Abstract
Background and aims
Patients with multiple sclerosis (PwMS) may suffer severely from falling and gait disturbance. Cognitive dysfunction, a common condition in MS patients, may also increase falling rates, regardless of physical disability. We planned this study to determine the fall rate and risk factors in MS patients, follow patients for falls, and reveal the relationship between falls and cognitive dysfunction.
Methods
The study was conducted on 124 patients who have RRMS diagnoses. Patients' gait speed, simultaneous gait speed during other tasks, functions of the upper extremity, balance rating, and fear of falling were evaluated with dual-task Timed-Up-and-Go-3 versions (TUG, TUG-C, TUG-M), Timed 25 Foot Walk (T25WFT), Nine Hole Peg Test (9HPT), Berg Balance Scale (BBS) and Falls Efficacy Scale-International (FES-I) tests. Cognitive functions, fatigue levels, and quality of life were measured with the Symbol Digit Modalities Test (SDMT), Fatigue Severity Scale (FSS), and Multiple Sclerosis Quality of Life (MSQoL) test. Two groups were formed as "fallers" and "non-faller patients". We monitored the patients in six months period.
Results
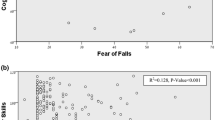
Forty-six patients fell at least once in the last one year before the study began. Fallers were older, less educated, had lower SDMT scores and higher disability scores. Non-faller patients scored lower in FES-I, TUG, and FSS tests. SDMT scores showed statistically significant, linear, positive, and moderate correlation with BBS and 9HPT scores (r = 0.307, p = 0.038, and r = 0.320, p = 0.030, respectively).
Conclusion
We determined that advanced age, lower education level, and cognitive dysfunction adversely affect gait speed and balance. Among the fallers, those with lower SDMT and MoCA scores had higher falling rates. We determined that EDSS and BBS scores are predictive factors for falls in patients with MS. In conclusion, patients with cognitive impairment should be closely monitored for the risk of falling. Consideration of falls during follow-up examinations might be predictive of cognitive deterioration in patients with MS.

Similar content being viewed by others
Change history
22 April 2023
A Correction to this paper has been published: https://doi.org/10.1007/s10072-023-06819-4
References
Lublin FD, Reingold SC, Cohen et al (2014) Defining the clinical course of multiple sclerosis: the 2013 revisions. Neurology 83(3):278–286. https://doi.org/10.1212/WNL.0000000000000560
Deloire MS, Ruet A, Hamel D et al (2011) MRI predictors of cognitive outcome in early multiple sclerosis. Neurology 76(13):1161–1167. https://doi.org/10.1212/WNL.0b013e318212a8be
Gunn HJ, Newell P, Haas B et al (2013) Identification of risk factors for falls in multiple sclerosis: a systematic review and meta-analysis. Phys Ther 93(4):504–513. https://doi.org/10.2522/ptj.20120231
Prosperini L, Castelli L, De Luca F et al (2016) Task-dependent deterioration of balance underpinning cognitive-postural interference in MS. Neurology 87(11):1085–1092. https://doi.org/10.1212/WNL.0000000000003090
Motl RW, Learmonth YC (2014) Neurological disability and its association with walking impairment in multiple sclerosis: brief review. Neurodegenerative Dis Manag 4(6):491–500. https://doi.org/10.2217/nmt.14.32
D’Orio VL, Foley FW, Armentano F et al (2012) Cognitive and motor functioning in patients with multiple sclerosis: neuropsychological predictors of walking speed and falls. J Neurol Sci 316(1-2):42–46. https://doi.org/10.1016/j.jns.2012.02.003
Sumowski JF, Benedict R, Enzinger C et al (2018) Cognition in multiple sclerosis: State of the field and priorities for the future. Neurology 90(6):278–288. https://doi.org/10.1212/WNL.0000000000004977
Olazarán J, Cruz I, Benito-León J et al (2009) Cognitive dysfunction in multiple sclerosis: methods and prevalence from the GEDMA Study. Eur Neurol 61(2):87–93. https://doi.org/10.1159/000177940
