Abstract
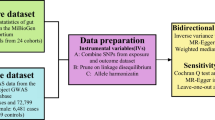
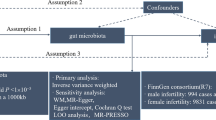
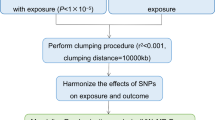
Previous research has confirmed the significant association between gut microbiota (GM) and male infertility (MI), but the causality between them remains unclear. This study aims to investigate the causal relationship between GM and MI using Mendelian randomization (MR) and provide supplementary information for the optimization of future randomized controlled trials (RCTs). Instrumental variables for 211 GM taxa were obtained from genome-wide association studies (GWAS), and inverse variance weighted (IVW) method was used as the main analysis method for two-sample MR analysis to assess the impact of GM on the risk of MI. Four methods were used to test for horizontal pleiotropy and heterogeneity of MR results to ensure the reliability of the MR findings. A total of 50 single-nucleotide polymorphisms (SNPs) closely related to GM were included, and ultimately identified 1 family and 4 general are causally associated with MI. Among them, Anaerotruncus (OR = 1.96, 95% CI 1.31–3.40, P = 0.016) is significantly associated with increased MI risk. Furthermore, we used four MR methods to evaluate the causality, and the results supported these findings. The leave-one-out analysis showed stable results with no instrumental variables exerting strong influence on the results. The causal direction indicated a positive effect, and the effects of heterogeneity and horizontal pleiotropy on the estimation of causal effect were minimized. We confirmed a causal relationship between GM taxa and MI, providing new insights into the mechanisms underlying GM-mediated MI.



Similar content being viewed by others
Data Availability
The gut microbiota and male infertility GWAS summary statistics are available from MiBioGen data (https://mibiogen.gcc.rug.nl/) and the FinnGen data (https://www.finngen.fi), respectively. Both of the GWAS data are publicly available.
Abbreviations
- MR:
-
Mendelian randomization
- MI:
-
Male infertility
- GM:
-
Gut microbiota
- SNPs:
-
Single-nucleotide polymorphisms
- GWAS:
-
Genome-wide association studies
- IVW:
-
Inverse variance weighted
- MR PRESSO:
-
MR pleiotropy residual sum and outlier
- IVs:
-
Instrumental variables
- RCTs:
-
Randomized controlled trials
References
Agarwal, A, Baskaran, S, Parekh, N, Cho, CL, Henkel, R, Vij, S, . . . Shah, R (2021) Male infertility. Lancet, 397(10271), 319–333. https://doi.org/10.1016/S0140-6736(20)32667-2
Al-Asmakh, M, Stukenborg, JB, Reda, A, Anuar, F, Strand, ML, Hedin, L, . . . Söder, O (2014) The gut microbiota and developmental programming of the testis in mice. PLoS One, 9(8), e103809. https://doi.org/10.1371/journal.pone.0103809
Anderson JE, Farr SL, Jamieson DJ, Warner L, Macaluso M (2009) Infertility services reported by men in the United States: national survey data. Fertil Steril 91(6):2466–2470. https://doi.org/10.1016/j.fertnstert.2008.03.022
Bowden J, Spiller W, Del Greco MF, Sheehan N, Thompson J, Minelli C, Smith GD (2018) Improving the visualization, interpretation and analysis of two-sample summary data Mendelian randomization via the Radial plot and Radial regression (vol 47, pg 1264, 2018). Int J Epidemiol 47(6):2100–2100. https://doi.org/10.1093/ije/dyy265
Brion MJ, Shakhbazov K, Visscher PM (2013) Calculating statistical power in Mendelian randomization studies. Int J Epidemiol 42(5):1497–1501. https://doi.org/10.1093/ije/dyt179
