Abstract
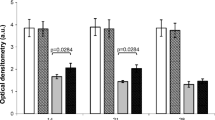
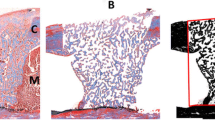
Laser-photobiomodulation (L-PBM) has been widely studied and its biomodulatory effects have been established on irradiated cells, increasing viability and proliferation and on damaged tissues. In addition, L-PBM may reduce and modulate the inflammatory process. The effect of 660-nm and 808-nm laser-photobiomodulation on bone repair around titanium dental implants placed in rat’s femur was evaluated by histomorphometry. Twenty-seven Wistar rats were divided into 3 groups of nine animals: group C — non-irradiated control; group R — λ=660nm irradiated; and group IR — λ=808nm irradiated. Each group was further divided in 3 subgroups of three animals each, according to histomorphometry analysis in 3 days, 7 days, and 14 days after irradiation. Histological H.E.-stained slides were photographed, and bone matrix measured in new-formed bone area. Bone matrix histomorphometry analysis indicates that at 7 days in the irradiated groups (R and IR), a bigger area matrix was observed in relation to control group (C) (p=0.04 and p=0.048 respectively). On the other hand, at 14 days, control group (C) presented a bigger area than infrared irradiated (IR) (p=0.001) and red irradiated group (R) also showed a bigger area than infrared irradiated group (IR) (p=0.019). Histological analysis indicates that irradiated groups (R and IR) exhibited a faster bone tissue matrix production than control group
Graphical abstract






Similar content being viewed by others
References
Al_Wattar WM (2021) Effect of low energy laser on the healing of tooth extraction wound: (Histological Study in Rat). Iraqi J Laser 20(1):30–38
Blay A, Blay CC, Tunchel S, Gehrke SA, Shibli JA, Groth EB, Zezell DM (2016) Effects of a low intensity laser on dental implant osseointegration: removal torque and resonance frequency analysis in rabbits. J Oral Implantol 42(4):316–20. https://doi.org/10.1563/aaid-joi-D-15-00064
Bosshardt DD, Chappuis V, Buser D (2000) Osseointegration of titanium, titanium alloy and zirconia dental implants: current knowledge and open questions. Periodontology 73(2017):22–40
Campanha BP, Gallina C, Geremia T, Loro RC, Valiati R, Hübler R, de Oliveira MG (2010) Low-level laser therapy for implants without initial stability. Photomed Laser Surg 28(3):365–9. https://doi.org/10.1089/pho.2008.2429
Cavalcanti MF, Maria DA, de Isla N, Leal-Junior EC, Joensen J, Bjordal JM, Lopes-Martins RA, Diomede F, Trubiani O, Frigo L (2015) Evaluation of the proliferative effects induced by low-level laser therapy in bone marrow stem cell culture. Photomed Laser Surg. 33(12):610–6. https://doi.org/10.1089/pho.2014.3864
Chen Y, Liu C, Chen X, Mo A (2019) Clinical evidence of photobiomodulation therapy (PBMT) on implant stability and success: a systematic review and meta-analysis. BMC Oral Health 19(1):77
De Vasconcellos LM, Barbara MA, Deco CP et al (2014) Healing of normal and osteopenic bone with titanium implant and low-level laser therapy (GaAlAs): a histomorphometric study in rats. Lasers Med Sci 29:575–580
De Vasconcellos LM, Barbara MA, Rovai ES et al (2016) Titanium scaffold osteogenesis in healthy and osteoporotic rats is improved by the use of low-level laser therapy (GaAlAs). Lasers Med Sci 31:899–905
Dörtbudak O, Haas R, Mailath-Pokorny G (2002) Effect of low-power laser irradiation on bony implant sites. Clin Oral Implants Res 13(3):288–92
Ferreira AN, Silveira L, Genovese WJ, de Araújo VC, Frigo L, de Mesquita RA, Guedes E (2006) Effect of GaAIAs laser on reactional dentinogenesis induction in human teeth. Photomed Laser Surg 24(3):358–65
Frigo L, Fávero GM, Lima HJ, Maria DA, Bjordal JM, Joensen J, Iversen VV, Marcos RL, Parizzoto NA, Lopes-Martins RA (2010) Low-level laser irradiation (InGaAlP-660 nm) increases fibroblast cell proliferation and reduces cell death in a dose-dependent manner. Photomed Laser Surg. 28(Suppl 1):S151-6. https://doi.org/10.1089/pho.2008.2475