Gunn H, Creanor S, Haas B et al (2014) Frequency, characteristics, and consequences of falls in multiple sclerosis: findings from a cohort study. Arch Phys Med Rehabil 95(3):538–545. https://doi.org/10.1016/j.apmr.2013.08.244
Coote S, Hogan N, Franklin S (2013) Falls in people with multiple sclerosis who use a walking aid: prevalence, factors, and effect of strength and balance interventions. Arch Phys Med Rehabil 94(4):616–621. https://doi.org/10.1016/j.apmr.2012.10.020
Matsuda PN, Shumway-Cook A, Ciol M et al (2012) Understanding falls in multiple sclerosis: association of mobility status, concerns about falling, and accumulated impairments. Phys Ther 92(3):407–415. https://doi.org/10.2522/ptj.20100380
Kalron A, Givon U, Frid L et al (2016) Static Posturography and Falls According to Pyramidal, Sensory and Cerebellar Functional Systems in People with Multiple Sclerosis. PloS one 11(10):e0164467. https://doi.org/10.1371/journal.pone.0164467
Ulus Y, Durmus D, Akyol Y et al (2012) Reliability and validity of the Turkish version of the Falls Efficacy Scale International (FES-I) in community-dwelling older persons. Arch Gerontol Geriatr 54(3):429–433. https://doi.org/10.1016/j.archger.2011.06.010
Vister E, Tijsma ME, Hoang PD et al (2017) Fatigue, Physical Activity, Quality of Life, and Fall Risk in People with Multiple Sclerosis. Int J MS Care 19(2):91–98. https://doi.org/10.7224/1537-2073.2015-077
Kurtzke JF (1983) Rating neurologic impairment in multiple sclerosis: an expanded disability status scale (EDSS). Neurology 33(11):1444–1452. https://doi.org/10.1212/wnl.33.11.1444
Feys P, Lamers I, Francis G et al (2017) The Nine-Hole Peg Test as a manual dexterity performance measure for multiple sclerosis. Multiple Sclerosis (Houndmills, Basingstoke, England) 23(5):711–720. https://doi.org/10.1177/1352458517690824
Cohen ET, Potter K, Allen DD et al (2015) Selecting Rehabilitation Outcome Measures for People with Multiple Sclerosis. Int J MS Care 17(4):181–189. https://doi.org/10.7224/1537-2073.2014-067
Zackowski KM, Wang JI, McGready J et al (2015) Quantitative sensory and motor measures detect change overtime and correlate with walking speed in individuals with multiple sclerosis. Mult Scler Relat Disord 4(1):67–74. https://doi.org/10.1016/j.msard.2014.11.001
Kalron A, Dolev M, Givon U (2017) Further construct validity of the Timed Up-and-Go Test as a measure of ambulation in multiple sclerosis patients. Eur J Phys Rehabil Med 53(6):841–847. https://doi.org/10.23736/S1973-9087.17.04599-3
Quinn G, Comber L, McGuigan C et al (2019) Discriminative ability and clinical utility of the Timed Up and Go (TUG) in identifying falls risk in people with multiple sclerosis: a prospective cohort study. Clin Rehabil 33(2):317–326. https://doi.org/10.1177/0269215518793481
Sahin F, Yilmaz F, Ozmaden A et al (2008) Reliability and validity of the Turkish version of the Berg Balance Scale. J Geriatr Phys Ther (2001) 31(1):32–37. https://doi.org/10.1519/00139143-200831010-00006
Muir SW, Berg K, Chesworth B et al (2008) Use of the Berg Balance Scale for predicting multiple falls in community-dwelling elderly people: a prospective study. Phys Ther 88(4):449–459. https://doi.org/10.2522/ptj.20070251
Aksoy S, Timer E, Mumcu S et al (2013) Screening for cognitive impairment in multiple sclerosis with MOCA test. Turk J Neurol 2013(19):52–55. https://doi.org/10.4274/Tnd.86570
Parmenter BA, Weinstock-Guttman B, Garg N et al (2007) Screening for cognitive impairment in multiple sclerosis using the Symbol digit Modalities Test. Mult Scler (Houndmills, Basingstoke, England) 13(1):52–57. https://doi.org/10.1177/1352458506070750
Krupp LB, LaRocca NG, Muir-Nash J et al (1989) The fatigue severity scale. Application to patients with multiple sclerosis and systemic lupus erythematosus. Arch Neurol 46(10):1121–1123. https://doi.org/10.1001/archneur.1989.00520460115022
Simeoni M, Auquier P, Fernandez O et al (2008) Validation of the Multiple Sclerosis International Quality of Life questionnaire. Mult Scler (Houndmills, Basingstoke, England) 14(2):219–230. https://doi.org/10.1177/1352458507080733
