Abstract
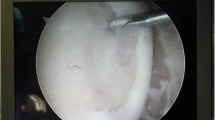
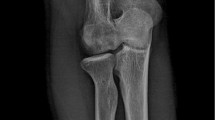
The purpose of our job was to evaluate integration and resumption of physical activities of patients treated with osteochondral transplantation using a synthetic scaffold (Trufit Plug® by Smith&Nephew). In our study we have retrospectively evaluated 30 patients (mean age 31, 8 years) that received a transplant with Trufit Plug® for osteochondral injury between 2006 and 2008. The patients had cartilage injuries with a surface between 0, 5 and 2 cm_; there weren’t side effects of the treatment. The patients were evaluated with generic cards for the state of health (SF-36) and with pathology-specific questionnaires (ICRS, Lysholm score, VAS). The mean value of the Lysholm Score improved from 46, 16 (range 44–68) pre-operatively to 87, 3 (range 79–100) after a mean follow-up of 15 months; using the ICRS, we have observed very good results in 30% (9 patients), good results in 50% (15 patients) and acceptable results in 16, 66% (5 patient); only in a single case we have observed a bad result. The SF-36 has shown encouraging results regarding functional resumption and perceived state of health. Our arthroscopic second look has allowed us to perform some histological evaluations that have shown extraneous body reactions and a slow process of integration. In conclusion, we believe that the Trufit Plug® can be suitable in cases of focal injury of limited size (within 10 mm) with involvement of the underlying bone, but a prudent rehabilitative protocol must be observed.
Similar content being viewed by others
References
Hunter W (1743) Of the structure and disease of articulating cartilages. Philos Trans R Soc Lond B Biol Sci 9:267
Curl WW, Krome J, Gordon ES et al (1997) Cartilage injuries: a review of 31,516 knee arthroscopies. Arthroscopy 13:456–460
Guettler JH, Demetropoulos CK, Yang KH, Jurist KA (2004) Osteochondral defects in the human knee: influence of defect size on cartilage rim stress and load redistribution to surrounding cartilage. Am J Sports Med. 32:1451–1458
Alford JW, Cole BJ (2005) Cartilage restoration, part 1: basic science, historical perspective, patient evaluation, and treatment options. Am J Sports Med 33:295–306
Noyes FR, Bassett RW, Grood ES, Butler DL (1980) Arthroscopy in acute traumatic hemarthrosis of the knee. Incidence of anterior cruciate tears and other injuries. J Bone Joint Surg Am 62:687–695
Bauer M, Jackson RW (1988) Chondral lesions of the femoral condyles: a system of arthroscopic classification. Arthroscopy 4:97–102
Alford JW, Cole BJ (2005) Cartilage restoration, part 2: techniques, outcomes, and future directions. Am J Sports Med 33:443–460
Lu L et al (2001) Effects of dynamic fluid pressure on chondrocytes cultured in polymer scaffolds. Trans Soc Biomater 24:254
Saris DB, Sanyal A, An KN et al (1999) Periosteum responds to dynamic fluid pressure by proliferating in vitro. J Orthop Res 17:668–677
Lu L, Zhu X, Valenzuela RG et al (2001) Biodegradable polymer scaffolds for cartilage tissue engineering. Clin Orthop 391[Suppl.]:251–270
Schlichting K, Schell H, Kleemann RU et al (2008) Influence of scaffold stiffness on subchondral bone and subsequent cartilage regeneration in an ovine model of osteochondral defect healing. Am J Sports Med 36:2379–2391
Apolone G, Mosconi P, Ware JE Jr (1997) Questionario sullo stato di salute SF-36. Guerini e Associati, Milano
International Cartilage Repair Society (ICRS) cartilage injury evaluation package. Articular cartilage classification. www.cartilage.org/files/ICRS_evaluation.pdf
Minas T (1998) Autologous cultured chondrocyte implantation in the repair of focal chondral lesions of the knee: clinical indications and operative technique. J Sports Traumatol 20:90–102
McDermott AG, Langer F, Pritzker KP, Gross AE (1985) Fresh small-fragment osteochondral allografts. Long-term follow-up study on first 100 cases. Clin Orthop 197:96–102
Matsusue Y, Yamamuro T, Hama H (1993) Arthroscopic multiple osteochondral transplantation to the chondral defect in the knee associated with anterior cruciate ligament disruption. Arthroscopy 9:318–321
Hangody L, Kish G, Kárpáti Z (1998) Mosaicplasty for the treatment of osteochondritis dissecans of the knee. J Sports Traumatol 20:126–133
Rieppo J, Hyttinen MM, Halmesmak IE et al (2004) Remodelation of collagen network architecture during cartilage maturation. Transactions Orthop Res Soc 29:549
Hu J, Feng K, Liu X, Ma PX (2009) Chondrogenic and osteogenic differentiations of human bone marrow-derived mesenchymal stem cells on a nanofibrous scaffold with designed pore network. Biomaterials Jun 27 [Epub ahead of print]
Spadaccio C, Rainer A, Trombetta M et al (2009) Poly-L-lactic acid/hydroxyapatite electrospun nanocomposites induce chondrogenic differentiation of human MSC. Ann Biomed Eng 37:1376–1389
Hutmacher DW (2000) Scaffolds in tissue engineering bone and cartilage. Biomaterials 21:2529–2543
Falcone L et al (2008) Cartilagine articolare ingegnerizzata: l’importanza di uno scaffold. Nuove frontiere. Artroscopia 8:55
Carmont MR, Carey-Smith R, Saithna A et al (2009) Delayed incorporation of a TruFit plug: perseverance is recommended. Arthroscopy 25:810–814
Author information
Authors and Affiliations
About this article
Cite this article
Adriani, E., Alfieri, A., Di Paola, B. et al. Trattamento delle lesioni osteocondrali focali con Trufit Plug® di Smith&Nephew: esperienza preliminare. Arch Ortop Reumatol 120, 32–34 (2009). https://doi.org/10.1007/s10261-009-0050-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10261-009-0050-7