Abstract
Background
Dialysis patients often take multiple oral medications, leading to a high pill burden. Phosphate binders (PBs) account for a large proportion of this daily pill burden (DPB). The relationship between DPB and mortality risk remains unclear, and we hypothesized that this relationship might be influenced by the proportion of PBs to all medications.
Methods
We divided DPB into those derived from PBs and non-PB drugs and analyzed the association with mortality risk over a 7-year period in 513 chronic hemodialysis patients using a baseline model.
Results
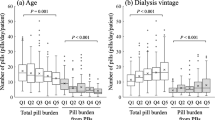
The median (interquartile range) DPB from all drugs was 15.8 (11.2–21.0) pills/day/patient, and the median ratio of PB pills to all drug pills was 29.3 (13.7–45.9)% at baseline. During a median observation period of 5.2 years, 161 patients (31.4%) died. Kaplan–Meier analysis showed no significant difference in all-cause mortality between PB users and non-users. However, a significant survival advantage was observed in the highest tertile of DPB from PBs compared to the lowest tertile. Conversely, the highest tertile of DPB from non-PB drugs was associated with worse survival. Consequently, the highest tertile of the ratio of PBs to all pills was associated with better survival. This association remained significant even after adjusting for patient characteristics in the Cox proportional hazards model. However, when serum nutritional parameters were included as covariates, the significant association disappeared.
Conclusions
Dialysis patients prescribed a higher rate of PB pills to all medications exhibited a lower mortality risk, possibly due to their better nutritional status.

Similar content being viewed by others
References
Sprague SM, Martin KJ, Coyne DW. Phosphate balance and CKD-mineral bone disease. Kidney Int Rep. 2021;6:2049–58.
McCullough PA. Phosphate control: the next frontier in dialysis cardiovascular mortality. Cardiorenal Med. 2021;11:123–32.
Palmer SC, Gardner S, Tonelli M, Mavridis D, Johnson DW, Craig JC, et al. Phosphate-binding agents in adults with CKD: a network meta-analysis of randomized trials. Am J Kidney Dis. 2016;68:691–702.
Isakova T, Gutiérrez OM, Chang Y, Shah A, Tamez H, Smith K, et al. Phosphorus binders and survival on hemodialysis. J Am Soc Nephrol. 2009;20:388–96.
Lopes AA, Tong L, Thumma J, Li Y, Fuller DS, Morgenstern H, et al. Phosphate binder use and mortality among hemodialysis patients in the dialysis outcomes and practice patterns study (DOPPS): evaluation of possible confounding by nutritional status. Am J Kidney Dis. 2012;60:90–101.
Cannata-Andía JB, Fernández-Martín JL, Locatelli F, London G, Gorriz JL, Floege J, et al. Use of phosphate-binding agents is associated with a lower risk of mortality. Kidney Int. 2013;84:998–1008.
Chiu YW, Teitelbaum I, Misra M, de Leon EM, Adzize T, Mehrotra R. Pill burden, adherence, hyperphosphatemia, and quality of life in maintenance dialysis patients. Clin J Am Soc Nephrol. 2009;4:1089–96.
Iwashita Y, Ohya M, Kunimoto S, Iwashita Y, Mima T, Negi S, et al. A survey of drug burden in patients undergoing maintenance hemodialysis in Japan. Intern Med. 2018;57:2937–44.
Murasawa M, Uehara A, Suzuki T, Shimizu S, Kojima S, Uchida D, et al. Association between pill burden and interdialytic weight gain in patients with hemodialysis: a multi-center cross-sectional study. Ther Apher Dial. 2021;25:475–82.
Nagano N, Ito K, Ono T, Ariyoshi Y, Masima S, Kobayashi H, et al. Prescription characteristics of phosphate binders in a high pill burden for hemodialysis patients. Ren Replace Ther. 2021;7:5.
Flythe JE, Katsanos SL, Hu Y, Kshirsagar AV, Falk RJ, Moore CR. Predictors of 30 day hospital readmission among maintenance hemodialysis patients: a hospital’s perspective. Clin J Am Soc Nephrol. 2016;11:1005–14.
Toida T, Toida R, Takahashi R, Uezono S, Komatsu H, Sato Y, et al. Impact of polypharmacy on all-cause mortality and hospitalization in incident hemodialysis patients: a cohort study. Clin Exp Nephrol. 2021;25:1215–23.
Tozawa M, Iseki K, Iseki C, Oshiro S, Higashiuesato Y, Yamazato M, et al. Analysis of drug prescription in chronic haemodialysis patients. Nephrol Dial Transplant. 2002;17:1819–24.
Kitamura M, Yamaguchi K, Ota Y, Notomi S, Komine M, Etoh R, et al. Prognostic impact of polypharmacy by drug essentiality in patients on hemodialysis. Sci Rep. 2021;11:24238.
