Abstract
Background
The aim of this study is to investigate the cumulative incidence and risk factors of postoperative inguinal hernia (PIH) in patients undergoing radical prostatectomy, i.e., laparoscopic prostatectomy (LRP) and robot-assisted laparoscopic prostatectomy (RARP).
Methods
This study included 1124 patients who had undergone radical prostatectomy or transurethral resection of bladder tumor from 2011−2016. We compared the cumulative incidence of PIH in the radical prostatectomy groups (460; LRP 341, RARP 119) and the control group (664; transurethral resection of bladder tumor), and we then analyzed the risk factors (age, operative methods, previous abdominal operative history, thickness and width of external oblique muscle and rectus muscle, thickness of abdominal subcutaneous fat layer at Hesselbach’s triangle level, body mass index, prostate-specific antigen, operative time, specimen weight, Gleason score, and pathology T-stage) of PIH in the radical prostatectomy groups.
Results
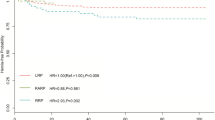
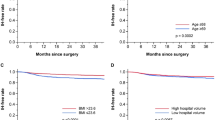
The median follow-up period in this study was 39.6 months. In Kaplan–Meier curve analysis, the cumulative incidence of PIH was 5.3, 4.2, and 0.5% for the LRP, RARP, and control groups, respectively (p < 0.001). Multiple logistic regressions showed that thickness of external oblique muscle and width of rectus muscle were significant risk factors (p < 0.001 and p = 0.027).
Conclusions
PIH is considered to be one of the complications of LRP and RARP. Moreover, we suggest that if the thickness of the muscle is <7.3 mm, thoughtful surgical manipulation is needed for radical prostatectomy, and care should be taken to determine whether hernia occurs during follow-up.


Similar content being viewed by others
References
Mottet N, Bellmunt J, Bolla M et al (2017) EAU-ESTRO-SIOG guidelines on prostate cancer. Part 1: screening, diagnosis, and local treatment with curative intent. Eur Urol 71(4):618–629. https://doi.org/10.1016/j.eururo.2016.08.003
Son SJ, Lee SC, Jeong CW et al (2013) Comparison of continence recovery between robot-assisted laparoscopic prostatectomy and open radical retropubic prostatectomy: a single surgeon experience. Korean J Urol 54(9):598–602. https://doi.org/10.4111/kju.2013.54.9.598
Asimakopoulos AD, Pereira Fraga CT, Annino F et al (2011) Randomized comparison between laparoscopic and robot-assisted nerve-sparing radical prostatectomy. J Sex Med 8(5):1503–1512. https://doi.org/10.1111/j.1743-6109.2011.02215.x
Goluboff ET, Saidi JA, Mazer S et al (1998) Urinary continence after radical prostatectomy: the Columbia experience. J Urol 159(4):1276–1280
Jacobsen NE, Moore KN, Estey E et al (2007) Open versus laparoscopic radical prostatectomy: a prospective comparison of postoperative urinary incontinence rates. J Urol 177(2):615–619. https://doi.org/10.1016/j.juro.2006.09.022
Stolzenburg JU, Graefen M, Kriegel C et al (2015) Effect of surgical approach on erectile function recovery following bilateral nerve-sparing radical prostatectomy: an evaluation utilizing data from a randomized, double-blind, double-dummy multicenter trial of tadalafil versus placebo. BJU Int. https://doi.org/10.1111/bju.13030
Regan TC, Mordkin RM, Constantinople NL et al (1996) Incidence of inguinal hernias following radical retropubic prostatectomy. Urology 47(4):536–537. https://doi.org/10.1016/S0090-4295(99)80491-9
Ichioka K, Yoshimura K, Utsunomiya N et al (2004) High incidence of inguinal hernia after radical retropubic prostatectomy. Urology 63(2):278–281. https://doi.org/10.1016/j.urology.2003.09.038
Stranne J, Hugosson J, Iversen P et al (2005) Inguinal hernia in stage M0 prostate cancer: a comparison of incidence in men treated with and without radical retropubic prostatectomy−an analysis of 1105 patients. Urology 65(5):847–851. https://doi.org/10.1016/j.urology.2004.11.014
Twu CM, Ou YC, Yang CR et al (2005) Predicting risk factors for inguinal hernia after radical retropubic prostatectomy. Urology 66(4):814–818. https://doi.org/10.1016/j.urology.2005.04.034
Abe T, Shinohara N, Harabayashi T et al (2007) Postoperative inguinal hernia after radical prostatectomy for prostate cancer. Urology 69(2):326–329. https://doi.org/10.1016/j.urology.2006.09.043
Yoshimine S, Miyajima A, Nakagawa K et al (2010) Extraperitoneal approach induces postoperative inguinal hernia compared with transperitoneal approach after laparoscopic radical prostatectomy. Jpn J Clin Oncol 40(4):349–352. https://doi.org/10.1093/jjco/hyp172
