Abstract
Background
Transanal total mesorectal excision (TATME) is difficult to learn and can result in serious complications. Current paradigms for assessing performance and competency may be insufficient. This study aims to develop and provide preliminary validity evidence for a TATME virtual assessment tool (TATME-VAT) to assess the cognitive skills necessary to safely complete TATME dissection.
Methods
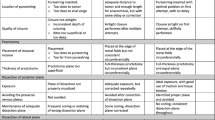
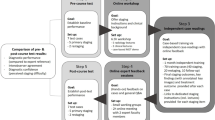
Participants from North America, Europe, Japan and China completed the test via an interactive online platform between 11/2019 and 05/2020. They were grouped into expert, experienced and novice surgeons depending on the number of independently performed TATMEs. TATME-VAT is a 24-item web-based assessment evaluating advanced cognitive skills, designed according to a blueprint from consensus guidelines. Eight items were multiple choice questions. Sixteen items required making annotations on still frames of TATME videos (VCT) and were scored using a validated algorithm derived from experts’ responses. Annotation (range 0–100), multiple choice (range 0–100), and overall scores (sum of annotation and multiple-choice scores, normalized to μ = 50 and σ = 10) were reported.
Results
There were significant differences between the expert, experienced, and novice groups for the annotation (p < 0.001), multiple-choice (p < 0.001), and overall scores (p < 0.001). The annotation (p = 0.439) and overall (p = 0.152) scores were similar between the experienced and novice groups. Annotation scores were higher in participants with 51 or more vs. 30–50 vs. less than 30 cases. Scores were also lower in users with a self-reported recent complication vs. those without.
Conclusions
This study describes the development of an interactive video-based virtual assessment tool for TATME dissection and provides initial validity evidence for its use.



Similar content being viewed by others
Availability of data and material
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
Code availability
Not applicable.
References
Rickles AS, Dietz DW, Chang GJ et al (2015) High rate of positive circumferential resection margins following rectal cancer surgery: a call to action. Ann Surg 262:891–898. https://doi.org/10.1097/sla.0000000000001391
Wibe A, Syse A, Andersen E, Tretli S, Myrvold HE, Søreide O (2004) Oncological outcomes after total mesorectal excision for cure for cancer of the lower rectum: anterior vs. abdominoperineal resection. Dis Colon Rectum 47:48–58. https://doi.org/10.1007/s10350-003-0012-y
Fleshman J, Branda M, Sargent DJ et al (2015) Effect of laparoscopic-assisted resection vs open resection of stage II or III rectal cancer on pathologic outcomes: the ACOSOG Z6051 randomized clinical trial. JAMA 314:1346–1355. https://doi.org/10.1001/jama.2015.10529
Stevenson AR, Solomon MJ, Lumley JW et al (2015) Effect of laparoscopic-assisted resection vs open resection on pathological outcomes in rectal cancer: the ALaCaRT randomized clinical trial. JAMA 314:1356–1363. https://doi.org/10.1001/jama.2015.12009
van der Pas MH, Haglind E, Cuesta MA et al (2013) Laparoscopic versus open surgery for rectal cancer (COLOR II): short-term outcomes of a randomised, phase 3 trial. Lancet Oncol 14:210–218. https://doi.org/10.1016/s1470-2045(13)70016-0
Sylla P, Rattner DW, Delgado S, Lacy AM (2010) NOTES transanal rectal cancer resection using transanal endoscopic microsurgery and laparoscopic assistance. Surg Endosc 24:1205–1210. https://doi.org/10.1007/s00464-010-0965-6
Penna M, Cunningham C, Hompes R (2017) Transanal total mesorectal excision: why, when, and how. Clin Colon Rectal Surg 30:339–345. https://doi.org/10.1055/s-0037-1606111
Penna M, Hompes R, Arnold S et al (2017) Transanal total mesorectal excision: international registry results of the first 720 cases. Ann Surg 266:111–117. https://doi.org/10.1097/sla.0000000000001948
van Oostendorp SE, Belgers HJ, Bootsma BT et al (2020) Locoregional recurrences after transanal total mesorectal excision of rectal cancer during implementation. Br J Surg 107:1211–1220. https://doi.org/10.1002/bjs.11525
Fearnhead NS, Acheson AG, Brown SR et al (2020) The ACPGBI recommends pause for reflection on transanal total mesorectal excision. Colorectal Dis 22:745–748. https://doi.org/10.1111/codi.15143
Larsen SG, Pfeffer F, Korner H, Norwegian Colorectal Cancer G (2019) Norwegian moratorium on transanal total mesorectal excision. Br J Surg 106:1120–1121. https://doi.org/10.1002/bjs.11287