Chen, X, Wang, Z, Su, J, Li, H, Xiong, J, Fu, K, . . . Shi, Z (2023) Altitude-dependent metabolite biomarkers reveal the mechanism of plateau pika adaptation to high altitudes. Integr Zool, 18(6), 1041–1055. https://doi.org/10.1111/1749-4877.12710
Colldén, H, Landin, A, Wallenius, V, Elebring, E, Fändriks, L, Nilsson, ME, . . . Ohlsson, C (2019) The gut microbiota is a major regulator of androgen metabolism in intestinal contents. Am J Physiol Endocrinol Metab, 317(6), E1182-e1192. https://doi.org/10.1152/ajpendo.00338.2019
Davey Smith G, Hemani G (2014) Mendelian randomization: genetic anchors for causal inference in epidemiological studies. Hum Mol Genet 23(R1):R89-98. https://doi.org/10.1093/hmg/ddu328
Davies NM, Holmes MV, Davey Smith G (2018) Reading Mendelian randomisation studies: a guide, glossary, and checklist for clinicians. BMJ 362:k601. https://doi.org/10.1136/bmj.k601
Ding, N, Zhang, X, Zhang, XD, Jing, J, Liu, SS, Mu, YP, . . . Zhao, AZ (2020) Impairment of spermatogenesis and sperm motility by the high-fat diet-induced dysbiosis of gut microbes. Gut, 69(9), 1608–1619. https://doi.org/10.1136/gutjnl-2019-319127
Emdin CA, Khera AV, Kathiresan S (2017) Mendelian Randomization Jama 318(19):1925–1926. https://doi.org/10.1001/jama.2017.17219
Farzi A, Fröhlich EE, Holzer P (2018) Gut microbiota and the neuroendocrine system. Neurotherapeutics 15(1):5–22. https://doi.org/10.1007/s13311-017-0600-5
Golubeva, AV, Crampton, S, Desbonnet, L, Edge, D, O'Sullivan, O, Lomasney, KW, . . . Cryan, JF (2015) Prenatal stress-induced alterations in major physiological systems correlate with gut microbiota composition in adulthood. Psychoneuroendocrinology, 60, 58–74. https://doi.org/10.1016/j.psyneuen.2015.06.002
Hao, Y, Feng, Y, Yan, X, Chen, L, Zhong, R, Tang, X, . . . Zhao, Y (2022) Gut microbiota-testis axis: FMT improves systemic and testicular micro-environment to increase semen quality in type 1 diabetes. Mol Med, 28(1), 45. https://doi.org/10.1186/s10020-022-00473-w
Hemani, G, Zheng, J, Elsworth, B, Wade, KH, Haberland, V, Baird, D, . . . Haycock, PC (2018) The MR-Base platform supports systematic causal inference across the human phenome. Elife, 7. https://doi.org/10.7554/eLife.34408
Hemani, G, Zhengn, J, Elsworth, B, Wade, KH, Haberland, V, Baird, D, . . . Haycock, PC (2018) The MR-Base platform supports systematic causal inference across the human phenome. Elife, 7. ARTN e34408 https://doi.org/10.7554/eLife.34408
Hudry, B, de Goeij, E, Mineo, A, Gaspar, P, Hadjieconomou, D, Studd, C, . . . Miguel-Aliaga, I (2019) Sex differences in intestinal carbohydrate metabolism promote food intake and sperm maturation. Cell, 178(4), 901–918.e916. https://doi.org/10.1016/j.cell.2019.07.029
Hwang LD, Lawlor DA, Freathy RM, Evans DM, Warrington NM (2019) Using a two-sample Mendelian randomization design to investigate a possible causal effect of maternal lipid concentrations on offspring birth weight. Int J Epidemiol 48(5):1457–1467. https://doi.org/10.1093/ije/dyz160
Kurilshikov A, Wijmenga C, Fu J, Zhernakova A (2017) Host genetics and gut microbiome: challenges and perspectives. Trends Immunol 38(9):633–647. https://doi.org/10.1016/j.it.2017.06.003
Kurilshikov, A, Medina-Gomez, C, Bacigalupe, R, Radjabzadeh, D, Wang, J, Demirkan, A, . . . Zhernakova, A (2021) Large-scale association analyses identify host factors influencing human gut microbiome composition. Nat Genet, 53(2), 156–165. https://doi.org/10.1038/s41588-020-00763-1
Li, P, Wang, H, Guo, L, Gou, X, Chen, G, Lin, D, . . . Liu, Z (2022) Association between gut microbiota and preeclampsia-eclampsia: a two-sample Mendelian randomization study. BMC Med, 20(1), 443. https://doi.org/10.1186/s12916-022-02657-x
