Abstract
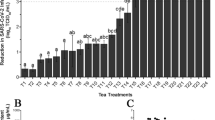
Porphyromonas gingivalis is a keystone pathogen and major colonizer in host tissue which plays a pivotal role in periodontitis among the other polymicrobial infections. Increasing facts demonstrate that curcumin has antibacterial activity and anti-biofilm effect against the periodontopathogens through diverse mechanisms that have a positive impact on periodontal health. The present study was aimed to elucidate the effect of curcumin on biofilm formation and virulence factor gene expression of P. gingivalis. By using gene expression studies, we exploited the mechanism of anti-biofilm effects of curcumin on P. gingivalis. The minimum inhibitory concentration and minimum bactericidal concentration of curcumin for both ATCC and clinical strains of P. gingivalis were found to be 62.5 and 125 µg ml−1 respectively. Curcumin prevented bacterial adhesion and biofilm formation in a dose-dependent manner. Further, curcumin attenuated the virulence of P. gingivalis by reducing the expression of genes coding for major virulence factors, including adhesions (fimA, hagA, and hagB) and proteinases (rgpA, rgpB, and kgp). The results indicated that curcumin has shown anti-biofilm as well as antibacterial activity against P. gingivalis. Further, curcumin because of its pleiotropic actions could be a simple and inexpensive therapeutic strategy in the treatment of periodontal disease.







Similar content being viewed by others
References
Shahzad M, Millhouse E, Culshaw S, Edwards CA, Ramage G, Combet E. Selected dietary (poly) phenols inhibit periodontal pathogen growth and biofilm formation. Food Funct. 2015;6(3):719–29. https://doi.org/10.1039/C4FO01087F.
Tonetti MS, Jepsen S, Jin L. Otomo-Corgel J Impact of the global burden of periodontal diseases on health, nutrition and wellbeing of mankind: a call for global action. J Clin Periodontol. 2017;44(5):456–62. https://doi.org/10.1111/jcpe.12732.
Sakanaka A, Takeuchi H, Kuboniwa M, Amano A. Dual lifestyle of Porphyromonas gingivalis in biofilm and gingival cells. Microb Pathog. 2016;94:42–7. https://doi.org/10.1016/j.micpath.2015.10.003.
Kim J, Amar S. Periodontal disease and systemic conditions: a bidirectional relationship. Odontology. 2006;94(1):10–211. https://doi.org/10.1007/s10266-006-0060-6.
How KY, Song KP, Chan KG. Porphyromonas gingivalis: an overview of periodontopathic pathogen below the gum line. Front Microbiol. 2016;7:53. https://doi.org/10.3389/fmicb.2016.00053.
Warinner C, Rodrigues JFM, Vyas R, Trachsel C, Shved N, Grossmann J, Radini A, Hancock Y, Tito RY, Fiddyment S, Speller C, et al. Pathogens and host immunity in the ancient human oral cavity. Nature Genet. 2014;46(4):336–44. https://doi.org/10.1038/ng.2906.
Pandit N, Changela R, Bali D, Tikoo P, Gugnani S. Porphyromonas gingivalis: its virulence and vaccine. J Int Clin Dent Res Org. 2015;7(1):51. https://doi.org/10.4103/2231-0754.153496.
Connolly E, Millhouse E, Doyle R, Culshaw S, Ramage G, Moran GP. The Porphyromonas gingivalis hemagglutinins HagB and HagC are major mediators of adhesion and biofilm formation. Mol Oral Microbiol. 2017;32(1):35–47. https://doi.org/10.1111/omi.12151.
Li N, Collyer CA. Gingipains from Porphyromonas gingivalis-complex domain structures confer diverse functions. Eur J Microbiol Immunol. 2011;1(1):41–58. https://doi.org/10.1556/EuJMI.1.2011.1.7.
Laheij AM, Van Loveren C, Deng D, de Soet JJ. The impact of virulence factors of Porphyromonas gingivalis on wound healing in vitro. J Oral Microbiol. 2015;7(1):27543. https://doi.org/10.3402/jom.v7.27543.
Tanwar J, Hungund S, Dodani K. Nonsurgical periodontal therapy: a review. J Oral Res Rew. 2016;8(1):39. https://doi.org/10.4103/2249-4987.182490.
Slots J, Ting M. Systemic antibiotics in the treatment of periodontal disease. Periodontol 2000. 2000;28(1):106–76. https://doi.org/10.1034/j.1600-0757.2002.280106.x.
Torwane NA, Hongal S, Goel P, Chandrashekar BR. Role of Ayurveda in management of oral health. Pharmacogn Rev. 2014;8(15):16–211. https://doi.org/10.4103/0973-7847.125518.
Peram MR, Jalalpure SS, Joshi SA, Palkar MB, Diwan PV. Single robust RP-HPLC analytical method for quantification of curcuminoids in commercial turmeric products, Ayurvedic medicines, and nanovesicular systems. J Liq Chromatogr Relat Technol. 2017;40(10):487–98. https://doi.org/10.1080/10826076.2017.1329742.
Mandroli PS, Bhat K. An in-vitro evaluation of antibacterial activity of curcumin against common endodontic bacteria. J Appl Pharm Sci. 2013;3(10):106–8. https://doi.org/10.7324/JAPS.2013.31018.
Li B, Li X, Lin H, Zhou Y. Curcumin as a promising antibacterial agent: effects on metabolism and biofilm formation in S. mutans. BioMed Res Int. 2018. https://doi.org/10.1155/2018/4508709.
Izui S, Sekine S, Maeda K, Kuboniwa M, Takada A, Amano A, Nagata H. Antibacterial activity of curcumin against periodontopathic bacteria. J Periodontol. 2016;87(1):83–90. https://doi.org/10.1902/jop.2015.150260.
