Abstract
Purpose
Increasing evidence has suggested that metformin may play positive roles in a wide range of infectious diseases. This study aimed to investigate the clinical impact of metformin exposure during Staphylococcus aureus bacteremia (SAB) in patients with diabetes.
Methods
A 3-year observational cohort study of 452 patients (aged ≥ 16 years) with SAB was performed at a tertiary care hospital. Metformin exposure was defined as receiving metformin during SAB, regardless of metformin use before the onset of bacteremia.
Results
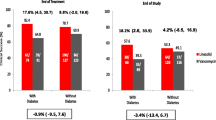
Of 452 patients, 51 (11.3%) were classified in Group A (diabetes with metformin exposure), 115 (25.4%) in Group B (diabetes without metformin exposure), and 286 (63.3%) in Group C (no diabetes). The 30-day mortality rate in Group A was significantly lower than that in Group B (3.9% [2/51] versus 14.8% [17/115]; p = 0.04) and lower than that in Group C (3.9% [2/51] versus 17.1% [49/286]; p = 0.02). The mortality rates did not differ between Group B and Group C (14.8% [17/115] versus 17.1% [49/286]; p = 0.57). The rates of persistent and recurrent bacteremia were comparable among the three groups. Multivariate analysis indicated that metformin exposure was significantly associated with reduced mortality (adjusted odds ratio, 0.20; 95% confidence interval, 0.04–0.88; p = 0.03).
Conclusions
Metformin exposure during SAB appears to be an independent predictor of survival in patients with diabetes.



Similar content being viewed by others
Data availability
The datasets generated during the current study are not publicly available as they contain health related data but limited datasets (without any identifiable, person-related data) are available from the corresponding author upon reasonable request.
References
Tong SYC, Davis JS, Eichenberger E, Holland TL, Fowler VG (2015) Staphylococcus aureus infections: epidemiology, pathophysiology, clinical manifestations, and management. Clin Microbiol Rev 28:603–661. https://doi.org/10.1128/CMR.00134-14
Smit J, Sogaard M, Schonheyder HC, Nielsen H, Froslev T, Thomsen RW (2016) Diabetes and risk of community-acquired Staphylococcus aureus bacteremia: a population-based case-control study. Eur J Endocrinol 174:631–639. https://doi.org/10.1530/EJE-16-0023
Hansen MU, Gotland N, Mejer N, Petersen A, Larsen AR, Benfield T, Danish Staphylococcal Bacteremia Study Group (2017) Diabetes increases the risk of disease and death due to Staphylococcus aureus bacteremia. A matched case-control and cohort study. Infect Dis (Lond) 49:689–697. https://doi.org/10.1080/23744235.2017.1331463
Kaasch AJ, Barlow G, Edgeworth JD, Fowler VG, Hellmich M, Hopkins S, Kern WV et al (2014) Staphylococcus aureus bloodstream infection: A pooled analysis of five prospective, observational studies. J Infect 68:242–251. https://doi.org/10.1016/j.jinf.2013.10.015
Malik F, Mehdi SF, Ali H, Patel P, Basharat A, Kumar A, Ashok F et al (2018) Is metformin poised for a second career as an antimicrobial? Diabetes Metab Res Rev 34:e2975. https://doi.org/10.1002/dmrr.2975
Liang H, Ding X, Li L, Wang T, Kan Q, Wang L, Sun T (2019) Association of preadmission metformin use and mortality in patients with sepsis and diabetes mellitus: a systematic review and meta-analysis of cohort studies. Crit Care 23:50. https://doi.org/10.1186/s13054-019-2346-4
Garnett JP, Baker EH, Naik S, Lindsay JA, Knight GM, Gill S, Tregoning JS et al (2013) Metformin reduces airway glucose permeability and hyperglycaemia-induced Staphylococcus aureus load independently of effects on blood glucose. Thorax 68:835–845. https://doi.org/10.1136/thoraxjnl-2012-203178
Friedman ND, Kaye KS, Stout JE, McGarry SA, Trivette SL, Briggs JP, Lamm W et al (2002) Health care-associated bloodstream infections in adults: a reason to change the accepted definition of community-acquired infections. Ann Intern Med 137:791–797. https://doi.org/10.7326/0003-4819-137-10-200211190-00007
Oliveira DC, de Lencastre H (2002) Multiplex PCR strategy for rapid identification of structural types and variants of the mec element in methicillin-resistant Staphylococcus aureus. Antimicrob Agents Chemother 46:2155–2161. https://doi.org/10.1128/AAC.46.7.2155-2161.2002
