Abstract
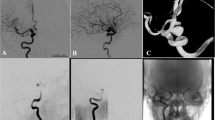
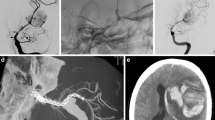
Fusiform aneurysms are less common than saccular aneurysms, but have higher associated mortality and rebleeding rates. Recently, flow diversion has emerged as a possible treatment option. The purpose of this study was to determine the safety and efficacy of the Pipeline Embolization Device (PED) for the treatment of ruptured and unruptured fusiform aneurysms. This was a retrospective analysis of patients with fusiform intracranial aneurysms treated with a PED at a quaternary care center between January 2012 and September 2019. Occlusion rates, neurologic morbidity/mortality, and other clinical variables were analyzed. Twenty-nine patients with 30 fusiform aneurysms were treated with a PED. Sixteen aneurysms (53%) were located in the anterior circulation and 14 aneurysms (47%) were in the posterior circulation. The mean maximal diameter of the aneurysms was 10.1 ± 5.6 mm (range 2.3–25 mm). Angiographic and clinical follow-up were available for 28 aneurysms (93%). The median follow-up was 17.4 months (IQR 4.8 to 28 months) and occlusion rates were graded according to the O’Kelly-Marotta (OKM) scale. Of patients with DSA follow-up, 15 aneurysms (60%) were completely occluded (OKM D) and 19 aneurysms (76%) had a favorable occlusion result (OKM C1-3 and D). The overall complication rate was 26.7% with a neurological morbidity rate of 6.7% and neurological mortality rate of 3.4%. Flow diversion can be an effective treatment for both ruptured and unruptured fusiform aneurysms. Nevertheless, complete occlusion rates are lower than for saccular aneurysms. Therefore, flow diversion should be considered only if other more direct treatment options, such as clipping or stent/coiling are not applicable. Flow diversion should be used cautiously in patients presenting with rupture.
Similar content being viewed by others
References
Alturki AY, Schmalz PG, Ogilvy CS, Thomas AJ (2018) Sequential coiling-assisted deployment of flow diverter for treatment of fusiform middle cerebral artery aneurysms. Oper Neurosurg (Hagerstown) 15:E13–E18
Anson JA, Lawton MT, Spetzler RF (1996) Characteristics and surgical treatment of dolichoectatic and fusiform aneurysms. J Neurosurg 84:185–193. https://doi.org/10.3171/jns.1996.84.2.0185
Awad AJ, Mascitelli JR, Haroun RR, De Leacy RA, Fifi JT, Mocco J (2017) Endovascular management of fusiform aneurysms in the posterior circulation: the era of flow diversion. Neurosurg Focus 42:E14. https://doi.org/10.3171/2017.3.Focus1748
Barletta EA, Ricci RL, Silva RDG, Gaspar R, Araujo JFM, Neves MWF, de Aquino JLB, Barba Belsuzarri TA (2018) Fusiform aneurysms: a review from its pathogenesis to treatment options. Surg Neurol Int 9:189. https://doi.org/10.4103/sni.sni_133_18
Becske T, Brinjikji W, Potts MB, Kallmes DF, Shapiro M, Moran CJ, Levy EI, McDougall CG, Szikora I, Lanzino G, Woo HH, Lopes DK, Siddiqui AH, Albuquerque FC, Fiorella DJ, Saatci I, Cekirge SH, Berez AL, Cher DJ, Berentei Z, Marosfoi M, Nelson PK (2017) Long-term clinical and angiographic outcomes following pipeline embolization device treatment of complex internal carotid artery aneurysms: five-year results of the pipeline for uncoilable or failed aneurysms trial. Neurosurgery 80:40–48. https://doi.org/10.1093/neuros/nyw014
Bhogal P, Perez MA, Ganslandt O, Bazner H, Henkes H, Fischer S (2017) Treatment of posterior circulation non-saccular aneurysms with flow diverters: a single-center experience and review of 56 patients. J Neurointerv Surg 9:471–481. https://doi.org/10.1136/neurintsurg-2016-012781
