Abstract
Background
Ceftaroline is a fifth-generation cephalosporin and represents an alternative in the treatment of infective endocarditis (IE). The main objective of this study was to describe the incidence of in-hospital and 42-day mortality in patients with IE treated with ceftaroline.
Methods
An observational retrospective study included adult patients with IE admitted during a 3.5-year period (January 2018–June 2021) and treated with ceftaroline in a single center. All cases were definite or possible IE according to the modified Duke criteria.
Results
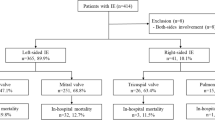
Seventy cases were analyzed. The mean age was 67.35 ± 16.62 (16–89) and 39 (55.7%) were males. The mean number of days of treatment with ceftaroline was 21.26 ± 16.17 (1–75). Overall mortality at 42 days was 30%, 20.7% in the first line, and 36.6% in rescue therapy. Predictors of 42 days-mortality were increased Charlson comorbidity index (CCI) (OR of 1.7 per 1 point increment, 95% CI 1.2–2.4, P 0.001), presence of methicillin-resistance (OR 6.8, 95% CI 1.3–36.8, P 0.026) and evidence of septic shock (OR 8.6 95% CI 1.7–44.2, P 0.01). Predictors of 42 days of therapeutic failure were the increase in the CCI (OR of 1.6 per 1 point increment, 95% CI 1.3–2.1, P 0.000) and septic shock (OR 4.5 95% CI 1.1–18 P 0.036). Adverse effects were described in 6/70 (8.6%) of the patients, precipitating in 4/70 (5.7%) the definitive withdrawal of the antibiotic.
Conclusions
The incidence of in-hospital and 42 day-mortality of IE patients treated with ceftaroline remains similar to literature data. Increased CCI, septic shock, and methicillin resistance are associated with poor prognosis.
Similar content being viewed by others
References
Murdoch DR, Corey GR, Hoen B, Miro JM, Fowler VG Jr, Bayer AS et al (2009) Clinical presentation, etiology, and outcome of infective endocarditis in the 21st century: the international collaboration on endocarditis prospective cohort study. Arch Intern Med 169:463–473. https://doi.org/10.1001/archinternmed.2008.603
Hoen B, Duval X (2013) Clinical practice. Infective endocarditis. N Engl J Med 368:1425–1433. https://doi.org/10.1056/NEJMcp1206782
Castillo JC, Anguita MP, Ramirez A, Siles JR, Torres F, Mesa D et al (2000) Long term outcome of infective endocarditis in patients who were not drug addicts: a 10 year study. Heart 83:525–530. https://doi.org/10.1136/heart.83.5.525
Slipczuk L, Codolosa JN, Davila CD, Romero-Corral A, Yun J, Pressman GS, Figueredo VM (2013) Infective endocarditis epidemiology over five decades: a systematic review. PLoS ONE 8(12):e82665. https://doi.org/10.1371/journal.pone.0082665
Zinforo® (ceftaroline fosamil). Full prescribing information. EMEA. Accessed October 25, 2021.Available at: https://ec.europa.eu/health/documents/communityregister/2014/20141030130093/anx_130093_es.pdf
Ho TT, Cadena J, Childs LM, Gonzalez-Velez M, Lewis JS 2nd (2012) Methicillin-resistant Staphylococcus aureus bacteraemia and endocarditis treated with ceftaroline salvage therapy. J Antimicrob Chemother 67:1267–1270. https://doi.org/10.1093/jac/dks006
Casapao AM, Davis SL, Barr VO, Klinker KP, Goff DA, Barber KE et al (2014) Large retrospective evaluation of the effectiveness and safety of ceftaroline fosamil therapy. Antimicrob Agents Chemother 58:2541–2546. https://doi.org/10.1128/AAC.02371-13
