Abstract
Background
Mortality and renal or cardiovascular prognosis in living kidney donors (LKDs) has been reported to be as same as the general population; however, it is known that the prevalence of hypertension, albuminuria and metabolic syndrome increases after donation. At present, data from Japanese donors are scarce and as a result the actual medical status of LKDs remains unclear. To evaluate cardiovascular disease (CVD) risk factors in Japanese LKDs, we conducted a cross-sectional study on LKDs at our tertiary care hospital and clinic.
Method
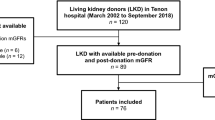
Thirty-six out of 63 LKDs who underwent kidney donation at the kidney disease center of the St. Marianna University Hospital were enrolled. The kidney function, albuminuria, and CVD risk factors including hypertension, dyslipidemia, hyperuricemia, glucose intolerance (GI) and obesity were cross-sectionally investigated.
Results
The kidney function by inulin clearance was 55.2 ± 10.3 ml/min/1.73 m2 on average, indicating that 63.9% of LKDs were categorized into chronic kidney disease (CKD) stage 3 after donation. Albuminuria developed in 16.7%. Blood pressure (BP) was not elevated after donation, but ambulatory BP monitoring revealed that 39.4% of LKDs were categorized as having non-dipper type BP. GI was shown in 25% of LKDs. Prevalence of dyslipidemia and hyperuricemia were 41.7% and 27.8%, respectively. Body mass index was not significantly changed after donation. Seven LKDs (19.4%) were diagnosed with metabolic syndrome.
Conclusion
Many Japanese LKDs were experiencing decreased kidney function corresponding to CKD stage 3. They also had a significant but not lower prevalence of albuminuria and CVD risk compared to the general Japanese population. LKDs should be followed closely with special attention to the management of renal and CVD risk factors.
Similar content being viewed by others
References
Horvat LD, Shariff SZ, Garg AX. Global trends in the rates of living kidney donation. Kidney Int. 2009;75:1088–98.
The Japanese Society for Clinical Renal Transplantation. Annual Progress Report from Japanese Renal Transplant Registry: Number of Renal Transplantation in 2008, part 2. Isyoku. 2009;44:548–58 (in Japanese).
Ibrahim HN, Foley R, Tan L, Rogers T, Bailey RF, Guo H, et al. Long-term consequences of kidney donation. N Engl J Med. 2009;360:459–69.
Segev DL, Muzaale AD, Caffo BS, Mehta SH, Singer AL, Taranto SE, et al. Perioperative mortality and long-term survival following live kidney donation. JAMA. 2010;303:959–66.
Fehrman-Ekholm I, Elinder CG, Stenbeck M, Tyden G, Groth CG. Kidney donors live longer. Transplantation. 1997;64:976–8.
Garg AX, Prasad GV, Thiessen-Philbrook HR, Ping L, Melo M, Gibney EM, Donor Nephrectomy Outcomes Research (DONOR) Network, et al. Cardiovascular disease and hypertension risk in living kidney donors: an analysis of health administrative data in Ontario, Canada. Transplantation. 2008;86:399–406.
Okamoto M, Akioka K, Nobori S, Ushigome H, Kozaki K, Kaihara S, et al. Short- and long-term donor outcomes after kidney donation: analysis of 601 cases over a 35-year period at Japanese single center. Transplantation. 2009;87:419–23.
Kido R, Shibagaki Y, Iwadoh K, Nakajima I, Fuchinoue S, Fujita T, et al. How do living kidney donors develop end-stage renal disease? Am J Transplant. 2009;9:2514–9.
Boudville N, Prasad GV, Knoll G, Muirhead N, Thiessen-Philbrook H, Yang RC, Donor Nephrectomy Outcomes Research (DONOR) Network, et al. Meta-analysis: risk for hypertension in living kidney donors. Ann Intern Med. 2006;145:185–96.