Stranne J, Johansson E, Nilsson A et al (2010) Inguinal hernia after radical prostatectomy for prostate cancer: results from a randomized setting and a nonrandomized setting. Eur Urol 58(5):719–726. https://doi.org/10.1016/j.eururo.2010.08.006
Lodding P, Bergdahl C, Nyberg M et al (2001) Inguinal hernia after radical retropubic prostatectomy for prostate cancer: a study of incidence and risk factors in comparison to no operation and lymphadenectomy. J Urol 166(3):964–967
Rabbani F, Yunis LH, Touijer K et al (2011) Predictors of inguinal hernia after radical prostatectomy. Urology 77(2):391–395. https://doi.org/10.1016/j.urology.2010.04.019
Yamada Y, Fujimura T, Fukuhara H et al (2017) Incidence and risk factors of inguinal hernia after robot-assisted radical prostatectomy. World J Surg Oncol 15(1):61. https://doi.org/10.1186/s12957-017-1126-3
Lee DH, Jung HB, Chung MS et al (2013) Patent processus vaginalis in adults who underwent robot-assisted laparoscopic radical prostatectomy: predictive signs of postoperative inguinal hernia in the internal inguinal floor. Int J Urol 20(2):177–182. https://doi.org/10.1111/j.1442-2042.2012.03118.x
Stranne J, Lodding P (2011) Inguinal hernia after radical retropubic prostatectomy: risk factors and prevention. Nat Rev Urol 8(5):267–273. https://doi.org/10.1038/nrurol.2011.40
Koie T, Yoneyama T, Kamimura N et al (2008) Frequency of postoperative inguinal hernia after endoscope-assisted mini-laparotomy and conventional retropubic radical prostatectomies. Int J Urol 15(3):226–229. https://doi.org/10.1111/j.1442-2042.2007.01983.x
Sun M, Lughezzani G, Alasker A et al (2010) Comparative study of inguinal hernia repair after radical prostatectomy, prostate biopsy, transurethral resection of the prostate or pelvic lymph node dissection. J Urol 183(3):970–975. https://doi.org/10.1016/j.juro.2009.11.036
Sekita N, Suzuki H, Kamijima S et al (2009) Incidence of inguinal hernia after prostate surgery: open radical retropubic prostatectomy versus open simple prostatectomy versus transurethral resection of the prostate. Int J Urol 16(1):110–113. https://doi.org/10.1111/j.1442-2042.2008.02190.x
Rosemar A, Angeras U, Rosengren A (2008) Body mass index and groin hernia: a 34-year follow-up study in Swedish men. Ann Surg 247(6):1064–1068. https://doi.org/10.1097/SLA.0b013e31816b4399
Burcharth J, Pommergaard HC, Bisgaard T et al (2015) Patient-related risk factors for recurrence after inguinal hernia repair: a systematic review and meta-analysis of observational studies. Surg Innov 22(3):303–317. https://doi.org/10.1177/1553350614552731
Pans A, Albert A, Lapiere CM et al (2001) Biochemical study of collagen in adult groin hernias. J Surg Res 95(2):107–113. https://doi.org/10.1006/jsre.2000.6024
Wagh PV, Read RC (1972) Defective collagen synthesis in inguinal herniation. Am J Surg 124(6):819–822
Zhu S, Zhang H, Xie L et al (2013) Risk factors and prevention of inguinal hernia after radical prostatectomy: a systematic review and meta-analysis. J Urol 189(3):884–890. https://doi.org/10.1016/j.juro.2012.08.241
Hermann M, Gustafsson O, Sandblom G (2017) Incidence of incisional hernia after minimally invasive and open radical prostatectomy: a population-based nationwide study. Scand J Urol 51(4):264–268. https://doi.org/10.1080/21681805.2017.1301991
Nomura T, Mimata H, Kitamura H et al (2005) Lower incidence of inguinal hernia: minilaparotomy radical retropubic prostatectomy compared with conventional technique. A preliminary report. Urol Int 74(1):32–37. https://doi.org/10.1159/000082706
Lin BM, Hyndman ME, Steele KE et al (2011) Incidence and risk factors for inguinal and incisional hernia after laparoscopic radical prostatectomy. Urology 77(4):957–962. https://doi.org/10.1016/j.urology.2010.12.011
Yasuhiro K, Koji M, Shigeyuki Y et al (2016) Urinary straining contributes to inguinal hernia after radical retropubic prostatectomy. Int J Urol 23(6):478–483. https://doi.org/10.1111/iju.13078
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
About this article
Cite this article
Ku, J.Y., Lee, C.H., Park, W.Y. et al. The cumulative incidence and risk factors of postoperative inguinal hernia in patients undergoing radical prostatectomy. Int J Clin Oncol 23, 742–748 (2018). https://doi.org/10.1007/s10147-018-1244-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10147-018-1244-0