Abstract
Background
To determine the peri-operative safety and oncological value of robotic-assisted radical cystectomy (RARC) for older and younger patients in an initial Japanese RARC series.
Methods
We retrospectively analyzed the demographics, complications, peri-operative and oncological outcomes of 253 consecutive patients with bladder cancer who underwent RARC at 34 institutions in Japan between April 2009 and March 2017. The patients were assigned to groups according to ages at surgery of < 70 (younger; n = 125) and ≥ 70 (older; n = 128) years.
Results
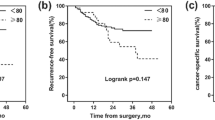
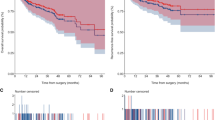
Mean Charlson comorbidity index (p = 0.045) and the incidence of a history of previous abdominal surgery (p = 0.002) were significantly higher, whereas a history of neoadjuvant chemotherapy (p = 0.028) and neobladder (p < 0.001) were significantly lower in the older group. Mean total operative time was significantly shorter (p = 0.019) and mean estimated blood loss (p = 0.013) was significantly lower in the older group. Post-operative Grade ≥ II complications were comparable at 0–30, 31–90 and 91 days after surgery despite urinary tract associations. Rates of positive surgical margins and mean numbers of removed lymph nodes were comparable between the two groups. Although 5-year overall survival rates were significantly lower (p = 0.03) for older patients, 5-year cancer-specific (p = 0.10) and recurrence-free survival rates were comparable (p = 0.20) between the groups.
Conclusion
Using RARC potentially allows the application of less invasive procedures and cancer control for septuagenarian patients that are equivalent to those for younger patients.

Similar content being viewed by others
References
American Cancer Society. Probability of developing invasive cancers over selected age intervals by sex, US 2002–2004. American Cancer Society. www.cancer.org/downloads/stt/CFF2008Table_pg14.pdf. Accessed 24 Oct 2009
Huang GJ, Stein JP (2007) Open radical cystectomy with lymphadenectomy remains the treatment of choice for invasive bladder cancer. Curr Opin Urol 17:369–375
Iwamoto H, Yumioka T, Yamaguchi N et al (2016) Robot-assisted radical cystectomy is a promising alternative to open surgery in the Japanese population with a high rate of octogenarians. Int J Clin Oncol 4:756–763
Cabinet Office, Government of Japan. annual report on the aging society: 2016. http://www8.cao.go.jp/kourei/english/annualreport/2016/2016pdf_e.html
Parekh DJ, Messer J, Fitzgerald J et al (2013) Perioperative outcomes and oncologic efficacy from a pilot prospective randomized clinical trial of open versus robotic assisted radical cystectomy. J Urol 189:474–479
Li K, Lin T, Fan X et al (2013) Systematic review and meta-analysis of comparative studies reporting early outcomes after robot-assisted radical cystectomy versus open radical cystectomy. Cancer Treat Rev 39:551–560
Novara G, Catto JW, Wilson T et al (2015) Systematic review and cumulative analysis of perioperative outcomes and complications after robot-assisted radical cystectomy. Eur Urol 67:376–401
Yuh B, Wilson T, Bochner B et al (2015) Systematic review and cumulative analysis of oncologic and functional outcomes after robot-assisted radical cystectomy. Eur Urol 67:402–422
Shen Z, Sun Z (2016) Systematic review and meta-analysis of randomised trials of perioperative outcomes comparing robot-assisted versus open radical cystectomy. BMC Urol 16:59
Abboudi H, Khan MS, Guru KA et al (2014) Learning curves for urological procedures: a systematic review. BJU Int 114:617–629
Fonteyne V, Ost P, Bellmunt J et al (2018) Curative treatment for muscle invasive bladder cancer in elderly patients: a systematic review. Eur Urol 73:40–50
Donat SM, Siegrist T, Cronin A et al (2010) Radical cystectomy in octogenarians—does morbidity outweigh the potential survival benefits? J Urol 183:2171–2177
Coward RM, Smith A, Raynor M et al (2011) Feasibility and outcomes of robotic-assisted laparoscopic radical cystectomy for bladder cancer in older patients. Urology 77:1111–1114
Guillotreau J, Miocinovic R, Gamé X et al (2012) Outcomes of laparoscopic and robotic radical cystectomy in the elderly patients. Urology 79:585–590
Nguyen DP, Al Hussein BA, Osterberg EC et al (2015) Postoperative complications and short-term oncological outcomes of patients aged ≥ 80 years undergoing robot-assisted radical cystectomy. World J Urol 33:1315–1321
Ng CK, Kauffman EC, Lee MM et al (2010) A comparison of postoperative complications in open versus robotic cystectomy. Eur Urol 57:274–281
