Abstract
Background
We evaluated the longer-term efficacy and safety of concurrent chemoradiotherapy (CCRT) incorporating high-dose-rate intracavitary brachytherapy (HDR-ICBT) with a lower cumulative radiotherapy (RT) protocol and analyzed prognostic risk factors for survival among patients with FIGO stage III–IVA squamous cell carcinoma (SCC) of the cervix.
Patients and methods
Ninety-nine patients with FIGO stage III–IVA SCC of the cervix between 1997 and 2008 were treated with CCRT using cisplatin 20 mg/m2 for 5 days every 3 weeks or 40 mg/m2 weekly. Acute and late toxicities were evaluated. Overall survival (OS) and disease-free survival (DFS) were estimated by the Kaplan–Meier method. The Cox proportional hazard model was used for multivariate analysis.
Results
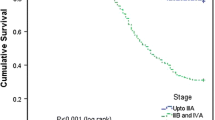
Median age was 53.5 years. Median follow-up period was 58 months (range 6–170 months). Pathologically complete response was achieved in 93 patients (96.9 %). The 5-year OS and DFS were 72.0 and 69.3 %, respectively. The 5-year local and distant DFS were 83.0 and 75.1 %, respectively. Thirty-one patients (31.3 %) experienced recurrence. Multivariate analysis showed that tumor size and pretreatment hemoglobin level remained an independent risk factor for OS and DFS. Acute toxicity was moderate. In terms of late adverse effects, 2 patients (2.0 %) suffered from grade 4 late intestinal toxicity because of radiation enterocolitis, with both requiring intestinal surgery.
Conclusions
Our study demonstrates that the CCRT schedule in patients with FIGO stage III–IVA SCC is efficacious and safe. In addition, the assessment of tumor size and pretreatment anemia can provide valuable prognostic information.


Similar content being viewed by others
References
Morris M, Eifel PJ, Lu J et al (1999) Pelvic radiation with concurrent chemotherapy compared with pelvic and para-aortic radiation for high-risk cervical cancer. N Engl J Med 340:1137–1143
Peters WA 3rd, Liu PY, Barrett RJ 2nd et al (2000) Concurrent chemotherapy and pelvic radiation therapy compared with pelvic radiation therapy alone as adjuvant therapy after radical surgery in high-risk early-stage cancer of the cervix. J Clin Oncol 18:1606–1613
Rose PG, Bundy BN, Watkins EB et al (1999) Concurrent cisplatin-based radiotherapy and chemotherapy for locally advanced cervical cancer. N Engl J Med 340:1144–1153
Whitney CW, Sause W, Bundy BN et al (1999) Randomized comparison of fluorouracil plus cisplatin versus hydroxyurea as an adjunct to radiation therapy in stage IIB-IVA carcinoma of the cervix with negative para-aortic lymph nodes: a Gynecologic Oncology Group and Southwest Oncology Group study. J Clin Oncol 17:1339–1348
Keys HM, Bundy BN, Stehman FB et al (1999) Cisplatin, radiation, and adjuvant hysterectomy compared with radiation and adjuvant hysterectomy for bulky stage IB cervical carcinoma. N Engl J Med 340:1154–1161
Rose PG, Ali S, Watkins E et al (2007) Long-term follow-up of a randomized trial comparing concurrent single agent cisplatin, cisplatin-based combination chemotherapy, or hydroxyurea during pelvic irradiation for locally advanced cervical cancer: a Gynecologic Oncology Group Study. J Clin Oncol 25:2804–2810
Monk BJ, Wang J, Im S et al (2005) Rethinking the use of radiation and chemotherapy after radical hysterectomy: a clinical–pathologic analysis of a Gynecologic Oncology Group/Southwest Oncology Group/Radiation Therapy Oncology Group trial. Gynecol Oncol 96:721–728
Monk BJ, Tiam C, Rose PG et al (2007) Which clinical/pathologic factors matter in the era of chemoradiation as treatment for locally advanced cervical carcinoma? Analysis of two Gynecologic Oncology Group (GOG) trials. Gynecol Oncol 105:427–433
Eifel PJ, Winter K, Morris M et al (2004) Pelvic irradiation with concurrent chemotherapy versus pelvic and para-aortic irradiation for high-risk cervical cancer: an update of radiation therapy oncology group trial (RTOG) 90–01. J Clin Oncol 22:872–880
Thomas GM (1999) Improved treatment for cervical cancer: concurrent chemotherapy and radiotherapy. N Engl J Med 340:1198–1200