Liu L, Shu A, Zhu Y, Chen Y (2021) Cornuside alleviates diabetes mellitus-induced testicular damage by modulating the gut microbiota. Evid Based Complement Alternat Med 2021:5301942. https://doi.org/10.1155/2021/5301942
Liu K, Zou J, Fan H, Hu H, You Z (2022) Causal effects of gut microbiota on diabetic retinopathy: a Mendelian randomization study. Front Immunol 13:930318. https://doi.org/10.3389/fimmu.2022.930318
Lundy, SD, Sangwan, N, Parekh, NV, Selvam, MKP, Gupta, S, McCaffrey, P, . . . Eng, C (2021) Functional and taxonomic dysbiosis of the gut, urine, and semen microbiomes in male infertility. Eur Urol, 79(6), 826–836. https://doi.org/10.1016/j.eururo.2021.01.014
Malivindi, R, Rago, V, De Rose, D, Gervasi, MC, Cione, E, Russo, G, . . . Aquila, S (2018) Influence of all-trans retinoic acid on sperm metabolism and oxidative stress: its involvement in the physiopathology of varicocele-associated male infertility. J Cellular Physiol, 233(12), 9526–9537. https://doi.org/10.1002/jcp.26872
Markle, JG, Frank, DN, Mortin-Toth, S, Robertson, CE, Feazel, LM, Rolle-Kampczyk, U, . . . Danska, JS (2013) Sex differences in the gut microbiome drive hormone-dependent regulation of autoimmunity. Science, 339(6123), 1084–1088. https://doi.org/10.1126/science.1233521
Mondot S, de Wouters T, Doré J, Lepage P (2013) The human gut microbiome and its dysfunctions. Dig Dis 31(3–4):278–285. https://doi.org/10.1159/000354678
Pagoni P, Dimou NL, Murphy N, Stergiakouli E (2019) Using Mendelian randomisation to assess causality in observational studies. Evid Based Ment Health 22(2):67–71. https://doi.org/10.1136/ebmental-2019-300085
Panghal A, Jena G (2023) Gut-gonad perturbations in type-1 diabetes mellitus: role of dysbiosis, oxidative stress, inflammation and energy-dysbalance. Curr Diabetes Rev. https://doi.org/10.2174/1573399820666230822151740
Skrivankova, VW, Richmond, RC, Woolf, BAR, Yarmolinsky, J, Davies, NM, Swanson, SA, . . . Richards, JB (2021) Strengthening the reporting of observational studies in epidemiology using Mendelian randomization: the STROBE-MR statement. Jama, 326(16), 1614–1621. https://doi.org/10.1001/jama.2021.18236
Sun, BB, Kurki, MI, Foley, CN, Mechakra, A, Chen, CY, Marshall, E, . . . Runz, H (2022) Genetic associations of protein-coding variants in human disease. Nature, 603(7899), 95–102. https://doi.org/10.1038/s41586-022-04394-w
Vander Borght M, Wyns C (2018) Fertility and infertility: definition and epidemiology. Clin Biochem 62:2–10. https://doi.org/10.1016/j.clinbiochem.2018.03.012
Verbanck M, Chen CY, Neale B, Do R (2018a) Detection of widespread horizontal pleiotropy in causal relationships inferred from Mendelian randomization between complex traits and diseases. Nat Genet 50(5):693–698. https://doi.org/10.1038/s41588-018-0099-7
Verbanck M, Chen CY, Neale B, Do R (2018b) Detection of widespread horizontal pleiotropy in causal relationships inferred from Mendelian randomization between complex traits and diseases (vol 50, 693, 2018). Nat Genet 50(8):1196–1196. https://doi.org/10.1038/s41588-018-0164-2
Wang Y, Xie Z (2022) Exploring the role of gut microbiome in male reproduction. Andrology 10(3):441–450. https://doi.org/10.1111/andr.13143
Wootton, RE, Lawn, RB, Millard, LAC, Davies, NM, Taylor, AE, Munafo, MR, . . . Haworth, CMA (2018) Evaluation of the causal effects between subjective wellbeing and cardiometabolic health: mendelian randomisation study. Bmj-British Med J, 362. ARTN k3788 https://doi.org/10.1136/bmj.k3788