Ahmad O, Crawford TN, Myint T (2020) Comparing the outcomes of ceftaroline plus vancomycin or daptomycin combination therapy versus monotherapy in adults with complicated and prolonged methicillin-resistant Staphylococcus aureus bacteremia initially treated with supplemental ceftaroline. Infect Dis Ther 9:77–87. https://doi.org/10.1007/s40121-019-00277-2
Destache CJ, Guervil DJ, Kaye KS (2019) Ceftaroline fosamil for the treatment of Gram-positive endocarditis: CAPTURE study experience. Int J Antimicrob Agents 53:644–649. https://doi.org/10.1016/j.ijantimicag.2019.01.014
Li JS, Sexton DJ, Mick N, Nettles R, Fowler VG Jr, Ryan T et al (2000) Proposed modifications to the Duke criteria for the diagnosis of infective endocarditis. Clin Infect Dis 30:633–638. https://doi.org/10.1086/313753
Charlson ME, Pompei P, Ales KL, Mackenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chron Dis 40:373–383. https://doi.org/10.1016/0021-9681(87)90171-8
Singer M, Deutschman CS, Seymour CW, Shankar-Hari M, Annane D, Bauer M et al (2016) The third international consensus definitions for sepsis and septic shock (Sepsis-3). JAMA 315:801–810. https://doi.org/10.1001/jama.2016.0287
Chu VH, Cabell CH, Benjamin DK Jr, Kuniholm EF, Fowler VG Jr, Engemann J, Sexton DJ, Corey GR et al (2004) Early predictors of in-hospital death in infective endocarditis. Circulation 109(14):1745–1749. https://doi.org/10.1161/01.CIR.0000124719.61827.7F
Hill EE, Herijgers P, Claus P, Vanderschueren S, Herregods MC, Peetermans WE (2007) Infective endocarditis: changing epidemiology and predictors of 6-month mortality: a prospective cohort study. Eur Heart J 28(2):196–203. https://doi.org/10.1093/eurheartj/ehl427
Habib G, Erba PA, Iung B, Donal E, Cosyns B, Laroche C, Popescu BA, et al. Clinical presentation, aetiology and outcome of infective endocarditis. Results of the ESC-EORP EURO-ENDO (European infective endocarditis) registry: a prospective cohort study. Eur Heart J 2019;40:3222–3232. https://doi.org/10.1093/eurheartj/ehz620
Park LP, Chu VH, Peterson G, Skoutelis A, Lejko-Zupa T, Bouza E et al (2016) Validated risk score for predicting 6-month mortality in infective endocarditis. J Am Heart Assoc 5(4):e003016. https://doi.org/10.1161/JAHA.115.003016
Armiñanzas C, Fariñas-Alvarez C, Zarauza J, Muñoz P, González Ramallo V, Martínez Sellés M et al (2019) Role of age and comorbidities in mortality of patients with infective endocarditis. Eur J Intern Med 64:63–71. https://doi.org/10.1016/j.ejim.2019.03.006
Cresti A, Chiavarelli M, Scalese M, Nencioni C, Valentini S, Guerrini F, D’Aiello I, Picchi A et al (2017) Epidemiological and mortality trends in infective endocarditis, a 17-year population-based prospective study. Cardiovasc Diagn Ther 7:27–35. https://doi.org/10.21037/cdt.2016.08.09
Wang A, Gaca JG, Chu VH (2018) Management considerations in infective endocarditis: a review. JAMA 320(1):72–83. https://doi.org/10.1001/jama.2018.7596
Pericàs JM, Hernández-Meneses M, Muñoz P, Álvarez-Uría A, Pinilla-Llorente B, de Alarcón A et al (2021) Outcomes and risk factors of septic shock in patients with infective endocarditis: a prospective cohort study. Open Forum Infect Dis 8(6):ofab119. https://doi.org/10.1093/ofid/ofab119
Krajinovic V, Ivancic S, Gezman P, Barsic B (2018) Association between cardiac surgery and mortality among patients with infective endocarditis complicated by sepsis and septic shock. Shock 49(5):536–542. https://doi.org/10.1097/SHK.0000000000001013
