Abstract
Objective
To evaluate the reliability of the standard planimetric methodology of volumetric analysis and three different open-source semi-automated approaches of brain tumor segmentation.
Materials and methods
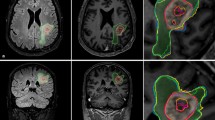
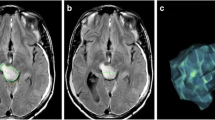
The volumes of subependymal giant cell astrocytomas (SEGA) examined by 30 MRI studies of 10 patients from a previous everolimus-related trial (EMINENTS study) were estimated using four methods: planimetric method (modified MacDonald ellipsoid method), ITK-Snap (pixel clustering, geodesic active contours, region competition methods), 3D Slicer (level-set thresholding), and NIRFast (k-means clustering, Markov random fields). The methods were compared, and a trial simulation was performed to determine how the choice of approach could influence the final decision about progression or response.
Results
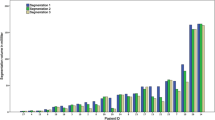
Intraclass correlation coefficient was high (0.95; 95% CI 0.91–0.98). The planimetric method always overestimated the size of the tumor, while virtually no mean difference was found between ITK-Snap and 3D Slicer (P = 0.99). NIRFast underestimated the volume and presented a proportional bias. During the trial simulation, a moderate level of agreement between all the methods (kappa 0.57–0.71, P < 0.002) was noted.
Conclusion
Semi-automated segmentation can ease oncological follow-up but the moderate level of agreement between segmentation methods suggests that the reference standard volumetric method for SEGA tumors should be revised and chosen carefully, as the selection of volumetry tool may influence the conclusion about tumor progression or response.


Similar content being viewed by others
References
Jóźwiak S, Nabbout R, Curatolo P (2013) Management of subependymal giant cell astrocytoma (SEGA) associated with tuberous sclerosis complex (TSC): clinical recommendations. Eur J Paediatr Neurol 17:348–352
Cappellano AM, Senerchia AA, Adolfo F, Paiva PM, Pinho R, Covic A, Cavalheiro S, Saba N (2013) Successful everolimus therapy for SEGA in pediatric patients with tuberous sclerosis complex. Child’s Nerv Syst 29:2301–2305
Eisenhauer EA, Therasse P, Bogaerts J, Schwartz LH, Sargent D, Ford R, Dancey J, Arbuck S, Gwyther S, Mooney M, Rubinstein L, Shankar L, Dodd L, Kaplan R, Lacombe D, Verweij J (2009) New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer 45:228–247
Franz DN, Agricola K, Mays M, Tudor C, Care MM, Holland-Bouley K, Berkowitz N, Miao S, Peyrard S, Krueger DA (2015) Everolimus for subependymal giant cell astrocytoma: 5-year final analysis. Ann Neurol 78:929–938
Menze BH, Jakab A, Bauer S, Kalpathy-Cramer J, Farahani K, Kirby J, Burren Y, Porz N, Slotboom J, Wiest R, Lanczi L, Gerstner E, Weber MA, Arbel T, Avants BB, Ayache N, Buendia P, Collins DL, Cordier N, Corso JJ, Criminisi A, Das T, Delingette H, Demiralp Ç, Durst CR, Dojat M, Doyle S, Festa J, Forbes F, Geremia E, Glocker B, Golland P, Guo X, Hamamci A, Iftekharuddin KM, Jena R, John NM, Konukoglu E, Lashkari D, Mariz JA, Meier R, Pereira S, Precup D, Price SJ, Raviv TR, Reza SMS, Ryan M, Sarikaya D, Schwartz L, Shin HC, Shotton J, Silva CA, Sousa N, Subbanna NK, Szekely G, Taylor TJ, Thomas OM, Tustison NJ, Unal G, Vasseur F, Wintermark M, Ye DH, Zhao L, Zhao B, Zikic D, Prastawa M, Reyes M, Van Leemput K (2015) The multimodal brain tumor image segmentation benchmark (BRATS). IEEE Trans Med Imaging 34:1993–2024
Gordillo N, Montseny E, Sobrevilla P (2013) State of the art survey on MRI brain tumor segmentation. Magn Reson Imaging 31:1426–1438
Trelinska J, Dachowska I, Baranska D, Stawiski K, Kotulska K, Fendler W, Jozwiak S, Mlynarski W (2016) Maintenance therapy with everolimus for subependymal giant cell astrocytoma in patients with tuberous sclerosis (the EMINENTS study). Pediatr Blood Cancer 1–7. doi:10.1002/pbc.26347
Therasse P, Arbuck SG, Eisenhauer EA, Wanders J, Kaplan RS, Rubinstein L, Verweij J, Van Glabbeke M, van Oosterom AT, Christian MC, Gwyther SG (2000) New guidelines to evaluate the response to treatment in solid tumors. J Natl Cancer Inst 92:205–216
Yushkevich PA, Piven J, Hazlett HC, Smith RG, Ho S, Gee JC, Gerig G (2006) User-guided 3D active contour segmentation of anatomical structures: significantly improved efficiency and reliability. Neuroimage 31:1116–1128
Fedorov A, Beichel R, Kalpathy-Cramer J, Finet J, Fillion-Robin JC, Pujol S, Bauer C, Jennings D, Fennessy F, Sonka M, Buatti J, Aylward S, Miller JV, Pieper S, Kikinis R (2012) 3D Slicer as an image computing platform for the quantitative imaging network. Magn Reson Imaging 30:1323–1341
Byrne N, Velasco Forte M, Tandon A, Valverde I, Hussain T (2016) A systematic review of image segmentation methodology, used in the additive manufacture of patient-specific 3D printed models of the cardiovascular system. JRSM Cardiovasc Dis 5:1–9
