Abstract
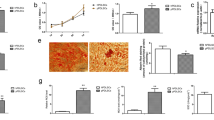
Photobiomodulation (PBM) has been used to modulate the inflammatory and immune responses, pain relief, and to promote wound healing. PBM is widely used in dental practice and its cellular effects should be investigated. The aim was to evaluate if PBM changes proteins cell death–related, such as caspase-6 and Bcl-2, in periodontal ligament cells. Eighteen mice were divided in three groups (n = 6), i.e., (I) control, (II) 3 J cm−2, and (III) 30 J cm−2. Low power infrared laser (830 nm) parameters were power at 10 mW, energy densities at 3 and 30 J cm−2 in continuous emission mode, exposure time of 15 and 150 s, respectively for 4 days in a row. Twenty-four hours after last irradiation, the animals were euthanized, and their jaws were fixed and decalcified. Caspase-6 and Bcl-2 were analyzed by real-time polymerase chain reaction and immunocytochemical techniques, and DNA fragmentation was evaluated by TUNEL. Statistical differences were not significant to caspase-6 mRNA relative levels in tissues from jaws at both energy densities, but a significant increase of Bcl-2 mRNA relative levels was obtained at 30 J cm−2 group. Also, 30 J cm−2 group showed caspase-6 positive–labeled cells decreased and Bcl-2 positive–labeled cells significantly increased. TUNEL-labeled cells demonstrated DNA fragmentation decreased at 30 J cm−2. PBM can alter Bcl-2 mRNA relative level and both caspase-6 and Bcl-2 protein, modulating cell survival, as well as to reduce DNA fragmentation. More studies must be performed in order to obtain conclusive results about photobiostimulation effects using infrared low-level laser in apoptosis process as to achieve the optimum dosage.




Similar content being viewed by others
References
Hamblin MR (2018) Mechanisms and mitochondrial redox signaling in photobiomodulation. Photochem Photobiol 94(2):199–212. https://doi.org/10.1111/php.12864
Karu TI (2008) Mitochondrial signaling in mammalian cells activated by red and near-IR radiation. Photochem Photobiol 84(5):1091–1099. https://doi.org/10.1111/j.1751-1097.2008.00394.x
Freitas LF, Hamblim MR (2016) Proposed mechanism of photobiomodulation or low-level light therapy. IEEE J Sel Top Quantum Electron 22(3):1–37. https://doi.org/10.1109/JSTQE.2016.2561201
Wu S, Xing D, Gao X, Chen WR (2009) High fluence low-power laser irradiation induces mitochondrial permeability transition mediated by reactive oxygen species. J Cell Physiol 218(3):603–611. https://doi.org/10.1002/jcp.21636
Rahman SU, Mosca RC, Govindool Reddy S et al (2018) Learning from clinical phenotypes: low-dose biophotonics therapies in oral diseases. Oral Dis 24(1-2):261–276. https://doi.org/10.1111/odi.12796
Javed F, Kellesarian SV, Romanos GE (2017) Role of diode lasers in oro-facial pain management. J Biol Regul Homeost Agents 31(1):153–155
Fornaini C, Rocca JP, Bertrand MF et al (2007) Nd:YAG and diode laser in the surgical management of soft tissues related to orthodontic treatment. Photomed Laser Surg 25(5):381–392. https://doi.org/10.1089/pho.2006.2068
Seo BM, Miura M, Gronthos S et al (2004) Investigation of multipotent postnatal stem cells from human periodontal ligament. Lancet 364(9429):149–155. https://doi.org/10.1016/s0140-6736(04)16627-0
Liu L, Zhang Z, Xing D (2011) Cell death via mitochondrial apoptotic pathway due to activation of Bax by lysosomal photodamage. Free Radic Biol Med 51(1):53–68. https://doi.org/10.1016/j.freeradbiomed.2011.03.042
Saraste A, Pulkki K (2000) Morphologic and biochemical hallmarks of apoptosis. Cardiovasc Res 45(3):528–537. https://doi.org/10.1016/s0008-6363(99)00384-3
Untergasser A, Cutcutache I, Koressaar T et al (2012) Primer3--new capabilities and interfaces. Nucleic Acids Res 40(15):e115. https://doi.org/10.1093/nar/gks596
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)). Methods 25(4):402–408. https://doi.org/10.1006/meth.2001.1262