Garg AX, Muirhead N, Knoll G, Yang RC, Prasad GV, Thiessen-Philbrook H, Donor Nephrectomy Outcomes Research (DONOR) Network, et al. Proteinuria and reduced kidney function in living kidney donors: a systematic review, meta-analysis, and meta-regression. Kidney Int. 2006;70:1801–10.
Rizvi SA, Naqvi SA, Jawad F, Ahmed E, Asghar A, Zafar M, et al. Living kidney donor follow-up in a dedicated clinic. Transplantation. 2005;79:1247–51.
Kuzuya T, Nakagawa S, Satoh J, Kanazawa Y, Iwamoto Y, Kobayashi M, et al. Committee of the Japan Diabetes Society on the diagnostic criteria of diabetes mellitus. Report of the Committee on the classification and diagnostic criteria of diabetes mellitus. Diabetes Res Clin Pract. 2002;55:65–85.
National Kidney Foundation. K/DOQI clinical practice guidelines for chronic kidney disease: evaluation, classification, and stratification. Am J Kidney Dis. 2002;39:S1–266.
Horio M, Yasuda Y, Takahara S, Imai E, Watanabe T, Matsuo S. Comparison of a simple and a standard method for inulin renal clearance. Clin Exp Nephrol. 2010;14(5):427–30.
Horio M, Imai E, Yasuda Y, Hishida A, Matsuo S, Japanese Equation for Estimating GFR. Simple sampling strategy for measuring inulin renal clearance. Clin Exp Nephrol. 2009;13:50–4.
Matsuo S, Imai E, Horio M, Yasuda Y, Tomita K, Nitta K, et al. Collaborators developing the Japanese equation for estimated GFR. Revised equations for estimated GFR from serum creatinine in Japan. Am J Kidney Dis. 2009;53:982–92.
Matsuzawa Y. Metabolic syndrome-definition and diagnostic criteria in Japan. J Jpn Soc Med. 2005;94:188–203.
Hakoda M. Epidemiology of hyperuricemia and gout in Japan. Nippon Rinsho. 2008;66:647–52 (in Japanese).
Kido R, Shibagaki Y, Iwadoh K, Nakajima I, Fuchinoue S, Fujita T, et al. Very low but stable glomerular filtration rate after living kidney donation: is the concept of “chronic kidney disease” applicable to kidney donors? Clin Exp Nephrol. 2010;14:356–62.
Kakuta Y, Okumi M, Ichimaru N, Abe T, Nonomura N, Okuyama A, et al. Utility of the Japanese GFR estimation equation for evaluating potential donor kidney function. Clin Exp Nephrol. 2010;14:63–7.
Tan JC, Ho B, Busque S, Blouch K, Derby G, Efron B, et al. Imprecision of creatinine-based GFR estimates in uninephric kidney donors. Clin J Am Soc Nephrol. 2010;5:497–502.
Imai E. Equation for estimating GFR from creatinine in Japan. Nippon Rinsho. 2008;66:1725–9 (in Japanese).
Iseki K. Chronic kidney disease in Japan. Intern Med. 2008;47:681–9.
Imai E, Horio M, Yamagata K, Iseki K, Hara S, Ura N, et al. Slower decline of glomerular filtration rate in the Japanese general population: a longitudinal 10-year follow-up study. Hypertens Res. 2008;31:433–41.
Iseki K, Kinjo K, Iseki C, Takishita S. Relationship between predicted creatinine clearance and proteinuria and the risk of developing ESRD in Okinawa, Japan. Am J Kidney Dis. 2004;44:806–14.
Nakayama M, Metoki H, Terawaki H, Ohkubo T, Kikuya M, Sato T, et al. Kidney dysfunction as a risk factor for first symptomatic stroke events in a general Japanese population—the Ohasama study. Nephrol Dial Transplant. 2007;22:1910–5.
Konta T, Hao Z, Abiko H, Ishikawa M, Takahashi T, Ikeda A, et al. Prevalence and risk factor analysis of microalbuminuria in Japanese general population: the Takahata study. Kidney Int. 2006;70:751–6.
