Summary
Background
Our aim was to demonstrate the analgesic efficacy of the bilateral superficial cervical plexus block (BSCPB) combined with bilateral greater occipital nerve block (BGONB) on different sources of pain after thyroid surgery; in terms of pain scores and morphine-PCA consumption in the first 24 h.
Materials and method
Sixty patients were randomized into three groups; Group C (n = 20) to receive management without blocks; Group GS (n = 20), the combination of BSCPB and BGONB; and Group S (n = 20), BSCPB alone. Levobupivacaine of 0.25 % (15 ml (each side) for BSCPB; 5 ml (each side) BGONB) was used for nerve blocks. All patients received morphine-PCA for the first 24 h postoperatively. In all, 0 h, 1 h, 2 h, 4 h, 6 h, 12 h, and 24 h were the measurement times for incision pain at rest, pain on swallowing, headache, and posterior neck pain scores (VAS) and PONV. Requirement for rescue analgesics and 24 h morphine consumption were recorded.
Results
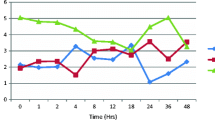
Incision pain scores at rest and on swallowing was lower in Groups GS and S (p < 0.001). Posterior neck pain scores were lower in Group GS (p < 0.001). Headache was similar in all groups, but the number of patients with pain scores VAS > 3 was lower in Group GS (p < 0.001). In Groups GS and S 24 h morphine consumption was lower, compared to Group C (p < 0.001). PONV and rescue analgesic use were similar.
Conclusion
The combination of three-injection technique BSCPB with BGONB performed before surgical incision by using 0.25 % levobupivacaine, significantly reduced incision pain at rest, incision pain on swallowing, headache and posterior neck pain after thyroid surgery, while reducing morphine consumption in 24 h postoperatively.



Similar content being viewed by others
References
Andrieu G, Amrouni H, Robin E, Carnaille B, Wattier JM, Pattou F, et.al. Analgesic efficacy of bilateral superficial cervical plexus block administered before thyroid surgery under general anaesthesia. Br J Anaesth. 2007;99(4):561–6.
Motamed C, Merle JC, Yakhou L, Combes X, Dumerat M, Vodinh J, et.al. Intraoperative i.v. morphine reduces pain scores and length of stay in the post anaesthetic care unit after thyroidectomy. Br J Anaesth. 2004;93(2):306–7.
Gozal Y, Shapira SC, Gozal D, Magora F. Bupivacaine wound infiltration in thyroid surgery reduces postoperative pain and opioid demand. Acta Anaesth Scand. 1994;38:813–5.
Dieudonne N, Gomola A, Bonnichon P, Ozier YM. Prevention of postoperative pain after thyroid surgery: a double blind randomized study of bilateral superficial cervical plexus blocks. Anesth Analg. 2001;92:1538–42.
Aunac S, Carlier M, Singelyn F, De Kock M. The analgesic efficacy of bilateral combined superficial and deep cervical plexus block administered before thyroid surgery under general anesthesia. Anesth Analg. 2002;95(3):746–50.
Shih ML, Duh QY, Hsieh CB, Liu YC, Lu CH, Wong CS, Yu JC, Yeh CC. Bilateral superficial cervical plexus block combined with general anesthesia administered in thyroid operations. World J Surg. 2010;34:2338–43.
Suh YJ, Kim YS, In JH, Joo JD, Jeon YS, Kim HK. Comparison of analgesic efficacy between bilateral Superficial and combined (superficial and deep) cervical plexus block administered before thyroid surgery. Eur J Anaesthesiol. 2009;26:1043–47.
Han DW, Koo BN, Chung WY. Park CS, Kim SY, Palmer P, et.al. Preoperative greater occipital nerve block in total thyroidectomy patients can reduce postoperative occipital headache and posterior neck pain. Thyroid. 2006; 16(6):599–603.
Eti Z, Irmak P, Gulluoglu BM, Manukyan MN, Gogüs FY. Does bilateral superficial cervical plexus block decrease analgesic requirement after thyroid surgery? Anesth Analg. 2006;102:1174–6.
Steffen T, Warschkow R, Brändle M, Tarantino I, Clerici T. Randomized controlled trial of bilateral superficial cervical plexus block versus placebo in thyroid surgery. Br J Surg. 2010;97:1000–6.
Hadzic A. Section 2. Nerve stimulator and surface-based nerve block techniques. Chapter 11. Cervical plexus block. In: Hadzic A, editor. Hadzic’s peripheral nerve blocks and anatomy for ultrasound-guided regional anesthesia. 2 ed. China: McGraw-Hill; 2011. pp. 139–48.
Kesisoglou I, Papavramidis TS, Michalopoulos N, Ioannidis K, Trikoupi A, Sapalidis K, et al. Superfıcıal selectıve cervıcal plexus block followıng total thyroıdectomy: a randomızed trıal. Head Neck. 2010;32(8):984–8.
1Herbland A, Cantini O, Reynier P, Valat P, Jougon J, Arimone Y, et al. The bilateral superficial cervical plexus block with 0.75 % ropivacaine administered before or after surgery does not prevent postoperative pain after total thyroidectomy. Reg Anesth Pain Med. 2006; 31(1):34–9.
Pandit JJ, Dutta D, Morris JF. Spread of injectate with superficial cervicalplexus block in humans: an anatomical study. Br J Anaesth. 2003;91:733–5.
Acknowledgements
No funding and no conflicts of interest. We appreciate the work for statistical analysis of Salih Ergocen, MSc.
Funding
None.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
The study was held in ‘Turkish Ministry of Health Ankara Dişkapi Yildirim Beyazit Research and Teaching Hospital, Anesthesiology and Reanimation Clinic, Ankara, Turkey’, while Dr. Filiz Uzumcugil was working there. Dr. Uzumcugil presently works in Hacettepe University School of Medicine, Department of Anesthesiology and Reanimation as an Instructor.
Rights and permissions
About this article
Cite this article
Kılınçkan, F., Uzumcugil, F., Sayın, M. et al. Bilateral superficial cervical plexus block combined with bilateral greater occipital nerve block reduces the impact of different sources of pain after thyroid surgery with less consumption of morphine-PCA: a randomized trial. Eur Surg 47, 181–187 (2015). https://doi.org/10.1007/s10353-015-0322-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10353-015-0322-z