Schlachta CM, Ali S, Ahmed H, Eagleson R (2015) A novel method for assessing visual perception of surgical planes. Can J Surg 58:87–91. https://doi.org/10.1503/cjs.007414
Heald RJ (2013) A new solution to some old problems: transanal TME. Tech Coloproctol 17:257–258. https://doi.org/10.1007/s10151-013-0984-0
Penna M, Whiteford M, Hompes R, Sylla P (2017) Developing and assessing a cadaveric training model for transanal total mesorectal excision: initial experience in the UK and USA. Colorectal Dis 19:476–484. https://doi.org/10.1111/codi.13525
Penna M, Hompes R, Mackenzie H, Carter F, Francis NK (2016) First international training and assessment consensus workshop on transanal total mesorectal excision (taTME). Tech Coloproctol 20:343–352. https://doi.org/10.1007/s10151-016-1454-2
Wynn GR, Austin RCT, Motson RW (2018) Using cadaveric simulation to introduce the concept and skills required to start performing transanal total mesorectal excision. Colorectal Dis 20:496–501. https://doi.org/10.1111/codi.14034
Francis N, Penna M, Mackenzie H, Carter F, Hompes R (2017) Consensus on structured training curriculum for transanal total mesorectal excision (TaTME). Surg Endosc 31:2711–2719. https://doi.org/10.1007/s00464-017-5562-5
Motson RW, Whiteford MH, Hompes R, Albert M, Miles WF (2016) Current status of trans-anal total mesorectal excision (TaTME) following the Second International Consensus Conference. Colorectal Dis 18:13–18. https://doi.org/10.1111/codi.13131
Atallah SB, DuBose AC, Burke JP et al (2017) Uptake of transanal total mesorectal excision in North America: initial assessment of a structured training program and the experience of delegate surgeons. Dis Colon Rectum 60:1023–1031. https://doi.org/10.1097/dcr.0000000000000823
Madani A, Vassiliou MC, Watanabe Y et al (2017) What are the principles that guide behaviors in the operating room?: Creating a framework to define and measure performance. Ann Surg 265:255–267. https://doi.org/10.1097/sla.0000000000001962
Madani A, Grover K, Watanabe Y (2019) Measuring and teaching intraoperative decision-making using the visual concordance test: deliberate practice of advanced cognitive skills. JAMA Surg. https://doi.org/10.1001/jamasurg.2019.4415
Madani A, Gornitsky J, Watanabe Y et al (2018) Measuring decision-making during thyroidectomy: validity evidence for a web-based assessment tool. World J Surg 42:376–383. https://doi.org/10.1007/s00268-017-4322-y
Madani A, Watanabe Y, Bilgic E et al (2017) Measuring intra-operative decision-making during laparoscopic cholecystectomy: validity evidence for a novel interactive Web-based assessment tool. Surg Endosc 31:1203–1212. https://doi.org/10.1007/s00464-016-5091-7
Ogrinc G, Davies L, Goodman D, Batalden P, Davidoff F, Stevens D (2016) SQUIRE 2.0 (Standards for QUality Improvement Reporting Excellence): revised publication guidelines from a detailed consensus process. BMJ Qual Saf 25:986–992. https://doi.org/10.1136/bmjqs-2015-004411
Antoun A, Chau J, Alsharqawi N et al (2020) P338: summarizing measures of proficiency in transanal total mesorectal excision-a systematic review. Surg Endosc. https://doi.org/10.1007/s00464-020-07935-4
Knol J, Chadi SA (2016) Transanal total mesorectal excision: technical aspects of approaching the mesorectal plane from below. Minim Invasive Ther Allied Technol 25:257–270. https://doi.org/10.1080/13645706.2016.1206572
Adamina M, Buchs NC, Penna M, Hompes R (2018) St.Gallen consensus on safe implementation of transanal total mesorectal excision. Surg Endosc 32:1091–1103. https://doi.org/10.1007/s00464-017-5990-2
Atallah S, Albert M, Monson JR (2016) Critical concepts and important anatomic landmarks encountered during transanal total mesorectal excision (taTME): toward the mastery of a new operation for rectal cancer surgery. Tech Coloproctol 20:483–494. https://doi.org/10.1007/s10151-016-1475-x
Tsai AY, Mavroveli S, Miskovic D et al (2019) Surgical quality assurance in COLOR III: standardization and competency assessment in a randomized controlled trial. Ann Surg 270:768–774. https://doi.org/10.1097/SLA.0000000000003537
Leppink J, Perez-Fuster P (2017) We need more replication research—a case for test-retest reliability. Perspect Med Educ 6:158–164. https://doi.org/10.1007/s40037-017-0347-z
Wasmuth HH, Faerden AE, Myklebust TA et al (2020) Transanal total mesorectal excision for rectal cancer has been suspended in Norway. Br J Surg 107:121–130. https://doi.org/10.1002/bjs.11459
