Abstract
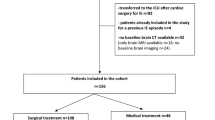
The optimal timing of cardiac surgery remains unclear for patients with neurological complications of infective endocarditis (IE). However, neuroimaging findings may allow more refined clinical decision-making. We analyzed clinical and advanced neuroimaging data for 135 patients with IE who had preoperatively diagnosed ischemic cerebral complications (86 patients) or hemorrhagic complications (49 patients), between January 1997 and May 2013. The effect of early surgery (within 3 and 7 days of ischemic and hemorrhagic complications respectively) on in-hospital mortality and 1-year adverse outcomes (mortality, relapse, or new embolic events) was estimated. Small cerebral emboli (≤2 cm) led to early surgery (cases with ischemic complications: 57% vs 26%, p = 0.04; cases with hemorrhagic complications: 56% vs 13%, p = 0.02). Early surgery was not significantly associated with increased rates of in-hospital mortality and 1-year adverse outcomes among patients with ischemic complications (14% vs 9%, odds ratio [OR] 1.67, 95% confidence interval [CI] 0.44–6.38, p = 0.52; 17% vs 14%, OR 1.27, 95% CI 0.39–4.14, p = 0.7 respectively). Only 1 patient (4%) with hemorrhagic complications experienced in-hospital mortality in the early surgery group, and early surgery was not significantly associated with 1-year adverse outcomes (21% vs 12%, OR 1.93, 95% CI 0.41–9.16, p = 0.46). The risks of in-hospital mortality and 1-year adverse outcome were not increased, even if cardiac surgery had been carried out earlier than previously described. Our findings suggest that early surgery, when indicated, may be performed for patients with IE and neurological complications, especially if the cerebral embolus has a diameter of ≤2 cm.


Similar content being viewed by others
References
Thuny F, Beurtheret S, Mancini J et al (2011) The timing of surgery influences mortality and morbidity in adults with severe complicated infective endocarditis: a propensity analysis. Eur Heart J 32:2027–2033
Chu VH, Park LP, Athan E et al (2015) Association between surgical indications, operative risk, and clinical outcome in infective endocarditis: a prospective study from the international collaboration on Endocarditis. Circulation 131:131–140
Iung B, Doco-Lecompte T, Chocron S et al (2016) Cardiac surgery during the acute phase of infective endocarditis: discrepancies between European Society of Cardiology guidelines and practices. Eur Heart J 37:840–848
Hoen B, Duval X (2013) Infective endocarditis. N Engl J Med 368:785
Kang DH, Kim YJ, Kim SH et al (2012) Early surgery versus conventional treatment for infective endocarditis. N Engl J Med 366:2466–2473
Kim DH, Kang DH, Lee MZ et al (2010) Impact of early surgery on embolic events in patients with infective endocarditis. Circulation 122:S17–S22
Thuny F, Grisoli D, Collart F et al (2012) Management of infective endocarditis: challenges and perspectives. Lancet 379:965–975
Baddour LM, Wilson WR, Bayer AS et al (2015) Infective endocarditis in adults: diagnosis, antimicrobial therapy, and management of complications. A scientific statement for healthcare professionals from the American Heart Association. Circulation 131:1435–1486
Habib G, Lancellotti P, Antunes MJ et al (2015) 2015 ESC guidelines for the management of infective endocarditis. Eur Heart J 36:3075–3128
Byrne JG, Rezai K, Sanchez JA et al (2011) Surgical management of endocarditis: the Society of Thoracic Surgeons clinical practice guideline. Ann Thorac Surg 91:2012–2019
Yoshioka D, Sakaguchi T, Yamauchi T et al (2012) Impact of early surgical treatment on postoperative neurologic outcome for active infective endocarditis complicated by cerebral infarction. Ann Thorac Surg 94:489–495
Sorabella RA, Han SM, Grbic M et al (2015) Early operation for endocarditis complicated by preoperative cerebral emboli is not associated with worsened outcomes. Ann Thorac Surg 100:501–508
Ruttmann E, Willeit J, Ulmer H et al (2006) Neurological outcome of septic cardioembolic stroke after infective endocarditis. Stroke 37:2094–2099
Barsic B, Dickerman S, Krajinovic V et al (2013) Influence of the timing of cardiac surgery on the outcome of patients with infective endocarditis and stroke. Clin Infect Dis 56:209–217
