Abstract
Purpose
In the emergency setting, flank pain commonly leads to a noncontrast CT despite a significant percentage of patients having alternative diagnoses, often difficult to characterize without contrast. We investigated the combined utility of urinalysis and history of urolithiasis in identifying patients who are unlikely to have urolithiasis and may benefit from a contrast-enhanced study.
Methods
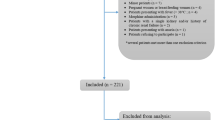
Retrospective review of 350 patients from May 2013 to May 2016 was performed for patients in the emergency department with renal colic that underwent noncontrast CT and urinalysis testing.
Results
Urolithiasis was present in 282 of the 350 patients reviewed (81%), of which 175 (62%) had an obstructing calculus. RBC-positive urinalysis was present in 231 patients with calculi on CT (sensitivity 82%). Patient history of urolithiasis plus urinalysis had a sensitivity of 94% for detecting calculi. Thirty-five patients (10%) had alternative diagnoses, 33 of which were in patients without obstructing calculi. Sixty-seven patients underwent noncontrast CT despite no history of urolithiasis and a negative urinalysis, 10 of which (15%) had alternative diagnoses. Only three cases in this subset (4%) had nonobstructing 1–2-mm calculi, potentially missed with contrast. In this subset, the projected proportion of optimally characterized cases with intravenous contrast is 96%, compared to 85% without contrast (p = .03).
Discussion
Given the high combined sensitivity of urinalysis and patient history (94%), this simple analysis can confidently direct clinicians to a contrast-enhanced CT in “rule-out” cases of flank pain in patients with a negative history and negative urinalysis, particularly given that 15% of these patients had alternative diagnoses.




Similar content being viewed by others
References
Scales CD Jr, Smith AC, Hanley JM et al (2012) Prevalence of kidney stones in the United States. Eur Urol 62:160
Pearle MS, Calhoun EA, Curhan GC (2005) Urologic diseases in America project: urolithiasis. J Urol 173:848–857
Rucker CM, Menias CO, Bhalla S (2004) Mimics of renal colic: alternative diagnoses at unenhanced helical CT. Radiographics 24(suppl 1):S11–S28
Kitagawa M, Kotani T, Miyamoto Y, Kuriu Y, Tsurudome H, Nishi H, Yabe M, Otsuji E (2009) Noncontrast and contrast enhanced computed tomography for diagnosing acute appendicitis: a retrospective study for the usefulness. J Radiol Case Rep 3(6):26–33. https://doi.org/10.3941/jrcr.v3i6.101
Jang HJ, Lim HK, Lee SH, Kim EY, Kim SH (2000) Acute diverticulitis of the cecum and ascending colon: the value of thin-section helical CT findings in excluding colonic carcinoma. AJR Am J Roentgenol 174(5):1397–1402
DeStigter KK, Keating DP (2009) Imaging update: acute colonic diverticulitis. Clin Colon Rectal Surg 22(3):147–155. https://doi.org/10.1055/s-0029-1236158
Dym RJ, Duncan DR, Spektor M, Cohen HW, Scheinfeld MH (2014) Renal stones on portal venous phase contrast-enhanced CT: does intravenous contrast interfere with detection? Abdom Imaging 39(3):526–532
Bove P, Kaplan D, Dalrymple N et al (1999) Reexamining the value of hematuria testing in patients with acute flank pain. J Urol 162:685–687
Teichman JMH (2004) Acute renal calculus from ureteral calculus. N Engl J Med 350:684–693
Dalrymple N, Verga M, Anderson K et al (1998) The value of unenhanced helical computerized tomography in the management of acute flank pain. J Urol 159:735–740
Vieweg J, Chu T, Freed K et al (1998) Unenhanced helical CT for the evaluation of patients with acute flank pain. J Urol 160:679–684
Katz D, Scheer M, Lumerman J, Mellinger B, Stillman C, Lane M (2000) Alternative or additional diagnoses on unenhanced helical computed tomography for suspected renal colic: experience with 1000 consecutive examinations. Urology 56:53–57
Nachmann M, Harkaway R, Summerton S et al (2000) Helical CT scanning: the primary imaging modality for acute flank pain. Am J Emerg Med 18:649–652
Kanzaria HK, Hoffman JR, Probst MA, Caloyeras JP, Berry SH, Brook RH (2015) Emergency physician perceptions of medically unnecessary advanced diagnostic imaging. Acad Emerg Med 22(4):390–398
Drescher FS, Sirovich BE (2016) Use of computed tomography in emergency departments in the United States. JAMA Intern Med 176(2):273–275
Meltzer AC, Pines JM, Richards LM, Mullins P, Mazer-Amirshahi M (2017) US emergency department visits for adults with abdominal and pelvic pain 2007–13: trends in demographics, resource utilization and medication usage. Am J Emerg Med 35(12):1966–1969
Shoenfeld EM, Pekow PS, Shieh M, Scales CD, Lagu T, Lindenauer PK (2017) The diagnosis and management of patients with renal colic across a sample of US hospitals: high CT utilization despite low rates of admission and inpatient urologic intervention. PLoS One 12(1):e0169160
Raja AS, Mortele KJ, Hanson R, Sodickson AD, Zane R, Khorasani R (2011) Abdominal imaging utilization in the emergency department: trends over two decades. Int J Emerg Med 4:19
Rao VM, Levin DC, Parker L, Frangos AJ, Sunshine JH (2011) Trends in utilization rates of the various imaging modalities in emergency departments: nationwide Medicare data from 2000 to 2008. JACR 8(10):706–709
Bellolio MF, Heien HC, Sangaralingham LR, Jeffery MM, Campbell RL, Cabrera D, Shah ND, Hess EP (2017) Increased computed tomography utilization in the emergency department and its association with hospital admission. West J Emerg Med 18(5):835–845
Beckett KR, Moriarity AK, Langer JM (2015) Safe use of contrast media: what the radiologist needs to know. Radiographics 35(6):1738–1750
Anzai Y, Heilbrun ME, Haas D, Boi L, Moshre K, Minoshima S, Kaplan R, Lee VS (2017) Dissecting costs of CT study: application of TDABC (time-driven activity-based costing) in a tertiary academic center. Acad Radiol 24(2):200–208
Perisinakis K, Tzedakis A, Spanakis K, Papadakis AE, Hatzidakis A, Damilakis J (2018) The effect of iodine uptake on radiation dose absorbed by patient tissues in contrast enhanced CT imaging: implications for CT dosimetry. Eur Radiol 28(1):151–158
Dropkin BM, Moses RA, Sharma D, Pais VM Jr (2015) The natural history of nonobstructing asymptomatic renal stones managed with active surveillance. J Urol 193(4):1265–1269
Ordon M, Andonian S, Blew B, Shuler T, Chew B, Pace KT (2015) CUA guideline: management of ureteral calculi. Can Urol Assoc J 9(11–12):E837–E851
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Institutional Review Board approval was obtained for this retrospective study.
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
ESM 1
(XLSX 21 kb)
Rights and permissions
About this article
Cite this article
Desai, V., Cox, M., Deshmukh, S. et al. Contrast-enhanced or noncontrast CT for renal colic: utilizing urinalysis and patient history of urolithiasis to decide. Emerg Radiol 25, 455–460 (2018). https://doi.org/10.1007/s10140-018-1604-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10140-018-1604-0