Abstract
Background
Restorative proctectomy for rectal cancer is associated with a high incidence of low anterior resection syndrome (LARS), but few studies report longitudinal results for bowel function. The aim of our study was to examine the trajectory of change of LARS over the first 18 months after restorative proctectomy for rectal cancer.
Methods
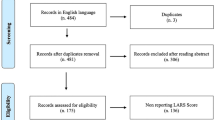
A prospective database measuring functional outcomes in rectal cancer patients from a single university-affiliated specialist colorectal referral center from 10/2018 to 03/2020 was queried. Patients were included in this study if they underwent restorative proctectomy for rectal cancer and had at least three assessments in the first 18 months after primary surgery or after closure of proximal diversion. Bowel function was assessed using the LARS score, administered at every surveillance follow-up after restoration of bowel continuity. Latent-class growth curve (trajectory) analysis was used to identify different trajectories of LARS changes over the first 18 months and group patients into these trajectory groups. These groups were then compared to identify predictors for each trajectory.
Results
A total of 95 patients were included (63 males, mean age. 61.3 ± 12.5 years). Trajectory analysis identified three distinct trajectory groups. Group 1 had stable minimal LARS over time (26%). Group 2 had early LARS scores consistent with the minor LARS category and improved with time (28%). Group 3 had persistently high LARS scores (45%). Neoadjuvant therapy, intersphincteric resection, and proximal diversion were more common in group 3.
Conclusions
We identified three main trajectories of change of LARS in the 18 months after restorative proctectomy. These data may be used to better inform patients of their expected postoperative bowel function.




Similar content being viewed by others
Data availability
Data are available upon reasonable request.
References
Shahjehan F, Kasi PM, Habermann E et al (2019) Trends and outcomes of sphincter-preserving surgery for rectal cancer: a national cancer database study. Int J Colorectal Dis 34:239–245. https://doi.org/10.1007/s00384-018-3171-y
Mohammed S, Anaya DA, Awad SS, Albo D, Berger DH, Artinyan A (2015) Sphincter preservation rates after radical resection for rectal cancer in the United States veteran population: opportunity for improvement in early disease. Ann Surg Oncol 22:216–223. https://doi.org/10.1245/s10434-014-4101-z
Emmertsen KJ, Laurberg S (2012) Low anterior resection syndrome score: development and validation of a symptom-based scoring system for bowel dysfunction after low anterior resection for rectal cancer. Ann Surg 255:922–928. https://doi.org/10.1097/SLA.0b013e31824f1c21
Keane C, Fearnhead NS, Bordeianou LG et al (2020) International consensus definition of low anterior resection syndrome. Dis Colon Rectum 63:274–284. https://doi.org/10.1097/DCR.0000000000001583
Chapman SJ, Bolton WS, Corrigan N, Young N, Jayne DG (2017) A Cross-sectional review of reporting variation in postoperative bowel dysfunction after rectal cancer surgery. Dis Colon Rectum 60:240–247. https://doi.org/10.1097/DCR.0000000000000649
Lai X, Wong FK, Ching SS (2013) Review of bowel dysfunction of rectal cancer patients during the first five years after sphincter-preserving surgery: a population in need of nursing attention. Eur J Oncol Nurs 17:681–692. https://doi.org/10.1016/j.ejon.2013.06.001
Faria S, Kopek N, Hijal T et al (2014) Phase II trial of short-course radiotherapy followed by delayed surgery for locoregionally advanced rectal cancer. Colorectal Dis 16:O66-70. https://doi.org/10.1111/codi.12466
Kennedy ED, Simunovic M, Jhaveri K et al (2019) Safety and feasibility of using magnetic resonance imaging criteria to identify patients with “good prognosis” rectal cancer eligible for primary surgery: the phase 2 nonrandomized quicksilver clinical trial. JAMA Oncol 5:961–966. https://doi.org/10.1001/jamaoncol.2019.0186
Caycedo-Marulanda A, Brown CJ, Chadi SA et al (2020) Canadian taTME expert collaboration (CaTaCO) position statement. Surg Endosc 34:3748–3753. https://doi.org/10.1007/s00464-020-07680-8