Sung HH, Ahn JS, Seo SI et al (2012) A comparison of early complications between open and robot-assisted radical cystectomy. J Endourol 26:670–675
Bochner BH, Dalbagni G, Sjoberg DD et al (2015) Comparing open radical cystectomy and robot-assisted laparoscopic radical cystectomy: a randomized clinical trial. Eur Urol 67:1042–1050
Bak DJ, Lee YJ, Woo MJ (2016) Complications and oncologic outcomes following robot-assisted radical cystectomy: what is the real benefit? Investig Clin Urol 57:260–267
Pridgeon S, Bishop CV, Adshead J et al (2013) Lower limb compartment syndrome as a complication of robot-assisted radical prostatectomy: the UK experience. BJU Int 112:485–488
Simms MS, Terry TR (2005) Well leg compartment syndrome after pelvic and perineal surgery in the lithotomy position. Postgrad Med J 81:534–536
Herr H, Lee C, Chang S et al (2004) Bladder Cancer Collaborative Group: standardization of radical cystectomy and pelvic lymph node dissection for bladder cancer—a collaborative group report. J Urol 171:1823–1828
Snow-Lisy DC, Campbell SC, Gill IS et al (2014) Robotic and laparoscopic radical cystectomy for bladder cancer: long-term oncologic outcomes. Eur Urol 65:193–200
Raza SJ, Al-Daghmin A, Zhuo S et al (2014) Oncologic outcomes following robot-assisted radical cystectomy with minimum 5-year follow-up: the Roswell Park cancer institute experience. Eur Urol 66:920–928
Desai MM, Gill IS, de Castro Abreu AL et al (2014) Robotic intracorporeal orthotopic neobladder during radical cystectomy in 132 patients. J Urol 192:1734–1740
Acknowledgements
These clinicopathological statistics are based on the results from a number of institutions in Japan. We are grateful for the cooperation of many Japanese urologists. This document was created by the Japanese Society of Endourology. Cooperative institutions for the present study are: Department of Urology, the University of Tokyo Graduate School of Medicine; Department of Urology, Kobe University Graduate School of Medicine; Department of Urology, Hamamatsu University School of Medicine; Department of Urology, Iwate Medical University School of Medicine; Department of Urology, Kagawa University, Faculty of Medicine,; Department of Urology, Shiga University of Medical Science; Department of Urology, Takamatsu Red Cross Hospital; Department of Urology, Teine Keijinkai Medical Center; Department of Urology, Kobe City Medical Center General Hospital; Ibaraki Clinical Education and Training Center, Faculty of Medicine; Department of Urology, St. Luke’s International Hospital; Department of Urology, Wakayama Medical University: Department of Urology, Kyoto City Hospital; Department of Urology, Nagoya University Graduate School of Medicine; Department of Urology, Kyoto University Hospital; Department of Urology, Ehime Prefectural Central Hospital; Department of Urology, Gifu Prefectural General Medical Center; Department of Urology, Hiroshima City Hiroshima Citizens Hospital; Department of Urology Aichi Medical University School of Medicine; Department of Urology, Kitasato University School of Medicine; Department of Urology, Ehime University Graduate School of Medicine; Department of Urology, Shizuoka General Hospital; Department of Urology, Tohoku University Graduate School of Medicine; Department of Urology, Tokyo Medical University; Department of Urology, Tokushima University Graduate School; Department of Urology, Akita University School of Medicine; Department of Urology, Institute of Biomedical and Health Science, Hiroshima University; Department of Urology, Kochi Medical School, Kochi University; Department of Urology, Hirosaki University Graduate School of Medicine; Department of Urology, Fujita Health University; Department of Urology, Juntendo University; Department of Urology, Shimane University School of Medicine; Department of Urology, Jyoban Hospital of Tokiwa Foundation; Division of Urology, Department of Surgery, Tottori University Faculty of Medicine.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No author has any conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
About this article
Cite this article
Iwamoto, H., Morizane, S., Koie, T. et al. Peri-operative efficacy and long-term survival benefit of robotic-assisted radical cystectomy in septuagenarian patients compared with younger patients: a nationwide multi-institutional study in Japan. Int J Clin Oncol 24, 1588–1595 (2019). https://doi.org/10.1007/s10147-019-01470-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10147-019-01470-6