Carrero JJ, Stenvinkel P, Cuppari L, Ikizler TA, Kalantar-Zadeh K, Kaysen G, et al. Etiology of the protein-energy wasting syndrome in chronic kidney disease: a consensus statement from the international society of renal nutrition and metabolism (ISRNM). J Ren Nutr. 2013;23:77–90.
Toledo FR, Antunes AA, Vannini FC, Silveira LV, Martin LC, Barretti P, et al. Validity of malnutrition scores for predicting mortality in chronic hemodialysis patients. Int Urol Nephrol. 2013;45:1747–52.
Takahashi H, Inoue K, Shimizu K, Hiraga K, Takahashi E, Otaki K, et al. Comparison of nutritional risk scores for predicting mortality in Japanese chronic hemodialysis patients. J Ren Nutr. 2017;27:201–6.
Brown-Tortorici AR, Narasaki Y, You AS, Norris KC, Streja E, Peralta RA, et al. The interplay between dietary phosphorous, protein intake, and mortality in a prospective hemodialysis cohort. Nutrients. 2022;14:3070.
Dalrymple LS, Go AS. Epidemiology of acute infections among patients with chronic kidney disease. Clin J Am Soc Nephrol. 2008;3:1487–93.
Annual dialysis data report. JSDT renal data registry. J Jpn Soc Dial Ther. 2020;53:579–632.
Fissell RB, Karaboyas A, Bieber BA, Sen A, Li Y, Lopes AA, et al. Phosphate binder pill burden, patient-reported non-adherence, and mineral bone disorder markers: findings from the DOPPS. Hemodial Int. 2016;20:38–49.
Vallée M, Weinstein J, Battistella M, Papineau R, Moseley D, Wong G. Multidisciplinary perspectives of current approaches and clinical gaps in the management of hyperphosphatemia. Int J Nephrol Renovasc Dis. 2021;14:301–11.
Doshi SM, Wish JB. Past, present, and future of phosphate management. Kidney Int Rep. 2022;7:688–98.
Covic A, Rastogi A. Hyperphosphatemia in patients with ESRD: assessing the current evidence linking outcomes with treatment adherence. BMC Nephrol. 2013;14:153.
Wang S, Alfieri T, Ramakrishnan K, Braunhofer P, Newsome BA. Serum phosphorus levels and pill burden are inversely associated with adherence in patients on hemodialysis. Nephrol Dial Transplant. 2014;29:2092–9.
Colombijn JMT, Vonk S, Cornelis T, Boorsma S, Krekels MME, Abrahams AC, et al. Impact of phosphate binders on quality of life in dialysis patients: results from the prospective Dutch nocturnal and home dialysis study to improve clinical outcomes study. Nephrology. 2022;27:834–44.
Akizawa T, Sato Y, Ikejiri K, Kanda H, Fukagawa M. Effect of tenapanor on phosphate binder pill burden in hemodialysis patients. Kidney Int Rep. 2021;6:2371–80.
Acknowledgements
We thank Ms. Ayako Minegishi (Pharmaceutical Department, Hidaka Hospital, Gunma, Japan) for her valuable advice regarding the drugs prescribed in this study. We also thank Editage (www.editage.com) for English language editing.
Funding
There is nothing to be declare.
Author information
Authors and Affiliations
Contributions
NN designed the study, analyzed the data, and wrote the first and second draft of the manuscript. KI and TT reviewed and revised the manuscript, and TO is responsible for the final version of the manuscript. CZ, AT, MM, NT, SM, TA, TO, and KI were responsible for drug prescriptions for patients. TO supervised the study. All the authors read and approved the final version of this manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Consultancies: Nobuo Nagano (Kyowa Kirin Co., Ltd and Sanwa Kagaku Kenkyusho Co., Ltd), Honoraria: Nobuo Nagano (Kyowa Kirin Co., Ltd, Torii Pharmaceutical Co., Ltd, and Kissei Pharmaceutical Co., Ltd.). The other authors have declared that no conflict of interest exists.
Ethical approval
All procedures in studies involving human participants were performed in accordance with the ethical standards of the Hidaka Hospital Medical Ethics Committee (approval number: 348) and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This study did not include any animal studies performed by any of the authors.
Informed consent
This was a retrospective analysis of drug prescription and routine blood chemistry records. Individual informed consent was not required, because many patients died or were transferred to other hospitals at the time of application to the institutional ethics committee.
Consent for publication
All authors gave consent for publication to the journal.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
About this article
Cite this article
Nagano, N., Zushida, C., Tagahara, A. et al. Association between phosphate binder pill burden and mortality risk in patients on maintenance hemodialysis: a single-center cohort study with 7-year follow-up of 513 patients. Clin Exp Nephrol 27, 961–971 (2023). https://doi.org/10.1007/s10157-023-02388-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-023-02388-0