Damiano RJ, Ma D, Xiang J, Siddiqui AH, Snyder KV, Meng H (2015) Finite element modeling of endovascular coiling and flow diversion enables hemodynamic prediction of complex treatment strategies for intracranial aneurysm. J Biomech 48:3332–3340
Damiano RJ, Tutino VM, Paliwal N, Ma D, Davies JM, Siddiqui AH, Meng H (2017) Compacting a single flow diverter versus overlapping flow diverters for intracranial aneurysms: a computational study. AJNR Am J Neuroradiol 38:603–610. https://doi.org/10.3174/ajnr.A5062
Dashti R, Hernesniemi J, Lehto H, Niemela M, Lehecka M, Rinne J, Porras M, Ronkainen A, Phornsuwannapha S, Koivisto T, Jaaskelainen JE (2007) Microneurosurgical management of proximal anterior cerebral artery aneurysms. Surg Neurol 68:366–377. https://doi.org/10.1016/j.surneu.2007.07.084
Drake CG, Peerless SJ (1997) Giant fusiform intracranial aneurysms: review of 120 patients treated surgically from 1965 to 1992. J Neurosurg 87:141–162. https://doi.org/10.3171/jns.1997.87.2.0141
Fischer S, Perez MA, Kurre W, Albes G, Bäzner H, Henkes H (2014) Pipeline embolization device for the treatment of intra-and extracranial fusiform and dissecting aneurysms: initial experience and long-term follow-up. Neurosurgery 75:364–374
Flemming KD, Wiebers DO, Brown RD Jr, Link MJ, Huston J III, McClelland RL, Christianson TJ (2005) The natural history of radiographically defined vertebrobasilar nonsaccular intracranial aneurysms. Cerebrovasc Dis 20:270–279
Jabbour P, Chalouhi N, Tjoumakaris S, Gonzalez LF, Dumont AS, Randazzo C, Starke RM, Hasan D, Chitale R, Singhal S, Moukarzel LA, Rosenwasser R (2013) The pipeline embolization device: learning curve and predictors of complications and aneurysm obliteration. Neurosurgery 73:113–120; discussion 120. https://doi.org/10.1227/01.neu.0000429844.06955.39
Kabbasch C, Mpotsaris A, Behme D, Dorn F, Stavrinou P, Liebig T (2016) Pipeline embolization device for treatment of intracranial aneurysms-the more, the better? A single-center retrospective observational study. J Vasc Interv Neurol 9:14–20
Kallmes DF, Hanel R, Lopes D, Boccardi E, Bonafe A, Cekirge S, Fiorella D, Jabbour P, Levy E, McDougall C, Siddiqui A, Szikora I, Woo H, Albuquerque F, Bozorgchami H, Dashti SR, Delgado Almandoz JE, Kelly ME, Turner R, Woodward BK, Brinjikji W, Lanzino G, Lylyk P (2015) International retrospective study of the pipeline embolization device: a multicenter aneurysm treatment study. AJNR Am J Neuroradiol 36:108–115. https://doi.org/10.3174/ajnr.A4111
Lin N, Brouillard AM, Krishna C, Mokin M, Natarajan SK, Sonig A, Snyder KV, Levy EI, Siddiqui AH (2015) Use of coils in conjunction with the pipeline embolization device for treatment of intracranial aneurysms. Neurosurgery 76:142–149. https://doi.org/10.1227/neu.0000000000000579
Maragkos GA, Ascanio LC, Salem MM, Gopakumar S, Gomez-Paz S, Enriquez-Marulanda A, Jain A, Schirmer CM, Foreman PM, Griessenauer CJ, Kan P, Ogilvy CS, Thomas AJ (2019) Predictive factors of incomplete aneurysm occlusion after endovascular treatment with the pipeline embolization device. J Neurosurg 132:1–8. https://doi.org/10.3171/2019.1.Jns183226
Monteith SJ, Tsimpas A, Dumont AS, Tjoumakaris S, Gonzalez LF, Rosenwasser RH, Jabbour P (2014) Endovascular treatment of fusiform cerebral aneurysms with the pipeline embolization device. J Neurosurg 120:945–954. https://doi.org/10.3171/2013.12.Jns13945
