Abstract
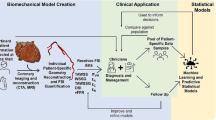
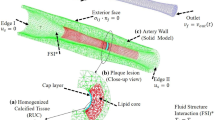
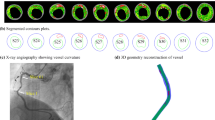
Patient-specific biomechanical modeling of atherosclerotic arteries has the potential to aid clinicians in characterizing lesions and determining optimal treatment plans. To attain high levels of accuracy, recent models use medical imaging data to determine plaque component boundaries in three dimensions, and fluid–structure interaction is used to capture mechanical loading of the diseased vessel. As the plaque components and vessel wall are often highly complex in shape, constructing a suitable structured computational mesh is very challenging and can require a great deal of time. Models based on unstructured computational meshes require relatively less time to construct and are capable of accurately representing plaque components in three dimensions. These models unfortunately require additional computational resources and computing time for accurate and meaningful results. A two-stage modeling strategy based on unstructured computational meshes is proposed to achieve a reasonable balance between meshing difficulty and computational resource and time demand. In this method, a coarsegrained simulation of the full arterial domain is used to guide and constrain a fine-scale simulation of a smaller region of interest within the full domain. Results for a patient-specific carotid bifurcation model demonstrate that the two-stage approach can afford a large savings in both time for mesh generation and time and resources needed for computation. The effects of solid and fluid domain truncation were explored, and were shown to minimally affect accuracy of the stress fields predicted with the two-stage approach.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Bluestein D, Alemu Y et al (2008) Influence of microcalcifications on vulnerable plaque mechanics using FSI modeling. J Biomech 41: 1111–1118
Chau AH, Chan RC et al (2004) Mechanical analysis of atherosclerotic plaques based on optical coherence tomography. Ann Biomed Eng 32(11): 1494–1503
Cheng GC, Loree HM et al (1993) Distribution of circumferential stress in ruptured and stable atherosclerotic lesions. A structural analysis with histopathological correlation. Circulation 87(4): 1179–1187
de Weert TT, de Monye C et al (2008) Assessment of atherosclerotic carotid plaque volume with multidetector computed tomography angiography. Int J Cardiovasc Imaging 24(7): 751–759
de Weert TT, Ouhlous M et al (2006) In vivo characterization and quantification of atherosclerotic carotid plaque components with multidetector computed tomography and histopathological correlation. Arterioscler Thromb Vasc Biol 26(10): 2366–2372
Forrester JS (2007) The pathogenesis of atherosclerosis and plaque instability. In: Holtzman JL (eds) Atherosclerosis and oxidant stress: a new perspective. Springer, New York
Holzapfel GA, Gasser TC et al (2000) A new constitutive framework for arterial wall mechanics and a comparative study of material models. J Elast 61: 1–48
Holzapfel GA, Sommer G (2004) Anisotropic mechanical properties of tissue components in human atherosclerotic plaques. J Biomech Eng 126: 657–665
Huang H, Virmani R et al (2001) The impact of calcification on the biomechanical stability of atherosclerotic plaques. Circulation 103: 1051–1056
Humphrey JD (2002) Cardiovascular solid mechanics : cells, tissues, and organs. Springer, New York
Kaazempur-Mofrad MR, Isasi AG et al (2004) Characterization of the atherosclerotic carotid bifurcation using MRI, finite element modeling, and histology. Ann Biomed Eng 32(7): 932–946
Kock SA, Nygaard JV et al (2008) Mechanical stresses in carotid plaques using MRI-based fluid–structure interaction models. J Biomech 41(8): 1651–1658
Lafont A (2003) Basic aspects of plaque vulnerability. Heart 89(10): 1262–1267
Lee RT, Grodzinsky AJ et al (1991) Structure-dependent dynamic mechanical behavior of fibrous caps from human atherosclerotic plaques. Circulation 83(5): 1764–1770
Li ZY, Howarth SP et al (2007) Structural analysis and magnetic resonance imaging predict plaque vulnerability: a study comparing symptomatic and asymptomatic individuals. J Vasc Surg 45(4): 768–775
Loree HM, Kamm RD et al (1992) Effects of fibrous cap thickness on peak circumferential stress in model atherosclerotic vessels. Circ Res 71: 850–858
Richardson PD (2002) Biomechanics of plaque rupture: progress, problems, and new frontiers. Ann Biomed Eng 30: 524–536
Rosamond W, Flegal K et al (2007) Heart disease and stroke statistics-2007 update: a report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation 115(5): e69–e171
Saam T, Hatsukami TS et al (2007) The vulnerable, or high-risk, atherosclerotic plaque: noninvasive MR imaging for characterization and assessment. Radiology 244(1): 64–77
Stoll G, Bendszus M (2006) Inflammation and atherosclerosis: novel insights into plaque formation and destabilization. Stroke 37: 1923–1932
Tang D, Yang C et al (2004a) Effect of a lipid pool on stress/strain distributions in stenotic arteries: 3-D fluid–structure interactions (FSI) models. J Biomech Eng 126(3): 363–370
Tang D, Yang C et al (2004b) 3D MRI-based multicomponent FSI models for atherosclerotic plaques. Ann Biomed Eng 32(7): 947–960
Tang D, Yang C et al (2005) Quantifying effects of plaque structure and material properties on stress distributions in human atherosclerotic plaques using 3D FSI models. J Biomech Eng 127(7): 1185–1194
Tang D, Yang C et al (2008) A negative correlation between human carotid atherosclerotic plaque progression and plaque wall stress: in vivo MRI-based 2D/3D FSI models. J Biomech 41(4): 727–736
Versluis A, Bank AJ et al (2006) Fatigue and plaque rupture in myocardial infarction. J Biomech 39: 339–347
Virmani R, Burke AP et al (2002) Pathology of the unstable plaque. Prog Cardiovasc Dis 44(5): 349–356
Virmani R, Burke AP et al (2006) Pathology of the vulnerable plaque. J Am Coll Cardiol 47(8 Suppl): C13–C18
Yuan C, Kerwin WS (2004) MRI of atherosclerosis. J Magn Reson Imaging 19(6): 710–719
Yushkevich PA, Piven J et al (2006) User-guided 3D active contour segmentation of anatomical structures: significantly improved efficiency and reliability. Neuroimage 31(3): 1116–1128
Acknowledgments
The authors thank Bruno Soares and Max Wintermark for providing medical imaging data. The authors also wish to thank LoicBoussel for help with nodal pressure data comparison. Funding support was provided by the following grants: American Heart Association Pre-doctoral Fellowship 0715072Y (JL), VA MERIT Review Award (DS), and NS059944 from the NINDS.
Open Access
This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License (https://creativecommons.org/licenses/by-nc/2.0), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Leach, J.R., Rayz, V.L., Mofrad, M.R.K. et al. An efficient two-stage approach for image-based FSI analysis of atherosclerotic arteries. Biomech Model Mechanobiol 9, 213–223 (2010). https://doi.org/10.1007/s10237-009-0172-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10237-009-0172-3