Abstract
Background
Very late-onset neuromyelitis optica spectrum disorder–related optic neuritis is limited to a few case reports.
Objective
To investigate the clinical features and visual prognosis of very late-onset neuromyelitis optica spectrum disorder–related optic neuritis.
Methods
This study evaluated 22 patients with first-onset optic neuritis and fulfilled the 2015 diagnosis criteria for neuromyelitis optica spectrum disorders.
Results
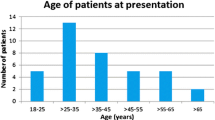
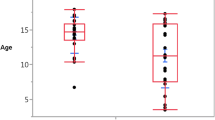
The mean age at optic neuritis onset was 73.91 ± 4.71 (range: 70–82) years with a female predominance (81.8%; ratio: 4.5:1). Antinuclear antibody seropositivity and seronegativity were identified in 12 (55.5%) and 10 (45.5%) patients, respectively. Severe visual loss persisted in 19 (19/42, 45.3%) eyes at the last follow-up. Although patients with antinuclear antibody seropositivity had a significantly higher frequency of attacks (P = 0.015), but they had a longer median time to reach severe visual loss (37 vs. 26 months; log-rank test, P = 0.023). Multivariate logistic regression analysis revealed antinuclear antibody seropositivity (hazard ratio = 4.849, 95% confidence interval: 1.309–17.965, P = 0.018) as a good predictor of visual acuity improvement.
Conclusion
Patients with very late-onset neuromyelitis optica spectrum disorder–related optic neuritis may develop severe optic neuritis, and those with antinuclear antibody seronegativity have a similar clinical presentation but worse outcome than those with seropositivity.

Similar content being viewed by others
References
Wingerchuk DM, Lennon VA, Lucchinetti CF et al (2007) The spectrum of neuromyelitis optica. Lancet Neurol 6:805–815
Sepulveda M, Delgado-García G, Blanco Y et al (2019) Late-onset neuromyelitis optica spectrum disorder: the importance of autoantibody serostatus. Neurol Neuroimmunol Neuroinflamm 6:e607
Nakahara K, Nakane S, Nagaishi A et al (2021) Very late onset neuromyelitis optica spectrum disorders. Eur J Neurol 28:2574–2581
Carnero Contentti E, Daccach Marques V, Soto de Castillo I et al (2020) Clinical features and prognosis of late-onset neuromyelitis optica spectrum disorders in a Latin American cohort. J Neurol 267:1260–1268
Lefaucheur R, Bourre B, Ahtoy P et al (2011) Neuromyelitis optica with very late onset. J Am Geriatr Soc 59:1138–1140
Fujiwara S, Manabe Y, Morihara R et al (2020) Two cases of very-late-onset neuromyelitis optica spectrum disorder (NMOSD) in patients over the age of 80. Case Rep Neurol 12:13–17
Krumbholz M, Hofstadt-van Oy U, Angstwurm K et al (2015) Very late-onset neuromyelitis optica spectrum disorder beyond the age of 75. J Neurol 262:1379–1384
Cai LJ, Zhang Q, Zhang Y et al (2020) Clinical characteristics of very late-onset neuromyelitis optica spectrum disorder. Mult Scler Relat Disord 46:102515
Thongmee W, Narongkhananukul C, Padungkiatsagul T et al (2021) Comparison of early- and late-onset NMOSD-related optic neuritis in Thai patients: clinical characteristics and long-term visual outcomes. Clin Ophthalmol 15:419–429
Lennon VA, Wingerchuk DM, Kryzer TJ et al (2004) A serum autoantibody marker of neuromyelitis optica: distinction from multiple sclerosis. Lancet 364:2106–2112
Sepúlveda M, Armangué T, Sola-Valls N et al (2016) Neuromyelitis ´optica spectrum disorders. Comparison according to the phenotype and serostatus. Neurol Neuroimmunol Neuroinflamm 3:e225
Ramos-Casals M, García-Carrasco M, Brito MP et al (2003) Autoimmunity and geriatrics: clinical significance of autoimmune manifestations in the elderly. Lupus 12:341–355
Wang R, Sun DR, Du Q et al (2023) Serum antinuclear antibodies associate with severe disease activity in neuromyelitis optica spectrum disorder. J Neuroimmunol 382:578151
Masuda H, Mori M, Uzawa A et al (2016) Serum antinuclear antibody may be associated with less severe disease activity in neuromyelitis optica. Eur J Neurol 23:276–281
Szmyrka-Kaczmarek M, Pokryszko-Dragan A, Pawlik B et al (2012) Antinuclear and antiphospholipid antibodies in patients with multiple sclerosis. Lupus 21:412–420
Wingerchuk DM, Banwell B, Bennett JL et al (2015) International consensus diagnostic criteria for neuromyelitis optica spectrum disorders. Neurology 85:177–189
Petzold A, Fraser CL, Abegg M et al (2022) Diagnosis and classification of optic neuritis. Lancet Neurol 27(21):00200–00209
Wingerchuk DM, Hogancamp WF, O’Brien PC et al (1999) The clinical course of neuromyelitis optica (Devic’s syndrome). Neurology 53:1107–1114
Yu J, Yan S, Niu P et al (2022) Relatively early and late-onset neuromyelitis optica spectrum disorder in central China: clinical characteristics and prognostic features. Front Neurol 13:859276
Seok JM, Cho HJ, Ahn SW et al (2017) Clinical characteristics of late-onset neuromyelitis optica spectrum disorder: a multicenter retrospective study in Korea. Mult Scler 23:1748–1756
Kim SH, Mealy MA, Levy M et al (2018) Racial differences in neuromyelitis optica spectrum disorder. Neurology 91:e2089–e2099
Yang Q, Sun L, Wang Q et al (2019) Primary optic neuropathy in Behçet’s syndrome. Mult Scler 25:1132–1140
Mealy MA, Mossburg SE, Kim SH et al (2019) Long-term disability in neuromyelitis optica spectrum disorder with a history of myelitis is associated with age at onset, delay in diagnosis/preventive treatment, MRI lesion length and presence of symptomatic brain lesions. Mult Scler Relat Disord 28:64–68
Margoni M, Carotenuto A (2019) Very late-onset recurrent myelitis in a patient diagnosed with antiphospholipid syndrome: a puzzle of autoimmunity. J Neuroimmunol 337:577051
Mao Z, Yin J, Zhong X et al (2015) Late-onset neuromyelitis optica spectrum disorder in AQP4-seropositivepatients in a Chinese population. BMC Neurol 15:160
Lee EJ, Lim YM, Kim SY et al (2019) The clinical and prognostic value of antinuclear antibodies in NMO-IgG seropositive neuromyelitis optica spectrum disorder. J Neuroimmunol 328:1–4
Schwartz M, Kipnis J (2005) Protective autoimmunity and neuroprotection in inflammatory and noninflammatory neurodegenerative diseases. J Neurol Sci 233:163–166
Pashnina IA, Krivolapova IM, Fedotkina TV et al (2021) Antinuclear autoantibodies in health: autoimmunity is not a synonym of autoimmune disease. Antibodies (Basel) 10:9
Acknowledgements
The authors thank the NMOSD patients at the Beijing Tongren Hospital for their participation and support.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
None.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yang, Q., Lai, C., Meng, C. et al. Clinical features and visual prognosis of very late-onset neuromyelitis optica spectrum disorder–related optic neuritis. Neurol Sci 45, 2191–2197 (2024). https://doi.org/10.1007/s10072-023-07187-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-023-07187-9