Dehghani H, Eames ME, Yalavarthy PK, Davis SC, Srinivasan S, Carpenter CM, Pogue BW, Paulsen KD (2009) Near infrared optical tomography using NIRFAST: algorithm for numerical model and image reconstruction. Commun Numer Methods Eng 25:711–732
Jermyn M, Ghadyani H, Mastanduno MA, Turner W, Davis SC, Dehghani H, Pogue BW (2013) Fast segmentation and high-quality three-dimensional volume mesh creation from medical images for diffuse optical tomography. J Biomed Opt 18:86007
Sedgwick P (2013) Limits of agreement (Bland–Altman method). BMJ Br Med J 1630:1–2
Jones M, Dobson A, O’brian S (2011) A graphical method for assessing agreement with the mean between multiple observers using continuous measures. Int J Epidemiol 40:1308–1313
Trelinska J, Dachowska I, Kotulska K, Baranska D, Fendler W, Jozwiak S, Mlynarski W (2015) Factors affecting response to everolimus therapy for subependymal giant cell astrocytomas associated with tuberous sclerosis. Pediatr Blood Cancer 62:616–621
Wetzel SG, Johnson G, Tan AGS, Cha S, Knopp EA, Lee VS, Thomasson D, Rofsky NM (2002) Three-dimensional, T1-weighted gradient-echo imaging of the brain with a volumetric interpolated examination. Am J Neuroradiol 23:995–1002
Takeda T, Takeda A, Nagaoka T, Kunieda E, Takemasa K, Watanabe M, Hatou T, Oguro S, Katayama M (2008) Gadolinium-enhanced three-dimensional magnetization-prepared rapid gradient-echo (3D MP-RAGE) imaging is superior to spin-echo imaging in delineating brain metastases. Acta Radiol 49:1167–1173
Markl M, Leupold J (2012) Gradient echo imaging. J Magn Reson Imaging 35:1274–1289
Cromb A, Saranathan M, Ruet A, Durieux M, De Roquefeuil E, Ouallet JC, Brochet B, Dousset V, Tourdias T (2015) MS lesions are better detected with 3D T1 gradient-echo than with 2D T1 spin-echo gadolinium-enhanced imaging at 3T. Am J Neuroradiol 36:501–507
Weissheimer A, De Menezes LM, Sameshima GT, Enciso R, Pham J, Grauer D (2012) Imaging software accuracy for 3-dimensional analysis of the upper airway. Am J Orthod Dentofac Orthop 142:801–813
Larjani S, Monsalves E, Pebdani H, Krischek B, Gentili F, Cusimano M, Laperriere N, Hayhurst C, Zadeh G (2014) Identifying predictors of early growth response and adverse radiation effects of vestibular schwannomas to radiosurgery. PLoS One 9:e110823
Yuan Q, Rubic M, Seah J, Rae C, Wright IMR, Kaltenbach K, Feller JM, Abdel-Latif ME, Chu C, Oei JL (2014) Do maternal opioids reduce neonatal regional brain volumes? A pilot study. J Perinatol 34:909–913
Liu X, Tuncali K, Wells WM, Morrison PR, Zientara GP (2012) Fully automatic 3D segmentation of iceball for image-guided cryoablation. In: Proc Annu Int Conf IEEE Eng Med Biol Soc EMBS 2012, pp 2327–2330
Follwell MJ, Khu KJ, Cheng L, Xu W, Mikulis DJ, Millar B-A, Tsao MN, Laperriere NJ, Bernstein M, Sahgal A (2012) Volume specific response criteria for brain metastases following salvage stereotactic radiosurgery and associated predictors of response. Acta Oncol (Madr) 51:629–635
Egger J, Kapur T, Fedorov A, Pieper S, Miller JV, Veeraraghavan H, Freisleben B, Golby AJ, Nimsky C, Kikinis R (2013) GBM volumetry using the 3D Slicer medical image computing platform. Sci Rep 3:1364
Dang M, Modi J, Roberts M, Chan C, Mitchell JR (2013) Validation study of a fast, accurate, and precise brain tumor volume measurement. Comput Methods Progr Biomed 111:480–487
Juan-Albarracín J, Fuster-Garcia E, Manjón JV, Robles M, Aparici F, Martí-Bonmatí L, García-Gómez JM (2015) Automated glioblastoma segmentation based on a multiparametric structured unsupervised classification. PLoS One 10:e0125143
Hu T-T, Yan L, Yan P-F, Wang X, Yue G-F (2015) Assessment of the ABC/2 method of epidural hematoma volume measurement as compared to computer-assisted planimetric analysis. Biol Res Nurs 18(1):5–1
Author’s contribution
Stawiski—protocol/project development, data analysis; Trelinska—protocol/project development, data collection or management; Baranska—protocol/project development, data collection or management; Dachowska—data collection or management; Kotulska—data collection or management; Jozwiak—data collection or management, critical review; Fendler—protocol/project development, data analysis, critical review; Mlynarski—data collection or management, critical review.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study was previously approved by the Bioethics Committee of the Medical University of Lodz (# RNN/306/13/KE).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflicts of interest
The authors declare that they have no conflict of interest.
Ethical standard
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Funding
The project is financed by the National Science Center grant number 2015/19/B/NZ5/02229.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Stawiski, K., Trelińska, J., Baranska, D. et al. What are the true volumes of SEGA tumors? Reliability of planimetric and popular semi-automated image segmentation methods. Magn Reson Mater Phy 30, 397–405 (2017). https://doi.org/10.1007/s10334-017-0614-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10334-017-0614-3