Abstract
Purpose
To compare refractive changes in operated eyes and fellow unoperated eyes following unilateral lateral rectus recession in early school-aged children.
Study design
A retrospective case control study.
Methods
The medical records of children under ten years of age with intermittent exotropia who underwent unilateral lateral recession surgery were reviewed. The operated eyes were reviewed and the fellow unoperated eyes were used as control. The rate of myopic progression was calculated by spherical equivalent (SE) changes per year, and by the rate of refractive growth (RRG) equation.
Results
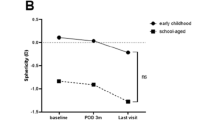
SE showed a myopic shift one week after surgery and in the following months, from -1.43 ± 1.84 diopters (D) at 1 week post operation to -1.57 ± 2.22 D at one year and, finally -2.95 ± 2.97 D at the average 4.62 years following surgery. However, the SE shift was not significantly different from the unoperated eye. The low myopia group (under -3.0 D) showed a significantly higher myopic change in the operated eye until one year post operation (p = 0.022). The average myopic shift ratio was -0.53 ± 0.46 D yearly in the operated eye.
Conclusions
This study presents data of a large series of refractive changes secondary to lateral rectus recession, and of long-term myopia progression in Korean population.




Similar content being viewed by others
References
Rajavi Z, Mohammad Rabei H, Ramezani A, Heidari A, Daneshvar F. Refractive effect of the horizontal rectus muscle recession. Int ophthalmol. 2008;28:83–8.
Hong SW, Kang NY. Astigmatic changes after horizontal rectus muscle surgery in intermittent exotropia. Korean J Ophthalmol. 2012;26:438–45.
Noh JH, Park KH, Lee JY, Jung MS, Kim SY. Changes in refractive error and anterior segment parameters after isolated lateral rectus muscle recession. J AAPOS. 2013;17:291–5.
Shin KH, Hyun SH, Kim IN, Paik HJ. The impact of intermittent exotropia and surgery for intermittent exotropia on myopic progression among early school-aged children with myopia. Br J Ophthalmol. 2014;98:1250–4.
Leshno A, Mezad-Koursh D, Ziv-Baran T, Stolovitch C. A paired comparison study on refractive changes after strabismus surgery. J AAPOS. 2017;21(460–2):e1.
Bae SH, Choi DG. Changes of corneal topographic measurements and higher-order aberrations after surgery for exotropia. PLoS One. 2018;13:e0202864.
Christensen AM, Wallman J. Evidence that increased scleral growth underlies visual deprivation myopia in chicks. Investig Ophthalmol Vis Sci. 1991;32:2143–50.
Smith EL 3rd. Spectacle lenses and emmetropization: the role of optical defocus in regulating ocular development. Optometry Vis Sci. 1998;75:388–98.
Horwood AM, Riddell PM. Evidence that convergence rather than accommodation controls intermittent distance exotropia. Acta Ophthalmol. 2012;90:e109–17.
Ekdawi NS, Nusz KJ, Diehl NN, Mohney BG. The development of myopia among children with intermittent exotropia. Am J Ophthalmol. 2010;149:503–7.
Gwiazda J, Thorn F. Development of refraction and strabismus. Curr Opin Ophthalmol. 1998;9:3–9.
McClatchey SK, Hofmeister EM. The optics of aphakic and pseudophakic eyes in childhood. Surv Ophthalmol. 2010;55:174–82.
Bagheri A, Farahi A, Guyton DL. Astigmatism induced by simultaneous recession of both horizontal rectus muscles. J AAPOS. 2003;7:42–6.
Preslan MW, Cioffi G, Min YI. Refractive error changes following strabismus surgery. J Pediatric Ophthalmol Strabismus. 1992;29:300–4.
Schaeffel F, Glasser A, Howland HC. Accommodation, refractive error and eye growth in chickens. Vis Res. 1988;28:639–57.
Irving EL, Sivak JG, Callender MG. Refractive plasticity of the developing chick eye. Ophthalmic Physiol Opt. 1992;12:448–56.
Smith EL 3rd, Hung LF. The role of optical defocus in regulating refractive development in infant monkeys. Vis Res. 1999;39:1415–35.
Wallman J, Adams JI. Developmental aspects of experimental myopia in chicks: susceptibility, recovery and relation to emmetropization. Vis Res. 1987;27:1139–63.
Wildsoet CF. Active emmetropization–evidence for its existence and ramifications for clinical practice. Ophthalmic Physiol Opt. 1997;17:279–90.
Suzuki H, Hikoya A, Komori M, Inagaki R, Haseoka T, Arai S, et al. Changes in conjunctival-scleral thickness after strabismus surgery measured with anterior segment optical coherence tomography. Jpn J Ophthalmol. 2018;62:554–9.
Wong HB, Machin D, Tan SB, Wong TY, Saw SM. Ocular component growth curves among Singaporean children with different refractive error status. Investig Ophthalmol Vis Sci. 2010;51:1341–7.
Jones LA, Mitchell GL, Mutti DO, Hayes JR, Moeschberger ML, Zadnik K. Comparison of ocular component growth curves among refractive error groups in children. Investig Ophthalmol Vis Sci. 2005;46:2317–27.
Lam CS, Edwards M, Millodot M, Goh WS. A 2-year longitudinal study of myopia progression and optical component changes among Hong Kong schoolchildren. Optometry Vis Sci. 1999;76:370–80.
Shih YF, Chiang TH, Hsiao CK, Chen CJ, Hung PT, Lin LL. Comparing myopic progression of urban and rural Taiwanese schoolchildren. Jpn J Ophthalmol. 2010;54:446–51.
Saw SM, Nieto FJ, Katz J, Schein OD, Levy B, Chew SJ. Factors related to the progression of myopia in Singaporean children. Optometry Vis Sci. 2000;77:549–54.
Kwitko S, Feldon S, McDonnell PJ. Corneal topographic changes following strabismus surgery in Grave’s disease. Cornea. 1992;11:36–40.
Asejczyk-Widlicka M, Pierscionek BK. The elasticity and rigidity of the outer coats of the eye. Br J Ophthalmol. 2008;92:1415–8.
Dottan SA, Hoffman P, Oliver MD. Astigmatism after strabismus surgery. Ophthalmic Surg. 1988;19:128–9.
Acknowledgements
There is no competing interest for any of the authors. This study was supported by the Catholic Medical Center Research Foundation made in the program year of 2018. Design of the study (Y.P., S.H.P., S.Y.S.), collection of the data (Y.P. and Y.J.A.), management and analysis of the data (Y.P.), interpretation of the data (Y.P. and S.Y.S.), writing of the article (Y.P. and Y.J.A.), approval of the manuscript (Y.P., S.H.P., S.Y.S.), obtaining of funding (S.Y.S.), searching the literature (Y.P.).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
Y. Park, None; Y. J. Ahn, None; S. H. Park, None; S. Y. Shin, None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Corresponding Author: Sun Young Shin
About this article
Cite this article
Park, Y., Ahn, Y.J., Park, S.H. et al. Interocular difference associated with myopic progression following unilateral lateral rectus recession in early school-aged children. Jpn J Ophthalmol 63, 474–482 (2019). https://doi.org/10.1007/s10384-019-00689-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10384-019-00689-0