Fujimoto K, Kiyosaki T, Mitsui N et al (2010) Low-intensity laser irradiation stimulates mineralization via increased BMPs in MC3T3-E1 cells. Lasers Surg Med 42:519–526
Guglielmotti MB, Olmedo DG, Cabrini RL (2000) Research on implants and osseointegration. Periodontology 2019(79):178–189
Hamblin MR (2017) Mechanisms and applications of the anti-inflammatory effects of photobiomodulation. AIMS Biophys 4(3):337–361. https://doi.org/10.3934/biophy.2017.3.337
Hosseinpour S, Fekrazad R, Arany PR, Ye Q (2019) Molecular impacts of photobiomodulation on bone regeneration: a systematic review. Prog Biophys Mol Biol 149:147–159. https://doi.org/10.1016/j.pbiomolbio.2019.04.005
Khadra M, Rønold HJ, Lyngstadaas SP, Ellingsen JE, Haanaes HR (2004) Low-level laser therapy stimulates bone-implant interaction: an experimental study in rabbits. Clin Oral Implants Res 15(3):325–32
Luca Francetti NC, Taschieri Silvio, Corbella Stefano (2019) Ten years follow-up retrospective study on implant survival rates and prevalence of peri-implantitis in implant-supported full-arch rehabilitations. Clin Oral Implants Res 30:8
Massotti FP, Gomes FV, Mayer L, de Oliveira MG, Baraldi CE, Ponzoni D et al (2015) Histomorphometric assessment of the influence of low-level laser therapy on peri-implant tissue healing in the rabbit mandible. Photomed Laser Surg 33:123–8
Mussttaf RA, Jenkins DFL, Jha AN (2019) Assessing the impact of low level laser therapy (LLLT) on biological systems: a review. Int J Radiat Biol 95(2):120–143. https://doi.org/10.1080/09553002.2019.1524944
Oh SL, Shiau HJ, Reynolds MA (2020) Survival of dental implants at sites after implant failure: a systematic review. J Prosthet Dent 123(1):54–60. https://doi.org/10.1016/j.prosdent.2018.11.007
Pallotta RC, Bjordal JM, Frigo L, Leal Junior EC, Teixeira S, Marcos RL, Ramos L, MessiasFde M, Lopes-Martins RA (2012) Infrared (810-nm) low-level laser therapy on rat experimental knee inflammation. Lasers Med Sci 27(1):71–8. https://doi.org/10.1007/s10103-011-0906-1
Petrellis MC, Frigo L, Marcos RL, Pallotta RC, de Carvalho MHC, Muscará MN, Maria DA, Lopes-Martins RÁB (2017) Laser photobiomodulation of pro-inflammatory mediators on Walker Tumor 256 induced rats. J Photochem Photobiol B 177:69–75. https://doi.org/10.1016/j.jphotobiol.2017.09.011
Piva JA, Abreu EM, Silva Vdos S, Nicolau RA (2011) Effect of low-level laser therapy on the initial stages of tissue repair: basic principles. An Bras Dermatol 86(5):947–54
Ruh AC, Frigo L, Cavalcanti MFXB, Svidnicki P, Vicari VN, Lopes-Martins RAB, Leal Junior ECP, De Isla N, Diomede F, Trubiani O, Favero GM (2018) Laser photobiomodulation in pressure ulcer healing of human diabetic patients: gene expression analysis of inflammatory biochemical markers. Lasers Med Sci 33(1):165–171. https://doi.org/10.1007/s10103-017-2384-6
Wang P, Li T (2019) Which wavelength is optimal for transcranial low-level laser stimulation? J Biophotonics 12(2):e201800173. https://doi.org/10.1002/jbio.201800173
Wu Q, Xuan W, Ando T, Xu T, Huang L, Huang YY, Dai T, Dhital S, Sharma SK, Whalen MJ, Hamblin MR (2012) Low-level laser therapy for closed-head traumatic brain injury in mice: effect of different wavelengths. Lasers Surg Med 44(3):218–26. https://doi.org/10.1002/lsm.22003
Acknowledgements
We would like to thank DentoflexTM — Brazil that gently provided all the implant material used in this experiment.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Ethical consideration
This work was approved by the ethics committee of Universidade Federal de Pernambuco, Brazil, number: 23076.026402/2011-17 and respects laws of using animals for scientific purposes, in accordance with the ethical standards of the Helsinki Declaration of 1975 and revised in 2000.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
da Fonseca, G.A.M.D., Cavalcanti, M.F.X.B., de Souza Maior, J.D. et al. Laser-photobiomodulation on titanium implant bone healing in rat model: comparison between 660- and 808-nm wavelength. Lasers Med Sci 37, 2179–2184 (2022). https://doi.org/10.1007/s10103-021-03481-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-021-03481-0