Xue HR, Shen XT, Pan W (2021) Constrained maximum likelihood-based Mendelian randomization robust to both correlated and uncorrelated pleiotropic effects. Am J Hum Genet 108(7):1251–1269. https://doi.org/10.1016/j.ajhg.2021.05.014
Yang, XL, Zhu, QT, Zhang, L, Pei, YF, Xu, XJ, Liu, XN, . . . Wang, Y (2022) Causal relationship between gut microbiota and serum vitamin D: evidence from genetic correlation and Mendelian randomization study. Eur J Clin Nutrition, 76(7), 1017–1023. https://doi.org/10.1038/s41430-021-01065-3
Yeung CHC, Au Yeung SL, Kwok MK, Zhao JV, Schooling CM (2023) The influence of growth and sex hormones on risk of Alzheimer’s disease: a mendelian randomization study. Eur J Epidemiol 38(7):745–755. https://doi.org/10.1007/s10654-023-01015-2
Yuan C, Xiang LY, Jian ZY, Liao BH (2023) Vitamin D levels and risk of male factor infertility: a Mendelian randomization study. World J Mens Health. https://doi.org/10.5534/wjmh.220109
Zeng Y, Cao S, Yang H (2023) Roles of gut microbiome in epilepsy risk: a Mendelian randomization study. Front Microbiol 14:1115014. https://doi.org/10.3389/fmicb.2023.1115014
Zhang, PF, Feng, YN, Li, L, Ge, W, Yu, S, Hao, YA, . . . Zhao, Y (2021) Improvement in sperm quality and spermatogenesis following faecal microbiota transplantation from alginate oligosaccharide dosed mice. Gut, 70(1), 222-+. https://doi.org/10.1136/gutjnl-2020-320992
Zhang, T, Sun, P, Geng, Q, Fan, H, Gong, Y, Hu, Y, . . . Zhou, Y (2022a) Disrupted spermatogenesis in a metabolic syndrome model: the role of vitamin A metabolism in the gut-testis axis. Gut, 71(1), 78–87. https://doi.org/10.1136/gutjnl-2020-323347
Zhang, T, Sun, P, Geng, Q, Fan, H, Gong, YT, Hu, YT, . . . Zhou, Y (2022b) Disrupted spermatogenesis in a metabolic syndrome model: the role of vitamin A metabolism in the gut-testis axis. Gut, 71(1), 78–87. https://doi.org/10.1136/gutjnl-2020-323347
Zhao QY, Wang JS, Hemani G, Bowden J, Small DS (2020a) Statistical inference in two-sample summary-data Mendelian randomization using robust adjusted profile score. Ann Stat 48(3):1742–1769. https://doi.org/10.1214/19-Aos1866
Zhao, Y, Zhang, PF, Ge, W, Feng, YN, Li, L, Sun, ZY, . . . Shen, W (2020) Alginate oligosaccharides improve germ cell development and testicular microenvironment to rescue busulfan disrupted spermatogenesis. Theranostics, 10(7), 3308–3324. https://doi.org/10.7150/thno.43189
Acknowledgements
Not applicable.
Funding
This work was supported by Medical Research Subject of Jiangsu Provincial Health Commission (ZDB2020020) and the National Natural Science Foundation of China, Regional Science Foundation Project (82060866).
Author information
Authors and Affiliations
Contributions
Conceptualization: Runpei Deng, Qingqi Zeng. Data curation: Runpei Deng, Yebao Huang, Zhaohui Tian. Formal analysis: Runpei Deng, Yebao Huang. Funding acquisition: Qingqi Zeng, Yebao Huang. Investigation:Runpei Deng, Qingqi Zeng. Methodology: Runpei Deng, Yebao Huang. Project administration: Runpei Deng, Yebao Huang, Qingqi Zeng. Resources: Runpei Deng, Yebao Huang, Zhaohui Tian. Software: Runpei Deng, Yebao Huang. Supervision: Runpei Deng. Validation: Runpei Deng, Yebao Huang, Zhaohui Tian. Visualization: Runpei Deng, Yebao Huang. Writing—original draft: Runpei Deng. Writing—review and editing: Runpei Ddeng, Yebao Huang, Zhaohui Tian, Qingqi Zeng.
All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Deng, R., Huang, Y., Tian, Z. et al. Association between gut microbiota and male infertility: a two-sample Mendelian randomization study. Int Microbiol (2024). https://doi.org/10.1007/s10123-024-00512-y
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10123-024-00512-y