Abstract
Objective
Primary brainstem hemorrhage (PBSH) is a devastating acute neurological disorder with a poor prognosis. This study aimed to identify risk factors associated with poor outcomes in PBSH patients and develop a novel nomogram for predicting prognosis, with external validation.
Methods
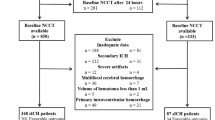
A total of 379 patients with PBSH were included in the training cohort. The primary outcome of interest was a modified Rankin Scale score (mRS) of 4–6 at 90 days post-onset. Multivariable logistic regression was used to construct a nomogram based on relevant variables. Model performance was tested in the training cohort and externally validated for discriminatory ability, calibration, and clinical utility at a separate institution. The nomogram was also compared to the ICH score in terms of predictive ability.
Results
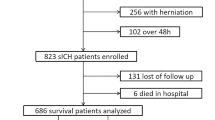
The poor outcome rate at 90 days was 57.26% (217/379) in the training cohort and 61.27% (106/173) in the validation cohort. Multivariable logistic regression analysis identified age, Glasgow Coma Scale (GCS) score, and hematoma size as significant risk factors for poor outcomes. Nomograms based on these variables demonstrated good discrimination, with an area under the curve (AUC) of 0.855 and 0.836 in the training and validation cohorts, respectively. Furthermore, the nomogram showed superior predictive value to the ICH score for the 90-day outcome in both cohorts.
Conclusion
This study developed and externally validated a nomogram risk prediction model for predicting poor outcomes at 90 days in patients with PBSH, using age, GCS score, and hematoma size as predictors. The nomogram demonstrated good discrimination, calibration, and clinical validity, serving as a valuable assessment and decision-making tool.





Similar content being viewed by others
Data Availability
Data is available on reasonable request.
References
Nakajima K (1983) Clinicopathological study of pontine hemorrhage. Stroke 14(4):485–493. https://doi.org/10.1161/01.str.14.4.485
Takeuchi S, Suzuki G, Takasato Y, Masaoka H, Hayakawa T, Otani N, Yatsushige H, Shigeta K, Momose T, Wada K, Nawashiro H (2013) Prognostic factors in patients with primary brainstem hemorrhage. Clin Neurol Neurosurg 115(6):732–735. https://doi.org/10.1016/j.clineuro.2012.08.022
Cole FM, Yates PO (1967) The occurrence and significance of intracerebral micro-aneurysms. J Pathol Bacteriol 93(2):393–411. https://doi.org/10.1002/path.1700930202
van Asch CJ, Luitse MJ, Rinkel GJ, van der Tweel I, Algra A, Klijn CJ (2010) Incidence, case fatality, and functional outcome of intracerebral haemorrhage over time, according to age, sex, and ethnic origin: a systematic review and meta-analysis. Lancet Neurol 9(2):167–176. https://doi.org/10.1016/S1474-4422(09)70340-0
Wijdicks EF, St Louis E (1997) Clinical profiles predictive of outcome in pontine hemorrhage. Neurology 49(5):1342–1346. https://doi.org/10.1212/wnl.49.5.1342
Nilsson OG, Lindgren A, Brandt L, Saveland H (2002) Prediction of death in patients with primary intracerebral hemorrhage: a prospective study of a defined population. J Neurosurg 97(3):531–536. https://doi.org/10.3171/jns.2002.97.3.0531
Wang SS, Yang Y, Velz J, Keller E, Luft AR, Regli L, Neidert MC, Bozinov O (2019) Management of brainstem haemorrhages. Swiss Med Wkly 149:w20062. https://doi.org/10.4414/smw.2019.20062
Dziewas R, Kremer M, Ludemann P, Nabavi DG, Drager B, Ringelstein B (2003) The prognostic impact of clinical and CT parameters in patients with pontine hemorrhage. Cerebrovasc Dis 16(3):224–229. https://doi.org/10.1159/000071120
Parry-Jones AR, Abid KA, Di Napoli M, Smith CJ, Vail A, Patel HC, King AT, Tyrrell PJ (2013) Accuracy and clinical usefulness of intracerebral hemorrhage grading scores: a direct comparison in a UK population. Stroke 44(7):1840–1845. https://doi.org/10.1161/STROKEAHA.113.001009
Huang K, Ji Z, Sun L, Gao X, Lin S, Liu T, Xie S, Zhang Q, Xian W, Zhou S, Gu Y, Wu Y, Wang S, Lin Z, Pan S (2017) Development and validation of a grading scale for primary pontine hemorrhage. Stroke 48(1):63–69. https://doi.org/10.1161/STROKEAHA.116.015326
