Abstract
Purpose
To evaluate the long-term outcomes of penetrating keratoplasty (PKP) according to the corneal disease diagnosis and the number of PKP procedures performed.
Methods
Five-hundred-and-nine eyes from 403 patients who underwent PKP at Miyata Eye Hospital in Japan from 1998 through 2014, were included in this study. Medical charts were retrospectively examined to ascertain the corneal disease diagnosis and the period of graft survival. Graft survival rates were compared among various corneal disease diagnoses and among the number of PKP procedures performed. Changes in corneal endothelial cell density (ECD) were analyzed using a mixed-effects model. The presence/absence of various risk factors was compared between transparent grafts and failed grafts.
Results
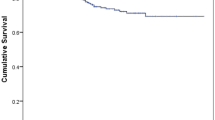
The overall rate of graft survival at 12 years was 60.4%. The rates of graft survival in keratoconus was 100%, in corneal dystrophy 100%, in leukoma 70.8%, and in bullous keratopathy 51.7%. The rates of graft survival at 12 years for the first PKP was 65.4% and for the second PKP, 43.4% (p < 0.001). All cases of third PKP and fourth PKP failed within 8 years. Preoperative mean ECD (95% confidence interval) was 2722 (2666–2778) cells/mm2; it decreased exponentially after PKP. Mean ECD was 659 (440–878) cells/mm2 at 10 years. Rejection, trauma, and infection occurred significantly more frequently in failed grafts than in transparent grafts.
Conclusions
The long-term prognosis of PKP depends on the original diagnosis. The long-term prognosis of re-grafting is worse than that of primary grafts. Rejection, trauma, and infection are risk factors for graft failure.





Similar content being viewed by others
References
Thompson RW Jr, Price MO, Bowers PJ, Price FW Jr. Long-term graft survival after penetrating keratoplasty. Ophthalmology. 2003;10:1396–402.
Ing JJ, Ing HH, Nelson LR, Hodge DO, Bourne WM. Ten-year postoperative results of penetrating keratoplasty. Ophthalmology. 1998;105:1855–65.
Patel SV, Hodge DO, Bourne WM. Corneal endothelium and postoperative outcomes 15 years after penetrating keratoplasty. Am J Ophthalmol. 2005;139:311–9.
Muraine M, Sanchez C, Watt L, Retout A, Brasseur G. Long-term results of penetrating keratoplasty. A 10-year-plus retrospective study. Graefes Arch Clin Exp Ophthalmol. 2003;241:571–6.
Writing Committee for the Cornea Donor Study Research Group. Factors associated with corneal graft survival in the cornea donor study. JAMA Ophthalmol. 2015;133:246–54.
Tan DT, Janardhanan P, Zhou H, Chan YH, Htoon HM, Ang LP, et al. Penetrating keratoplasty in Asian eyes: the Singapore corneal transplant study. Ophthalmology. 2008;115:975–82.
Inoue K, Amano S, Oshika T, Sawa M, Tsuru T. A 10-year review of penetrating keratoplasty. Jpn J Ophthalmol. 2000;44:139–45.
Tsuchida H, Arakaki Y, Uchiyama S, Ikehara M, Kobayashi K, Yuguchi T, et al. Outcome of primary penetrating keratoplasty at Kaiya Eye Clinic. Rinsho Ganka (in Japanese). 2007;61:81–6.
Yamamoto S, Shimmura-Tomita M, Satake Y, Shimazaki-Den S, Shimmura S, Shimazaki J. Factors affecting outcomes of repeated penetrating keratoplasty. Nippon Ganka Gakkai Zasshi (in Japanese). 2015;119:625–31.
Al-Mezaine H, Wagoner MD. Repeat penetrating keratoplasty: indications, graft survival, and visual outcome. Br J Ophthalmol. 2006;90:324–7.
Weisbrod DJ, Sit M, Naor J, Slomovic AR. Outcomes of repeat penetrating keratoplasty and risk factors for graft failure. Cornea. 2003;22:429–34.
Yu AL, Kaiser M, Schaumberger M, Messmer E, Kook D, Welge-Lussen U. Perioperative and postoperative risk factors for corneal graft failure. Clin Ophthalmol. 2014;8:1641–7.
Vajpayee RB, Boral SK, Dada T, Murthy GVS, Pandey RM, Satpathy G. Risk factors for graft infection in India: a case-control study. Br J Ophthalmol. 2002;86:261–5.
Vajpayee RB, Sharma N, Sinha R, Agarwal T, Singhvi A. Infectious keratitis following keratoplasty. Surv Ophthalmol. 2007;52:1–12.
Moorthy S, Graue E, Jhanji V, Constantinou M, Vajpayee RB. Microbial keratitis after penetrating keratoplasty: impact of sutures. Am J Ophthalmol. 2011;152:189–94.
Shimazaki J, Shinozaki N, Shimmura S, Holland EJ, Tsubota K. Efficacy and safety of international donor sharing: a single-center, case-controlled study on corneal transplantation. Transplantation. 2004;78:216–20.
Inoue K, Kimura C, Amano S, Sato T, Fujita N, Kagaya F, et al. Long-term outcome of systemic cyclosporine treatment following penetrating keratoplasty. Jpn J Ophthalmol. 2001;45:378–82.
Birnbaum F, Mayweg S, Reis A, Böhringer D, Seitz B, Engelmann K, et al. Mycophenolate mofetil (MMF) following penetrating high-risk keratoplasty: long-term results of a prospective, randomised, multicentre study. Eye (Lond). 2009;23:2063–70.
Reinhard T, Mayweg S, Sokolovska Y, Seitz B, Mittelviefhaus H, Engelmann K, et al. Systemic mycophenolate mofetil avoids immune reactions in penetrating high-risk keratoplasty: preliminary results of an ongoing prospectively randomized multicentre study. Transpl Int. 2005;18:703–8.
Acknowledgements
We would like to thank Dr. Toshihito Furukawa (Biostatistical Research CO., LTD) for statistical analyses and Editage (http://www.editage.jp) for English language editing.
Conflicts of interest
T. Ono, None; S. Ishiyama, None; T. Hayashidera, None; Y. Mori, Grants (Alcon, AMO, BD, HOYA, Mitsubishi Chemical Medience, Otsuka pharmaceutical, Santen pharmaceutical, Senju pharmaceutical), Lecture fees (HOYA, Otsuka pharmaceutical, Pfizer, Senju pharmaceutical); R. Nejima, None; K. Miyata, Grants (Alcon, AMO, HOYA, Otsuka Pharmaceutical, Santen Pharmaceutical, Senju Pharmaceutical), Lecture fees (Alcon, AMO, Chuo Sangio, HOYA, Otsuka Pharmaceutical, Senju Pharmaceutical); S. Amano, Grants (Alcon, AMO, HOYA, Otsuka Pharmaceutical, Santen Pharmaceutical, Senju Pharmaceutical), Lecture fees (Alcon, AMO, HOYA, Otsuka Pharmaceutical, Santen Pharmaceutical, Senju Pharmaceutical).
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Ono, T., Ishiyama, S., Hayashidera, T. et al. Twelve-year follow-up of penetrating keratoplasty. Jpn J Ophthalmol 61, 131–136 (2017). https://doi.org/10.1007/s10384-016-0489-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10384-016-0489-2