Abstract
Background
The number of kidney transplant recipients (KTRs) from diabetic nephropathy (DN) and with cardiovascular disease (CVD) history has increased worldwide. Nevertheless, epidemiologic evidence of CVD in KTRs remains limited.
Methods
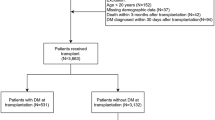
We investigated post-transplant CVD in 1614 adult KTRs between 1990 and 2014. CVD was defined according to the international classification of diseases (ICD-10). All-cause mortality was also investigated. Final follow-up was performed in March 2016. The KTRs were categorized into four groups according to DN and CVD at surgery.
Results
During the follow-up period, 309 KTRs experienced CVDs and 124 KTRs died. The 15-year cumulative CVDs rate was 87% in KTRs with both DN and CVD history, and the rate in KTRs without those was 22.3%. DN and CVD were associated with increased risk of post-transplant CVD [hazard ratio (HR), 3.44; 95% confidence interval (CI), 2.03–5.82; P < 0.001], and the impact marked increased after 7.5 years follow-up period (HR, 16.56; 95% CI, 6.56–41.8; P < 0.001). DN and CVD in KTRs were associated with mortality (HR, 3.32; 95% CI, 1.34–8.22; P = 0.009), and post-transplant CVD was the leading cause (35.5%) of overall death. However, DN and CVD were not associated with increased graft failure rate.
Conclusions
The risk of post-transplant CVDs incidence in KTRs with DN and CVD history is high, and it increases during the late transplant period. Appropriate routine cardiovascular screening and evaluation are needed to reduce late-onset CVD incidence.


Similar content being viewed by others
References
Go AS, Mozaffarian D, Roger VL, Benjamin EJ, Berry JD, Blaha MJ, et al. Heart disease and stroke statistics–2014 update: a report from the American Heart Association. Circulation. 2014;129(3):e28–292.
Grundy SM, Benjamin IJ, Burke GL, Chait A, Eckel RH, Howard BV, et al. Diabetes and cardiovascular disease: a statement for healthcare professionals from the American Heart Association. Circulation. 1999;100(10):1134–46.
Chang SH, Russ GR, Chadban SJ, Campbell SB, McDonald SP. Trends in kidney transplantation in Australia and New Zealand, 1993–2004. Transplantation. 2007;84(5):611–8.
Lim WH, Wong G, Pilmore HL, McDonald SP, Chadban SJ. Long-term outcomes of kidney transplantation in people with type 2 diabetes: a population cohort study. Lancet Diabetes Endocrinol. 2017;5(1):26–33.
Israni AK, Snyder JJ, Skeans MA, Peng Y, Maclean JR, Weinhandl ED, et al. Predicting coronary heart disease after kidney transplantation: Patient Outcomes in Renal Transplantation (PORT) Study. Am J Transplant. 2010;10(2):338–53.
Jardine AG, Gaston RS, Fellstrom BC, Holdaas H. Prevention of cardiovascular disease in adult recipients of kidney transplants. Lancet. 2011;378(9800):1419–27.
Kidney Disease: Improving Global Outcomes Transplant Work G. KDIGO. clinical practice guideline for the care of kidney transplant recipients. Am J Transplant. 2009;9(Suppl 3):S1–155.
Tanaka K, Watanabe T, Takeuchi A, Ohashi Y, Nitta K, Akizawa T, et al. Cardiovascular events and death in Japanese patients with chronic kidney disease. Kidney Int. 2017;91(1):227–34.
Okumi M, Unagami K, Tachibana H, Hirai T, Ishida H, Tanabe K, et al. Association between body mass index and outcomes in Japanese living kidney transplant recipients: the role of sex differences. Int J Urol. 2016;23(9):776–84.
Okumi M, Sato Y, Unagami K, Hirai T, Ishida H, Tanabe K, et al. Preemptive kidney transplantation: a propensity score matched cohort study. Clin Exp Nephrol. 2016;. https://doi.org/10.1007/s10157-016-1345-x.
Okumi M, Toki D, Nozaki T, Shimizu T, Shirakawa H, Omoto K, et al. ABO-Incompatible living kidney transplants: Evolution of Outcomes and Immunosuppressive Management. Am J Transplant. 2016;16(3):886–96.
Matsuo S, Imai E, Horio M, Yasuda Y, Tomita K, Nitta K, et al. Revised equations for estimated GFR from serum creatinine in Japan. Am J Kidney Dis. 2009;53(6):982–92.
Lam NN, Kim SJ, Knoll GA, McArthur E, Lentine KL, Naylor KL, et al. The risk of cardiovascular disease is not increasing over time despite aging and higher comorbidity burden of kidney transplant recipients. Transplantation. 2017;101(3):588–96.
Meier-Kriesche HU, Schold JD, Srinivas TR, Kaplan B. Lack of improvement in renal allograft survival despite a marked decrease in acute rejection rates over the most recent era. Am J Transplant. 2004;4(3):378–83.
Weiner DE, Carpenter MA, Levey AS, Ivanova A, Cole EH, Hunsicker L, et al. Kidney function and risk of cardiovascular disease and mortality in kidney transplant recipients: the FAVORIT trial. Am J Transplant. 2012;12(9):2437–45.
Briggs JD. Causes of death after renal transplantation. Nephrol Dial Transplant. 2001;16(8):1545–9.
Writing Group M, Mozaffarian D, Benjamin EJ, Go AS, Arnett DK, Blaha MJ, et al. Heart Disease and Stroke Statistics-2016 Update: A Report From the American Heart Association. Circulation. 2016;133(4):e38–60.
