Abstract
Background
Diabetic nephropathy (DMN) is the most common cause of end-stage renal disease. Progression of DMN leads to impairment of physical activity, restriction of daily activities, and diminished social participation. Therefore, the precise assessment of the physical and psychosocial problems of DMN patients is important. The objective of this study was to validate the Comprehensive International Classification of Functioning, Disability and Health Core Set for Diabetes Mellitus (ICF-CS for DM) from the perspective of DMN patients.
Methods
A total of 176 DMN outpatients were interviewed using the ICF-CS for DM. Content and construct validity were evaluated. Patients were divided into 2 groups: DMN patients without hemodialysis (HD) (non-HD group) and DMN patients undergoing HD (HD group). Content validity was evaluated based on the frequency of patients who had a problem in each category. For construct validity, the patients were divided into two groups based on DM duration and hemoglobin A1C levels.
Results
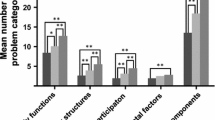
Content validity evaluation revealed 58 categories reported as problem categories: 39 categories in the non-HD group and 50 categories in the HD group. Construct validity evaluation showed that longer DM duration and poor glycemic control contributes to increased problems.
Conclusions
Content and construct validity of the ICF-CS for DM was supported from the DMN patients’ perspective. Some categories of the “Environmental factors” component need further studies to be appropriate.
Similar content being viewed by others
References
Remuzzi G, Schieppatia A, Ruggenenti P. Nephropathy in patients with type 2 diabetes. N Engl J Med. 2002;346:1145–51.
American Diabetes Association. Standards of medical care in diabetes—2009. Diabetes Care. 2009;32:S13–61.
Akinci A, Yildirim A, Gözü H, Sargin H, Orbay E, Sargin M. Assessment of health-related quality of life (HRQoL) of patients with type 2 diabetes in Turkey. Diabetes Res Clin Pract. 2008;79:117–23.
Nakahara R, Yoshiuchi K, Kumano H, Hara Y, Suematsu H, Kuboki T. Prospective study on influence of psychosocial factors on glycemic control in Japanese patients with type 2 diabetes. Psychosomatics. 2006;47:240–6.
World Health Organization. International classification of functioning, disability and health: ICF. Geneva: World Health Organization; 2001.
Stucki G, Ewert T, Cieza A. Value and application of the ICF in rehabilitation medicine. Disabil Rehabil. 2002;24:932–8.
Ruof J, Cieza A, Wolff B, Angst F, Ergeletzis D, Omar Z, et al. ICF Core Sets for diabetes mellitus. J Rehabil Med. 2004;Suppl 44:100–6.
Baden M, Obata Y, Hosokawa Y, Saisho K, Tanba S, Yamamoto K, et al. Evaluation of diabetic polyneuropathy by Pain Vision PS-2100, the device for quantitative analysis of perception and pain. J Japan Diabetes Soc. 2011;54:493–8 (in Japanese).
Schwegler U, Anne J, Boldt C, Glässel A, Lay V, De Boer WE, et al. Aspects of functioning and environmental factors in medical work capacity evaluations of persons with chronic widespread pain and low back pain can be represented by a combination of applicable ICF core sets. BMC Public Health. 2012;12:1088.
Cieza A, Geyh S, Chatterji S, Kostanjsek N, Ustün BT, Stucki G. Identification of candidate categories of the international classification of functioning, disability and health (ICF) for a generic ICF core set based on regression modeling. BMC Med Res Methodol. 2006;6:36.
The research committee of diabetic nephropathy. The renewal of classification by Research Committee of the Japanese Ministry of Health, Labour and Welfare for Disorders of diabetes mellitus. J Jpn Diabetes Soc. 2001;44:623 (in Japanese).
Mirrakhimov AE. Obstructive sleep apnea and kidney disease: is there any direct link? Sleep Breath. 2012;16:1009–16.
Van Steenbergen-Weijenburg KM, van Puffelen AL, Horn EK, Nuyen J, van Dam PS, van Benthem TB, et al. More co-morbid depression in patients with type 2 diabetes with multiple complications. An observational study at a specialized. Diabet Med. 2011;28:86–9.
Soman M, Ganekal S, Nair U, Nair K. Association of systematic comorbidity in diabetic serous macular detachment and comparison of various combination therapies in its management. Clin Ophthalmol. 2013;7:113–9.
Min TZ, Stephens MW, Kumar P, Chudleigh RA. Renal complications of diabetes. Br Med Bull. 2012;104:113–27.
Van Buren PN, Toto RD. The pathogenesis and management of hypertension in diabetic kidney disease. Med Clin N Am. 2013;97:31–51.
Macdonald JH, Fearn L, Jibani M, Marcora SM. Exertional fatigue in patients with CKD. Am J Kidney Dis. 2012;60:930–9.
Viberti GC, Hill RD, Jarrett RJ, Argyropoulos A, Mahmud U, Keen H. Microalbuminuria as a predictor of clinical nephropathy in insulin-dependent diabetes mellitus. Lancet. 1982;1:1430–2.
Goreshi R, Chock M, Foering K, Feng R, Okawa J, Rose M, et al. Quality of life in dermatomyositis. J Am Acad Dermatol. 2011;65:1107–16.
Amatya B, Agrawal S, Dhali T, Sharma S, Pandey SS. Pattern of skin and nail changes in chronic renal failure in Nepal: a hospital-based study. J Dermatol. 2008;35:140–5.
Tsutsui H, Koike T, Yamazaki C, Ito A, Kato F, Sato H, et al. Identification of hemodialysis patients’ common problems using the International Classification of Functioning, Disability and Health. Ther Apher Dial. 2009;13:186–92.
Mueher RJ, Schatell D, Witten B, Gangnon R, Becker BN, Hofmann RM. Factors affecting employments at initiation of dialysis. Clin J Am Soc Nephrol. 2011;6:489–96.
Afsar B, Elsurer R, Sezer S, Ozdemir NF. Dose metabolic syndrome have an impact on the quality of life and mood of hemodialysis patients? J Ren Nutr. 2009;19:365–71.
Covic A, Seica A, Gusbeth-Tatomir P, Gavrilovici O, Goldsmith DJA. Illness representations and quality of life scores in hemodialysis patients. Nephrol Dial Transplant. 2004;19:2078–83.
Acknowledgments
This study was supported by a grant from the Kidney Foundation, Japan (JKF10-5), and a research grant from the Aichi Kidney Foundation. The authors thank the staff members of the following organizations for their clinical support: Ishiguro Internal Medical Clinic, Akishima Clinic, Tawada Hospital, Tawada Clinic, and Sakashita Clinic.
Conflict of interest
The authors declare no conflict of interest with regard to this manuscript.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Tsutsui, H., Ojima, T., Ozaki, N. et al. Validation of the Comprehensive International Classification of Functioning, Disability and Health (ICF) Core Set for Diabetes Mellitus in patients with diabetic nephropathy. Clin Exp Nephrol 19, 254–263 (2015). https://doi.org/10.1007/s10157-014-0983-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-014-0983-0