Kang DH (2015) Timing of surgery in infective endocarditis. Heart 101:1786–1791
Bennet JE, Dolin R, Blaser MJ (2014) Mandell, Douglas, and Bennett’s principles and practice of infectious diseases, 8th edn. Saunders, Elsevier, New York, p 1019
García-Cabrera E, Fernández-Hidalgo N, Almirante B et al (2013) Neurological complications of infective endocarditis: risk factors, outcome, and impact of cardiac surgery: a multicenter observational study. Circulation 127:2272–2284
Angstwurm K, Borges AC, Halle E et al (2004) Timing the valve replacement in infective endocarditis involving the brain. J Neurol 251:1220–1226
Thuny F, Avierinos JF, Tribouilloy C et al (2007) Impact of cerebrovascular complications on mortality and neurologic outcome during infective endocarditis: a prospective multicenter study. Eur Heart J 28:1155–1161
Snygg-Martin U, Gustafsson L, Rosengren L et al (2008) Cerebrovascular complications in patients with left-sided infective endocarditis are common: a prospective study using magnetic resonance imaging and neurochemical brain damage markers. Clin Infect Dis 47:23–30
Wilbring M, Irmscher L, Alexiou K et al (2014) The impact of preoperative neurological events in patients suffering from native infective endocarditis. Interact Cardiovasc Thorac Surg 18:740–747
Yoshioka D, Toda K, Sakaguchi T et al (2014) Valve surgery in active endocarditis patients complicated by intracranial hemorrhage: the influence of the timing of surgery on neurological outcomes. Eur J Cardiothorac Surg 45:1082–1088
Cahill TJ, Baddour LM, Habib G et al (2017) Challenges in infective endocarditis. J Am Coll Cardiol 69:325–344
Li JS, Sexton DJ, Mick N et al (2000) Proposed modifications to the Duke criteria for the diagnosis of infective endocarditis. Clin Infect Dis 30:633–638
Charlson ME, Pompei P, Ales KL et al (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Gaca JG, Sheng S, Daneshmand MA et al (2011) Outcomes for endocarditis surgery in North America: a simplified risk scoring system. J Thorac Cardiovasc Surg 141:98–106
Ben-Ami R, Giladi M, Carmeli Y et al (2004) Hospital-acquired infective endocarditis. Should the definition be broadened? Clin Infect Dis 38:843–850
Tatu L, Moulin T, Bogousslavsky J et al (1996) Arterial territories of the human brain: brainstem and cerebellum. Neurology 47:1125–1135
Tatu L, Moulin T, Bogousslavsky J et al (1998) Arterial territories of the human brain: cerebral hemisphere. Neurology 50:1699–1708
Wong KS, Gao S, Chan YL et al (2002) Mechanisms of acute cerebral infarctions in patients with middle cerebral artery stenosis: a diffusion-weighted imaging and microemboli monitoring study. Ann Neurol 52:74–81
Prendergast BD, Tornos P (2010) Surgery for infective endocarditis: who and when? Circulation 121:1141–1152
San Román JA, Vilacosta I, López J et al (2015) Critical questions about left-sided infective endocarditis. J Am Coll Cardiol 66:1068–1076
Derex L, Bonnefoy E, Delahaye F (2010) Impact of stroke on therapeutic decision making in infective endocarditis. J Neurol 257:315–321
Piper C, Wiemer M, Schulte HD et al (2001) Stroke is not a contraindication for urgent valve replacement in acute infective endocarditis. J Heart Valve Dis 10:703–711
Okita Y, Minakata K, Yasuno S et al (2016) Optimal timing of surgery for active infective endocarditis with cerebral complications: a Japanese multicenter study. Eur J Cardiothorac Surg 50:374–382
Lee SJ, SS O, Lim DS et al (2014) Clinical significance of cerebrovascular complications in patients with acute infective endocarditis: a retrospective analysis of a 12-year single-center experience. BMC Neurol 14:30
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None of the authors has any potential conflicts of interest.
Ethical approval
The study was approved by the Asan Medical Center Institutional Review Board (IRB).
Informed consent
Informed consent was not required because of the retrospective nature of the present study.
Rights and permissions
About this article
Cite this article
Kim, Y.K., Choi, C.G., Jung, J. et al. Effect of cerebral embolus size on the timing of cardiac surgery for infective endocarditis in patients with neurological complications. Eur J Clin Microbiol Infect Dis 37, 545–553 (2018). https://doi.org/10.1007/s10096-017-3148-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-017-3148-8