Abstract
Background
Da Vinci® Single Port (dvSP) was recently developed. Its application in colorectal surgery is under investigation. The aim of this study was to explore the safety and feasibility of dvSP for intersphincteric (dvSP-ISR), right colectomy (dvSP-RC), and transverse colectomy (dvSP-TC). Surgical indication and short-term results were analyzed.
Methods
All consecutive patients from a prospective database of patients who underwent dvSP-ISR, dvSP-RC, and dvSP-TC at Korea University Anam Hospital from November 2020 to December 2021, were analyzed. Perioperative, pathological, and oncological short-term outcomes were analyzed.
Results
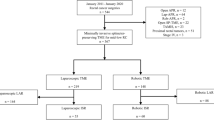
A total of 7 dvSP-ISR, 5 dvSP-RC, and 1 dvSP-TC were performed. Median age was 56.0 (55.0–61.0) years for the dvSP-ISR and 54.0 (44.7–63.5) years for the dvSP-RC/TC. Median body mass index was 22.8 (17.1–24.8) kg/m2 for the dvSP-ISR and 23.6 (20.8–26.9) kg/m2 for the dvSP-RC/TC. All dvSP-ISR patients received neoadjuvant long-course chemoradiotherapy, including one patient with squamocellular carcinoma who was treated with 5-fluorouracil (5-FU)/mitomycin. All other patients, excluding one dvSP-RC patient with Crohn’s disease, had an adenocarcinoma. Median operation time was 280 (240–370) minutes for the dvSP-ISR and 220 (201–270) minutes for the dvSP-RC/TC. Estimated blood loss was insignificant. No intraoperative complications or conversions to multiport/open surgery was reported. Median post-operative stay was 7.0 (6.0–10.0) days for the dvSP-ISR and 5.0 (4.0–6.7) days for the dvSP-RC/TC. Quality of mesorectum was complete for six patients, and nearly complete for one. Median number of retrieved lymph nodes were 21 (17–25) for the dvSP-ISR and 28 (24–49) for the dvSP-RC/TC. Proximal and distal resection margins were tumor free. Four patients experienced post-operative complications not related to the platform which were: ileus, voiding dysfunction, infected pelvic hematoma, and wound infection. Median follow-up was 9 (6–11) months and 11 (7–17) months for the dvSP-ISR and dvSP-RC/TC, respectively. Two patients had systemic recurrence; all others were tumor free.
Conclusions
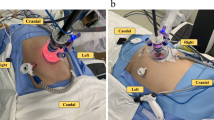
The dvSP platform is safe and feasible for intersphincteric resection with right lower quadrant access, and right/transverse colectomy with suprapubic access. Further studies are needed to evaluate benefit differences compared to multiport robotic platform.




Similar content being viewed by others
References
Chouhan H, Shin J, Kim SH (2018) Is robotic rectal resection the preferred option for resectable cancer? Mini-invasive Surg 2:18
Piozzi GN, Baek SJ, Kwak JM, Kim J, Kim SH (2021) Anus-preserving surgery in advanced low-lying rectal cancer: a perspective on oncological safety of intersphincteric resection. Cancers 13:4793
Baek SJ, Kim CH, Cho MS, Bae SU, Hur H, Min BS et al (2015) Robotic surgery for rectal cancer can overcome difficulties associated with pelvic anatomy. Surg Endosc 29:1419–1424
Piozzi GN, Lee TH, Kwak JM, Kim J, Kim SH (2021) Robotic-assisted resection for beyond TME rectal cancer: a novel classification and analysis from a specialized center. Updates Surg 73:1103–1114
Jayne D, Pigazzi A, Marshall H, Croft J, Corrigan N, Copeland J et al (2017) Effect of robotic-assisted vs conventional laparoscopic surgery on risk of conversion to open laparotomy among patients undergoing resection for rectal cancer: the ROLARR randomized clinical trial. JAMA 318:1569–1580
