Abstract
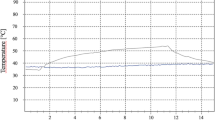
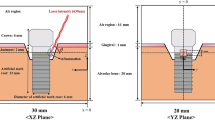
The prevalence of peri-implantitis and the absence of a standard approach for decontamination of the dental implant surface have led to searches for effective therapies. Since the source of diode lasers is portable, has reduced cost, and does not cause damage to the titanium surface of the implant, high-power diode lasers have been used for this purpose. The effect of laser irradiation on the implants is the elevation of the temperature surface. If this elevation exceeds 47 °C, the bone tissue is irreversibly damaged, so for a safety therapy, the laser parameters should be controlled. In this study, a diode laser of GaAsAl was used to irradiate titanium dental implants, for powers 1.32 to 2.64 W (real) or 2.00 to 4.00 W (nominal), in continuous/pulsed mode DC/AC, with exposure time of 5/10 s, with/without air flow for cooling. The elevation of the temperature was monitored in real time in two positions: cervical and apical. The best results for decontamination using a 968-nm diode laser were obtained for a power of 1.65 and 1.98 W (real) for 10 s, in DC or AC mode, with an air flow of 2.5 l/min. In our perspective in this article, we determine a suggested approach for decontamination of the dental implant surface using a 968-nm diode laser.





Similar content being viewed by others
References
Buser D, Janner SFM, Wittneben JG, Brägger U, Ramseier CA, Salvi GE (2012) 10-year survival and success rates of 511 titanium implants with a sandblasted and acid-etched surface: a retrospective study in 303 partially edentulous patients. Clin Implant Dent Relat Res 14(6):839–851
Dierens M, Vandeweghe S, Kisch J, Nilner K, De Bruyn H (2012) Long-term follow-up of turned single implants placed in periodontally healthy patients after 16-22 years: radio- graphic and peri-implant outcome. Clin Oral Implants Res 23:197–204
Lindhe J, Meyle J (2008) Peri-implant diseases: consensus report of the sixth European workshop on periodontology. J Clin Periodontol 35(8):282–285
Koldsland OC, Scheie AA, Aass AM (2010) Prevalence of peri-implantitis related to severity of the disease with different degrees of bone loss. J Periodontol 81(2):231–238
Atieh MA, Alsabeeha NHM, Faggion CM Jr, Duncan WJ (2013) The frequency of peri-implant diseases: a systematic review and meta-analysis. J Periodontol 84(11):1586–1598
Algraffee H, Borumand F, Cascarini L (2012) Peri-implantitis. Braz J Oral Maxillofac Surg 50(8):689–694
Kotsovilis S, Karoussis IK, Trianti M, Fourmousis I (2008) Therapy of peri-implantitis: a systematic review. J Clin Periodontol 35(7):621–629
Kamel MS, Khosa A, Tawse-Smith A, Leichter J (2014) The use of laser therapy for dental implant surface decontamination: a narrative review of in vitro studies. Lasers Med Sci 29(6):1977–1985
Kotsakis GA, Konstantinnidis I, Karoussis IK, Ma X, Chu H (2014) Systematic review and meta-analysis of the effect of various laser wavelengths in the treatment of peri-implantitis. J Periodontol 85(9):1203–1213
Mailoa J, Lin GH, Chan HL, MacEachern M, Wang HL (2014) Clinical outcomes of using lasers for peri-implantitis surface detoxification: a systematic review and meta-analysis. J Periodontol 85(9):1194–202
Gerber J, Wenaweser D, Heitz-Mayfield L, Lang NP, Persson GR (2006) Comparison of bacterial plaque samples from titanium implant and tooth surfaces by different methods. Clin Oral Implants Res 17(1):1–7
Shibli JA, Martins MC, Lotufo RF, Marcantonio E Jr (2003) Microbiologic and radiographic analysis of ligature-induced peri-implantitis with different dental implant surfaces. Int J Oral Maxillofac lmplants 18(3):383–390
Romanos GE, Everts H, Nentwing GH (2000) Effects of diode and Nd:YAG laser irradiation on titanium discs: a scanning electron microscope examination. J Periodontol 71(5):810–815
Pirnat S (2007) Versatility of an 810 nm diode laser in dentistry: an overview. J Laser Health Acad 2007(4):1–9
Kreisler M, Götz H, Duschne H (2002) Effect of Nd:YAG, Ho:YAG, Er:YAG, CO2, and GaAIAs laser irradiation on surface properties of endosseous dental implants. Int J Oral Maxillofac Implants 17(2):202–211