van Oostendorp SE, Belgers HJ, Bootsma BT et al (2020) Locoregional recurrences after transanal total mesorectal excision of rectal cancer during implementation. Br J Surg. https://doi.org/10.1002/bjs.11525
Sylla P, Knol JJ, D’Andrea AP et al (2019) Urethral injury and other urologic injuries during transanal total mesorectal excision: an international collaborative study. Ann Surg. https://doi.org/10.1097/SLA.0000000000003597
Caycedo-Marulanda A, Verschoor CP (2020) Experience beyond the learning curve of transanal total mesorectal excision (taTME) and its effect on the incidence of anastomotic leak. Tech Coloproctol 24:309–316. https://doi.org/10.1007/s10151-020-02160-6
Veltcamp Helbach M, van Oostendorp SE, Koedam TWA et al (2020) Structured training pathway and proctoring; multicenter results of the implementation of transanal total mesorectal excision (TaTME) in the Netherlands. Surg Endosc 34:192–201. https://doi.org/10.1007/s00464-019-06750-w
Deijen CL, Tsai A, Koedam TW et al (2016) Clinical outcomes and case volume effect of transanal total mesorectal excision for rectal cancer: a systematic review. Tech Coloproctol 20:811–824. https://doi.org/10.1007/s10151-016-1545-0
Koedam TWA, Veltcamp Helbach M, van de Ven PM et al (2018) Transanal total mesorectal excision for rectal cancer: evaluation of the learning curve. Tech Coloproctol 22:279–287. https://doi.org/10.1007/s10151-018-1771-8
Lee L, Kelly J, Nassif GJ, deBeche-Adams TC, Albert MR, Monson JRT (2020) Defining the learning curve for transanal total mesorectal excision for rectal adenocarcinoma. Surg Endosc 34:1534–1542. https://doi.org/10.1007/s00464-018-6360-4
Alsagheir A, Koziarz A, Belley-Cote EP, Whitlock RP (2021) Expertise-based design in surgical trials: a narrative review. Can J Surg 64:E594–E602. https://doi.org/10.1503/cjs.008520
Birkmeyer JD, Finks JF, O’Reilly A et al (2013) Surgical skill and complication rates after bariatric surgery. N Engl J Med 369:1434–1442. https://doi.org/10.1056/NEJMsa1300625
Meyer VM, Benjamens S, Moumni ME, Lange JFM, Pol RA (2022) Global overview of response rates in patient and health care professional surveys in surgery: a systematic review. Ann Surg 275:e75–e81. https://doi.org/10.1097/SLA.0000000000004078
Banning LBD, Meyer VM, Keupers J, Lange JFM, Pol RA, Benjamens S (2021) Surveys in surgical education: a systematic review and reporting guideline. Eur Surg Res 62:61–67. https://doi.org/10.1159/000516125
Curtis NJ, Foster JD, Miskovic D et al (2020) Association of surgical skill assessment with clinical outcomes in cancer surgery. JAMA Surg 155:590–598. https://doi.org/10.1001/jamasurg.2020.1004
Brajcich BC, Stulberg JJ, Palis BE et al (2020) Association between surgical technical skill and long-term survival for colon cancer. JAMA Oncol. https://doi.org/10.1001/jamaoncol.2020.5462
Gershon RC (2005) Computer adaptive testing. J Appl Meas 6:109–127
Funding
LL is supported by a Career Development Award from the American Society of Colon and Rectal Surgeons (CDA-019).
Author information
Authors and Affiliations
Contributions
Conceptualization: HN, JC, AM, JM, CM, LL. Data acquisition and analysis: HN, JC, PK CM, LL. Interpretation of the data: HN, JC, AM, PK, JM, CM, LL. Drafting of the manuscript: HN, PK, CM, LL. Critical revision: JC, PK, AM, JM, CM, LL. Approval of the final version to be submitted: HN, JC, AM, JK, JM, CM, LL.
Corresponding author
Ethics declarations
Conflict of interest
Dr. Hamzeh Naghawi: No conflicts of interest. Dr. Johnny Chau: No conflicts of interest. Dr. Amin Madani: No conflicts of interest. Ms. Pepa Kaneva: No conflicts of interest. Dr. John Monson: JM reports speaker fees from Applied Medical. Dr. Carmen Mueller: CM reports educational grant from TheatOR. Dr. Lawrence Lee: LL is supported by a Career Development Award from the American Society of Colon and Rectal Surgeons (CDA-019). LL also reports speaker fees from Stryker.
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. Ethics approval for this study has been granted by the McGill University Faculty of Medicine institutional review board under IRB study number A09-E66-18B.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Naghawi, H., Chau, J., Madani, A. et al. Development and evaluation of a virtual knowledge assessment tool for transanal total mesorectal excision. Tech Coloproctol 26, 551–560 (2022). https://doi.org/10.1007/s10151-022-02621-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10151-022-02621-0