Ogihara T, Kikuchi K, Matsuoka H, Fujita T, Higaki J, Horiuchi M, Japanese Society of Hypertension Committee, et al. The Japanese Society of Hypertension Guidelines for the Management of Hypertension (JSH 2009). Hypertens Res. 2009;32:3–107.
Ohkubo T, Hozawa A, Yamaguchi J, Kikuya M, Ohmori K, Michimata M, et al. Prognostic significance of the nocturnal decline in blood pressure in individuals with and without high 24-h blood pressure: the Ohasama study. J Hypertens. 2002;20:2183–9.
Hoshide S, Kario K, Hoshide Y, Umeda Y, Hashimoto T, Kunii O, et al. Associations between nondipping of nocturnal blood pressure decrease and cardiovascular target organ damage in strictly selected community-dwelling normotensives. Am J Hypertens. 2003;16:434–8.
Eberhard OK, Kliem V, Offner G, Oldhafer K, Fangmann J, Pichlmay R, et al. Assessment of long-term risks for living related kidney donors by 24-h blood pressure monitoring and testing for microalbuminuria. Clin Transplant. 1997;11:415–9.
Fukuda M, Goto N, Kimura G. Hypothesis on renal mechanism of non-dipper pattern of circadian blood pressure rhythm. Med Hypotheses. 2006;67:802–6.
Hakoda M. Epidemiology of hyperuricemia and gout in Japan. Nippon Rinsho. 2008;66:647–52 (in Japanese).
Madero M, Sarnak MJ, Wang X, Greene T, Beck GJ, Kusek JW, et al. Uric acid and long-term outcomes in CKD. Am J Kidney Dis. 2009;53:796–803.
Okamoto M, Suzuki T, Fujiki M, Nobori S, Ushigome H, Sakamoto S, et al. The consequences for live kidney donors with preexisting glucose intolerance without diabetic complication: analysis at a single Japanese center. Transplantation. 2010;89:1391–5.
Muntner P, He J, Astor BC, Folsom AR, Coresh J. Traditional and nontraditional risk factors predict coronary heart disease in chronic kidney disease: results from the atherosclerosis risk in communities study. J Am Soc Nephrol. 2005;16:529–38.
Schaeffner ES, Kurth T, Curhan GC, Glynn RJ, Rexrode KM, Baigent C, et al. Cholesterol and the risk of renal dysfunction in apparently healthy men. J Am Soc Nephrol. 2003;14:2084–91.
Appel GB, Radhakrishnan J, Avram MM, DeFronzo RA, Escobar-Jimenez F, Campos MM, BMRENAAL Study, et al. Analysis of metabolic parameters as predictors of risk in the RENAAL study. Diabetes Care. 2003;26:1402–7.
Delmonico F, Council of the Transplantation Society. A report of the Amsterdam forum on the care of the live kidney donor: data and medical guidelines. Transplantation. 2005;79:S53–66.
Issa N, Stephany B, Fatica R, Nurko S, Krishnamurthi V, Goldfarb DA, et al. Donor factors influencing graft outcomes in live donor kidney transplantation. Transplantation. 2007;83:593–9.
Health and Welfare Statistics Association. J Health Welf Stat. 2009;56:84.
Praga M, Hernandez E, Herrero JC, Morales E, Revilla Y, Diaz-Gonzalez R, et al. Influence of obesity on the appearance of proteinuria and renal insufficiency after unilateral nephrectomy. Kidney Int. 2000;58:2111–8.
Acknowledgments
We sincerely thank Ms. Yumiko Kakuta, chief nurse and orderly of the kidney disease center at St. Marianna University School of Medicine Hospital, for cooperation with inspections.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Yazawa, M., Kido, R., Shibagaki, Y. et al. Kidney function, albuminuria and cardiovascular risk factors in post-operative living kidney donors: a single-center, cross-sectional study. Clin Exp Nephrol 15, 514–521 (2011). https://doi.org/10.1007/s10157-011-0441-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-011-0441-1