Abstract
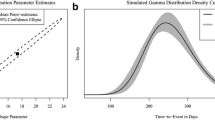
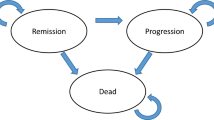
Guidelines of economic evaluations suggest that probabilistic analysis (using probability distributions as inputs) provides less biased estimates than deterministic analysis (using point estimates) owing to the non-linear relationship of model inputs and model outputs. However, other factors can also impact the magnitude of bias for model results. We evaluate bias in probabilistic analysis and deterministic analysis through three simulation studies. The simulation studies illustrate that in some cases, compared with deterministic analyses, probabilistic analyses may be associated with greater biases in model inputs (risk ratios and mean cost estimates using the smearing estimator), as well as model outputs (life-years in a Markov model). Point estimates often represent the most likely value of the parameter in the population, given the observed data. When model parameters have wide, asymmetric confidence intervals, model inputs with larger likelihoods (e.g., point estimates) may result in less bias in model outputs (e.g., costs and life-years) than inputs with lower likelihoods (e.g., probability distributions). Further, when the variance of a parameter is large, simulations from probabilistic analyses may yield extreme values that tend to bias the results of some non-linear models. Deterministic analysis can avoid extreme values that probabilistic analysis may encounter. We conclude that there is no definitive answer on which analytical approach (probabilistic or deterministic) is associated with a less-biased estimate in non-linear models. Health economists should consider the bias of probabilistic analysis and select the most suitable approach for their analyses.



Similar content being viewed by others
References
Briggs, A., Sculpher, M., Claxton, K.: Decision modelling for health economic evaluation. Oxford University Press (2006)
Epstein, D., Onida, S., Bootun, R., Ortega-Ortega, M., Davies, A.H.: Cost-effectiveness of current and emerging treatments of varicose veins. Value Health 21(8), 911–920 (2018). https://doi.org/10.1016/j.jval.2018.01.012
Hamdan, A.: Management of varicose veins and venous insufficiency. JAMA 308(24), 2612–2621 (2012). https://doi.org/10.1001/jama.2012.111352
Canadian Agency for Drugs and Technologies in Health. Guidelines for the economic evaluation of health technologies: Canada. 4th ed. Ottawa (ON); 2017. https://www.cadth.ca/sites/default/files/pdf/guidelines_for_the_economic_evaluation_of_health_technologies_canada_4th_ed.pdf
Institute For Clinical And Economic Review. ICER’s Reference Case for Economic Evaluations: Principles and Rationale. 2018:15. https://icer-review.org/wp-content/uploads/2018/07/ICER_Reference_Case_July-2018.pdf
National Institute for Health and Care Excellence: Methods for the development of NICE public health guidance, 3rd edn. The Institute (2012)
Thompson, K.M., Graham, J.D.: Going beyond the single number: using probabilistic risk assessment to improve risk management. Hum Ecol Risk Assess 2(4), 1008–1034 (1996)
Claxton, K., Sculpher, M., McCabe, C., et al.: Probabilistic sensitivity analysis for NICE technology assessment: not an optional extra. Health Econ. 14(4), 339–347 (2005). https://doi.org/10.1002/hec.985
Kirkwood, B.R., Sterne, J.A.C.: Essential medical statistics. Blackwell Science (2003)
Kasahara, R., Kino, S., Soyama, S., Matsuura, Y.: Noninvasive glucose monitoring using mid-infrared absorption spectroscopy based on a few wavenumbers. Biomed Opt Express 9(1), 289–302 (2018)
Ngamkham, T., Volodin, A., Volodin, I.: Confidence intervals for a ratio of binomial proportions based on direct and inverse sampling schemes. Lobachevskii J Math 34(4), 466–496 (2016). https://doi.org/10.1134/S1995080216040132
Morris, T.P., White, I.R., Crowther, M.J.: Using simulation studies to evaluate statistical methods. Stat Med 38(11), 2074–2102 (2019). https://doi.org/10.1002/sim.8086
Burton, A., Altman, D.G., Royston, P., Holder, R.L.: The design of simulation studies in medical statistics. Stat Med 25(24), 4279–4292 (2006). https://doi.org/10.1002/sim.2673
Wicklin, R.: Simulating data with SAS. SAS Institute Inc (2013)
Krahn, M.D., Bremner, K.E., Zagorski, B., et al.: Health care costs for state transition models in prostate cancer. Med Decis Mak 34(3), 366–378 (2014). https://doi.org/10.1177/0272989X13493970
Duan, N.: Smearing estimate: a non-parametric retransformation method. J Am Stat Assoc 78, 605–610 (1983)
Elbasha, E.H., Chhatwal, J.: Characterizing heterogeneity bias in cohort-based models. Pharmacoeconomics 33(8), 857–865 (2015). https://doi.org/10.1007/s40273-015-0273-z
Naversnik, K., Rojnik, K.: Handling input correlations in pharmacoeconomic models. Value Health 15(3), 540–549 (2012). https://doi.org/10.1016/j.jval.2011.12.008
Author information
Authors and Affiliations
Corresponding authors
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Xie, X., Schaink, A.K., Liu, S. et al. Understanding bias in probabilistic analysis in model-based health economic evaluation. Eur J Health Econ 24, 307–319 (2023). https://doi.org/10.1007/s10198-022-01472-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10198-022-01472-8