Park EJ, Cho MS, Baek SJ, Hur H, Min BS, Baik SH et al (2015) Long-term oncologic outcomes of robotic low anterior resection for rectal cancer: a comparative study with laparoscopic surgery. Ann Surg 261:129–137
Cho MS, Baek SJ, Hur H, Min BS, Baik SH, Lee KY et al (2015) Short and long-term outcomes of robotic versus laparoscopic total mesorectal excision for rectal cancer: a case-matched retrospective study. Med (Baltim) 94:e522
Kim J, Baek SJ, Kang DW, Roh YE, Lee JW, Kwak HD et al (2017) Robotic resection is a good prognostic factor in rectal cancer compared with laparoscopic resection: long-term survival analysis using propensity score matching. Dis Colon Rectum 60:266–273
Park SY, Lee SM, Park JS, Kim HJ, Choi GS (2021) Robot surgery shows similar long-term oncologic outcomes as laparoscopic surgery for mid/lower rectal cancer but is beneficial to ypT3/4 after preoperative chemoradiation. Dis Colon Rectum 64:812–821
Remzi FH, Kirat HT, Kaouk JH, Geisler DP (2008) Single-port laparoscopy in colorectal surgery. Colorectal Dis 10:823–826
Bucher P, Pugin F, Morel P (2008) Single port access laparoscopic right hemicolectomy. Int J Colorectal Dis 23:1013–1016
Tei M, Sueda T, Matsumura T, Furukawa H, Koga C, Wakasugi M et al (2021) Systematic review of single-port vs. multi-port surgery for rectal cancer. Mol Clin Oncol 14:24
Lee YS, Kim JH, Kim HJ, Lee SC, Kang BM, Kim CW et al (2021) Short-term outcomes of single-port versus multiport laparoscopic surgery for colon cancer: the SIMPLE multicenter randomized clinical trial. Ann Surg 273:217–223
Watanabe J, Ishibe A, Suwa H, Ota M, Fujii S, Kubota K et al (2021) Long-term outcomes of a randomized controlled trial of single-incision versus multi-port laparoscopic colectomy for colon cancer. Ann Surg 273:1060–1065
Marks JH, Kunkel E, Salem JF, Martin C, Anderson B, Agarwal S (2021) First clinical experience with single-port robotic transanal minimally invasive surgery (SP Rtamis) for benign rectal neoplasms. Tech Coloproctol 25:117–124
Marks JH, Perez RE, Salem JF (2021) Robotic transanal surgery for rectal cancer. Clin Colon Rectal Surg 34:317–324
Song SH, Kim HJ, Choi GS, Park JS, Park SY, Lee SM et al (2021) Initial experience with a suprapubic single-port robotic right hemicolectomy in patients with colon cancer. Tech Coloproctol 25:1065–1071
Noh GT, Oh BY, Han M, Chung SS, Lee RA, Kim KH (2020) Initial clinical experience of single-incision robotic colorectal surgery with da Vinci SP platform. Int J Med Robot 16:e2091
Kim HJ, Choi GS, Song SH, Park JS, Park SY, Lee SM et al (2021) An initial experience with a novel technique of single-port robotic resection for rectal cancer. Tech Coloproctol 25:857–864
Piozzi GN, Park H, Lee TH, Kim JS, Choi HB, Baek SJ, et al. Risk factors for local recurrence and long term survival after minimally invasive intersphincteric resection for very low rectal cancer: multivariate analysis in 161 patients. Eur J Surg Oncol 2021
Weiser MR (2018) AJCC 8th edition: colorectal cancer. Ann Surg Oncol 25:1454–1455
Quirke P, Steele R, Monson J, Grieve R, Khanna S, Couture J et al (2009) Effect of the plane of surgery achieved on local recurrence in patients with operable rectal cancer: a prospective study using data from the MRC CR07 and NCIC-CTG CO16 randomised clinical trial. Lancet 373:821–828
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
von Elm E, Altman DG, Egger M, Pocock SJ, Gotzsche PC, Vandenbroucke JP et al (2008) The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. J Clin Epidemiol 61:344–349