Munich SA, Tan LA, Keigher KM, Chen M, Moftakhar R, Lopes DK (2014) The pipeline embolization device for the treatment of posterior circulation fusiform aneurysms: lessons learned at a single institution. J Neurosurg 121:1077–1084
Natarajan SK, Lin N, Sonig A, Rai AT, Carpenter JS, Levy EI, Siddiqui AH (2016) The safety of pipeline flow diversion in fusiform vertebrobasilar aneurysms: a consecutive case series with longer-term follow-up from a single US center. J Neurosurg 125:111–119. https://doi.org/10.3171/2015.6.Jns1565
Nelson PK, Lylyk P, Szikora I, Wetzel SG, Wanke I, Fiorella D (2011) The pipeline embolization device for the intracranial treatment of aneurysms trial. AJNR Am J Neuroradiol 32:34–40. https://doi.org/10.3174/ajnr.A2421
O'kelly C, Krings T, Fiorella D, Marotta T (2010) A novel grading scale for the angiographic assessment of intracranial aneurysms treated using flow diverting stents. Interv Neuroradiol 16:133–137
Park MS, Kilburg C, Taussky P, Albuquerque FC, Kallmes DF, Levy EI, Jabbour P, Szikora I, Boccardi E, Hanel RA, Bonafe A, McDougall CG (2016) Pipeline embolization device with or without adjunctive coil embolization: analysis of complications from the IntrePED registry. AJNR Am J Neuroradiol 37:1127–1131. https://doi.org/10.3174/ajnr.A4678
Park MS, Nanaszko M, Sanborn MR, Moon K, Albuquerque FC, McDougall CG (2016) Re-treatment rates after treatment with the pipeline embolization device alone versus pipeline and coil embolization of cerebral aneurysms: a single-center experience. J Neurosurg 125:137–144. https://doi.org/10.3171/2015.7.Jns15582
Park SH, Yim MB, Lee CY, Kim E, Son EI (2008) Intracranial fusiform aneurysms: It's pathogenesis, clinical characteristics and managements. J Korean Neurosurg Soc 44:116–123. https://doi.org/10.3340/jkns.2008.44.3.116
Rouchaud A, Brinjikji W, Lanzino G, Cloft HJ, Kadirvel R, Kallmes DF (2016) Delayed hemorrhagic complications after flow diversion for intracranial aneurysms: a literature overview. Neuroradiology 58:171–177. https://doi.org/10.1007/s00234-015-1615-4
Sacho RH, Saliou G, Kostynskyy A, Menezes R, Tymianski M, Krings T, Radovanovic I, Terbrugge K, Rinkel GJ, Willinsky R (2014) Natural history and outcome after treatment of unruptured intradural fusiform aneurysms. Stroke 45:3251–3256. https://doi.org/10.1161/strokeaha.114.006292
Tan LA, Keigher KM, Munich SA, Moftakhar R, Lopes DK (2015) Thromboembolic complications with pipeline embolization device placement: impact of procedure time, number of stents and pre-procedure P2Y12 reaction unit (PRU) value. J Neurointerv Surg 7:217–221. https://doi.org/10.1136/neurintsurg-2014-011111
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approved
This retrospective chart review study involving human participants was in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The Human Investigation Committee (IRB) of Duke University approved this study.
Informed consent
Informed consent is not applicable as this is a retrospective study. Due to the nature of this retrospective study, it is not feasible to obtain informed consent from study subjects. Subjects to be included may no longer be receiving medical care at Duke University Health System or have current contact information on file at Duke. Further, this study may include deceased subjects, from whom it is not possible to obtain informed consent.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Griffin, A., Lerner, E., Zuchowski, A. et al. Flow diversion of fusiform intracranial aneurysms. Neurosurg Rev 44, 1471–1478 (2021). https://doi.org/10.1007/s10143-020-01332-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-020-01332-0