Abstract
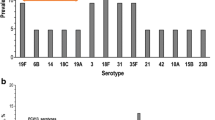
A prospective clinical study was performed to correlate nasopharyngeal carriage of bacteria with the type of lower respiratory tract infections (LRTI) in hospitalised children. To determine bacterial load in nasopharyngeal aspirates (NPA) we used semiquantitative culturing and quantitative TaqMan-PCR for those pathogens difficult to culture. Specimens and clinical data were obtained from 311 children between 0 and 16 years of age with LRTI during the period of 2006–2008. The most common detected potentially pathogenic colonisers were Haemophilus influenzae (32.1 %), Moraxella catharralis (26.7 %), Staphylococcus aureus (17.7 %) and Streptococcus pneumoniae (16.7 %). As expected S. aureus was the most common coloniser in children less than 4 months of age, whereas H. influenzae detection peaked in older children. Co-colonisation with other bacterial pathogens were more often observed in children with S. aureus (46 %) and S. pneumoniae (49 %) than in those with H. influenzae (30 %) or M. catharralis (27 %). Children with S. aureus co-colonisation had higher levels of C-reactive-protein, received antibiotics more frequently and stayed longer in hospital than those with S. aureus single colonisation. In contrast, children with H. influenzae, M. catharralis or S. pneumoniae colonisation suffered more often from pneumonia than children with S. aureus colonisation. Coloniser specific analysis of bacterial quantity revealed no significant reduction of the bacterial carriage from the first to the second NPA. No correlation of a high bacterial load and occurrence of pneumonia could be detected. In conclusion, clinical characteristics in children with LRTIs are associated with a specific bacterial set of colonisers detected in the nasopharynx rather than on their quantity.

Similar content being viewed by others
References
Franz A, Adams O, Willems R, Bonzel L, Neuhausen N, Schweizer-Krantz S, Ruggeberg JU, Willers R, Henrich B, Schroten H, Tenenbaum T (2010) Correlation of viral load of respiratory pathogens and co-infections with disease severity in children hospitalized for lower respiratory tract infection. J Clin Virol 48(4):239–245
Bezerra PG, Britto MC, Correia JB, Duarte Mdo C, Fonceca AM, Rose K, Hopkins MJ, Cuevas LE, McNamara PS (2011) Viral and atypical bacterial detection in acute respiratory infection in children under five years. PLoS One 6(4):e18928
Juven T, Mertsola J, Waris M, Leinonen M, Meurman O, Roivainen M, Eskola J, Saikku P, Ruuskanen O (2000) Etiology of community-acquired pneumonia in 254 hospitalized children. Pediatr Infect Dis J 19(4):293–298
Weigl JA, Puppe W, Belke O, Neususs J, Bagci F, Schmitt HJ (2005) The descriptive epidemiology of severe lower respiratory tract infections in children in Kiel, Germany. Klin Padiatr 217(5):259–267
Nohynek H, Eskola J, Kleemola M, Jalonen E, Saikku P, Leinonen M (1995) Bacterial antibody assays in the diagnosis of acute lower respiratory tract infection in children. Pediatr Infect Dis J 14(6):478–484
Vu HT, Yoshida LM, Suzuki M, Nguyen HA, Nguyen CD, Nguyen AT, Oishi K, Yamamoto T, Watanabe K, Vu TD (2011) Association between nasopharyngeal load of Streptococcus pneumoniae, viral coinfection, and radiologically confirmed pneumonia in Vietnamese children. Pediatr Infect Dis J 30(1):11–18
Morris A, Wei K, Afshar K, Huang L (2008) Epidemiology and clinical significance of pneumocystis colonization. J Infect Dis 197(1):10–17
Waites KB, Schelonka RL, Xiao L, Grigsby PL, Novy MJ (2009) Congenital and opportunistic infections: Ureaplasma species and Mycoplasma hominis. Semin Fetal Neonatal Med 14(4):190–199
Hardegger D, Nadal D, Bossart W, Altwegg M, Dutly F (2000) Rapid detection of Mycoplasma pneumoniae in clinical samples by real-time PCR. J Microbiol Methods 41(1):45–51
Bonzel L, Tenenbaum T, Schroten H, Schildgen O, Schweitzer-Krantz S, Adams O (2008) Frequent detection of viral coinfection in children hospitalized with acute respiratory tract infection using a real-time polymerase chain reaction. Pediatr Infect Dis J 27(7):589–594
