Abstract
Background
The pathophysiology of pelvic organ prolapse is largely unknown. We hypothesized that reduced muscle mass on magnetic resonance defecography (MRD) is associated with increased pelvic floor laxity. The aim of this study was to compare the psoas and puborectalis muscle mass composition and cross-sectional area among patients with or without pelvic laxity.
Methods
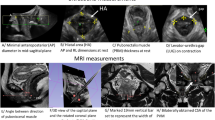
An observational retrospective study was conducted on women > age 18 years old who had undergone MRD for pelvic floor complaints from January 2020 to December 2020 at Stanford Pelvic Health Center. Pelvic floor laxity, pelvic organ descent, and rectal prolapse were characterized by standard measurements on MRD and compared to the psoas (L4 level) and puborectalis muscle index (cross-sectional area adjusted by height) and relative fat fraction, quantified by utilizing a 2-point Dixon technique. Regression analysis was used to quantify the association between muscle characteristics and pelvic organ measurements.
Results
The psoas fat fraction was significantly elevated in patients with abnormally increased resting and strain H and M lines (p < 0.05) and increased with rising grades of Oxford rectal prolapse (p = 0.0001), uterovaginal descent (p = 0.001) and bladder descent (p = 0.0005). In multivariate regression analysis, adjusted for age and body mass index, the psoas fat fraction (not muscle index) was an independent risk factor for abnormal strain H and M line; odds ratio (95% confidence interval) of 17.8 (2–155.4) and 18.5 (1.3–258.3) respectively, and rising Oxford grade of rectal prolapse 153.9 (4.4–5383) and bladder descent 12.4 (1.5–106). Puborectalis fat fraction was increased by rising grades of Oxford rectal prolapse (p = 0.0002).
Conclusions
Severity of pelvic organ prolapse appears to be associated with increasing psoas muscle fat fraction, a biomarker for reduced skeletal muscle mass. Future prospective research is needed to determine if sarcopenia may predict postsurgical outcomes after pelvic organ prolapse repair.



Similar content being viewed by others
References
Mattsson NK, Karjalainen PK, Tolppanen A-M et al (2020) Pelvic organ prolapse surgery and quality of life—a nationwide cohort study. Am J Obstet Gynecol 222:588.e1-588.e10. https://doi.org/10.1016/j.ajog.2019.11.1285
Dieter AA, Wilkins MF, Wu JM (2015) Epidemiological trends and future care needs for pelvic floor disorders. Curr Opin Obstet Gynecol 27:380–384. https://doi.org/10.1097/GCO.0000000000000200
Nygaard I (2008) Prevalence of symptomatic pelvic floor disorders in US women. JAMA 300:1311. https://doi.org/10.1001/jama.300.11.1311
Delancey JOL, Kane Low L, Miller JM et al (2008) Graphic integration of causal factors of pelvic floor disorders: an integrated life span model. Am J Obstet Gynecol 199:610.e1–5. https://doi.org/10.1016/j.ajog.2008.04.001
Handa VL, Lockhart ME, Kenton KS et al (2009) Magnetic resonance assessment of pelvic anatomy and pelvic floor disorders after childbirth. Int Urogynecol J 20:133–139. https://doi.org/10.1007/s00192-008-0736-2
Silva RRL, Coutinho JFV, Vasconcelos CTM et al (2021) Prevalence of sarcopenia in older women with pelvic floor dysfunction. Eur J Obstet Gynecol Reprod Biol 263:159–163. https://doi.org/10.1016/j.ejogrb.2021.06.037
Nygaard IE, Shaw JM (2016) Physical activity and the pelvic floor. Am J Obstet Gynecol 214:164–171. https://doi.org/10.1016/j.ajog.2015.08.067
Wiedmer P, Jung T, Castro JP et al (2020) Sarcopenia—molecular mechanisms and open questions. Ageing Res Rev. https://doi.org/10.1016/j.arr.2020.101200
Cruz-Jentoft AJ, Baeyens JP, Bauer JM et al (2010) Sarcopenia: European consensus on definition and diagnosis: report of the European working group on sarcopenia in older people. Age Ageing 39:412–423. https://doi.org/10.1093/ageing/afq034
Byun S-E, Kim S, Kim K-H, Ha Y-C (2019) Psoas cross-sectional area as a predictor of mortality and a diagnostic tool for sarcopenia in hip fracture patients. J Bone Miner Metab 37:871–879. https://doi.org/10.1007/s00774-019-00986-1