Cheong JY, Choo JM, Kim JS, Rusli SM, Kim J, Kim SH (2022) Da Vinci SP System Optimized for Intersphincteric Resection of Very Low Rectal Cancer. Dis Colon Rectum 65:e174
Choo JM, Jim JS, Cheong JY, Rusli SM, Park H, Kim SH. Application of a single-port robotic system for right colectomy: a novel suprapubic approach. Dis Colon Rectum 2022. (In press)
Cruz CJ, Yang HY, Kang I, Kang CM, Lee WJ (2019) Technical feasibility of da Vinci SP single-port robotic cholecystectomy: a case report. Ann Surg Treat Res 97:217–221
Piozzi GN, Park H, Kim JS, Choi HB, Lee TH, Baek SJ, et al. Anatomical landmarks for transabdominal robotic-assisted intersphincteric dissection for ultralow anterior resection. Dis Colon Rectum 2021
Lujan JA, Soriano MT, Abrisqueta J, Perez D, Parrilla P (2015) Single-port colectomy VS multi-port laparoscopic colectomy. systematic review and meta-analysis of more than 2800 procedures. Cir Esp 93:307–19
Hata T, Kawai K, Naito A, Kagawa Y, Kitahara T, Hiraki M, et al. Short- and long-term outcomes of single-incision laparoscopic surgery for right-side colon cancer. Eur Surg Res 2021
Benlice C, Stocchi L, Costedio MM, Gorgun E, Kessler H (2016) Impact of the specific extraction-site location on the risk of incisional hernia after laparoscopic colorectal resection. Dis Colon Rectum 59:743–750
Choi HB, Chung D, Kim JS, Lee TH, Baek SJ, Kwak JM et al (2022) Midline incision vs. transverse incision for specimen extraction is not a significant risk factor for developing incisional hernia after minimally invasive colorectal surgery: multivariable analysis of a large cohort from a single tertiary center in Korea. Surg Endosc 36:1199–205
Lee L, Abou-Khalil M, Liberman S, Boutros M, Fried GM, Feldman LS (2017) Incidence of incisional hernia in the specimen extraction site for laparoscopic colorectal surgery: systematic review and meta-analysis. Surg Endosc 31:5083–5093
Widmar M, Aggarwal P, Keskin M, Strombom PD, Patil S, Smith JJ et al (2020) Intracorporeal anastomoses in minimally invasive right colectomies are associated with fewer incisional hernias and shorter length of stay. Dis Colon Rectum 63:685–692
Cheong JY, Kim J, Kim SH (2021) How to do robotic low anterior resection using Da Vinci-Xi system: addressing the ergonomics dilemma. ANZ J Surg 91:2518–2520
Park JS, Choi GS, Kim SH, Kim HR, Kim NK, Lee KY et al (2013) Multicenter analysis of risk factors for anastomotic leakage after laparoscopic rectal cancer excision: the Korean laparoscopic colorectal surgery study group. Ann Surg 257:665–671
Thies S, Langer R (2013) Tumor regression grading of gastrointestinal carcinomas after neoadjuvant treatment. Front Oncol 3:262
Author information
Authors and Affiliations
Contributions
Conceptualization: GNP, SHK; methodology: GNP, J-SK, JMC, SHS, JSK, T-HL; formal analysis and investigation: GNP, SHS; writing—original draft preparation: GNP; writing—review and editing: S-JB, J-MK, JK, SHK; supervision: SHK.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest do disclose.
Ethical approval
This study was approved by the Institutional Review Board.
Informed consent
As this study was a retrospective analysis of routine clinical data, participants’ informed consent was waived by the institutional review board.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Piozzi, G.N., Kim, JS., Choo, J.M. et al. Da Vinci SP robotic approach to colorectal surgery: two specific indications and short-term results. Tech Coloproctol 26, 461–470 (2022). https://doi.org/10.1007/s10151-022-02597-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10151-022-02597-x