Goodkin DA, Bragg-Gresham JL, Koenig KG, Wolfe RA, Akiba T, Andreucci VE, et al. Association of comorbid conditions and mortality in hemodialysis patients in Europe, Japan, and the United States: the Dialysis Outcomes and Practice Patterns Study (DOPPS). J Am Soc Nephrol. 2003;14(12):3270–7.
Yoshino M, Kuhlmann MK, Kotanko P, Greenwood RN, Pisoni RL, Port FK, et al. International differences in dialysis mortality reflect background general population atherosclerotic cardiovascular mortality. J Am Soc Nephrol. 2006;17(12):3510–9.
Lentine KL, Costa SP, Weir MR, Robb JF, Fleisher LA, Kasiske BL, et al. Cardiac disease evaluation and management among kidney and liver transplantation candidates: a scientific statement from the American Heart Association and the American College of Cardiology Foundation: endorsed by the American Society of Transplant Surgeons, American Society of Transplantation, and National Kidney Foundation. Circulation. 2012;126(5):617–63.
de Mattos AM, Prather J, Olyaei AJ, Shibagaki Y, Keith DS, Mori M, et al. Cardiovascular events following renal transplantation: role of traditional and transplant-specific risk factors. Kidney Int. 2006;70(4):757–64.
Okumi M, Unagami K, Hirai T, Shimizu T, Ishida H, Tanabe K, et al. Diabetes mellitus after kidney transplantation in Japanese patients: The Japan Academic Consortium of Kidney Transplantation study. Int J Urol. 2017;24(3):197–204.
Kajimoto K, Sato N, Takano T, Investigators A. eGFR and Outcomes in Patients with Acute Decompensated Heart Failure with or without Elevated BUN. Clin J Am Soc Nephrol. 2016;11(3):405–12.
Sarnak MJ, Levey AS, Schoolwerth AC, Coresh J, Culleton B, Hamm LL, et al. Kidney disease as a risk factor for development of cardiovascular disease: a statement from the American Heart Association Councils on Kidney in Cardiovascular Disease, High Blood Pressure Research, Clinical Cardiology, and Epidemiology and Prevention. Circulation. 2003;108(17):2154–69.
Minami Y, Kajimoto K, Sato N, Hagiwara N, Takano T, Investigators As. End-stage renal disease patients on chronic maintenance hemodialysis in a hospitalized acute heart failure cohort: prevalence, clinical characteristics, therapeutic options, and mortality. Int J Cardiol. 2016;224:267–70.
Di Lullo L, Rivera R, Barbera V, Bellasi A, Cozzolino M, Russo D, et al. Sudden cardiac death and chronic kidney disease: from pathophysiology to treatment strategies. Int J Cardiol. 2016;217:16–27.
Foley RN, Parfrey PS, Sarnak MJ. Clinical epidemiology of cardiovascular disease in chronic renal disease. Am J Kidney Dis. 1998;32(5 Suppl 3):S112–9.
Acknowledgments
We appreciate the support provided by Katsunori Shimada, PhD (STATZ Institute, Inc., Tokyo, Japan), who provided expert assistance with statistical analyses.
Astellas Pharma Inc. (Tokyo, Japan) supported this study with a grant. The sponsor was not involved in the study design, patient enrollment, data collection, analysis, interpretation, or preparation of the manuscript.
JACK Investigators
Participating Centers
Department of Urology, Tokyo Women’s Medical University: Kazunari Tanabe (principal investigator), Hideki Ishida, Masashi Inui, Tomokazu Shimizu, Masayoshi Okumi, Toshihito Hirai, and Daisuke Toki.
Department of Nephrology, Tokyo Women’s Medical University: Kohei Unagami.
Department of Transplant Surgery, Kidney Center, Toda Chuo General Hospital: Hiroshi Toma and Kazuya Omoto.
Department of Urology, Ohkubo Hospital: Hiroki Shirakawa.
Transplant Coordinator
Department of Urology, Tokyo Women’s Medical University: Miyuki Furusawa.
Clinical Research Coordinators
Department of Urology, Tokyo Women’s Medical University: Makiko Fujiwara and Kayo Kusubayashi.
Biostatistics and Data Center
Department of Biostatistics, STATZ Institute, Inc., Tokyo, Japan: Katsunori Shimada.
General Management Office
Department of Urology, Tokyo Women’s Medical University: Masayoshi Okumi.
Author information
Authors and Affiliations
Consortia
Contributions
MO performed the research, participated in the data analysis and in writing the manuscript, conducted the research and was responsible for the study’s design. YK participated in the data analysis and revising the manuscript. KU, RM, KM, JI, TT, HI and KT performed the research.
Corresponding author
Ethics declarations
Compliance with ethical standards
The study was carried out according to the principles of the Declaration of Helsinki. This study protocol was approved by the research ethics committee (approval number: 3366-R). Information for the JACK study has been provided in the registration with the University Hospital Medical Information Network (UMIN000018327).
Conflict of interest
None of the authors has any of conflict of interest to declare with regard to the content of this article.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Members of Japan Academic Consortium of Kidney Transplantation are mentioned in Acknowledgements.
About this article
Cite this article
Okumi, M., Kakuta, Y., Unagami, K. et al. Cardiovascular disease in kidney transplant recipients: Japan Academic Consortium of Kidney Transplantation (JACK) cohort study. Clin Exp Nephrol 22, 702–709 (2018). https://doi.org/10.1007/s10157-017-1500-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-017-1500-z