Brown CJ, Fenech DS, McLeod RS (2008) Reconstructive techniques after rectal resection for rectal cancer. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD006040.pub2
Kang CY, Halabi WJ, Chaudhry OO et al (2013) Risk factors for anastomotic leakage after anterior resection for rectal cancer. JAMA Surg 148:65–71. https://doi.org/10.1001/2013.jamasurg.2
Shalabi A, Duek SD, Khoury W (2016) Water-soluble enema prior to ileostomy closure in patients undergoing low anterior resection: is it necessary? J Gastrointest Surg 20:1732–1737. https://doi.org/10.1007/s11605-016-3218-8
Network NCC. NCCN Clinical Practice Guidelines in Oncology—Rectal Cancer [Available from: https://www.nccn.org/professionals/physician_gls/pdf/rectal.pdf. Accessed 1 Mar 2021
Nagin DS, Odgers CL (2010) Group-based trajectory modeling in clinical research. Annu Rev Clin Psychol 6:109–138. https://doi.org/10.1146/annurev.clinpsy.121208.131413
Keane C, Park J, Oberg S et al (2019) Functional outcomes from a randomized trial of early closure of temporary ileostomy after rectal excision for cancer. Br J Surg 106:645–652. https://doi.org/10.1002/bjs.11092
Haviland AM, Jones BL, Nagin DS (2011) Group-based trajectory modeling extended to account for nonrandom participant attrition. Sociol Methods Res 40:367–390
Wells CI, Vather R, Chu MJ, Robertson JP, Bissett IP (2015) Anterior resection syndrome—a risk factor analysis. J Gastrointest Surg 19:350–359. https://doi.org/10.1007/s11605-014-2679-x
Battersby NJ, Bouliotis G, Emmertsen KJ et al (2018) Development and external validation of a nomogram and online tool to predict bowel dysfunction following restorative rectal cancer resection: the POLARS score. Gut 67:688–696. https://doi.org/10.1136/gutjnl-2016-312695
Sandberg S, Asplund D, Bisgaard T et al (2020) Low anterior resection syndrome in a Scandinavian population of patients with rectal cancer: a longitudinal follow-up within the QoLiRECT study. Colorectal Dis 22:1367–1378. https://doi.org/10.1111/codi.15095
Vogel I, Reeves N, Tanis PJ et al (2021) Impact of a defunctioning ileostomy and time to stoma closure on bowel function after low anterior resection for rectal cancer: a systematic review and meta-analysis. Tech Coloproctol 25:751–760. https://doi.org/10.1007/s10151-021-02436-5
Choy KT, Yang TWW, Prabhakaran S, Heriot A, Kong JC, Warrier SK (2021) Comparing functional outcomes between transanal total mesorectal excision (TaTME) and laparoscopic total mesorectal excision (LaTME) for rectal cancer: a systematic review and meta-analysis. Int J Colorectal Dis. https://doi.org/10.1007/s00384-021-03849-2
van der Heijden JAG, Qaderi SM, Verhoeven R et al (2021) Transanal total mesorectal excision and low anterior resection syndrome. Br J Surg 108:991–997. https://doi.org/10.1093/bjs/znab056
Alimova I, Chernyshov S, Nagudov M, Rybakov E (2021) Comparison of oncological and functional outcomes and quality of life after transanal or laparoscopic total mesorectal excision for rectal cancer: a systematic review and meta-analysis. Tech Coloproctol 25:901–913. https://doi.org/10.1007/s10151-021-02420-z
Keller DS, Paspulati R, Kjellmo A et al (2014) MRI-defined height of rectal tumours. Br J Surg 101:127–132. https://doi.org/10.1002/bjs.9355
Wasserman MA, McGee MF, Helenowski IB, Halverson AL, Boller AM, Stryker SJ (2016) The anthropometric definition of the rectum is highly variable. Int J Colorectal Dis 31:189–195. https://doi.org/10.1007/s00384-015-2458-5
Rullier E, Denost Q, Vendrely V, Rullier A, Laurent C (2013) Low rectal cancer: classification and standardization of surgery. Dis Colon Rectum 56:560–567. https://doi.org/10.1097/DCR.0b013e31827c4a8c
Kim MJ, Park JW, Lee MA et al (2021) Two dominant patterns of low anterior resection syndrome and their effects on patients’ quality of life. Sci Rep 11:3538. https://doi.org/10.1038/s41598-021-82149-9
Ribas Y, Aguilar F, Jovell-Fernandez E, Cayetano L, Navarro-Luna A, Munoz-Duyos A (2017) Clinical application of the LARS score: results from a pilot study. Int J Colorectal Dis 32:409–418. https://doi.org/10.1007/s00384-016-2690-7