Schaeffer A, Henrich B (2008) Rapid detection of Chlamydia trachomatis and typing of the Lymphogranuloma venereum associated L-Serovars by TaqMan PCR. BMC Infect Dis 8:56
Antonishyn NA, McDonald RR, Chan EL, Horsman GB (2005) High-throughput qualitative multiplex 5' nuclease assay using post-only PCR analysis. Mol Cell Probes 19(5):329–333
Brenneisen W (2008) Diagnostik urogenital relevanter Krankheitskeime: Entwicklung einer TaqMan Real Time PCR. VDM Verlag Dr. Müller
Tenenbaum T, Heusch A, Henrich B, MacKenzie CR, Schmidt KG, Schroten H (2005) Acute hemorrhagic pericarditis in a child with pneumonia due to Chlamydophila pneumoniae. J Clin Microbiol 43(1):520–522
Feigin RD, Cherry CJ (2009) Textbook of pediatric infectious diseases. W.B. Saunders Company, Philadelphia
Global Initiative for Asthma (GINA) (2011) Global strategy for asthma management and prevention 2011. http://www.ginasthma.org. Accessed 24 June 2012
Organization WH Pneumonia Vaccine Trial Investigators' Group (2001) Standardization of interpretation of chest radiographs for the diagnosis of pneumonia in children. http://www.who.int/vaccines-documents/DocsPDF01/www616.pdf. Accessed 24 June 2012
Garcia-Rodriguez JA, Fresnadillo Martinez MJ (2002) Dynamics of nasopharyngeal colonization by potential respiratory pathogens. J Antimicrob Chemother 50(Suppl S2):59–73
Ruckinger S, van der Linden M, Reinert RR, von Kries R, Burckhardt F, Siedler A (2009) Reduction in the incidence of invasive pneumococcal disease after general vaccination with 7-valent pneumococcal conjugate vaccine in Germany. Vaccine 27(31):4136–4141
Konno M, Baba S, Mikawa H, Hara K, Matsumoto F, Kaga K, Nishimura T, Kobayashi T, Furuya N, Moriyama H, Okamoto Y, Furukawa M, Yamanaka N, Matsushima T, Yoshizawa Y, Kohno S, Kobayashi K, Morikawa A, Koizumi S, Sunakawa K, Inoue M, Ubukata K (2006) Study of upper respiratory tract bacterial flora: first report. Variations in upper respiratory tract bacterial flora in patients with acute upper respiratory tract infection and healthy subjects and variations by subject age. J Infect Chemother 12(2):83–96
Zhang Q, Finn A (2004) Mucosal immunology of vaccines against pathogenic nasopharyngeal bacteria. J Clin Pathol 57(10):1015–1021
Abdullahi O, Nyiro J, Lewa P, Slack M, Scott JA (2008) The descriptive epidemiology of Streptococcus pneumoniae and Haemophilus influenzae nasopharyngeal carriage in children and adults in Kilifi district, Kenya. Pediatr Infect Dis J 27(1):59–64
Ercibengoa M, Arostegi N, Marimon JM, Alonso M, Perez-Trallero E (2012) Dynamics of pneumococcal nasopharyngeal carriage in healthy children attending a day care center in northern Spain. Influence of detection techniques on the results. BMC Infect Dis 12(1):69
Prevaes SM, van Wamel WJ, de Vogel CP, Veenhoven RH, van Gils EJ, van Belkum A, Sanders EA, Bogaert D (2012) Nasopharyngeal colonization elicits antibody responses to staphylococcal and pneumococcal proteins that are not associated with a reduced risk of subsequent carriage. Infect Immun 80(6):2186–193
Lebon A, Moll HA, Tavakol M, van Wamel WJ, Jaddoe VW, Hofman A, Verbrugh HA, van Belkum A (2010) Correlation of bacterial colonization status between mother and child: the Generation R Study. J Clin Microbiol 48(3):960-962
Pettigrew MM, Gent JF, Revai K, Patel JA, Chonmaitree T (2008) Microbial interactions during upper respiratory tract infections. Emerg Infect Dis 14(10):1584–1591
Regev-Yochay G, Dagan R, Raz M, Carmeli Y, Shainberg B, Derazne E, Rahav G, Rubinstein E (2004) Association between carriage of Streptococcus pneumoniae and Staphylococcus aureus in Children. JAMA 292(6):716–720
Madhi SA, Adrian P, Kuwanda L, Cutland C, Albrich WC, Klugman KP (2007) Long-term effect of pneumococcal conjugate vaccine on nasopharyngeal colonization by Streptococcus pneumoniae–and associated interactions with Staphylococcus aureus and Haemophilus influenzae colonization–in HIV-Infected and HIV-uninfected children. J Infect Dis 196(11):1662–1666
Lee GM, Huang SS, Rifas-Shiman SL, Hinrichsen VL, Pelton SI, Kleinman K, Hanage WP, Lipsitch M, McAdam AJ, Finkelstein JA (2009) Epidemiology and risk factors for Staphylococcus aureus colonization in children in the post-PCV7 era. BMC Infect Dis 9:110
