Abstract
Purpose
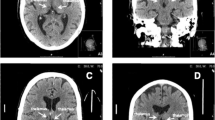
Occlusion of artery of Percheron (AOP), a rare variant of paramedian branches of posterior cerebral artery, results in a characteristic pattern of ischemic lesions in bilateral paramedian thalami with or without midbrain and anterior thalami involvement.
Aim
To evaluate the prevalence, the clinical, and the imaging features of AOP infarction in a single comprehensive stroke center experience.
Methods
We retrospectively search in our stroke center database, patients with ischemic lesions in the AOP distribution. We collected clinical features and time between hospital admission and diagnosis. Imaging findings were categorized following a pre-selected classification.
Results
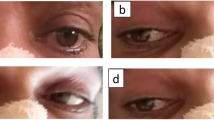
Of 2830 ischemic stroke admitted in our center, we identified 15 patients with AOP infarction (0.53%). Clinical manifestations were variable, but oculomotor disturbances, particularly vertical gaze palsy, were the most observed, followed by consciousness impairment, varying from drowsiness to coma. The most frequent imaging pattern was bilateral paramedian thalamic infarction with midbrain infarction, and the V-sign was recognized in 6 cases from this group. In 8 patients a fetal origin of the PCA was observed. The average time from first hospital admission to diagnosis was 28.09 h.
Conclusions
The prevalence of AOP infarction in our center was 0.53%. Diagnosis of AOP infarction can be challenging and should be suspected in case of sudden altered consciousness.




