Abstract
Background
Birdshot chorioretinopathy, acute posterior multifocal placoid pigment epitheliopathy, and retinal pigment epithelial detachment have been reported as rare manifestations associated with sarcoidosis, suggesting that ocular sarcoidosis may affect the choroidal circulation. We report a case of ocular sarcoidosis representing a choroidal circulatory disturbance without the appearance of retinal lesions or loss of retinal function.
Case
A 20-year-old woman was referred with blurred vision in the left eye. Inflammatory change in the anterior segment of the eye was noted with multiple nodules on the iris.
Observations
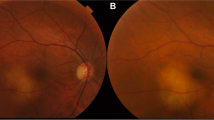
Hematological examination revealed elevated lysozyme levels. Bilateral hilar lymphadenopathy was noted on chest X-ray. Specimens obtained by transbronchial lung biopsy revealed granuloma with Langhans giant cells, which led to the diagnosis of sarcoidosis. The eye was treated with topical steroid. The symptoms and the inflammatory change in the anterior segment disappeared within 10 days. However, despite the normal appearance of the ocular fundus, fluorescein angiography revealed multiple puncta of hyperfluorescence. In indocyanine green angiography, a filling delay was noted in the area corresponding to the punctate lesions. Static visual field testing and multifocal electroretinography showed no significant changes. At the last visit, 15 months after the left eye became asymptomatic, the choroidal lesions had disappeared with no residual alteration of the funduscopic appearance or visual function.
Conclusions
This case indicates that choroidal circulatory disturbance can underlie ocular sarcoidosis even in the absence of funduscopically detectable lesions and loss of visual function.
Similar content being viewed by others
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Machida, S., Tanaka, M., Murai, K. et al. Choroidal Circulatory Disturbance in Ocular Sarcoidosis Without the Appearance of Retinal Lesions or Loss of Visual Function. Jpn J Ophthalmol 48, 392–396 (2004). https://doi.org/10.1007/s10384-004-0087-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10384-004-0087-6