Womer AL, Brady JT, Kalisz K et al (2018) Do psoas muscle area and volume correlate with postoperative complications in patients undergoing rectal cancer resection? Am J Surg 215:503–506. https://doi.org/10.1016/j.amjsurg.2017.10.052
Hanaoka M, Yasuno M, Ishiguro M et al (2017) Morphologic change of the psoas muscle as a surrogate marker of sarcopenia and predictor of complications after colorectal cancer surgery. Int J Colorectal Dis 32:847–856. https://doi.org/10.1007/s00384-017-2773-0
Codari M, Zanardo M, di Sabato ME et al (2020) MRI-derived biomarkers related to sarcopenia: a systematic review. J Magn Reson Imaging 51:1117–1127. https://doi.org/10.1002/jmri.26931
Comiter CV, Vasavada SP, Barbaric ZL et al (1999) Grading pelvic prolapse and pelvic floor relaxation using dynamic magnetic resonance imaging. Urology 54:454–457. https://doi.org/10.1016/S0090-4295(99)00165-X
Derstine BA, Holcombe SA, Ross BE et al (2018) Skeletal muscle cutoff values for sarcopenia diagnosis using T10 to L5 measurements in a healthy US population. Sci Rep 8:11369. https://doi.org/10.1038/s41598-018-29825-5
Collinson R, Cunningham C, D’Costa H, Lindsey I (2009) Rectal intussusception and unexplained faecal incontinence: findings of a proctographic study. Colorectal Dis 11:77–83. https://doi.org/10.1111/j.1463-1318.2008.01539.x
Staller K, Song M, Grodstein F et al (2018) Physical activity, BMI, and risk of fecal incontinence in the nurses’ health study. Clin Transl Gastroenterol 9:e200. https://doi.org/10.1038/s41424-018-0068-6
Dalle S, Rossmeislova L, Koppo K (2017) The role of inflammation in age-related sarcopenia. Front Physiol 8:1045. https://doi.org/10.3389/fphys.2017.01045
Becker L, Nguyen L, Gill J et al (2018) Age-dependent shift in macrophage polarisation causes inflammation-mediated degeneration of enteric nervous system. Gut 67:827–836. https://doi.org/10.1136/gutjnl-2016-312940
Derstine BA, Holcombe SA, Goulson RL et al (2017) Quantifying sarcopenia reference values using lumbar and thoracic muscle areas in a healthy population. J Nutr Health Aging 21:180–185. https://doi.org/10.1007/s12603-017-0983-3
Boutin RD, Yao L, Canter RJ, Lenchik L (2015) Sarcopenia: current concepts and imaging implications. Am J Roentgenol 205:W255–W266. https://doi.org/10.2214/AJR.15.14635
Tseng LA, Delmonico MJ, Visser M et al (2014) Body composition explains sex differential in physical performance among older adults. J Gerontol A Biol Sci Med Sci 69:93–100. https://doi.org/10.1093/gerona/glt027
Brown AD, Li B, Gabriel S et al (2021) Association between sarcopenia and adverse events following transcatheter aortic valve implantation. CJC Open. https://doi.org/10.1016/j.cjco.2021.09.012
Baracos VE (2017) Psoas as a sentinel muscle for sarcopenia: a flawed premise: editorial. J Cachexia Sarcopenia Muscle 8:527–528. https://doi.org/10.1002/jcsm.12221
Burian E, Syväri J, Holzapfel C et al (2018) Gender-and age-related changes in trunk muscle composition using chemical shift encoding-based water−fat MRI. Nutrients. https://doi.org/10.3390/nu10121972
Ding J, Cao P, Chang H-C et al (2020) Deep learning-based thigh muscle segmentation for reproducible fat fraction quantification using fat-water decomposition MRI. Insights Imaging 11:128. https://doi.org/10.1186/s13244-020-00946-8
Acknowledgments
We appreciate Mrs. Nilima Amin-Reddy and Madison McCarthy for their assistance.
Author information
Authors and Affiliations
Contributions
LN and VS designed the study, PL and VS analyzed the data, TL conducted the statistical analysis; BG and LB contributed to the conception and interpretation of data for the work; LN drafted the manuscript. All authors helped with revising the manuscript critically for important intellectual content. All authors have read and approved the final draft submitted.
Corresponding author
Ethics declarations
Conflict of interest
There is no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Neshatian, L., Lam, J.P., Gurland, B.H. et al. MRI biomarker of muscle composition is associated with severity of pelvic organ prolapse. Tech Coloproctol 26, 725–733 (2022). https://doi.org/10.1007/s10151-022-02651-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10151-022-02651-8