Mazumder R, Lambert WE, Nguyen T et al (2015) Fear of Falling Is Associated with Recurrent Falls in People with Multiple Sclerosis: A Longitudinal Cohort Study. Int J MS Care 17(4):164–170. https://doi.org/10.7224/1537-2073.2014-042
Kalron A, Aloni R, Allali G (2018) The relationship between depression, anxiety and cognition and its paradoxical impact on falls in multiple sclerosis patients. Mult Scler Relat Disord 25:167–172. https://doi.org/10.1016/j.msard.2018.07.029
Nilsagård Y, Gunn H, Freeman J et al (2015) Falls in people with MS--an individual data meta-analysis from studies from Australia, Sweden, United Kingdom and the United States. Mult Scler (Houndmills, Basingstoke, England) 21(1):92–100. https://doi.org/10.1177/1352458514538884
Amato MP, Portaccio E, Goretti B et al (2010) Cognitive impairment in early stages of multiple sclerosis. Neurol Sci 31(Suppl 2):S211–S214. https://doi.org/10.1007/s10072-010-0376-4
Rosso AL, Studenski SA, Chen WG et al (2013) Aging, the central nervous system, and mobility. J Gerontol A Biol Sci Med Sci 68(11):1379–1386. https://doi.org/10.1093/gerona/glt089
Matsuda PN, Shumway-Cook A, Bamer AM et al (2011) Falls in multiple sclerosis. PM R 3(7):624–632. https://doi.org/10.1016/j.pmrj.2011.04.015
Kalron A, Allali G, Achiron A (2018) Cerebellum and cognition in multiple sclerosis: the fall status matters. J Neurol 265(4):809–816. https://doi.org/10.1007/s00415-018-8774-2
Marrie RA, Cohen J, Stuve O et al (2015) A systematic review of the incidence and prevalence of comorbidity in multiple sclerosis: overview. Mult Scler (Houndmills, Basingstoke, England) 21(3):263–281. https://doi.org/10.1177/1352458514564491
Nilsagård Y, Lundholm C, Denison E et al (2009) Predicting accidental falls in people with multiple sclerosis -- a longitudinal study. Clin Rehabil 23(3):259–269. https://doi.org/10.1177/0269215508095087
Cameron MH, Nilsagard Y (2018) Balance, gait, and falls in multiple sclerosis. Handb Clin Neurol 159:237–250
Giannì C, Prosperini L, Jonsdottir J et al (2014) A systematic review of factors associated with accidental falls in people with multiple sclerosis: a meta-analytic approach. Clin Rehabil 28(7):704–716. https://doi.org/10.1177/0269215513517575
Tajali S, Shaterzadeh-Yazdi MJ, Negahban H et al (2017) Predicting falls among patients with multiple sclerosis: Comparison of patient-reported outcomes and performance-based measures of lower extremity functions. Mult Scler Relat Disord 17:69–74. https://doi.org/10.1016/j.msard.2017.06.014
Sosnoff JJ, Balantrapu S, Pilutti LA et al (2013) Cognitive processing speed is related to fall frequency in older adults with multiple sclerosis. Arch Phys Med Rehabil 94(8):1567–1572. https://doi.org/10.1016/j.apmr.2013.02.009
Twork S, Wiesmeth S, Spindler M et al (2010) Disability status and quality of life in multiple sclerosis: non-linearity of the Expanded Disability Status Scale (EDSS). Health Qual Life Outcomes 8:55. https://doi.org/10.1186/1477-7525-8-55
Kragt JJ, van der Linden FA, Nielsen JM et al (2006) Clinical impact of 20% worsening on Timed 25-foot Walk and 9-hole Peg Test in multiple sclerosis. Mult Scler (Houndmills, Basingstoke, England) 12(5):594–598. https://doi.org/10.1177/1352458506070768
Acknowledgements
There is no funding source of this study
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Authors have no competing interests to declare.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: The original article contains an error during online publication. In Material and methods under Study design and participants, “xxxxxx…” should be replace to "University of Health Sciences, Izmir Bozyaka Education and Research Hospital.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bilgin, Y.O.U., Koskderelioglu, A. & Gedizlioglu, M. Fall risk is related to cognitive functioning in ambulatory multiple sclerosis patients. Neurol Sci 44, 3233–3242 (2023). https://doi.org/10.1007/s10072-023-06770-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-023-06770-4