Abstract
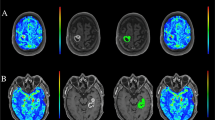
The purpose of the study was to determine the frequency of various unenhanced computed tomography (CT) findings of early cerebral ischemia within brain parenchyma, which could be useful to the radiologist who is interpreting CT studies by indicating the CT finding that is most likely to be present in early cerebral ischemia. We analyzed articles reporting the use of unenhanced CT in acute cerebral ischemia over the period 1976–2009 for frequency of the following brain parenchyma signs: loss of insular ribbon, obscuration of lentiform nucleus, sulcal effacement, and parenchymal hypodensity. We recorded data for the 2-, 3-, 6-, and 12-h intervals after symptom onset from various studies and (1) calculated percent of time intervals in which >50% of patients exhibited the finding in any study and (2) pooled results for patients reported as having a specific CT finding during a specific time interval. We hypothesized that CT findings indicating brain swelling, which would be expected to be a relatively late phenomenon, would be detected at a lower rate in the first 6 h than changes of decreased density of brain tissue and increased density of arteries. The loss of insular ribbon sign (83% of time intervals reported) and obscuration of lentiform nucleus sign (75%) were the most common signs present in >50% patients in a time interval in any article. Pooled results showed that the two most common findings in the first few hours were loss of insular ribbon (70% at 2 h; 77% at 3 h) and obscuration of lentiform nucleus (60% at 2 h; 82% at 3 h). At 6 h, parenchymal hypodensity (53%), loss of insular ribbon (46%), and obscuration of lentiform nucleus (46%) were most common, which validated our hypothesis. At 12 h, loss of insular ribbon (65%) and sulcal effacement (63%) were most common. Loss of insular ribbon and obscuration of lentiform nucleus appear to be the most common signs of early cerebral ischemia identified on unenhanced CT.




Similar content being viewed by others
References
Singer OC, Sitzer M, Du Mesnil de Rochemont R, Neumann-Haefelin T (2004) Practical limitations of acute stroke MRI due to patient-related problems. Neurology 25(62):1848–1849
Truwit CL, Barkovich AJ, Gean-Marton A, Hibri N, Norman D (1990) Loss of the insular ribbon: another early CT sign of acute middle cerebral artery infarction. Radiology 176:801–806
Koga M, Saku Y, Toyoda K, Takaba H, Ibayashi S, Iida M (2003) Reappraisal of early CT signs to predict the arterial occlusion site in acute embolic stroke. J Neurol Neurosurg Psychiatry 74:649–653
Moulin T, Cattin F, Crépin-Leblond T et al (1996) Early CT signs in acute middle cerebral artery infarction: predictive value for subsequent infarct locations and outcome. Neurology 47:366–375
Tomura N, Uemura K, Inugami A et al (1988) Early CT finding in cerebral infarction: obscuration of the lentiform nucleus. Radiology 168:463–467
Furlan A, Higashida R, Wechsler L et al (1999) Intra-arterial prourokinase for acute ischemic stroke. The PROACT II Study: a randomized controlled trial. JAMA 282:2003–2011
NINDS rt-PA Stroke Study Group (1995) Tissue plasminogen activator for acute ischemic stroke. N Engl J Med 333:1581–1587
Patel SC, Levine SR, Tilley BC et al (2001) Lack of clinical significance of early ischemic changes on computed tomography in acute stroke. JAMA 286:2830–2838
Barber PA, Darby DG, Desmond PM et al (1999) Identification of major ischemic change: diffusion-weighted imaging versus computed tomography. Stroke 30:2059–2065
Saur D, Kucinski T, Grzyska U et al (2003) Sensitivity and interrater agreement of CT and diffusion-weighted MR imaging in hyperacute stroke. AJNR Am J Neuroradiol 24:878–885
Roberts HC, Dillon WP, Furlan AJ et al (2002) Computed tomographic findings in patients undergoing intra-arterial thrombolysis for acute ischemic stroke due to middle cerebral artery occlusion: results from the PROACT II trial. Stroke 33:1557–1565
Wardlaw JM, Mielke O (2005) Early signs of brain infarction at CT: observer reliability and outcome after thrombolytic treatment—systematic review. Radiology 235:444–453
Lev MH, Farkas J, Gemmete JJ et al (1999) Acute stroke: improved nonenhanced CT detection—benefits of soft-copy interpretation by using variable window width and center level settings. Radiology 213:150–155
Pexman JH, Barber PA, Hill MD et al (2001) Use of the Alberta Stroke Program Early CT Score (ASPECTS) for assessing CT scans in patients with acute stroke. AJNR Am J Neuroradiol 22:1534–1542
Mullins ME, Lev MH, Schellingerhout D, Koroshetz WJ, Gonzalez RG (2002) Influence of availability of clinical history on detection of early stroke using unenhanced CT and diffusion-weighted MR imaging. AJR Am J Roentgenol 179:223–2238
Fox AJ (2002) Computed tomography of hyperacute infarctions in relation to intra-arterial clot lysis [Editorial]. Stroke 33:1565–1567
Camargo ECS, Furie KL, Singhal AB et al (2007) Acute brain infarct: detection and delineation with CT angiographic source images versus nonenhanced CT scans. Radiology 244:541–548
Aviv R, Shelef I, Malam S et al (2007) Early stroke detection and extent: impact of experience and the role of computed tomography angiography source images. Clin Radiol 62:447–452
Lin K, Kinh KG, Ong P et al (2009) Perfusion CT improves diagnostic accuracy for hyperacute ischemic stroke in the 3-hour window: study of 100 patients with diffusion MRI confirmation. Cerebrovasc Dis 28:72–79
Hopyan JJ, Gladstone DJ, Mallia G et al (2008) Renal safety of CT angiography and perfusion imaging in the emergency evaluation of acute stroke. AJNR Am J Neuroradiol 29:1827–1830
Acknowledgement
The authors acknowledge the very helpful review of the manuscript by Allan J. Fox, MD, FRCPC.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sarikaya, B., Provenzale, J. Frequency of various brain parenchymal findings of early cerebral ischemia on unenhanced CT scans. Emerg Radiol 17, 381–390 (2010). https://doi.org/10.1007/s10140-010-0870-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10140-010-0870-2