Romanos GE, Nentwig GH (1999) Diode laser (980 nm) in oral and maxillofacial surgical procedures: clinical observations based on clinical applications. J Clin Laser Med Surg 17(5):193–19
Kreisler M, Al Haj H, D’hoedt B (2003) Temperature changes induced by 809-nm GaAlAs laser at the implant-bone interface during simulated surface decontamination. Clin Oral Implants Res 14(1):91–96
Sennhenn-Kirchner S, Klaue S, Wolff N, Mergeryan H, Zepelin MB, Jacobs H (2007) Decontamination of rough titanium surfaces with diode lasers: microbiological findings on in vivo grown biofilms. Clin Oral Implants Res 18:126–132
Gonçalves F, Zanetti AL, Zanetti RV, Martelli FS, Avila-Campos MJ, Tomazino LF, Granjeiro JM (2010) Effectiveness of 980-mm diode and 1064-nm extra-long-pulse neodymium-doped yttrium aluminum garnet lasers in implant disinfection. Photomed Laser Surg 28(2):273–280
Hauser-Gerspach I, Stübinger S, Meyer J (2010) Bactericidal effects of different laser systems on bacteria adhered to dental implant surfaces: an in vitro study comparing zirconia with titanium. Clin Oral Implants Res 21:277–283
Eriksson AR, Albrektsson T (1983) Temperature threshold levels for heat-induced bone tissue injury: a vital-microscopic study in the rabbit. J Prosthet Dent 50(1):101–107
Eriksson AR, Albrektsson T, Magnusson B (1984) Assessment of bone viability after heat trauma. A histological, histochemical and vital microscopic study in the rabbit. Scand J Plast Reconstr Surg 18(3):261–268
Geminiani A, Caton JG, Romanos GE (2012) Temperature change during non-contact diode laser irradiation of implant surfaces. Lasers Med Sci 27:339–342
Leja C, Geminiani A, Caton J, Romanos GE (2013) Thermodynamic effects of laser irradiation of implants placed in bone: an in vitro study. Lasers Med Sci 28(6):1435–40
Mitsunaga S, Iwai T, Kitagima H, Yajima Y, Ohya T, Hitota M, Mitsudo K, Aoki N, Yamashita Y, Omura S, Tohnai I (2013) Cervicofacial subcutaneous emphysema associated with dental laser treatment. Aust Dent J 58:424–427
Mitsunaga S, Iwai T, Yamashita Y, Aoki N, Omura S, Matsui Y, Maegawa J, Hirota J, Mitsudo K, Tohnai I (2013) Cervicofacial subcutaneous and mediastinal emphysema caused by air cooling spray of dental laser. Oral Surg Oral Med Oral Pathol Oral Radiol 115:13–16
Hata T, Hosoda M (2001) Cervicofacial subcutaneous emphysema after oral laser treatment. Br J Oral Maxillofac Surg C 39:161–162
Imai T, Michizawa M, Arimoto E, Kimoto M, Yura Y (2009) Cervico-facial subcutaneous emphysema and pneumomediastinum after intraoral laser irradiation. J Oral Maxillofac Surg 67:428–430
Suzuki J, Takahashi S (2012) Subcutaneous emphysema and pneumo-mediastinum due to carbon dioxide laser therapy. J Pediatr 161:167
Tosun E, Tasar F, Strauss R, Kwanc DG, Ungor C (2012) Comparative evaluation of antimicrobial effects of Er:YAG, diode, and CO2 lasers on titanium discs: an experimental study. Int J Oral Maxillofac 70(5):1064–1069
Gokhale S, Padhye A, Sumanth S (2010) Bactericidal effect of Nd:YAG laser in an in vitro tissue model—a light microscopic evaluation. J Oral Laser Appl 10:17–22
Weis LC (2004) Aferição dos Equipamentos de Laser de Baixa Potência e Cracterização dos Procedimentos Empregados na sua Utilização Clínica. Thesis. Universidade Metodista de Piracicaba, Piracicaba
Zezel DM (2005) Interação da Luz Laser. IPEN/FOUSP, São Paulo, pp 24–30
Rodrigues DCGA, Santos TT (2011) Manual de Práticas de Processos Bioquímicos. Universidade Estadual do Rio de Janeiro, Rio de Janeiro
De Paula CE (2010) Lasers em Odontologia. Guanabara Koogan, Rio de Janeiro, pp 1–17
Author information
Authors and Affiliations
Corresponding authors
Appendices
Appendices
Appendix 1
Appendix 2
Experimental setup for carrying out the temperature measurements as a function of laser power and laser application time. A The automated system measures the temperature as a function of time. B Multimeters (Keithley® 196). C Thera Laser Surgery®. D Implants installed in the pork rib in thermal bath
Rights and permissions
About this article
Cite this article
Rios, F.G., Viana, E.R., Ribeiro, G.M. et al. Temperature evaluation of dental implant surface irradiated with high-power diode laser. Lasers Med Sci 31, 1309–1316 (2016). https://doi.org/10.1007/s10103-016-1974-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-016-1974-z