Huang KB, Ji Z, Wu YM, Wang SN, Lin ZZ, Pan SY (2012) The prediction of 30-day mortality in patients with primary pontine hemorrhage: a scoring system comparison. Eur J Neurol 19(9):1245–1250. https://doi.org/10.1111/j.1468-1331.2012.03724.x
Becker KJ, Baxter AB, Cohen WA, Bybee HM, Tirschwell DL, Newell DW, Winn HR, Longstreth WT Jr (2001) Withdrawal of support in intracerebral hemorrhage may lead to self-fulfilling prophecies. Neurology 56(6):766–772. https://doi.org/10.1212/wnl.56.6.766
Alkhachroum A, Bustillo AJ, Asdaghi N, Marulanda-Londono E, Gutierrez CM, Samano D, Sobczak E, Foster D, Kottapally M, Merenda A, Koch S, Romano JG, O’Phelan K, Claassen J, Sacco RL, Rundek T (2021) Withdrawal of life-sustaining treatment mediates mortality in patients with intracerebral hemorrhage with impaired consciousness. Stroke 52(12):3891–3898. https://doi.org/10.1161/STROKEAHA.121.035233
Hemphill JC 3rd, Bonovich DC, Besmertis L, Manley GT, Johnston SC (2001) The ICH score: a simple, reliable grading scale for intracerebral hemorrhage. Stroke 32(4):891–897. https://doi.org/10.1161/01.str.32.4.891
Kim Y, Margonis GA, Prescott JD, Tran TB, Postlewait LM, Maithel SK, Wang TS, Evans DB, Hatzaras I, Shenoy R, Phay JE, Keplinger K, Fields RC, Jin LX, Weber SM, Salem AI, Sicklick JK, Gad S, Yopp AC, Mansour JC, Duh QY, Seiser N, Solorzano CC, Kiernan CM, Votanopoulos KI, Levine EA, Poultsides GA, Pawlik TM (2016) Nomograms to predict recurrence-free and overall survival after curative resection of adrenocortical carcinoma. JAMA Surg 151(4):365–373. https://doi.org/10.1001/jamasurg.2015.4516
Divani AA, Majidi S, Luo X, Souslian FG, Zhang J, Abosch A, Tummala RP (2011) The ABCs of accurate volumetric measurement of cerebral hematoma. Stroke 42(6):1569–1574. https://doi.org/10.1161/STROKEAHA.110.607861
Wessels T, Moller-Hartmann W, Noth J, Klotzsch C (2004) CT findings and clinical features as markers for patient outcome in primary pontine hemorrhage. AJNR Am J Neuroradiol 25(2):257–260
Chung CS, Park CH (1992) Primary pontine hemorrhage: a new CT classification. Neurology 42(4):830–834. https://doi.org/10.1212/wnl.42.4.830
Qureshi AI, Palesch YY, Barsan WG, Hanley DF, Hsu CY, Martin RL, Moy CS, Silbergleit R, Steiner T, Suarez JI, Toyoda K, Wang Y, Yamamoto H, Yoon BW, Investigators A-T, the Neurological Emergency Treatment Trials N (2016) Intensive blood-pressure lowering in patients with acute cerebral hemorrhage. N Engl J Med 375(11):1033–1043. https://doi.org/10.1056/NEJMoa1603460
Flower O, Smith M (2011) The acute management of intracerebral hemorrhage. Curr Opin Crit Care 17(2):106–114. https://doi.org/10.1097/MCC.0b013e328342f823
Cheung RT, Zou LY (2003) Use of the original, modified, or new intracerebral hemorrhage score to predict mortality and morbidity after intracerebral hemorrhage. Stroke 34(7):1717–1722. https://doi.org/10.1161/01.STR.0000078657.22835.B9
Weimer JM, Nowacki AS, Frontera JA (2016) Withdrawal of life-sustaining therapy in patients with intracranial hemorrhage: self-fulfilling prophecy or accurate prediction of outcome? Crit Care Med 44(6):1161–1172. https://doi.org/10.1097/CCM.0000000000001570
Murata Y, Yamaguchi S, Kajikawa H, Yamamura K, Sumioka S, Nakamura S (1999) Relationship between the clinical manifestations, computed tomographic findings and the outcome in 80 patients with primary pontine hemorrhage. J Neurol Sci 167(2):107–111. https://doi.org/10.1016/s0022-510x(99)00150-1
Ye Z, Huang X, Han Z, Shao B, Cheng J, Wang Z, Zhang Z, Xiao M (2015) Three-year prognosis of first-ever primary pontine hemorrhage in a hospital-based registry. J Clin Neurosci 22(7):1133–1138. https://doi.org/10.1016/j.jocn.2014.12.024
Jang JH, Song YG, Kim YZ (2011) Predictors of 30-day mortality and 90-day functional recovery after primary pontine hemorrhage. J Korean Med Sci 26(1):100–107. https://doi.org/10.3346/jkms.2011.26.1.100
Behrouz R (2018) Prognostic factors in pontine haemorrhage: a systematic review. Eur Stroke J 3(2):101–109. https://doi.org/10.1177/2396987317752729
Meng X, Wang Q, Pei X, Xie F (2022) Prognosis and influencing factors of early microsurgery for severe hypertensive brainstem hemorrhage. Dis Markers 2022:5062591. https://doi.org/10.1155/2022/5062591
Matsukawa H, Shinoda M, Fujii M, Takahashi O, Murakata A (2015) Risk factors for mortality in patients with non-traumatic pontine hemorrhage. Acta Neurol Scand 131(4):240–245. https://doi.org/10.1111/ane.12312
