Abstract
Purpose
To report two cases of acute macular neuroretinopathy with unusually small parafoveal lesions, which showed later recurrent lesions either in the same eye or the fellow eye.
Methods
Observational case series.
Patients
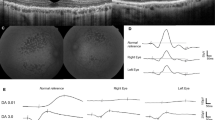
In case 1, a 48-year-old woman developed a sudden onset of a tiny paracentral scotoma associated with a small reddish-brown paracentral lesion. A new paracentral lesion with a corresponding scotoma developed 1 year later. In case 2, a 39-year-old man with diabetes type 1 developed a pracentral scotoma OS with a corresponding small reddish-brown lesion. Two months later, a similar lesion with a corresponding scotoma developed in the fellow eye.
Conclusions
Acute macular neuroretinopathy may present with tiny paracentral lesions difficult to detect with fundus examination, and may be associated with recurrent lesions either in the same eye or the fellow eye.



Similar content being viewed by others
References
Bos PLM, Deutman AF. Acute macular neuroretinopathy. Am J Ophthalmol. 1975;80:573–84.
Turbeville SD, Cowan LD, Gass JD. Acute macular neuroretinopathy: a review of the literature. Surv Ophthalmol. 2003;48:1–11.
Rush JA. Acute macular neuroretinopathy. Am J Ophthalmol. 1977;83:490–4.
Miller MH, Spalton DJ, Fitzke FW, Bird AC. Acute macular neuroretinopathy. Ophthalmology. 1989;96:265–9.
Feigl B, Haas A. Optical coherence tomography (OCT) in acute macular neuroretinopathy. Acta Ophthalmol Scand. 2000;78:714–6.
Monson BK, Greenberg PB, Greenberg E, Fujimoto JG, Srinivasan VJ, Duker JS. High-speed, ultra-high-resolution optical coherence tomography of acute macular neuroretinopathy. Br J Ophthalmol. 2007;91:119–20.
Acknowledgments
The authors have no proprietary interests in any of the material used in this study. The authors have no financial support.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Matsuo, Y., Uemura, A., Nakano, T. et al. Atypical presentation of acute macular neuroretinopathy with tiny parafoveal reddish-brown lesions. Jpn J Ophthalmol 55, 362–364 (2011). https://doi.org/10.1007/s10384-011-0028-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10384-011-0028-0