Enright MC, Day NP, Davies CE, Peacock SJ, Spratt BG (2000) Multilocus sequence typing for characterization of methicillin-resistant and methicillin-susceptible clones of Staphylococcus aureus. J Clin Microbiol 38:1008–1015. https://doi.org/10.1128/JCM.38.3.1008-1015.2000
Jarraud S, Mougel C, Thioulouse J, Lina G, Meugnier H, Forey F, Nesme X et al (2002) Relationships between Staphylococcus aureus genetic background, virulence factors, agr groups (alleles), and human disease. Infect Immun 70:631–641. https://doi.org/10.1128/IAI.70.2.631-641.2002
Rena G, Hardie DG, Pearson ER (2017) The mechanisms of action of metformin. Diabetologia 60:1577–1585. https://doi.org/10.1007/s00125-017-4342-z
Owen MR, Doran E, Halestrap AP (2000) Evidence that metformin exerts its anti-diabetic effects through inhibition of complex 1 of the mitochondrial respiratory chain. Biochem J 348:607–614. https://doi.org/10.1042/bj3480607
Madiraju AK, Erion DM, Rahimi Y, Zhang XM, Braddock DT, Albright RA, Prigaro BJ et al (2014) Metformin suppresses gluconeogenesis by inhibiting mitochondrial glycerophosphate dehydrogenase. Nature 510:542–546. https://doi.org/10.1038/nature13270
Wu H, Esteve E, Tremaroli V, Khan MT, Caesar R, Manneras-Holm L, Stahlman M et al (2017) Metformin alters the gut microbiome of individuals with treatment-naive type 2 diabetes, contributing to the therapeutic effects of the drug. Nat Med 23:850–858. https://doi.org/10.1038/nm.4345
Schuiveling M, Vazirpanah N, Radstake TRDJ, Zimmermann M, Broen JCA (2018) Metformin, a new era for an old drug in the treatment of immune mediated disease? Curr Drug Targets 19:945–959. https://doi.org/10.2174/1389450118666170613081730
Lv Z, Guo Y (2020) Metformin and its benefits for various diseases. Front Endocrinol (Lausanne) 11:191. https://doi.org/10.3389/fendo.2020.00191
Patkee WRA, Carr G, Baker EH, Baines DL, Garnett JP (2016) Metformin prevents the effects of Pseudomonas aeruginosa on airway epithelial tight junctions and restricts hyperglycaemia-induced bacterial growth. J Cell Mol Med 20:758–764. https://doi.org/10.1111/jcmm.12784
Inzucchi SE, Lipska KJ, Mayo H, Bailey CJ, McGuire DK (2014) Metformin in patients with type 2 diabetes and kidney disease: a systematic review. JAMA 312:2668–2675. https://doi.org/10.1001/jama.2014.15298
Magliano DJ, Harding JL, Cohen K, Huxley RR, Davis WA, Shaw JE (2015) Excess risk of dying from infectious causes in those with type 1 and type 2 diabetes. Diabetes Care 38:1274–1280. https://doi.org/10.2337/dc14-2820
Zoppini G, Fedeli U, Schievano E, Dauriz M, Targher G, Bonora E, Corti MC (2018) Mortality from infectious diseases in diabetes. Nutr Metab Cardiovasc Dis 28:444–450. https://doi.org/10.1016/j.numecd.2017.12.007
Funding
This research was supported by a grant of the Korea Health Technology R&D Project through the Korea Health Industry Development Institute (KHIDI), funded by the Ministry of Health & Welfare, Republic of Korea (grant number: HV22C1234). The funders had no role in study design, data collection and interpretation, or the decision to submit the work for publication.
Author information
Authors and Affiliations
Contributions
This study was conceived and designed by JYL and YSK. JYL, ESK, EC, SB, and JJ acquired the data. YJL, MJK, and YPC analysed and interpreted the data. The study was supervised by SHK, SHC, SOL, and YSK. YJL drafted the article, which was critically revised by SHK, SHC, SOL, and YSK.
Corresponding author
Ethics declarations
Ethical approval
The study was approved by the Asan Medical Center Institutional Review Board.
Consent to participate
Not applicable.
Consent to publish
All authors gave their consent for publication.
Competing interests
There are no potential conflicts of interest for any authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lee, J.Y., Kim, E.S., Chang, E. et al. Clinical impact of metformin exposure during Staphylococcus aureus bacteremia in patients with diabetes mellitus. Eur J Clin Microbiol Infect Dis 42, 1439–1447 (2023). https://doi.org/10.1007/s10096-023-04679-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-023-04679-6