Cavalcanti TM, Almeida-Barros RQ, Catão MH et al (2011) Knowledge of the physical properties and interaction of laser with biological tissue in dentistry. An Bras Dermatol 86(5):955–960 https://doi.org/10.1590/S0365-05962011000500014
Gao X, Xing D (2009) Molecular mechanisms of cell proliferation induced by low power laser irradiation. J Biomed Sci 16:4. https://doi.org/10.1186/1423-0127-16-4
Fonseca AS, Moreira TO, Paixão DL et al (2012) Effect of laser therapy on DNA damage. Lasers Surg Med 42(6):481–488. https://doi.org/10.1002/lsm.20921
Sergio LP, Campos VM, Vicentini SC et al (2016) Low-intensity red and infrared lasers affect mRNA expression of DNA nucleotide excision repair in skin and muscle tissue. Lasers Med Sci 31(3):429–435. https://doi.org/10.1007/s10103-016-1870-6
de Souza da Fonseca A, Mencalha AL, Araújo de Campos VM et al (2013) DNA repair gene expression in biological tissues exposed to low-intensity infrared laser. Lasers Med Sci 28(4):1077–1084. https://doi.org/10.1007/s10103-012-1191-3
da Silva PAV, Dos Anjos LMJ, Abduch TF et al (2019) Photobiomodulation can alter mRNA levels cell death-related. Lasers Med Sci 34(7):1373–1380. https://doi.org/10.1007/s10103-019-02732-5
Gulabivala K, Ng YL (2014) Tooth organogenesis, morphology and physiology. In Endodontics, 4th ed. Mosby 2–32. https://doi.org/10.1016/b978-0-7020-3155-7.00001-1
Nagata S (2018) Apoptosis and clearance of apoptotic cells. 36:489–517. https://doi.org/10.1146/annurev-immunol-042617-053010
Elmore S (2007) Apoptosis: a review of programmed cell death. Toxicol Pathol 35(4):495–516. https://doi.org/10.1080/01926230701320337
Yuan S, Akey CW (2013) Apoptosome structure, assembly, and procaspase activation. Structure 21(4):501–515. https://doi.org/10.1016/j.str.2013.02.024
Schinzel A, Kaufmann T, Borner C (2004) Bcl-2 family members: integrators of survival and death signals in physiology and pathology [corrected]. Biochim Biophys Acta 1644(2-3):95–105. https://doi.org/10.1016/j.bbamcr.2003.09.006
Cory S, Adams JM (2002) The Bcl2 family: regulators of the cellular life-or-death switch. Nat Rev Cancer 2(9):647–656. https://doi.org/10.1038/nrc883
Kushibiki T, Hirasawa T, Okawa S, Ishihara M (2013) Blue laser irradiation generates intracellular reactive oxygen species in various types of cells. Photomed Laser Surg 31(3):95–104. https://doi.org/10.1089/pho.2012.3361
De Paoli F, Cerqueira LR, Ramos MM et al (2015) DNA fragmentation and nuclear phenotype in tendons exposed to low-intensity infrared laser. Spie Digit Libr 9321:1–12. https://doi.org/10.1117/12.2075726
Dos Anjos LMJ, da Fonseca AS, Gameiro J, de Paoli F (2017) Apoptosis induced by low-level laser in polymorphonuclear cells of acute joint inflammation: comparative analysis of two energy densities. Lasers Med Sci 32(5):975–983. https://doi.org/10.1007/s10103-017-2196-8
Gao X, Xing D (2009) Molecular mechanisms of cell proliferation induced by low power laser irradiation. J Biomed Sci 16:4. https://doi.org/10.1186/1423-0127-16-4
Funding
This work was supported by Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq/Process no. 474405/2013-3), Fundação de Amparo à Pesquisa do Estado de Minas Gerais (FAPEMIG/Process no. CDS APQ 02123/15), and Universidade Federal de Juiz de Fora (UFJF).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they do not have conflict of interests.
Ethical approval
All procedures performed in studies involving animals were in accordance with the ethical standards of the institution or practice at which the studies were conducted. All experimental procedures were submitted and approved by the Ethical Committee of the University of Juiz de Fora (protocol no. 039/2014).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Faria, L.V., Andrade, I.N., dos Anjos, L.M.J. et al. Photobiomodulation can prevent apoptosis in cells from mouse periodontal ligament. Lasers Med Sci 35, 1841–1848 (2020). https://doi.org/10.1007/s10103-020-03044-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-020-03044-9