Pieniowski EHA, Palmer GJ, Juul T et al (2019) Low anterior resection syndrome and quality of life after sphincter-sparing rectal cancer surgery: a long-term longitudinal follow-up. Dis Colon Rectum 62:14–20. https://doi.org/10.1097/DCR.0000000000001228
Emmertsen KJ, Laurberg S, Rectal Cancer Function Study G (2013) Impact of bowel dysfunction on quality of life after sphincter-preserving resection for rectal cancer. Br J Surg 100:1377–1387. https://doi.org/10.1002/bjs.9223
Lee L, Tran T, Mayo NE, Carli F, Feldman LS (2014) What does it really mean to “recover” from an operation? Surgery 155:211–216. https://doi.org/10.1016/j.surg.2013.10.002
Keane C, Sharma P, Yuan L, Bissett I, O’Grady G (2020) Impact of temporary ileostomy on long-term quality of life and bowel function: a systematic review and meta-analysis. ANZ J Surg 90:687–692. https://doi.org/10.1111/ans.15552
Kverneng Hultberg D, Svensson J, Jutesten H et al (2020) The impact of anastomotic leakage on long-term function after anterior resection for rectal cancer. Dis Colon Rectum 63:619–628. https://doi.org/10.1097/DCR.0000000000001613
Kinugasa Y, Murakami G, Uchimoto K, Takenaka A, Yajima T, Sugihara K (2006) Operating behind Denonvilliers’ fascia for reliable preservation of urogenital autonomic nerves in total mesorectal excision: a histologic study using cadaveric specimens, including a surgical experiment using fresh cadaveric models. Dis Colon Rectum 49:1024–1032. https://doi.org/10.1007/s10350-006-0557-7
Wallner C, Lange MM, Bonsing BA et al (2008) Causes of fecal and urinary incontinence after total mesorectal excision for rectal cancer based on cadaveric surgery: a study from the Cooperative Clinical Investigators of the Dutch total mesorectal excision trial. J Clin Oncol 26:4466–4472. https://doi.org/10.1200/JCO.2008.17.3062
Sun V, Grant M, Wendel CS et al (2015) Dietary and behavioral adjustments to manage bowel dysfunction after surgery in long-term colorectal cancer survivors. Ann Surg Oncol 22:4317–4324. https://doi.org/10.1245/s10434-015-4731-9
Dulskas A, Smolskas E, Kildusiene I, Samalavicius NE (2018) Treatment possibilities for low anterior resection syndrome: a review of the literature. Int J Colorectal Dis 33:251–260. https://doi.org/10.1007/s00384-017-2954-x
Funding
The research leading to these results received funding from the American Society of Colon and Rectal Surgeons Career Development Award under grant agreement CDA-019 (recipient: Lawrence Lee).
Author information
Authors and Affiliations
Contributions
Conception and design: FA, SR, LSF, JFF, LL. Acquisition of data: FA, SR, ASL, PC, BS, LL. Analysis and interpretation of data: FA, SR, ASL, PC, BS, LSF, JFF, LL. Drafting the manuscript: FA, SR, LL. Critical revision: ASL, PC, BS, LSF, JFF, LL. Final approval of the version to be published: FA, SR, ASL, PC, BS, LSF, JFF, LL.
Corresponding author
Ethics declarations
Conflict of interests
The authors have no relevant financial interests to disclose. LL is the recipient of an investigator-initiated research grant from Johnson & Johnson and receives speaker fees from Stryker. LSF is the recipient of an investigator-initiated research grant from Merck. JFF is the recipient of an investigator-initiated research grants from Merck and receives consulting fees from Shinogi. SL receives consulting fees from Merck. FA, SR, PC, and BS have nothing to disclose.
Ethical approval
The study protocol was approved by the Research Ethics Board of the McGill University Health Centre Research Institution (TME/2018–3864).
Consent to participate
Participation in this study was voluntary and all subjects signed informed consent to participate.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Al-Rashid, F., Robitaille, S., Liberman, A.S. et al. Trajectory of change of low anterior resection syndrome over time after restorative proctectomy for rectal adenocarcinoma. Tech Coloproctol 26, 195–203 (2022). https://doi.org/10.1007/s10151-021-02561-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10151-021-02561-1