Green JA, Kirwan JM, Tierney JF et al (2001) Survival and recurrence after concomitant chemotherapy and radiotherapy for cancer of the uterine cervix: a systematic review and meta-analysis. Lancet 358:781–786
Toita T, Kodaira T, Shinoda A et al (2008) Patterns of radiotherapy practice for patients with cervical cancer (1999–2001): patterns of care study in Japan. Int J Radiat Oncol Biol Phys 70:788–794
Viswanathan AN, Creutzberg CL, Craighead P et al (2012) International brachytherapy practice patterns: a survey of the Gynecologic Cancer Intergroup (GCIG). Int J Radiat Oncol Biol Phys 82:250–255
Toita T, Kakinohana Y, Ogawa K et al (2003) Combination external beam radiotherapy and high-dose-rate intracavitary brachytherapy for uterine cervical cancer: analysis of dose and fractionation schedule. Int J Radiat Oncol Biol Phys 56:1344–1353
Toita T, Moromizato H, Ogawa K et al (2005) Concurrent chemoradiotherapy using high-dose-rate intracavitary brachytherapy for uterine cervical cancer. Gynecol Oncol 96:665–670
Nakano T, Kato S, Ohno T et al (2005) Long-term results of high-dose rate intracavitary brachytherapy for squamous cell carcinoma of the uterine cervix. Cancer (Phila) 103:92–101
Sakata K, Sakurai H, Suzuki Y, Japan Radiation Oncology Study Group et al (2008) Results of concomitant chemoradiation for cervical cancer using high dose rate intracavitary brachytherapy: study of JROSG (Japan Radiation Oncology Study Group). Acta Oncol 47:434–441
Toita T, Kitagawa R, Hamano T, Cervical Cancer (Vulva Cancer) Committee of the Japanese Gynecologic Oncology Group (JGOG) et al (2012) Phase II study of concurrent chemoradiotherapy with high-dose-rate intracavitary brachytherapy in patients with locally advanced uterine cervical cancer: efficacy and toxicity of low cumulative radiation dose schedules. Gynecol Oncol 126:211–216
Parker K, Gallop-Evans E, Hanna L et al (2009) Five years’ experience treating locally advanced cervical cancer with concurrent chemoradiotherapy and high-dose-rate brachytherapy: results from a single institution. Int J Radiat Oncol Biol Phys 74:140–146
Novetsky AP, Einstein MH, Goldberg GL et al (2007) Efficacy and toxicity of concomitant cisplatin with external beam pelvic radiotherapy and two high-dose-rate brachytherapy insertions for treatment of locally advanced cervical cancer. Gynecol Oncol 105:635–640
Atahan IL, Onal C, Ozyar E et al (2007) Long-term outcome and prognostic factors in patients with cervical carcinoma: a retrospective study. Int J Gynecol Cancer 17:833–842
Teh J, Yap SP, Tham I et al (2010) Concurrent chemoradiotherapy incorporating high-dose rate brachytherapy for locally advanced cervical carcinoma: survival outcomes, patterns of failure, and prognostic factors. Int J Gynecol Cancer 20:428–433
Tseng JY, Yen MS, Twu NF et al (2010) Prognostic nomogram for overall survival in stage IIB–IVA cervical cancer patients treated with concurrent chemoradiotherapy. Am J Obstet Gynecol 202:174.e1–7
Hirakawa M, Nagai Y, Toita T et al (2011) High-risk group for locoregional recurrence in patients with stage IB–IIB squamous cell carcinoma of the cervix treated with concurrent chemoradiotherapy. Anticancer Res 31:1437–1442
Hirakawa M, Nagai Y, Inamine M et al (2008) Predictive factors of distant recurrence in locally advanced squamous cell carcinoma of the cervix treated with concurrent chemoradiotherapy. Gynecol Oncol 108:126–129
Kim H, Kim W, Lee M et al (2007) Tumor volume and uterine body invasion assessed by MRI for prediction of outcome in cervical carcinoma treated with concurrent chemotherapy and radiotherapy. Jpn J Clin Oncol 37:858–866
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Kudaka, W., Nagai, Y., Toita, T. et al. Long-term results and prognostic factors in patients with stage III–IVA squamous cell carcinoma of the cervix treated with concurrent chemoradiotherapy from a single institution study. Int J Clin Oncol 18, 916–921 (2013). https://doi.org/10.1007/s10147-012-0457-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10147-012-0457-x