Abstract
Background
The neurovascular conflict (NVC) causing hemifacial spasm (HFS) can also cause compression of ventrolateral medulla (VLM) which contains the central sympathetic neurons. VLM compression has been associated with hypertension. Whether the VLM compression in HFS patients is associated with hypertension is not clear.
Objective
To determine the frequency, severity of VLM compression and its association with hypertension in HFS patients.
Methods
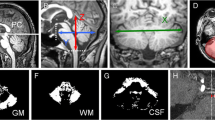
A cross-sectional, hospital-based, case control study and recruited 120 study subjects (50 cases of primary HFS, 30 hypertensive and 40 normotensive age-, sex- matched controls). The VLM compression was assessed in magnetic resonance imaging Constructive Interference in Steady State (CISS) 3D sequences.
Results
Hypertension was present in 30 cases (60%). Six patients with HFS (20%) were detected to be hypertensive after the onset of HFS. VLM compression was seen in 24 cases (48%), 7 hypertensive controls (23.3%) and 5 normotensive controls (10%) (p = 0.03). Twenty-four patients with hypertension had VLM compression and remaining 6 patients with hypertension did not have VLM compression (80% vs 20%; p = 0.02). Normotensive patients did not have VLM compression. Vertebral artery was the most common artery causing VLM compression (22 patients; 7 hypertensive and 5 normotensive controls).
Conclusion
VLM compression is more common in HFS patients as compared to hypertensive and normotensive controls. It is more common in hypertensive HFS patients in comparison with normotensive HFS patients. Microvascular decompression is an option in hypertensive HFS patients with VLM compression if the hypertension is medically refractory.

Similar content being viewed by others
Data availability
Data cannot be shared openly to protect study participant privacy.
References
Lefaucheur JP, Ben Daamer N, Sangla S, Le Guerinel C (2018) Diagnosis of primary hemifacial spasm. Neurochirurgie 64(2):82–86
Abbruzzese G, Berardelli A, Defazio G (2011) Hemifacial spasm. Handb Clin Neurol 100:675–680
Adler CA, Zimmerman RA, Savino PJ, Bernardi B, Bosley TM, Sergott RC (1992) Hemifacial spasm: evaluation by magnetic resonance imaging and magnetic resonance tomographic angiography. Ann Neurol 32:502–506
Leong JL, Li HH, Chan LL, Tan EK (2016) Revisiting the link between hypertension and hemifacial spasm. Sci Rep 19(6):21082
Sindou M, Mercier P (2018) Hemifacial spasm associated with other cranial nerve syndromes: literature review. Neurochirurgie 64(2):101–105
Sindou M, Mahmoudi M, Brînzeu A (2015) Hypertension of neurogenic origin: effect of microvascular decompression of the CN IX-X root entry/exit zone and ventrolateral medulla on blood pressure in a prospective series of 48 patients with hemifacial spasm associated with essential hypertension. J Neurosurg 123(6):1405–1413
Rudzińska M, Wójcik-Pędziwiatr M, Malec-Litwinowicz M, Grabska N, Hartel M, Flak M et al (2016) Is hypertension a risk factor of hemifacial spasm? Neurol Neurochir Pol 50(2):69–74
Jannetta PJ, Segal R, Wolfson SK Jr, Dujovny M, Semba A, Cook EE (1985) Neurogenic hypertension: etiology and surgical treatment. II. observations in an experimental nonhuman primate model. Ann Surg 202:253–261
Akimura T, Furutani Y, Jimi Y, Saito K, Kashiwagi S, Kato S, Ito H (1995) Essential hypertension and neurovascular compression at the ventrolateral medulla oblongata: MR evaluation. Am J Neuroradiol 16:401–405
Geiger H, Naraghi R, Schobel HP, Frank H, Sterzel RB, Fahlbusch R (1998) Decrease of blood pressure by ventrolateral medullary decompression in essential hypertension. Lancet 352(9126):446–449
Defazio G, Berardelli A, Abbruzzese G, Coviello V, De Salvia R, Federico F et al (2000) Primary hemifacial spasm and arterial hypertension: a multicenter case-control study. Neurology 54:1198–1200
Oliveira LD, Cardoso F, Vargas AP (1999) Hemifacial spasm and arterial hypertension. Mov Disord 14:832–835
Tan EK, Chan LL, Lum SY, Koh P, Han SY, Fook-Chong SM, Lo YL, Pavanni R, Wong MC, Lim SH (2003) Is hypertension associated with hemifacial spasm? Neurology 60(2):343–344
Colosimo C, Chianese M, Romano S, Vanacore N (2003) Is hypertension associated with hemifacial spasm? Neurology 61(4):587
Nakamura T, Osawa M, Uchiyama S, Iwata M (2007) Arterial hypertension in patients with left primary hemifacial spasm is associated with neurovascular compression of the left rostral ventrolateral medulla. Eur Neurol 57(3):150–155
Gajjar D, Egan B, Curè J, Rust P, VanTassel P, Patel SJ (2000) Vascular compression of the rostral ventrolateral medulla in sympathetic mediated essential hypertension. Hypertension 36(1):78–82
Levy EI, Scarrow AM, Jannetta PJ (2001) Microvascular decompression in the treatment of hypertension: review and update. Surg Neurol 55(1):2–10. https://doi.org/10.1016/s0090-3019(00)00352-9
Chan LL, Lee E, Fook-Chong S, Tan EK (2008) Case control MR-CISS and 3D TOF MRA imaging study of medullary compression and hypertension in hemifacial spasm. Mov Disord 23(13):1820–1824
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical compliance statement
Institute Ethics Committee approval was obtained (NO. NIMH/DO/IEC-BS& NS DIV/2021).
Competing interest
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Anudeep, D.D.S., Karthik, K., Holla, V.V. et al. Ventrolateral medullary compression by vascular contact in primary hemifacial spasm: a radiological analysis. Neurol Sci (2024). https://doi.org/10.1007/s10072-024-07602-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10072-024-07602-9