sakurai R, Sekido Y, Tanikawa A, et al. J Jpn Ophthalmol Soc. 2019;123:175 (abastract).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
H. Tanaka, None; A. Tanikawa, None; Y. Shimada, None; Y. Miyake, None; T. Mizuguchi, None; M. Horiguchi, None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Corresponding author: Tadashi Mizuguchi
About this article
Cite this article
Tanaka, H., Tanikawa, A., Shimada, Y. et al. Measurement of the volume of the vitrectomized space during vitrectomy in myopic patients with retinal detachment. Jpn J Ophthalmol 64, 210–215 (2020). https://doi.org/10.1007/s10384-019-00713-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10384-019-00713-3