Jourdain S, Smeesters PR, Denis O, Dramaix M, Sputael V, Malaviolle X, Van Melderen L, Vergison A (2011) Differences in nasopharyngeal bacterial carriage in preschool children from different socio-economic origins. Clin Microbiol Infect 17(6):907–914
Cohen R, Levy C, Thollot F, de La Rocque F, Koskas M, Bonnet E, Fritzell B, Varon E (2007) Pneumococcal conjugate vaccine does not influence Staphylococcus aureus carriage in young children with acute otitis media. Clin Infect Dis 45(12):1583–1587
Binks MJ, Cheng AC, Smith-Vaughan H, Sloots T, Nissen M, Whiley D, McDonnell J, Leach AJ (2011) Viral-bacterial co-infection in Australian Indigenous children with acute otitis media. BMC Infect Dis 11:161
Nilsson AC, Bjorkman P, Welinder-Olsson C, Widell A, Persson K (2010) Clinical severity of Mycoplasma pneumoniae (MP) infection is associated with bacterial load in oropharyngeal secretions but not with MP genotype. BMC Infect Dis 10:39
Levine OS, Liu G, Garman RL, Dowell SF, Yu S, Yang YH (2000) Haemophilus influenzae type b and Streptococcus pneumoniae as causes of pneumonia among children in Beijing, China. Emerg Infect Dis 6(2):165–170
Revai K, Mamidi D, Chonmaitree T (2008) Association of nasopharyngeal bacterial colonization during upper respiratory tract infection and the development of acute otitis media. Clin Infect Dis 46(4):e34–e37
Esposito S, Blasi F, Arosio C, Fioravanti L, Fagetti L, Droghetti R, Tarsia P, Allegra L, Principi N (2000) Importance of acute Mycoplasma pneumoniae and Chlamydia pneumoniae infections in children with wheezing. Eur Respir J 16(6):1142–1146
Normann E, Gnarpe J, Wettergren B, Janson C, Wickman M, Nordvall L (2006) Association between Chlamydia pneumoniae antibodies and wheezing in young children and the influence of sex. Thorax 61(12):1054–1058
Nagayama Y, Tsubaki T, Nakayama S, Sawada K, Taguchi K, Toba T, Kohno Y (2007) Bacterial colonization in respiratory secretions from acute and recurrent wheezing infants and children. Pediatr Allergy Immunol 18(2):110–117
Jartti T, Kuneinen S, Lehtinen P, Peltola V, Vuorinen T, Leinonen M, Ruuskanen O (2011) Nasopharyngeal bacterial colonization during the first wheezing episode is associated with longer duration of hospitalization and higher risk of relapse in young children. Eur J Clin Microbiol Infect Dis 30(2):233–241
Bisgaard H, Hermansen MN, Bonnelykke K, Stokholm J, Baty F, Skytt NL, Aniscenko J, Kebadze T, Johnston SL (2010) Association of bacteria and viruses with wheezy episodes in young children: prospective birth cohort study. BMJ 341:c4978
Pientong C, Ekalaksananan T, Teeratakulpisarn J, Tanuwattanachai S, Kongyingyoes B, Limwattananon C (2010) Atypical bacterial pathogen infection in children with acute bronchiolitis in northeast Thailand. J Microbiol Immunol Infect 44(2):95–100
Aujard Y, Maury L, Doit C, Mariani-Kurkdjian P, Baud O, Farnoux C, Bingen E (2005) Ureaplasma urealyticum and Mycoplasma hominis infections in newborns: personal data and review of the literature. Arch Pediatr 12(Suppl 1):S12–S18
Acknowledgment
We would like to thank all participating physicians, nurses and technical staff for recruiting and treating the patients, obtaining the NPAs and performing the assays.
Competing interests
The authors declare that they have no conflict of interest.
Authors' contributions
TT, AF, NN, RW, BH participated in the design, data collection and analysis, and drafted the manuscript; HS SSK, OA, contributed to the interpretation of the data and editing of the manuscript and supervised the design and execution of the study; JB performed the statistical analysis. The final version of the manuscript was approved by all of the authors.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tenenbaum, T., Franz, A., Neuhausen, N. et al. Clinical characteristics of children with lower respiratory tract infections are dependent on the carriage of specific pathogens in the nasopharynx. Eur J Clin Microbiol Infect Dis 31, 3173–3182 (2012). https://doi.org/10.1007/s10096-012-1682-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-012-1682-y