Cahill TJ, Baddour LM, Habib G, Hoen B, Salaun E, Pettersson GB, Schäfers HJ, Prendergast BD (2017) Challenges in Infective Endocarditis. J Am Coll Cardiol 69:325–344. https://doi.org/10.1016/j.jacc.2016.10.066
Chu VH, Miro JM, Hoen B, Cabell CH, Pappas PA, Jones P, Stryjewski ME, Anguera I, Braun S, Muñoz P, Commerford P et al (2009) Coagulase-negative Staphylococcal prosthetic valve endocarditis—a contemporary update based on the international collaboration on endocarditis. Heart 95:570–576. https://doi.org/10.1136/hrt.2008.152975
Carugati M, Petti CA, Arnold C, Miro JM, Pericàs JM, Garcia de la Maria C, Kanafani Z, et al. Antistaphylococcal β-Lactams versus vancomycin for treatment of infective endocarditis due to methicillin-susceptible coagulase-negative Staphylococci: a prospective cohort study from the international collaboration on endocarditis. Antimicrob Agents Chemother 2016;60:6341–6349. https://doi.org/10.1128/AAC.01531-16
Joo EJ, Park DA, Kang CI, Chung DR, Song JH, Lee SM et al (2019) Reevaluation of the impact of methicillin-resistance on outcomes in patients with Staphylococcus aureus bacteremia and endocarditis. Korean J Intern Med 34:1347–1362. https://doi.org/10.3904/kjim.2017.098
Rodríguez-García R, Rodríguez-Esteban MÁ, García-Carús E, Telenti M, Fernández J (2020) In vitro activity of ceftaroline and ceftobiprole against clinical isolates of Gram-positive bacteria from infective endocarditis: are these drugs potential options for the initial management of this disease? Diagn Microbiol Infect Dis 98:115153. https://doi.org/10.1016/j.diagmicrobio.2020.115153
Sader HS, Flamm RK, Streit JM, Farrell DJ, Jones RN (2015) Ceftaroline activity against bacterial pathogens frequently isolated in U.S. medical centers: results from five years of the AWARE surveillance program. Antimicrob Agents Chemother 59:2458–61. https://doi.org/10.1128/AAC.04614-14
File TM Jr, Low DE, Eckburg PB, Talbot GH, Friedland HD, Lee J et al (2011) FOCUS 1: a randomized, double-blinded, multicentre, phase III trial of the efficacy and safety of ceftaroline fosamil versus ceftriaxone in community-acquired pneumonia. J Antimicrob Chemother 66(19–32):iii. https://doi.org/10.1093/jac/dkr096
Low DE, File TM Jr, Eckburg PB, Talbot GH, David Friedland H, Lee J et al (2011) FO- CUS 2: a randomized, double-blinded, multicentre, phase III trial of the efficacy and safety of ceftaroline fosamil versus ceftriaxone in community-acquired pneumonia. J Antimicrob Chemother 66(33–44):iii. https://doi.org/10.1093/jac/dkr097
Author information
Authors and Affiliations
Contributions
Study concept and design: BND. Acquisition, analysis, and interpretation of date: GUJM, BND, and FOC. Drafting of the manuscript: BND, ML, GUJM, FOC, and MHI. Critical revision of the manuscript: GUJM, ML, and MHI. Statistical analysis: SJ.
Corresponding author
Ethics declarations
Ethics approval
The study was evaluated and approved by the Ethics Committee for Medicines of Galicia (CEIm-G) with registration code 2021/268.
Consent to participate
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Brandariz-Núñez, D., Suanzes, J., Gutiérrez-Urbón, J.M. et al. Incidence and risk factors for mortality in patients treated with combined ceftaroline for Gram-positive infective endocarditis. Eur J Clin Microbiol Infect Dis 41, 827–834 (2022). https://doi.org/10.1007/s10096-022-04443-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-022-04443-2