Wayne PA Clinical and laboratory standards institute. Performance standards for antimicrobial susceptibility testing. Twenty-third informational supplement CLSI document, 2011; 33(1) CLSI: USA M100-S23, 2013
Nalawade TM, Bhat KG, Sogi S. Antimicrobial activity of endodontic medicaments and vehicles using agar well diffusion method on facultative and obligate anaerobes. Int J Clin Pediatr Dent. 2016;9(4):335–41. https://doi.org/10.5005/jp-journals-10005-1388.
Kugaji MS, Kumbar VM, Peram MR, Patil S, Bhat KG, Diwan PV. Effect of resveratrol on biofilm formation and virulence factor gene expression of Porphyromonas gingivalis in periodontal disease. Apmis. 2019;127(4):187–95. https://doi.org/10.1111/apm.12930.
Jin Y, Samaranayake LP, Samaranayake Y, Yip HK. Biofilm formation of Candida albicans is variably affected by saliva and dietary sugars. Arch Oral Biol. 2004;49(10):789–98. https://doi.org/10.1016/j.archoralbio.2004.04.011.
Sandasi M, Leonard CM, Viljoen AM. The in vitro antibiofilm activity of selected culinary herbs and medicinal plants against Listeria monocytogenes. Lett Appl Microbiol. 2010;50(1):30–5. https://doi.org/10.1111/j.1472-765X.2009.02747.x.
Shukla SK, Rao TS. An improved crystal violet assay for biofilm quantification in 96-well microtitre plate. BioRxiv. 2017. https://doi.org/10.1101/100214.
Jaiswal S, Mishra P. Antimicrobial and antibiofilm activity of curcumin-silver nanoparticles with improved stability and selective toxicity to bacteria over mammalian cells. Med Microbiol Immunol. 2018;207(1):39–533. https://doi.org/10.1007/s00430-017-0525-y.
Grenier D, Morin MP, Fournier Larente J, Chen H. Vitamin D inhibits the growth of and virulence factor gene expression by Porphyromonas gingivalis and blocks activation of the nuclear factor kappa B transcription factor in monocytes. J Periodontal Res. 2016;51(3):359–65. https://doi.org/10.1111/jre.12315.
Shah T, Joshi K, Mishra S, Otiv S, Kumbar V. Molecular and cellular effects of vitamin B12 forms on human trophoblast cells in presence of excessive folate. Biomed Pharmacother. 2016;84:526–34. https://doi.org/10.1016/j.biopha.2016.09.071.
Cowan MM. Plant products as antimicrobial agents. Clin Microbiol Rev. 1999;12(4):564–82. https://doi.org/10.1128/CMR.12.4.564.
Bush K. Antibacterial drug discovery in the 21st century. Clin Microbiol Infect. 2004;10(54):10–7. https://doi.org/10.1111/j.1465-0691.2004.1005.x.
Kala BS, Gunjan C, Disha N, Shobha P. Treatment of periodontal disease-a herbal approach. Int J Pharm Sci Rev Res. 2015;33(2):126–36.
Donlan RM. Biofilms: microbial life on surfaces. Emerg Infect Dis. 2002;8(9):881–90. https://doi.org/10.3201/eid0809.020063.
Joo HS, Otto M. Molecular basis of in vivo biofilm formation by bacterial pathogens. Chem Biol. 2012;19(12):1503–13. https://doi.org/10.1016/j.chembiol.2012.10.022.
Grenier D, Chen H, Lagha AB, Fournier-Larente J, Morin MP. Dual action of myricetin on Porphyromonas gingivalis and the inflammatory response of host cells: a promising therapeutic molecule for periodontal diseases. PLoS ONE. 2015;10(6):e0131758. https://doi.org/10.1371/journal.pone.0131758.
Bao K, Belibasakis GN, Thurnheer T, Aduse-Opoku J, Curtis MA, Bostanci N. Role of Porphyromonas gingivalis gingipains in multi-species biofilm formation. BMC Microbiol. 2014;14:258. https://doi.org/10.1186/s12866-014-0258-7.
Kariu T, Nakao R, Ikeda T, Nakashima K, Potempa J, Imamura T. Inhibition of gingipains and Porphyromonas gingivalis growth and biofilm formation by prenyl flavonoids. J Periodontal Res. 2017;52(1):89–96. https://doi.org/10.1111/jre.12372.
Moran JM, Rodriguez-Velasco FJ, Roncero-Martin R, Vera V, Pedrera-Zamorano JD. Cytotoxic effects of curcumin in osteosarcoma cells. Int J Nanomed. 2014;9:5273–5. https://doi.org/10.2147/IJN.S75005.
Kriebel K, Hieke C, Müller-Hilke B, Nakata M, Kreikemeyer B. Oral biofilms from symbiotic to pathogenic interactions and associated disease-connection of periodontitis and rheumatic arthritis by peptidylarginine deiminase. Front Microbiol. 2018;9:53. https://doi.org/10.3389/fmicb.2018.00053.
Acknowledgements
Authors would like to thank Kancor Ingredients Ltd., India for supplying Curcumin as a gift sample.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there are no conflicts of interest in this study.
Ethical approval
The study was approved by the Institutional Review Board (Certificate No. 1810).
Informed consent
All authors read and agreed to the final manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kumbar, V.M., Peram, M.R., Kugaji, M.S. et al. Effect of curcumin on growth, biofilm formation and virulence factor gene expression of Porphyromonas gingivalis. Odontology 109, 18–28 (2021). https://doi.org/10.1007/s10266-020-00514-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10266-020-00514-y