Similar content being viewed by others
Data Availability
Anonymized data not published within this article will be made available by request from any qualified investigator.
References
Castaigne P, Lhermitte F, Buge A et al (1981) Paramedian thalamic and midbrain infarcts: clinical and neuropathological study. Ann Neurol 10:127–148
Carrera E, Michel P, Bogousslavsky J (2004) Anteromedian, central, and posterolateral infarcts of the thalamus: three variant types. Stroke 35:2826–2831
Uz A (2007) Variations in the origin of the thalamoperforating arteries. J Clin Neurosci 14:134–137
Percheron G (1973) The anatomy of the arterial supply of the human thalamus and its use for the interpretation of the thalamic vascular pathology. Z Neurol 205:1–13
Lazzaro NA, Wright B, Castillo M et al (2010) Artery of percheron infarction: imaging patterns and clinical spectrum. Am J Neuroradiol 31:1283–1289
Tucha O, Naumann M, Berg D et al (2001) Bilateral thalamic infarction: clinical, etiological and mri correlates. Acta Neurol Scand 103:35–42
Kostanian V, Cramer SC (2007) Artery of Percheron thrombolysis. Am J Neuroradiol 28:870–871
Hawkes MA, Arena JE, Rollán C et al (2015) Bilateral paramedian thalamic infarction. Neurologist 20:89–92
Matheus MG, Castillo M (2003) Imaging of acute bilateral paramedian thalamic and mesencephalic infarcts. Am J Neuroradiol 24:2005–2008
O’Reilly MK, Mogensen MA (2019) Artery of Percheron stroke: imaging and clinical findings. PM R 11:1135–1138
Kolominsky-Rabas PL, Weber M, Gefeller O et al (2001) Epidemiology of ischemic stroke subtypes according to TOAST criteria: incidence, recurrence, and long-term survival in ischemic stroke subtypes: a population-based study. Stroke 32:2735–2740
Olivato S, Nizzoli S, Cavazzuti M et al (2016) e-NIHSS: an expanded National Institutes of Health Stroke Scale weighted for anterior and posterior circulation strokes. J Stroke Cerebrovasc Dis 25:2953–2957
Caplan LR (1980) Top of the basilar syndrome. Neurology 30:72–79
Deleu D, Imam YZB, Mesraoua B et al (2012) Vertical one-and-a-half syndrome with contralesional pseudo-abducens palsy in a patient with thalamomesencephalic stroke. J Neurol Sci 312:180–183
Arauz A, Patiño-Rodríguez HM, Vargas-González JC et al (2014) Clinical spectrum of artery of percheron infarct: clinical-radiological correlations. J Stroke Cerebrovasc Dis 23:1083–1088
Xu Z, Sun L, Duan Y et al (2017) Assessment of Percheron infarction in images and clinical findings. J Neurol Sci 383:87–92
Cao W, Dong Q, Li L et al (2012) Bilateral thalamic infarction and DSA demonstrated AOP after thrombosis. Acta Radiol Short Rep 1:1–2
Stamm BJ, Lineback CM, Skolarus LE et al (2018) Artery of percheron infarct: 12 cases and their complex clinical courses. Neurohospitalist 8:141–145
Anghelescu A (2018) Uncommon association of two anatomical variants of cerebral circulation: a fetal-type posterior cerebral artery and inferred artery of Percheron, complicated with paramedian thalamomesencephalic stroke—case presentation and literature review. Case Rep Neurol Med 2018:1–9
Förster A, Nölte I, Wenz H et al (2014) Anatomical variations in the posterior part of the circle of willis and vascular pathology in bilateral thalamic infarction. J Neuroimaging 24:325–330
Jiménez Caballero PE (2010) Bilateral paramedian thalamic artery infarcts: report of 10 cases. J Stroke Cerebrovasc Dis 19:283–289
Sandvig A, Lundberg S, Neuwirth J (2017) Artery of Percheron infarction: a case report. J Med Case Rep 11:1–5
Roitberg BZ, Tuccar E, Alp MS (2002) Bilateral paramedian thalamic infarct in the presence of an unpaired thalamic perforating artery. Acta Neurochir (Wien) 144:301–304
Debray S, Demaerel P, Lemmens R et al (2017) Non-REM sleep EEG pattern in acute bithalamic paramedian infarction. Acta Neurol Belg 117:921–924
Schmahmann JD (2003) Vascular syndromes of the thalamus. Stroke 34:2264–2278
Weidauer S, Nichtweiß M, Zanella FE et al (2004) Assessment of paramedian thalamic infarcts: MR imaging, clinical features and prognosis. Eur Radiol 14:1615–1626
Schaller-Paule MA, Oeckel AM, Schüre JR, Keil F, Hattingen E, Foerch C, Rauch M (2021) Isolated thalamic stroke - analysis of clinical characteristics and asymmetry of lesion distribution in a retrospective cohort study. Neurol Res Pract 3(1):49. https://doi.org/10.1186/s42466-021-00148-7
Hindman J, Bowren MD, Bruss J et al (2018) Thalamic strokes that severely impair arousal extend into the brainstem. Ann Neurol 84:926
Acknowledgements
We thank the patients and the patients’ family for their kind cooperation. We would like to thank all professionals involved in stroke care during the pandemic.
Author information
Authors and Affiliations
Contributions
A.C., I.F, and F.Gi. contributed to the study design. I.F., and A.C. performed data collections. K.G., and F.Gr. performed imaging analysis. I.F., A.C., and F.Gi. wrote the article. F.Gr. reviewed and critiqued the manuscript. A.To., R.F.M., and P.L.S supervised the research.
Corresponding author
Ethics declarations
Ethics approval
All procedures performed in the studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The paper does not report on primary research. Our analysis looked retrospectively at outcomes for a large cohort of patients treated. All data analyzed were collected as part of routine diagnosis and treatment.
Consent to participate
Informed consent was waived given to the retrospective anonymous collection of data, according to Italian regulations.
Consent for publication
Informed consent was waived given to the retrospective anonymous collection of data, according to Italian regulations.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Antonio Ciacciarelli, Isabella Francalanza, and Fabrizio Giammello contributed equally to this work and should be considered co-first authors.
Francesca Granata and Paolino La Spina contributed equally to this work and should be considered co-last authors.
Supplementary Information
Below is the link to the electronic supplementary material.

Supplementary figure 1.
Electroencephalography of patient n. 11 (see main text). (PNG 151 kb)

Supplementary figure 2.
Electroencephalography of patient n. 8 (see main text). (PNG 166 kb)

Supplementary figure 3.
Correlation analysis and linear regression analysis of vomuletric measurement of thalamic lesion with NIHSS and GCS. The infarct volume correlates significantly with NIHSS on admission. The linear regression analysis showed a tendency to relate with higher NIHSS and lower GCS, considering both admission and discharge estimation. (PNG 43 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ciacciarelli, A., Francalanza, I., Giammello, F. et al. Prevalence, clinical features, and radiological pattern of artery of Percheron infarction: a challenging diagnosis. Neurol Sci 44, 2413–2419 (2023). https://doi.org/10.1007/s10072-023-06681-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-023-06681-4