An SJ, Kim TJ, Yoon BW (2017) Epidemiology, risk factors, and clinical features of intracerebral hemorrhage: an update. J Stroke 19(1):3–10. https://doi.org/10.5853/jos.2016.00864
Morotti A, Jessel MJ, Brouwers HB, Falcone GJ, Schwab K, Ayres AM, Vashkevich A, Anderson CD, Viswanathan A, Greenberg SM, Gurol ME, Romero JM, Rosand J, Goldstein JN (2016) CT angiography spot sign, hematoma expansion, and outcome in primary pontine intracerebral hemorrhage. Neurocrit Care 25(1):79–85. https://doi.org/10.1007/s12028-016-0241-2
Ding WL, Xiang YS, Liao JC, Wang SY, Wang XY (2020) Early tracheostomy is associated with better prognosis in patients with brainstem hemorrhage. J Integr Neurosci 19(3):437–442. https://doi.org/10.31083/j.jin.2020.03.25
Davis SM, Broderick J, Hennerici M, Brun NC, Diringer MN, Mayer SA, Begtrup K, Steiner T, Recombinant Activated Factor VIIIHTI (2006) Hematoma growth is a determinant of mortality and poor outcome after intracerebral hemorrhage. Neurology 66(8):1175–1181. https://doi.org/10.1212/01.wnl.0000208408.98482.99
Delcourt C, Huang Y, Arima H, Chalmers J, Davis SM, Heeley EL, Wang J, Parsons MW, Liu G, Anderson CS, Investigators I (2012) Hematoma growth and outcomes in intracerebral hemorrhage: the INTERACT1 study. Neurology 79(4):314–319
Chen D, Tang Y, Nie H, Zhang P, Wang W, Dong Q, Wu G, Xue M, Tang Y, Liu W, Pan C, Tang Z (2021) Primary brainstem hemorrhage: a review of prognostic factors and surgical management. Front Neurol 12:727962. https://doi.org/10.3389/fneur.2021.727962
Hara T, Nagata K, Kawamoto S, Sashida J, Abe T, Wada A, Sakamoto T (2001) Functional outcome of primary pontine hemorrhage: conservative treatment or stereotaxic surgery. No Shinkei Geka 29(9):823–829
Hemphill JC 3rd, Greenberg SM, Anderson CS, Becker K, Bendok BR, Cushman M, Fung GL, Goldstein JN, Macdonald RL, Mitchell PH, Scott PA, Selim MH, Woo D, American Heart Association Stroke C, Council on C, Stroke N, Council on Clinical C (2015) Guidelines for the management of spontaneous intracerebral hemorrhage: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 46(7):2032–2060. https://doi.org/10.1161/STR.0000000000000069
Steiner T, Al-Shahi Salman R, Beer R, Christensen H, Cordonnier C, Csiba L, Forsting M, Harnof S, Klijn CJ, Krieger D, Mendelow AD, Molina C, Montaner J, Overgaard K, Petersson J, Roine RO, Schmutzhard E, Schwerdtfeger K, Stapf C, Tatlisumak T, Thomas BM, Toni D, Unterberg A, Wagner M, European Stroke O (2014) European Stroke Organisation (ESO) guidelines for the management of spontaneous intracerebral hemorrhage. Int J Stroke 9(7):840–855. https://doi.org/10.1111/ijs.12309
Chen LH, Li FJ, Zhang HT, Chen WJ, Sun K, Xu RX (2021) The microsurgical treatment for primary hypertensive brainstem hemorrhage: Experience with 52 patients. Asian J Surg 44(1):123–130. https://doi.org/10.1016/j.asjsur.2020.04.016
Ichimura S, Bertalanffy H, Nakaya M, Mochizuki Y, Moriwaki G, Sakamoto R, Fukuchi M, Fujii K (2018) Surgical treatment for primary brainstem hemorrhage to improve postoperative functional outcomes. World Neurosurg 120:e1289–e1294. https://doi.org/10.1016/j.wneu.2018.09.055
Funding
This study was supported by the Wuxi City Social Development Science and Technology Demonstration Project (No. N20201008).
Author information
Authors and Affiliations
Contributions
All authors take responsibility for the integrity and the accuracy of this manuscript. YD: study concept and design, data collection, data analysis, writing the manuscript. YX: participated in the study design, data collection. YW: participated in the study design, revised. JD: participated in the study design, revised.
Corresponding author
Ethics declarations
Ethics approval
This study was approved by the Hospital Ethics Committee. Due to the retrospective character of this study, the requirement of informed consent was waived.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ding, Y., Xu, Y., Wang, Y. et al. A nomogram risk prediction model for poor outcome of primary brainstem hemorrhage based on clinical data and radiographic features. Neurol Sci 44, 3967–3978 (2023). https://doi.org/10.1007/s10072-023-06866-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-023-06866-x